Does Ex-Ante Underwriting Favor Some Over Others in Health Insurance?
Analysis reveals 7 key thematic connections.
Key Findings
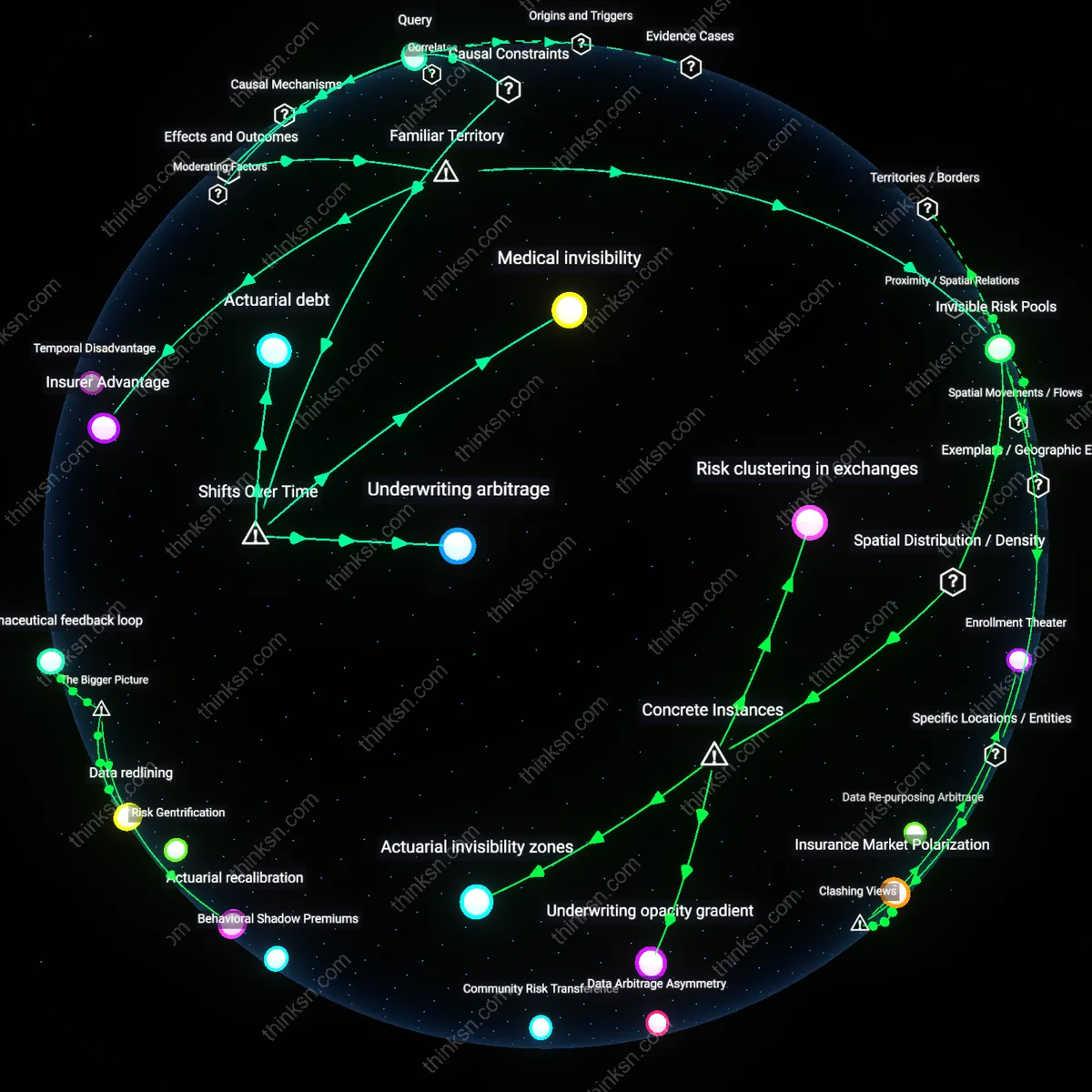
Insurer Advantage
Insurers benefit most directly from ex-ante underwriting because they gain early control over risk selection before medical claims emerge. This mechanism operates through actuarial screening protocols applied at enrollment, typically by leveraging demographic proxies and pre-existing condition flags in intake forms, which allows carriers to minimize adverse selection before coverage begins. The non-obvious reality beneath this familiar risk-selection narrative is that the greatest efficiency gain isn’t in pricing accuracy but in reducing administrative friction—processing applications without waiting for claims histories that haven’t yet materialized.
Invisible Risk Pools
Consumers with limited medical histories benefit secondarily because they gain access to baseline pricing unaffected by personal claims data, even if underwriting still uses group-level risk indicators like age or geography. This occurs through structured risk-pooling systems where minimal data forces reliance on broad actuarial categories, temporarily shielding low-information applicants from individualized penalties. What remains underappreciated in popular discourse is that this invisibility—being statistically ‘light’—can be a protective feature, not just a data gap, allowing short-term entry into coverage despite long-term uncertainty.
Temporal Disadvantage
Consumers with limited medical histories are systematically disadvantaged in ex-ante underwriting systems because insurers default to risk proxies such as age, gender, or lifestyle markers in the absence of longitudinal health data, which shifts actuarial risk onto demographically predictable but medically unverified traits. Insurers rely on population-level actuarial tables to fill data gaps, disproportionately penalizing younger or first-time applicants from marginalized backgrounds who lack archived health records, even if they are low-risk. This creates a paradox where risk mitigation mechanisms amplify inequity—precisely because the system is designed to reduce uncertainty, yet ends up depending on crude generalizations when individual-level data are absent, revealing how temporal gaps in data become structural liabilities for specific consumer groups.
Underwriting Arbitrage
Reinsurers and capital markets benefit from ex-ante underwriting because standardized risk classification enables the aggregation and securitization of insurance portfolios, turning asymmetric health risk assessments into tradable financial instruments. Primary insurers, under pressure to maintain profitability and balance sheet stability, offload concentrated risks to reinsurance entities that depend on clear actuarial distinctions to price coverage layers and manage exposure—especially in markets where health data are incomplete. This creates an incentive to codify underwriting rules that favor predictability over precision, subtly aligning the interests of large insurers and financial players in sustaining systems that extract value from risk stratification, even at the expense of consumers whose sparse medical histories increase valuation uncertainty and therefore transfer costs.
Actuarial debt
Insurers benefit from ex-ante underwriting because it allows them to price risk before exposure, a shift that became decisive after the 1980s healthcare deregulation in the U.S., when medical loss ratios were loosened and risk selection was institutionalized; this mechanism relies on the bottleneck of historical claims data, which excludes younger or healthier consumers with limited medical histories, making their coverage more costly or inaccessible despite lower actual risk—revealing how the temporal shift toward financialized insurance models has produced actuarial debt, where the system owes fair pricing to those it systematically misjudges.
Medical invisibility
Consumers with limited medical histories are harmed by ex-ante underwriting because the absence of data triggers default risk classifications, a dynamic that intensified after the 2000s, when predictive modeling replaced physician-mediated risk assessment; this causal chain depends on the bottleneck of documented medical continuity, which failed to adapt when young and low-income populations entered high-deductible plans post-ACA, exposing how the shift toward algorithmic underwriting has rendered short histories as suspicious, producing medical invisibility, where clean records are interpreted as incomplete rather than low-risk.
Underwriting arbitrage
Reinsurance markets benefit from ex-ante underwriting because primary insurers offload unpredictable risks only after initial screenings, a practice that expanded after the 2008 financial crisis, when capital adequacy rules forced insurers to optimize balance sheets through front-loaded risk rejection; this mechanism functions only if the bottleneck of regulatory lag allows insurers to classify conditions as preexisting, enabling denial before pooling—highlighting how the shift toward risk-layering in global reinsurance has created underwriting arbitrage, where value is extracted not from coverage but from exclusion timing.