Do Health Quotas Benefit Doctors or Patients?
Analysis reveals 10 key thematic connections.
Key Findings
Diagnostic dilution
Tying physician compensation to screening quotas systematically lowers the threshold for recommending diagnostic procedures to patients who are asymptomatic or at negligible risk, particularly in publicly funded systems like the UK’s NHS where targets influence performance reviews. This dynamic shifts clinical judgment from individual risk assessment to population-level metrics, increasing false positives and downstream invasive interventions that expose patients to harm without meaningful benefit. The overlooked consequence is not just overdiagnosis but the erosion of diagnostic specificity—where the meaning of a 'positive' screening result weakens across the system, undermining the reliability of the entire testing cascade. This transforms screening from prevention into a form of low-level systemic recklessness masked as diligence.
Compliance theater
In U.S. Medicaid managed care organizations, where health policy incentivizes screening completion rates as a measure of quality, clinics often respond by prioritizing documentation and referral compliance over actual patient engagement or understanding. This creates a performance ritual—clinicians recommend screenings in ways guaranteed to be ignored or abandoned, such as referring patients to distant facilities without transportation support—fulfilling the letter of the policy while nullifying its intent. The non-obvious cost is not just wasted resources but the normalization of symbolic medical acts, where recommendation becomes a bureaucratic gesture rather than a therapeutic one, corroding trust and reinforcing patient perceptions of medicine as performative rather than personal.
Prevention displacement
When public health systems in mid-income countries like Colombia tie funding to cancer screening quotas, primary care providers reallocate time and infrastructure away from chronic disease management and vaccine outreach to meet narrowly defined prevention metrics. This shifts the meaning of 'prevention' from a broad public health ethic to a targeted bureaucratic output, reducing clinic capacity for conditions like diabetes and hypertension that affect more people at greater daily risk. The hidden dependency is that prevention policies can cannibalize prevention itself—by elevating one measurable form of early intervention, they degrade less quantifiable but more impactful forms of primary care, with the greatest burden falling on patients with multimorbidity who rely on integrated services.
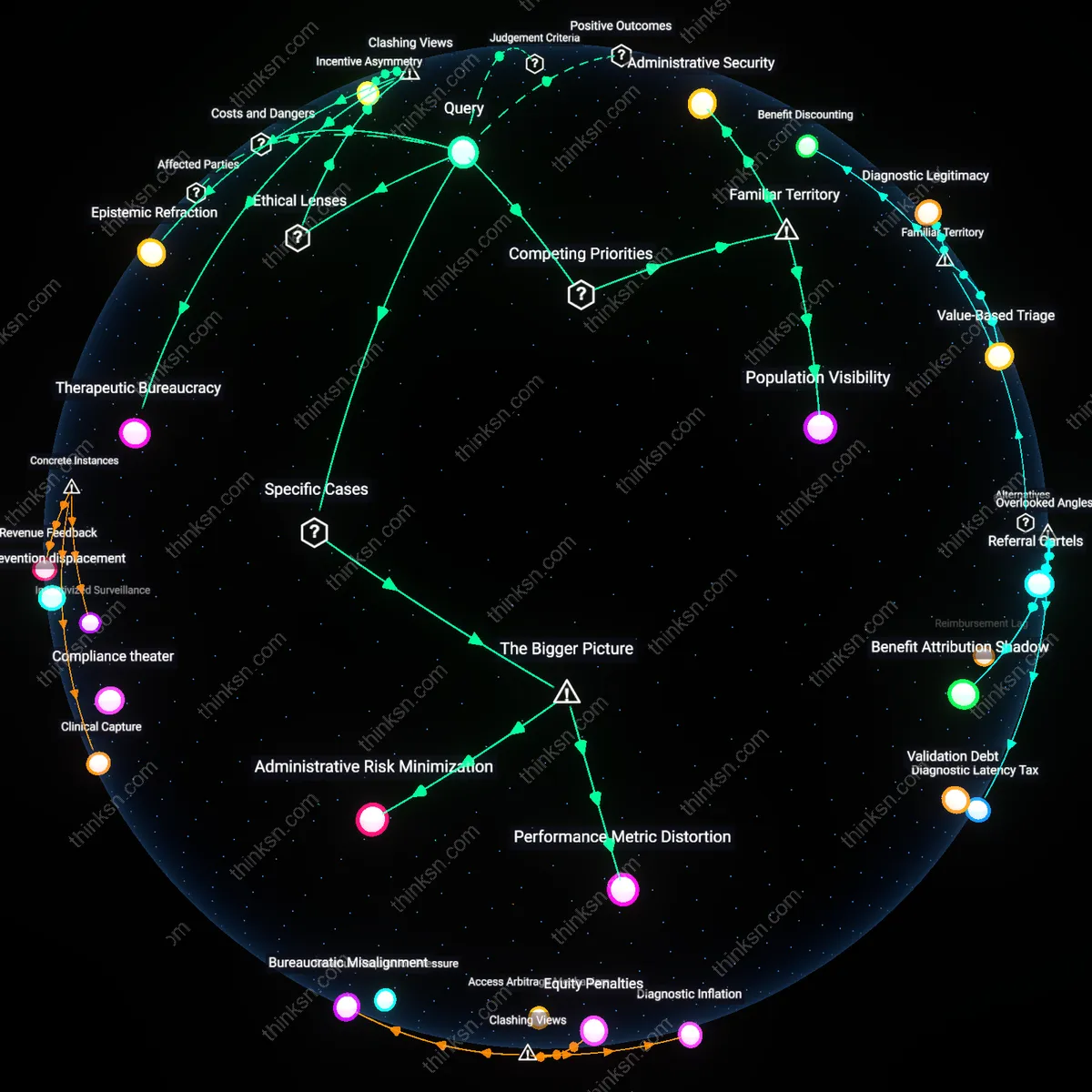
Administrative Security
When health systems prioritize screening quotas, they trade clinical discretion for institutional accountability, giving administrators and policymakers a sense of control over population health outcomes. Metrics like screening rates generate clean, auditable data that satisfy political demands for transparency and action, especially in publicly scrutinized systems such as those governed by the Affordable Care Act’s quality reporting mandates. But this security comes at the cost of eroding trust in physician judgment—what feels like oversight to administrators registers as interference to clinicians. The underappreciated effect is that the system begins to validate visible activity over meaningful outcomes, rewarding the appearance of diligence rather than its actual impact.
Population Visibility
Screening quotas increase the visibility of marginalized or hard-to-reach populations within health data infrastructures, making them legible to state monitoring and resource allocation mechanisms. In urban public health districts and rural safety-net clinics, capturing underserved patients through mandated screenings pulls them into formal care networks—not necessarily because they receive timely interventions, but because their bodies now generate reportable data. This benefits policymakers and funding agencies seeking evidence of equity efforts, while patients may experience coerced inclusion without corresponding increases in care quality. The rarely acknowledged trade is that visibility does not equate to empowerment; being counted can become a substitute for being cared for.
Therapeutic Bureaucracy
Health policies that tie physician compensation to screening quotas transform medical judgment into administrative compliance, privileging volume over clinical nuance; this occurs through Medicare's Merit-Based Incentive Payment System (MIPS) and similar value-based purchasing programs, which embed actuarial benchmarks into reimbursement, effectively outsourcing ethical prioritization to regulatory metrics. The mechanism—performance targets converted into financial incentives—recasts physicians as agents of public health administration rather than fiduciaries, shifting the moral locus from patient-specific care to population-level efficiency. Contrary to the intuition that such policies empower prevention, they systemically advantage institutions with robust data-tracking infrastructure, often at the expense of small practices and marginalized patients whose conditions resist metricization—revealing that the policy's ethical framework aligns with utilitarian statecraft, not medical ethics.
Epistemic Refraction
Screening quotas distort physician recommendations not through coercion but by altering the epistemic conditions under which clinical decisions appear rational, a process institutionalized in Medicaid’s preventive care mandates and HEDIS performance measures that redefine 'appropriate' care as quantifiably delivered services. Physicians, operating under time and documentation constraints, begin to see adherence to quotas as clinical diligence itself, refracting their perception of patient need through the lens of reportable outcomes. This undermines the Kantian principle of treating patients as ends, instead positioning them as conduits for performance data—what appears as increased screening activity is often a reconfiguration of medical attention, where the visibly measurable crowds out the contextually urgent. The policy thus benefits health systems that capitalize on risk adjustment and coding density, exposing a concealed transfer of epistemic authority from clinician to auditor.
Incentive Asymmetry
When health policies incentivize screening quotas, they create a structural bias toward overtesting among safety-net providers serving low-income populations, as seen in urban federally qualified health centers pressured to meet HRSA Uniform Data System benchmarks to retain federal funding. These clinics, serving patients with complex social needs, allocate scarce clinical time to screenings that are easily documented and reimbursed, even when clinically marginal, because the cost of non-compliance exceeds the benefit of individualized care. This dynamic, rooted in managerial neoliberalism that treats healthcare as a contractible output, advantages well-resourced providers who can stratify and game metrics, while the intended beneficiaries—underserved patients—receive more tests but less holistic care. Evidence indicates that such systems increase detection of indolent pathologies without reducing mortality, revealing that the primary beneficiaries are not patients but the policy infrastructure itself, which uses apparent compliance to legitimize its expansion.
Performance Metric Distortion
Health policies that tie physician compensation to screening quotas directly alter clinical recommendations by aligning provider incentives with measurable output rather than individual patient need, particularly visible in the UK's National Health Service General Practitioner Contract, where GPs face formal targets for cancer and cardiovascular screenings. The systemic integration of these quotas into performance reviews and funding allocations creates institutional pressure to prioritize quota fulfillment, even when clinical judgment might defer screening; this shifts medical decision-making from personalized risk assessment to population-level compliance. The non-obvious consequence is that the very metrics designed to improve preventive care can erode clinical autonomy and distort patient-doctor communication, privileging measurable activity over medical appropriateness.
Administrative Risk Minimization
In the U.S. Medicare Advantage program, insurers receive higher reimbursements for patients who undergo mandated screenings, which incentivizes health maintenance organizations like Kaiser Permanente and UnitedHealthcare to implement system-wide alerts and physician dashboards that promote screening adherence. Physicians operate within IT systems that flag missed screenings as performance deficiencies, creating a bureaucratic environment where avoiding audit triggers becomes as consequential as clinical outcomes. This reveals how downstream payment structures reshape front-line decisions not through direct orders but through ambient administrative surveillance, a dynamic often overlooked in debates focused on individual physician behavior rather than embedded digital governance.