Experimental Cancer Treatments: Why Insurers Deny Coverage Despite Proof?
Analysis reveals 7 key thematic connections.
Key Findings
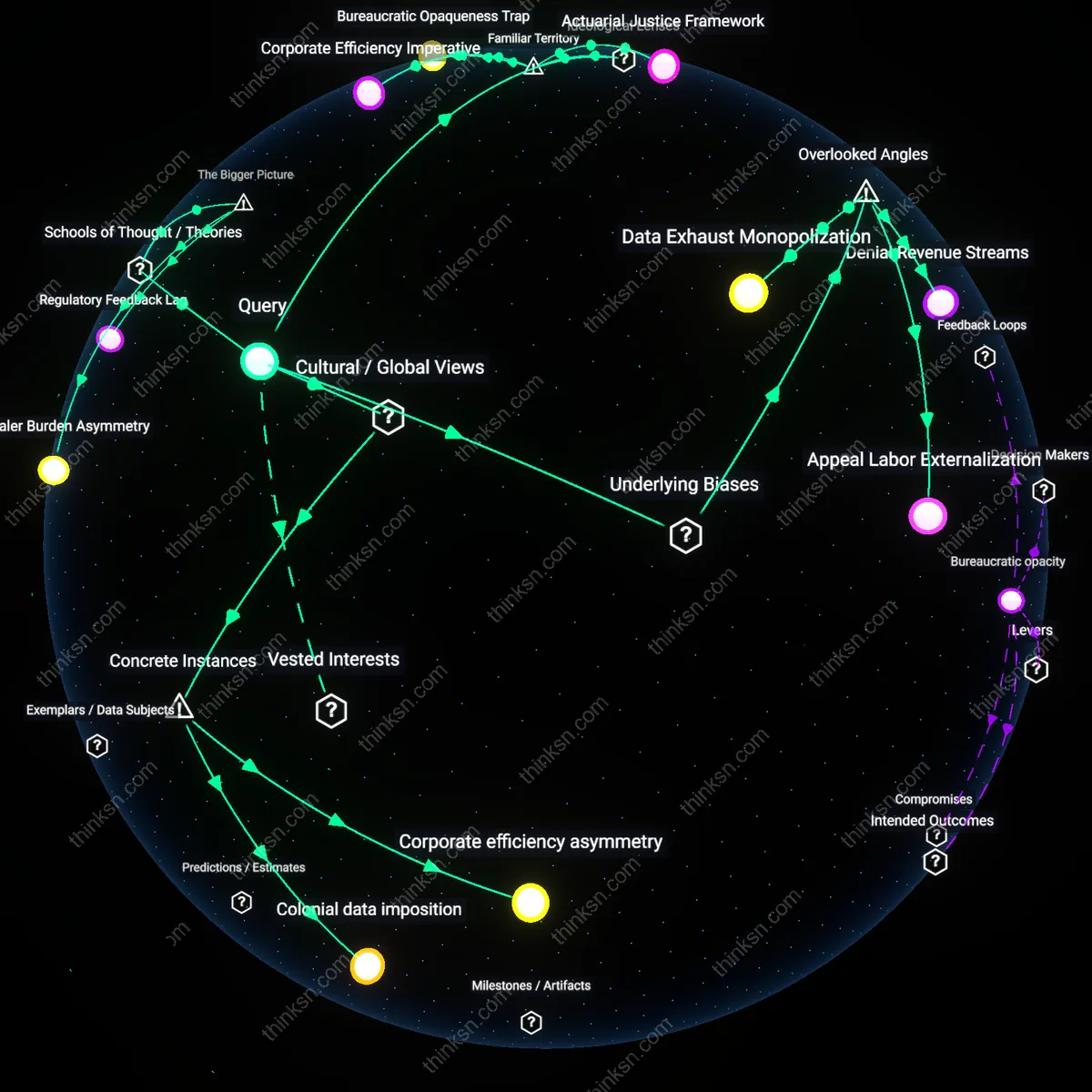
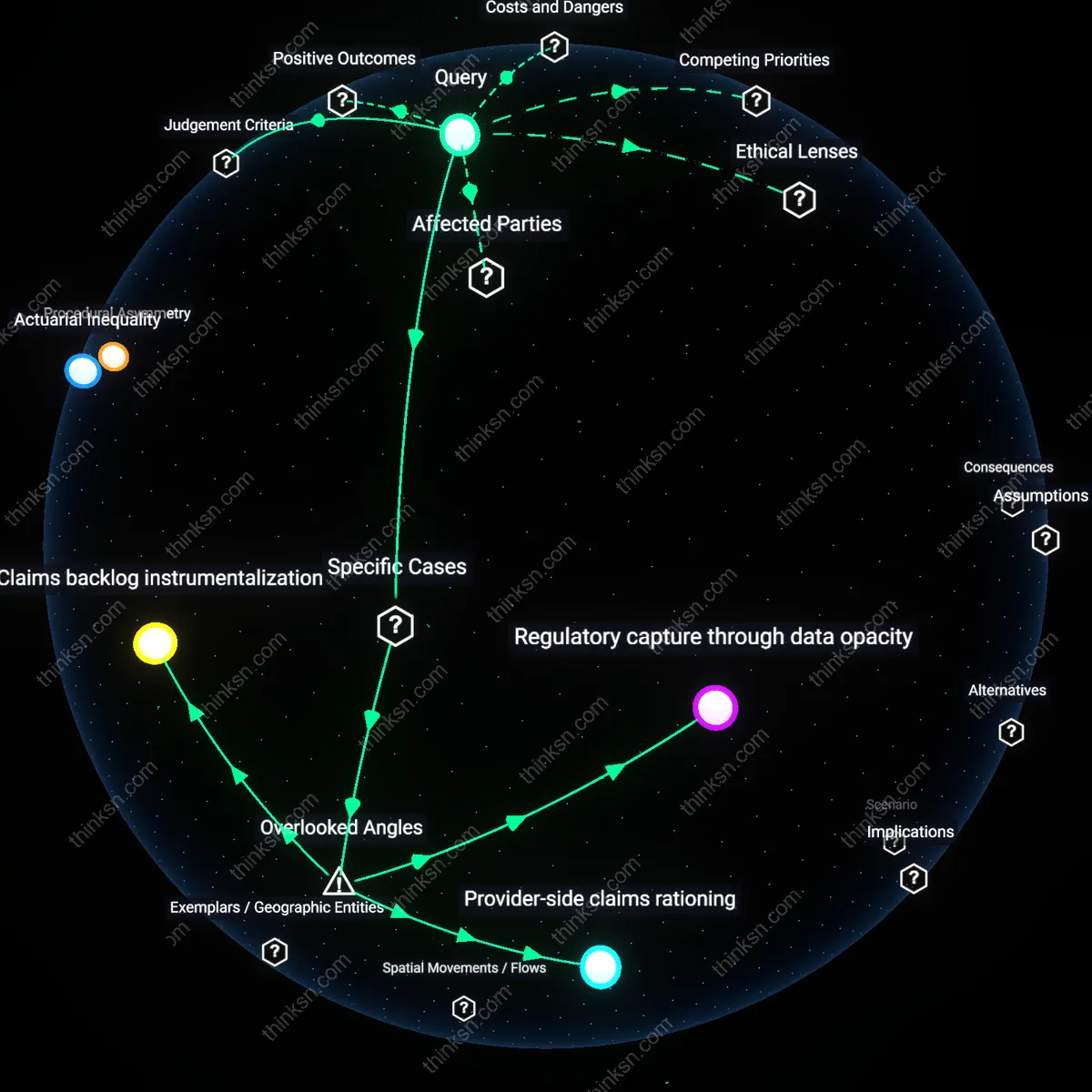
Regulatory Arbitrage
Insurers deny experimental cancer treatments because FDA approval serves as a gatekeeper for coverage, and many published studies—despite appearing in peer-reviewed journals—lack the phase III trial validation required by both regulators and payers. This creates a loophole where scientifically plausible interventions are excluded not due to absence of evidence, but because the evidence doesn’t match the regulatory format insurers legally rely on. The non-obvious insight is that insurers aren’t rejecting science per se, but outsourcing coverage decisions to a regulatory framework that prioritizes statistical certainty over clinical innovation, enabling them to avoid liability while maintaining cost control.
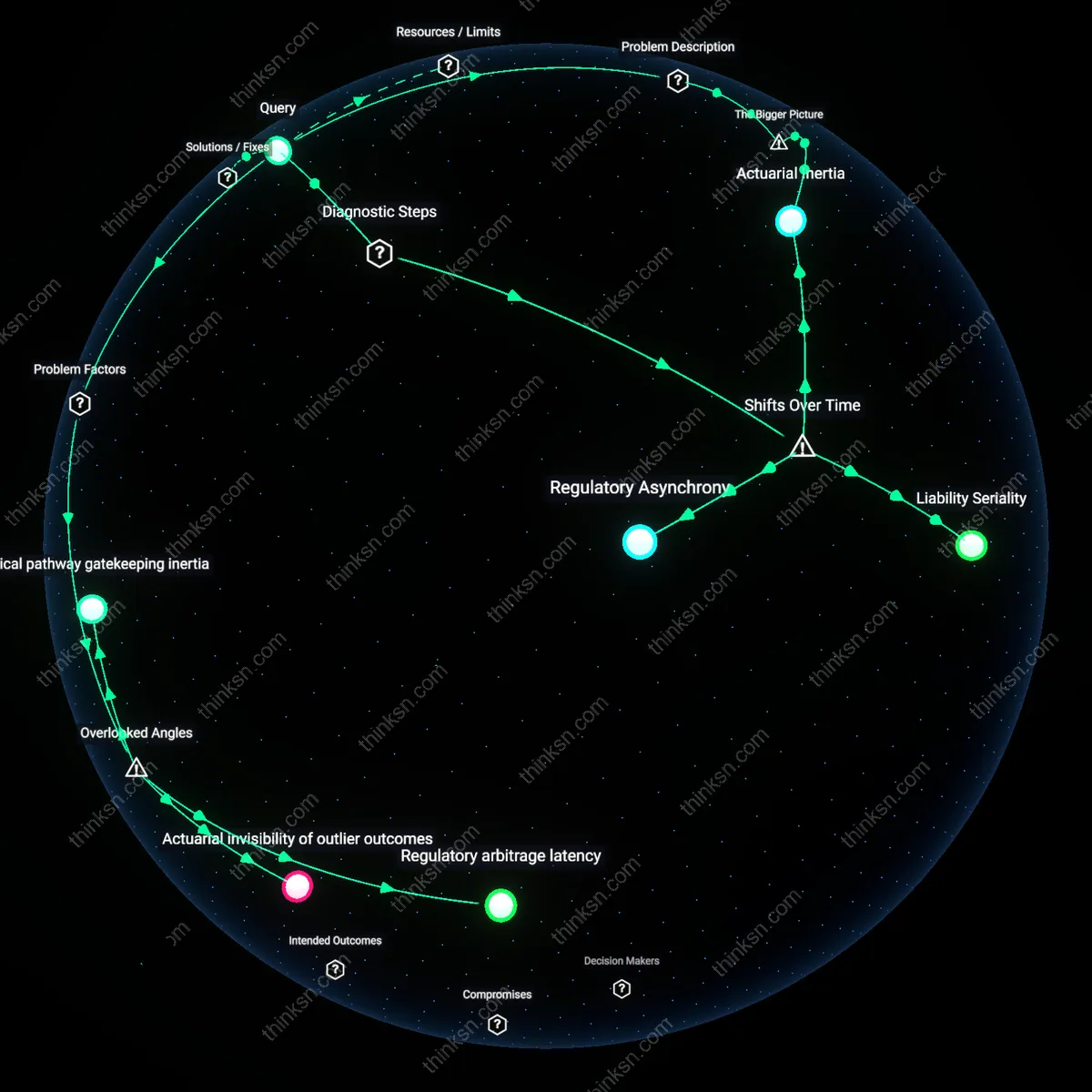
Actuarial Inertia
Insurance underwriting models are built on population-level risk pooling and historical claims data, making them structurally incapable of incorporating emerging scientific findings that haven’t yet translated into measurable utilization or outcomes trends. Even with published support, experimental treatments lack longitudinal data on complication rates, survival gains, or downstream costs—metrics essential for recalibrating risk algorithms. This reveals that the core incentive structure of private insurance rewards predictability over adaptability, where coverage decisions are delayed not by malice but by systemic slowness to update actuarial assumptions in the face of scientific novelty.
Regulatory arbitrage latency
Insurers delay coverage for experimental cancer treatments because regulatory agencies classify them as investigational until post-market surveillance data accumulates, creating a window where scientifically supported therapies are deemed not medically necessary—despite peer-reviewed evidence—due to rigid adherence to FDA approval status as a proxy for clinical validity. This mechanism privileges legal risk mitigation over medical innovation, embedding a structural lag between scientific discovery and reimbursement eligibility that disproportionately affects late-phase trial therapies with strong but not yet 'definitive' data. The overlooked dimension is not insurer resistance per se, but the silent coordination between private payers and federal regulatory milestones, which insulates insurers from accountability for denials during this arbitrage period, effectively outsourcing coverage logic to a slower, safety-optimized bureaucracy not designed for timely therapeutic access. This reveals how systemic incentives are shaped by inter-institutional deferral rather than clinical assessment.
Actuarial invisibility of outlier outcomes
Experimental cancer treatments are denied because actuarial models used by insurers systematically discount survival outliers—patients who respond exceptionally well to novel therapies—since risk pools depend on population-level predictability, not individual exceptionalism, and current models cannot incorporate sparse, high-variance response data without destabilizing premium calculations. This creates a blind spot where therapies with low average efficacy but high value for molecularly defined subgroups appear economically unjustifiable, even when biomarker-guided studies demonstrate clear benefit in narrow populations. The underappreciated dynamic is that statistical rigor in oncology trials often produces results that are scientifically valid but actuarially 'noisy,' making them incompatible with insurance pricing frameworks designed for homogeneous risk distribution, thereby privileging treatments with modest but consistent results over potentially curative but unpredictable ones. This exposes a misalignment between biological complexity and financial modeling assumptions.
Clinical pathway gatekeeping inertia
Denials persist because institutional oncology networks adopt clinical pathways—standardized treatment algorithms—that are tightly coupled to payer reimbursement contracts, meaning hospitals risk financial penalties or reduced referrals if they deviate into experimental regimens, even when supported by recent literature. These pathways are typically updated annually and governed by joint committees dominated by community oncologists and health system administrators who prioritize operational feasibility over experimental adoption, creating a feedback loop where payer policies shape clinical guidelines that then justify those same policies. The overlooked factor is that scientific support alone cannot penetrate this closed loop without pathway endorsement, which requires consensus-building slow enough to lag behind emerging evidence—thus, the real bottleneck is not cost or risk but the institutional time lag in renegotiating care standards embedded in contractual agreements. This reveals how systemic incentives are locked in through administrative alignment, not medical judgment.
Regulatory Asynchrony
Insurers reject experimental cancer treatments despite published support because the 1996–2004 expansion of evidence-based medicine frameworks created a temporal disconnect between clinical research cycles and payer reimbursement cycles. This mechanism functions through FDA-approval–driven formularies adopted by private and public payers, which lock treatment coverage to fixed review intervals that lag behind real-time scientific publication, privileging bureaucratic alignment over scientific velocity. The shift from ad hoc coverage decisions to codified benefit designs around 2001 entrenched a structural delay, making approval faster than payment, revealing that systemic incentives reward procedural compliance more than therapeutic promise.
Liability Seriality
Denial of experimental cancer treatments emerged as a dominant insurer practice after the 1997–2002 wave of managed care litigation, when courts began treating coverage decisions as procedural rather than clinical, shifting accountability from medical judgment to contractual fulfillment. This dynamic operates through legal precedents that shield insurers from malpractice liability so long as they follow plan documents, creating an incentive to reject marginal innovations even with scientific backing, as defensible denials minimize legal exposure. The transition from physician-led to protocol-driven adjudication in the early 2000s revealed that systemic incentives prioritize risk containment through repetition, producing liability-avoidance as the default clinical logic.