Could AI Telemedicine Undermine Chronic Care Specialization?
Analysis reveals 8 key thematic connections.
Key Findings
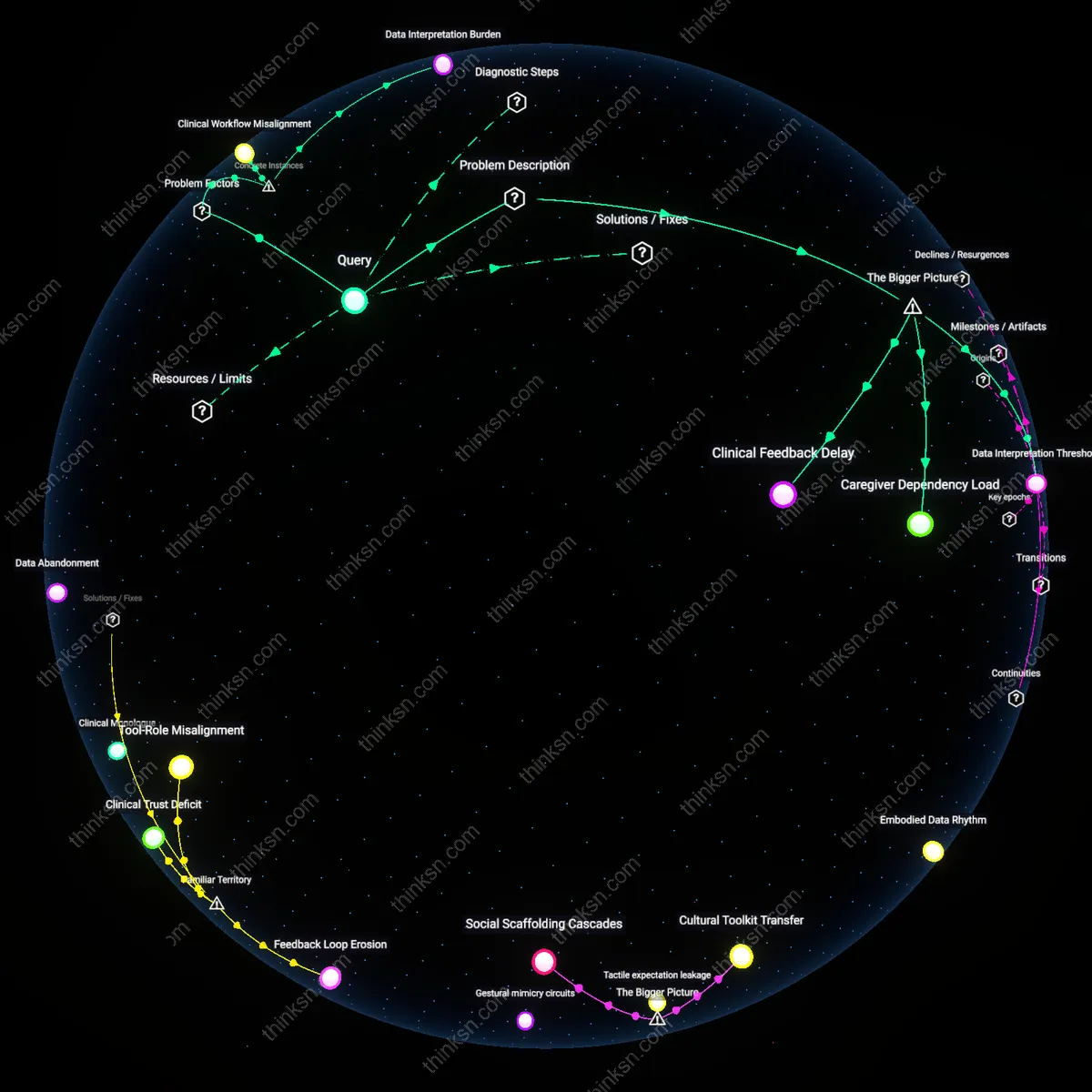
Clinical Role Redefinition
The expansion of AI-driven remote monitoring in diabetes management through platforms like Livongo has shifted diagnostic and adjustment responsibilities from primary-care physicians to algorithm-guided patient feedback loops, altering the physician’s role from active intervener to oversight supervisor. This shift depends on continuous biometric data streams interpreted by proprietary machine learning models, which generate patient-specific behavioral nudges without clinician input, thereby compressing the traditional feedback cycle between visit and intervention. What is underappreciated is that this does not merely augment care but reconfigures clinical authority, as treatment decisions are increasingly pre-empted by system-generated actions that physicians neither initiate nor control.
Asymmetric Workload Distribution
In the Veterans Health Administration’s adoption of AI-enhanced telemonitoring for heart failure patients, primary-care teams experienced a paradoxical increase in administrative burden despite reduced in-person visits, as clinicians were required to validate algorithmic alerts and reconcile discrepancies across disparate digital platforms. The mechanism—AI triaging patients into risk strata without seamless integration into existing EHR workflows—forces physicians to perform invisible cognitive labor auditing system outputs rather than engaging in direct care. This reveals that automation in chronic disease settings often transfers, rather than eliminates, labor, disproportionately accruing complexity onto generalists who lack specialized support staff.
Temporal Fragmentation of Care
The rollout of Babylon Health’s AI-powered chronic respiratory management program in NHS Lothian demonstrated that asynchronous symptom tracking and automated triage compressed patient-provider interactions into fragmented, event-driven exchanges, weakening the longitudinal continuity central to effective chronic-disease management. Because AI interventions respond to isolated data points rather than evolving patient narratives, physicians report difficulties maintaining holistic oversight, particularly for comorbid conditions requiring integrated treatment. The non-obvious consequence is that algorithmic continuity—based on data frequency—can actively erode clinical continuity, which depends on narrative coherence and trust built over time.
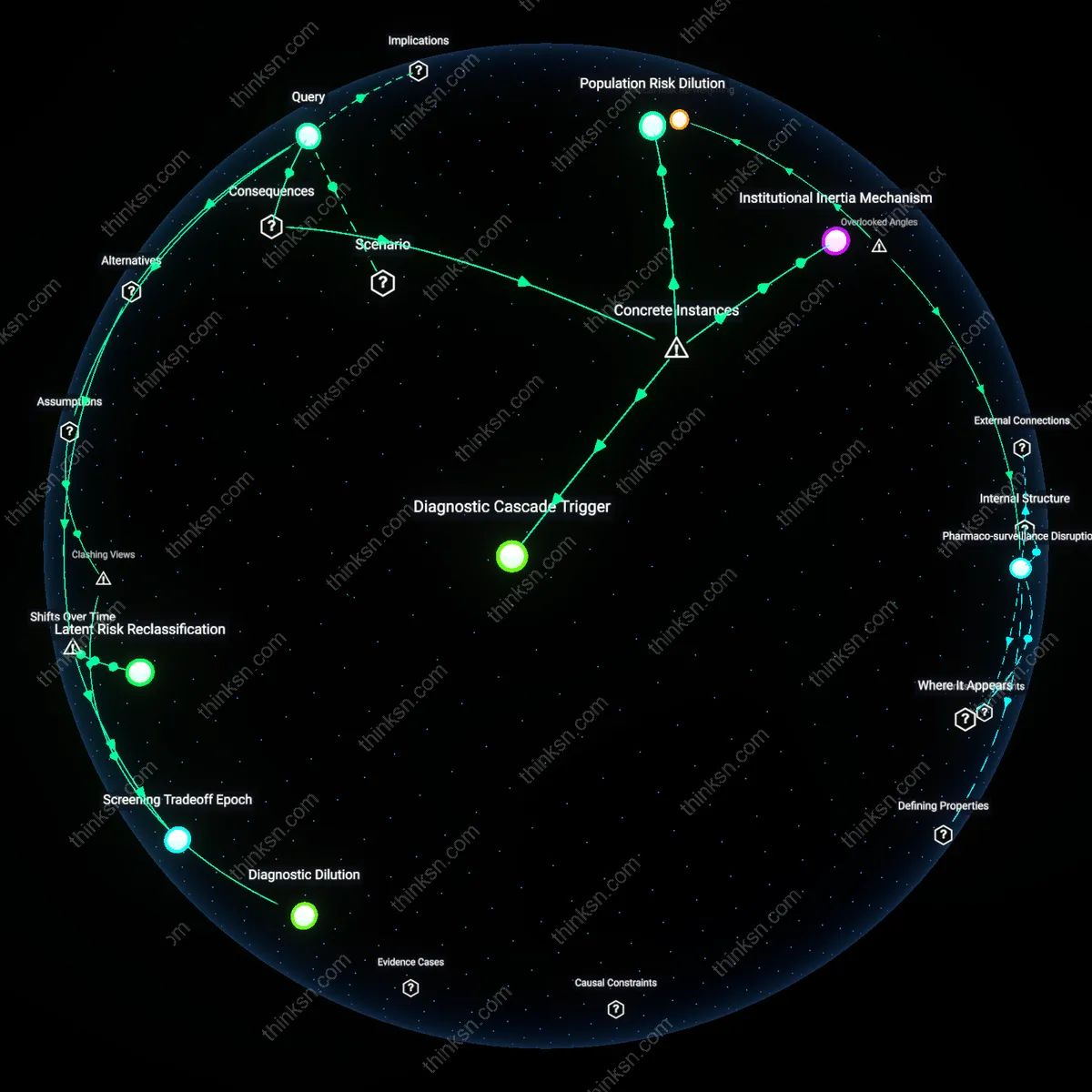
Diagnostic Erosion
AI-enabled telemedicine platforms will erode the diagnostic authority of primary-care physicians in chronic-disease management by redefining clinical judgment as a secondary input to algorithmic risk scores generated from remote monitoring devices. Insurance-linked wellness programs in states like California and Texas increasingly require patients with hypertension or diabetes to use FDA-cleared wearables whose data feed into AI systems that trigger automated care escalations—bypassing physician interpretation and reducing the doctor’s role to validating algorithmic decisions rather than initiating them. This shift weakens the physician’s epistemic position in the care chain, turning years of clinical training into post-hoc ratification of machine outputs, a dynamic rarely acknowledged in telemedicine’s patient-access narratives. The non-obvious consequence is not inefficiency or error, but the quiet reconfiguration of medical expertise as ancillary.
Regulatory Asymmetry
The uneven regulatory treatment of AI-enabled telemedicine tools versus physician decision-making exposes chronic-disease specialists to liability without commensurate control, as FDA-cleared algorithms operate in protected silos while physician deviations from their outputs are subject to malpractice scrutiny. When an AI system recommends a standard HbA1c target of 8% for an elderly diabetic and the physician overrides it for a frail patient, the clinician assumes full legal risk even if the algorithm’s one-size-fits-all logic is embedded in a platform shielded by software liability exemptions. This asymmetry transforms clinical judgment into a liability vector, discouraging nuanced care in favor of algorithmic conformity—a structural hazard that reframes physician autonomy not as a professional safeguard but as a compliance failure.
Diagnostic Sovereignty Erosion
AI-enabled telemedicine will progressively displace primary-care physicians from first-instance diagnostic authority in chronic disease, as remote monitoring platforms and algorithmic risk stratification tools—deployed by integrated payor-provider systems like UnitedHealth Group and Kaiser Permanente—routinize early detection and triage outside clinical encounters; this shift reframes the physician’s role from diagnostic initiator to intervention executor, a transition amplified by value-based care models that reward preemptive, data-driven interventions over symptom-driven consultations; the underappreciated consequence is that specialization in chronic-disease management may inadvertently lock physicians into downstream, algorithm-mediated care pathways where clinical autonomy diminishes despite rising technical complexity.
Temporal Compression Pressure
The acceleration of patient data flows through AI-augmented telemedicine platforms compresses the temporal window in which primary-care physicians can meaningfully intervene in chronic disease trajectories, as real-time analytics from wearable devices and home-based diagnostics trigger autonomous care escalations—often managed by nurse-led digital health teams or embedded behavioral nudges—before physicians are clinically notified; this systemic speeding-up, enabled by interoperable EHR infrastructures like Epic’s integrated telehealth modules and incentivized by CMS’s chronic care management reimbursement structure, transforms the physician’s expected response cadence from days to hours, an operational shift that favors protocol adherence over interpretive clinical judgment, a dynamic rarely accounted for in current medical training or workflow design.
Epidemiological Reconfiguration Risk
Widespread deployment of AI-driven telemedicine could unintentionally alter the observable epidemiology of chronic diseases by selectively engaging healthier, tech-literate, and urban-dwelling populations, thereby skewing the data used to train clinical algorithms and distorting disease prevalence signals that inform physician specialization decisions; this feedback loop, perpetuated by Silicon Valley–developed platforms (e.g., current ventures in AI-first diabetes management) that prioritize scalable, low-acuity user cohorts, risks misallocating clinical expertise toward conditions that appear dominant in digital datasets but underrepresent marginalized communities with higher actual disease burden; the systemic danger lies in physicians specializing into apparent demand that is artifactually inflated by digital stratification, not organic population need.