Do Low Reimbursements Drive Doctors to Specialize and Harm Equity?
Analysis reveals 9 key thematic connections.
Key Findings
Reimbursement squeeze
Setting primary-care reimbursement rates below cost directly reduces physician participation in primary care over time by eroding practice sustainability, particularly in community health centers and rural clinics after the 1992 Medicare fee schedule formalized relative value units that undervalued cognitive services compared to procedural specialties. As primary-care providers face narrowing margins, the mechanism operates through practice closures and workforce attrition, with younger physicians opting for residencies in higher-reimbursement specialties—a shift accelerated by the consolidation of medical practices under hospital systems after the 2010s that prioritized revenue-generating departments. Evidence indicates this erosion is not simply economic but structural, revealing how a policy artifact from cost-containment efforts in the 1980s became institutionalized, making primary care systematically less viable despite its demonstrated long-term value for population health outcomes.
Supply-Side Drain
Lower reimbursement rates in primary care directly reduce physician entry and retention in rural and underserved urban clinics, as doctors seek higher earnings in procedural specialties; this mechanism operates through individual financial viability calculations in practice formation, where rent, staffing, and administrative costs outpace revenue under current Medicare and Medicaid fee schedules. The result is a geographically uneven depletion of accessible first-contact care, which reinforces existing disparities in chronic disease management, particularly for diabetic and hypertensive populations in regions like the Mississippi Delta and Appalachia. What’s underappreciated is that this isn’t merely a wage preference but a structural exclusion—primary care becomes financially unsustainable, not just less attractive.
Equity Debt
Persistent underpayment of primary care creates compounding health deficits in low-income and Medicaid-enrolled populations, who rely exclusively on these services for preventive screenings, mental health, and care coordination; because reduced provider supply increases wait times and decreases continuity, conditions like asthma in children or prenatal care in Black and Hispanic communities deteriorate faster than in privately insured groups. Evidence indicates this dynamic entrenches race- and class-based gaps in life expectancy, turning payment policy into a silent determinant of mortality trajectories. The underappreciated insight is that reimbursement rates function as a form of deferred public investment—underpaying primary care today generates higher downstream costs and inequities tomorrow, much like underfunded infrastructure.
Reimbursement threshold
Setting primary-care reimbursement rates below cost fails to trigger widespread physician migration to specialization unless the disparity crosses a financial viability threshold where clinical revenue no longer covers practice overhead in specific local markets. This bottleneck exists because physician career trajectories are locked in by training pathways and geographic practice commitments, meaning only early-career or financially leveraged providers respond to income signals—those already established in primary care often absorb losses to maintain community presence, particularly in federally qualified health centers or rural health clinics where exit would violate service mandates. The non-obvious insight is that the economic pressure must be severe and localized to disrupt equilibrium, as broader national rate differences alone do not generate sufficient momentum for systemic specialty drift.
Care coordination deficit
When primary-care reimbursement is set below cost, the resulting depletion of primary-care capacity creates a downstream degradation in longitudinal patient monitoring and referral gatekeeping, which in turn amplifies inappropriate specialist utilization for conditions better managed at the primary level, such as hypertension or diabetes. This mechanism operates through fragmented care ecosystems—like those in U.S. Medicaid programs with fee-for-service payment models—where absent care coordination, patients cycle through emergency departments and high-cost subspecialists, exacerbating disparities in marginalized populations. The significance lies in recognizing that the harm is not primarily physician career choice, but the systemic unraveling of preventive oversight that specialists are structurally disincentivized to provide.
Specialization feedback loop
Low primary-care reimbursement indirectly accelerates specialization by reinforcing medical education and health system investment incentives that favor procedural, high-revenue specialties, particularly in teaching hospitals dependent on clinical cross-subsidies where outpatient primary care losses are offset by operating room profits. This dynamic persists because academic medical centers—funded disproportionately through specialty-driven revenue streams—train residents in environments where primary care is undervalued both financially and hierarchically, shaping career preferences before physicians enter practice. The underappreciated consequence is that reimbursement policy distorts professional socialization, turning payment rates into a hidden curriculum that reproduces inequity by design rather than individual choice.
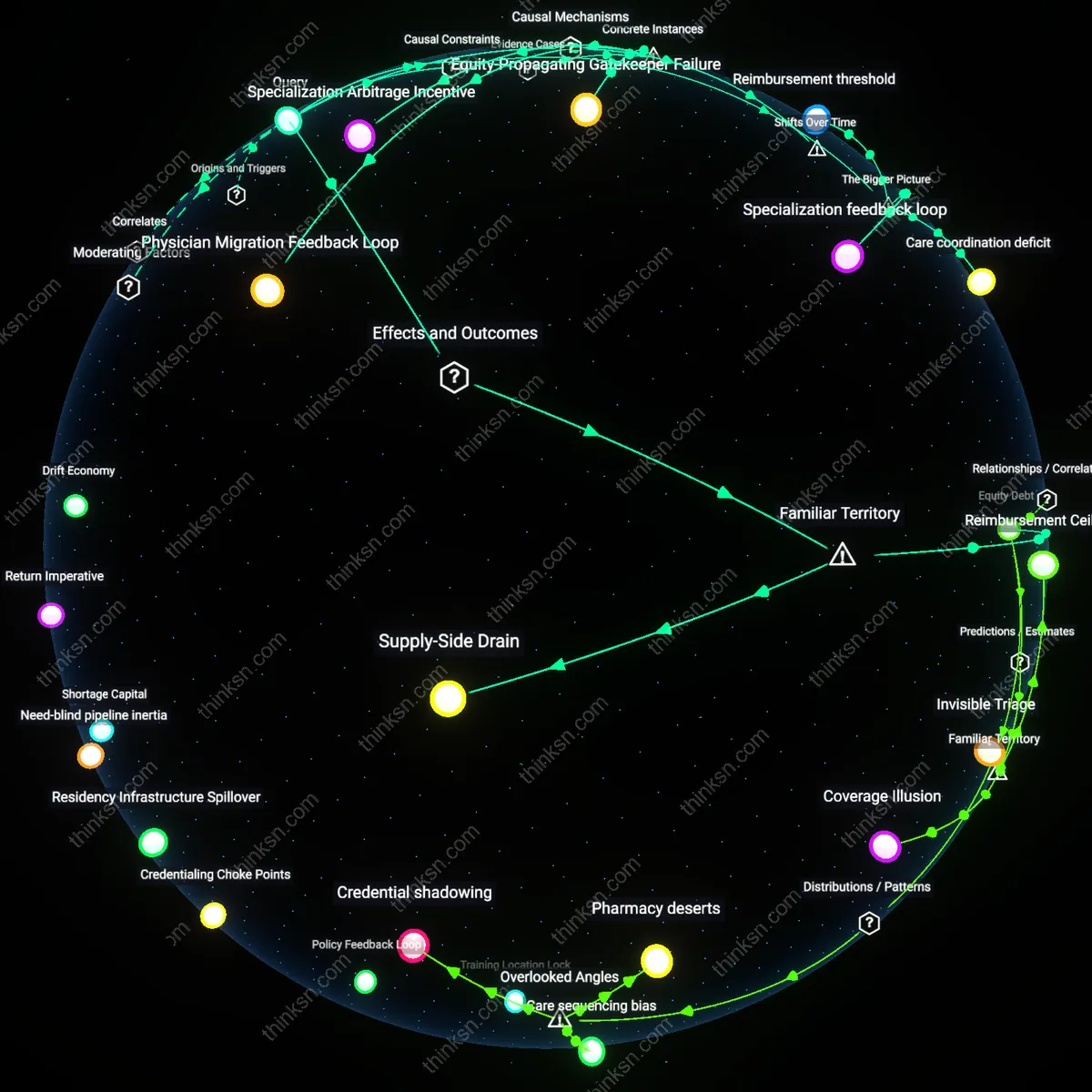
Physician Migration Feedback Loop
In rural Texas, primary-care physicians increasingly leave practice or transition to concierge models due to state reimbursement rates for Medicaid that are below 60% of Medicare levels, creating cascading shortages that force patients toward emergency departments or distant specialists, which in turn increases regional disparities in chronic disease management. The mechanism arises not from individual physician preference but from systemic underfunding embedded in Texas’ Medicaid fee schedule, which sets primary-care payments lower than the cost of delivering services, thereby making generalist practice financially unsustainable. This case reveals that underfunding operates not only as a deterrent to entry but as an active expulsion force—pushing existing providers out and removing local access points that are difficult to replace, a dynamic often masked by national workforce counts.
Specialization Arbitrage Incentive
Within the Veterans Health Administration, evidence indicates a structural shift in career trajectories among new medical graduates, who disproportionately pursue specialty fellowships after experiencing the flat reimbursement model for general internal medicine despite rising demand for primary care in veteran populations. The VHA pays similarly across primary care and subspecialty roles, but career mobility and perceived institutional prestige favor specialization, particularly when combined with bonus incentives tied to procedural volume. This instance exposes how even publicly funded systems, when failing to differentially reward cognitive labor and complex continuity care, generate internal labor markets where specialization functions as a rational economic response to stagnant compensation rather than clinical demand, effectively subsidizing upstream expertise at the cost of preventive capacity.
Equity-Propagating Gatekeeper Failure
In Detroit, where median household income is below $35,000 and over half of primary-care providers have opted out of Medicaid due to persistently low reimbursement from Michigan’s fee-for-service program, the nearest available primary-care appointment can take over six months to secure—pushing patients toward acute-care settings or no care at all. The withdrawal of providers from safety-net payer participation creates a localized collapse in gatekeeping function, disproportionately affecting Black and low-income residents who rely on public insurance. This breakdown demonstrates that inadequate reimbursement does not merely reduce provider supply but actively deconstructs the referral hierarchy necessary for equitable health navigation, transforming financial policy into a spatial and racial access barrier.