How Policy Can House Homeless Veterans Without Bureaucratic Walls?
Analysis reveals 9 key thematic connections.
Key Findings
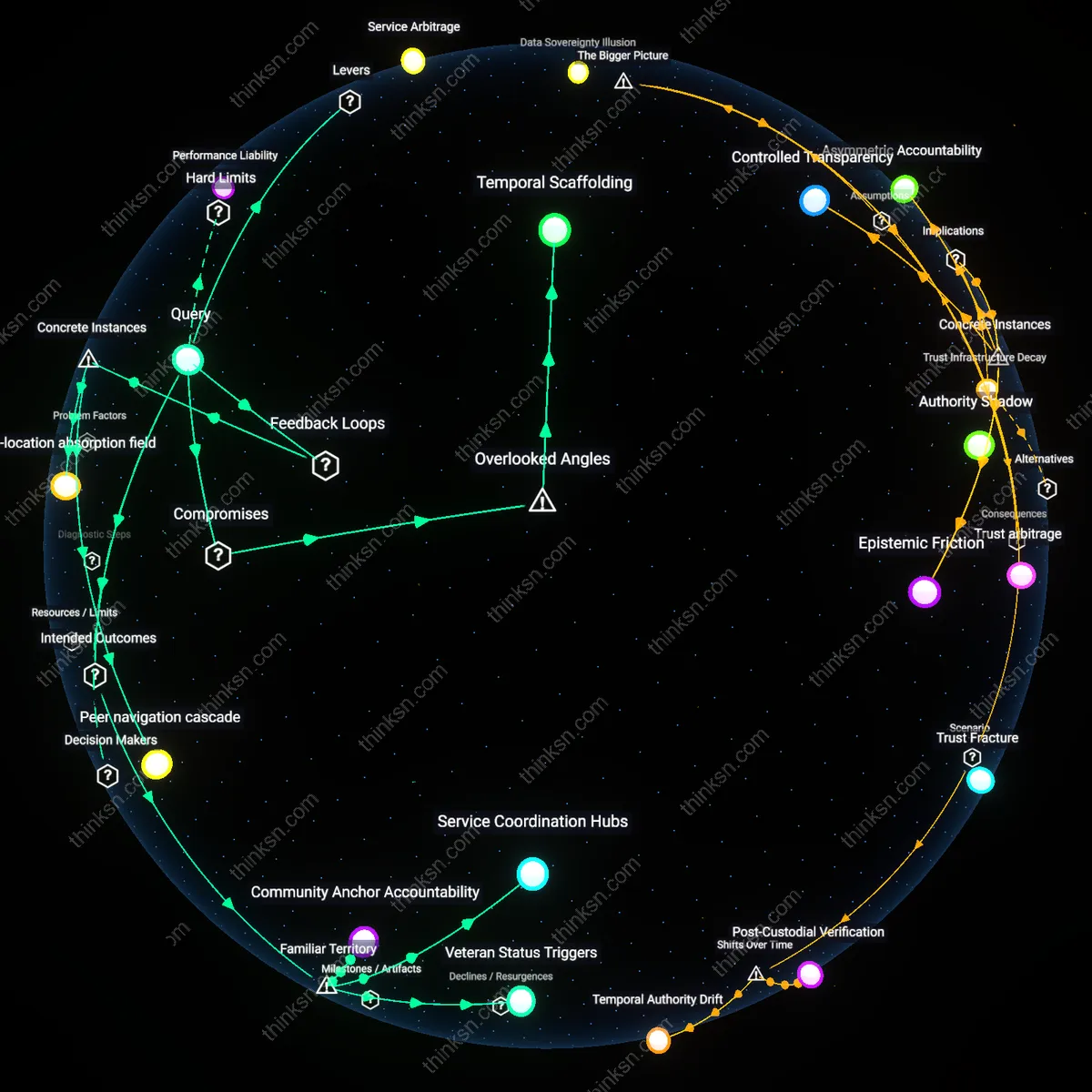
Data Sovereignty
Mandate veterans to control access to their own health and housing records across agencies, forcing integration through individual consent rather than interdepartmental agreements. When veterans, not bureaucracies, gatekeep data flow, agencies must align services to earn access, flipping the power from institutional silos to service recipients. This leverages informed consent as a binding operational constraint—non-compliance risks legal and reputational penalties—making interoperability a condition of care rather than a negotiation. The non-obvious insight is that fragmentation persists not from technical incompatibility but from agencies hoarding data as power; giving control to veterans disrupts this hidden incentive structure.
Performance Liability
Hold senior executives of VA, HUD, and DOD financially accountable for veteran homelessness recurrence within one year of service discharge, using clawback mechanisms on bonuses or base pay. By tethering leadership compensation to longitudinal outcomes—not service volume or process metrics—the incentive shifts from program fidelity to actual resolution of homelessness. This operates through existing payroll and performance review systems, bypassing interagency councils that dilute responsibility. Contrary to the dominant belief that coordination failures require more collaboration infrastructure, this reveals that fragmentation thrives in the absence of personal consequence for failure, even when solutions are known.
Service Arbitrage
Create a voucher system that allows veterans with PTSD-related homelessness to redeem federal benefits as portable credits at accredited nonprofit, private, or mutual-aid providers, including peer-run housing collectives. This introduces competition and exit options, forcing VA-affiliated facilities to integrate mental health and housing support or lose funding. Unlike top-down mandates, market-like pressure induces integration where it improves retention and effectiveness. This challenges the intuitive view that integrated services must be centrally designed, exposing that bureaucratic fragmentation endures because monopolized systems face no consequence for poor user experience.
Peer navigation cascade
Embedding trained veteran peers as navigators within integrated care teams, as piloted in the Veterans Integration to Community Living (VICL) initiative in Portland, Oregon, generates a reinforcing feedback loop where trust built through shared identity enables earlier identification of housing and mental health crises, accelerating referrals and reducing duplication across VA, HUD, and nonprofit providers. These peer navigators operate as human circuitry bridging bureaucratic silos, using experiential knowledge to guide system-avoidant veterans into care, which in turn increases program efficacy and justifies further interagency funding alignment. The underappreciated mechanism in this instance is that social similarity functions as a systems-level lubricant—one that propagates coordination not through policy mandates but through relational momentum, creating a cascade of integration downstream from initial contact.
Co-location absorption field
Co-locating VA mental health clinicians within nonprofit homeless shelters, as implemented at The Mission Continues in San Diego, creates a balancing feedback loop that resists bureaucratic drift by physically anchoring clinical services within community-based housing ecosystems, making service integration unavoidable rather than aspirational. This spatial integration forces iterative daily coordination between clinicians, case managers, and shelter staff, normalizing joint problem-solving and enabling real-time adjustments to treatment and housing plans, which increases veteran retention in care. The overlooked consequence of this arrangement is that proximity generates an absorption field—where organizational boundaries soften not through formal agreements but through repeated operational interdependence—revealing that geographic integration can function as a silent governance mechanism that sustains integration when policy churn threatens fragmentation.
Temporal Scaffolding
Policymakers must align the clock speeds of clinical care and housing placement by creating time-locked service corridors that force synchronization between VA mental health units and HUD-VASH coordinators. Clinical workflows operate in therapeutic time—iterative, nonlinear, and paced by patient readiness—while housing placement runs on administrative time—linear, deadline-driven, and constrained by lease cycles; when these temporal logics clash, veterans fall through the cracks not due to lack of resources but misaligned rhythms. By embedding time-bound but adjustable waypoints that require joint sign-off from clinical and housing teams, the system forces coordination at critical junctures, rendering otherwise invisible temporal incompatibilities visible and actionable. This reveals that bureaucratic fragmentation is not only about siloed agencies but about unacknowledged temporal dissonance, a hidden dependency rarely considered in service integration efforts.
Service Coordination Hubs
Co-locate VA healthcare providers, HUD housing specialists, and VSO advocates in urban triage centers to jointly assign cases. This integration forces shared accountability through colocation and routine cross-agency case review, replacing serial referrals with concurrent planning, which interrupts the usual drift between diagnosis and housing placement. While the public assumes 'integration' means better data sharing, the deeper failure is spatial and temporal disjunction—this redesign targets proximity and timing as active mechanisms, not just coordination rhetoric.
Veteran Status Triggers
Automatically enroll any veteran diagnosed with PTSD and identified as unstably housed into a federal support cascade covering housing vouchers, disability filing, and mental health triage. This trigger bypasses bureaucratic opt-in processes by treating service-connected PTSD as presumptive cause for integrated support, syncing eligibility across agencies at the moment of clinical determination. Most assume fragmented services stem from poor interagency communication, but the core issue is delayed activation—this shifts the system from reactive eligibility checks to automatic entitlement upon diagnosis.
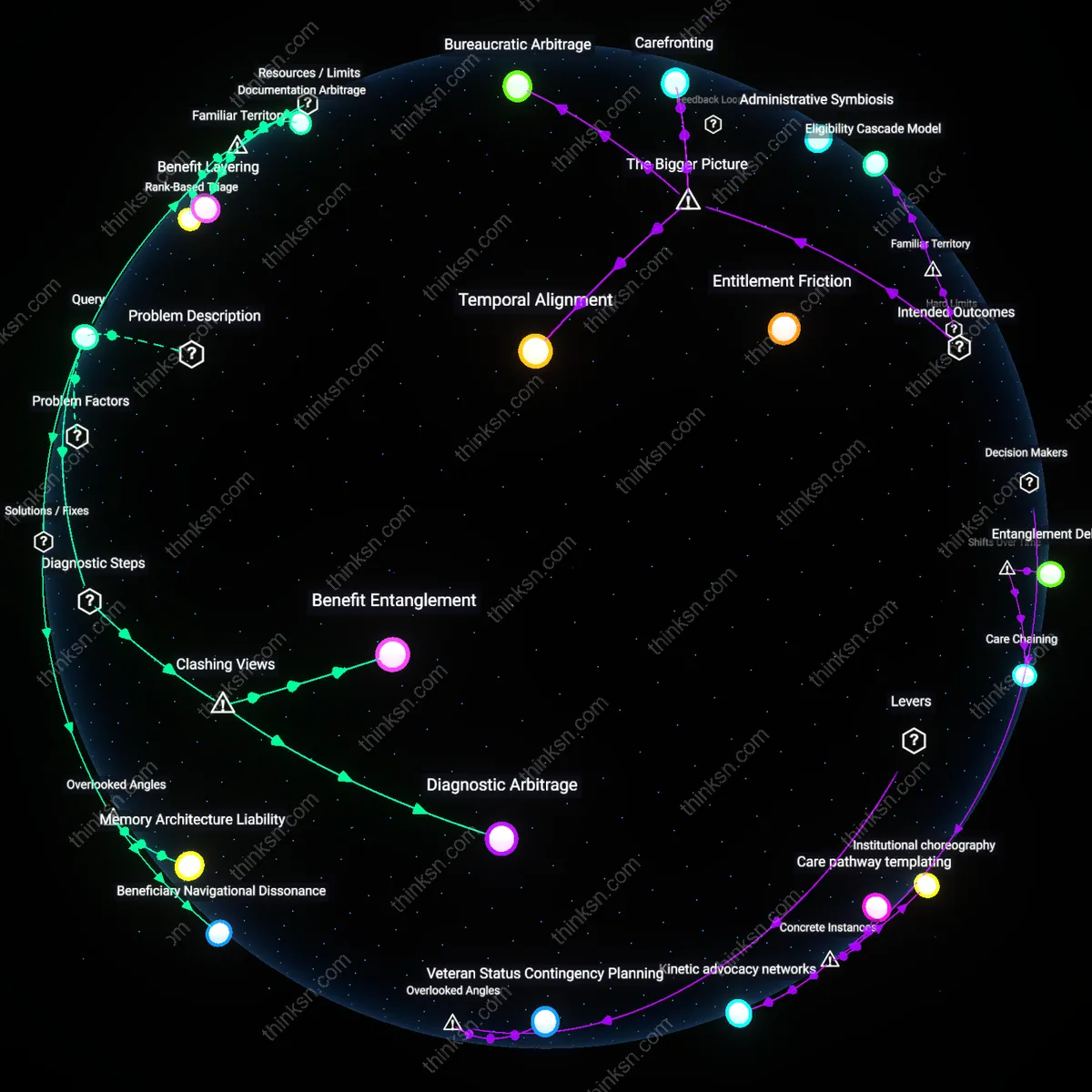
Community Anchor Accountability
Designate municipal homeless service centers as legally accountable partners in VA performance metrics for veteran housing stability, tying federal funding to local outcomes. This creates mutual dependency between distant federal agencies and hyperlocal providers, aligning incentives through shared consequences for failure. While public discourse frames veteran homelessness as a 'federal responsibility,' this approach leverages municipal institutions as enforcers of integration, transforming them from passive recipients to co-owners of veteran outcomes.