Should You Wait or Act Now for Moderate Psoriasis?
Analysis reveals 6 key thematic connections.
Key Findings
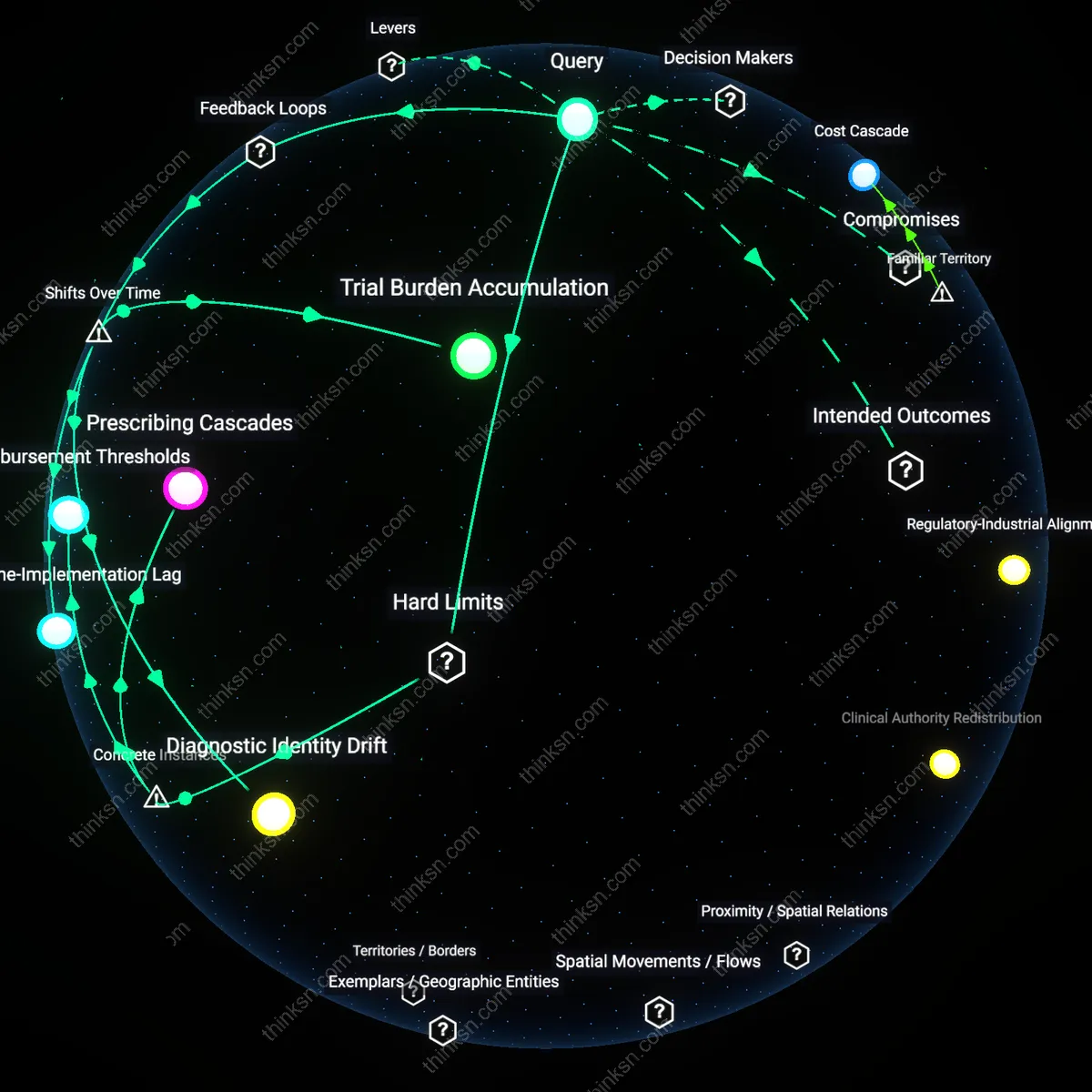
Reimbursement Thresholds
Insurance coverage dictates treatment escalation in moderate psoriasis when clinical evidence is equivocal, as seen in Germany’s statutory health insurance (GKV) requiring PASI 75 improvement within 12 weeks on phototherapy before approving biologics. This mechanism forces watchful waiting not due to clinical caution but fiscal gatekeeping, embedding cost-effectiveness—specifically the €25,000 per QALY threshold—into treatment initiation. The non-obvious reality is that therapeutic decisions pivot on budget impact assessments performed by the G-BA (Federal Joint Committee), not physician discretion or patient severity alone.
Prescribing Cascades
In the U.S. Veterans Health Administration, dermatologists delay biologic use in moderate psoriasis due to institutional protocols that mandate sequential failure on methotrexate and acitretin, creating a de facto prescribing cascade rooted in historical formulary constraints. This pathway persists despite newer evidence on biologic efficacy, because legacy treatment algorithms become embedded in EMR-based decision support tools that auto-flag deviations as outliers. The overlooked dynamic is that clinical inertia stems not from uncertainty but from systematized workflows that reify past resource limitations as current standards of care.
Market Authorization Gaps
In Japan, biologics like secukinumab are approved only for severe psoriasis, leaving moderate cases in a regulatory void regardless of individual response potential, which compels watchful waiting as a legal necessity rather than clinical choice. This boundary is enforced by the PMDA’s strict alignment of labeling with pivotal trial populations, blocking off-label use common in more permissive jurisdictions. The underappreciated point is that regulatory categorization—not disease manifestation—defines treatable thresholds, making administrative severity a structural determinant of access.
Trial Burden Accumulation
Shifting from episodic to continuous biologic access after 2015 intensified a feedback loop where patients cycle through multiple failed therapies, increasing reluctance to initiate new regimens despite eligibility; dermatologists, payers, and patients collectively reinforce this inertia through prior authorization demands, cost-sharing, and fear of long-term immunosuppression, making watchful waiting a de facto default even when guidelines favor early intervention. This dynamic emerged distinctly after the proliferation of IL-17 and IL-23 inhibitors, which created high expectations but also higher discontinuation rates due to partial responses, thereby exposing a system where therapeutic optimism is tempered by experiential fatigue—a temporally contingent outcome of the biologic saturation phase in moderate psoriasis care.
Diagnostic Identity Drift
The redefinition of 'moderate' psoriasis from a purely dermatological classification to a systemic-inflammatory proxy after 2010 established a reinforcing loop in which early biologic use generates new cardiovascular and metabolic monitoring data, which in turn justifies further early intervention, thus destabilizing watchful waiting; this shift was catalyzed by longitudinal studies linking psoriasis to comorbidities and embedded in integrated care models like psoriatic disease clinics in academic centers such as the University of Toronto and Kaiser Permanente. The non-obvious consequence is that the clinical ambiguity around treatment timing is no longer driven by skin severity alone but by the accelerating feedback between systemic risk profiling and therapeutic escalation—an identity transformation of the disease category itself over the past decade.
Guideline-Implementation Lag
Following the 2019 AAD-NPF consensus update advocating earlier biologics in moderate cases with high burden, a balancing loop formed between guideline promulgation and real-world adoption, where slow integration into electronic health record decision supports and formulary criteria delays actual practice change, particularly in rural U.S. dermatology practices reliant on legacy step therapy protocols; this lag reveals a structural inertia in which clinical evidence is filtered through institutional timelines—pharmacy benefit managers and health systems require 3–5 years to align coverage, creating a transitional phase where evidence conflict is not epistemic but temporal. The underappreciated insight is that the decision to wait or treat is less about individual risk assessment and more about the delayed synchronization of knowledge production with policy execution.