Why Do Hospitals Stick to Fee-for-Service Despite Costly Consequences?
Analysis reveals 9 key thematic connections.
Key Findings
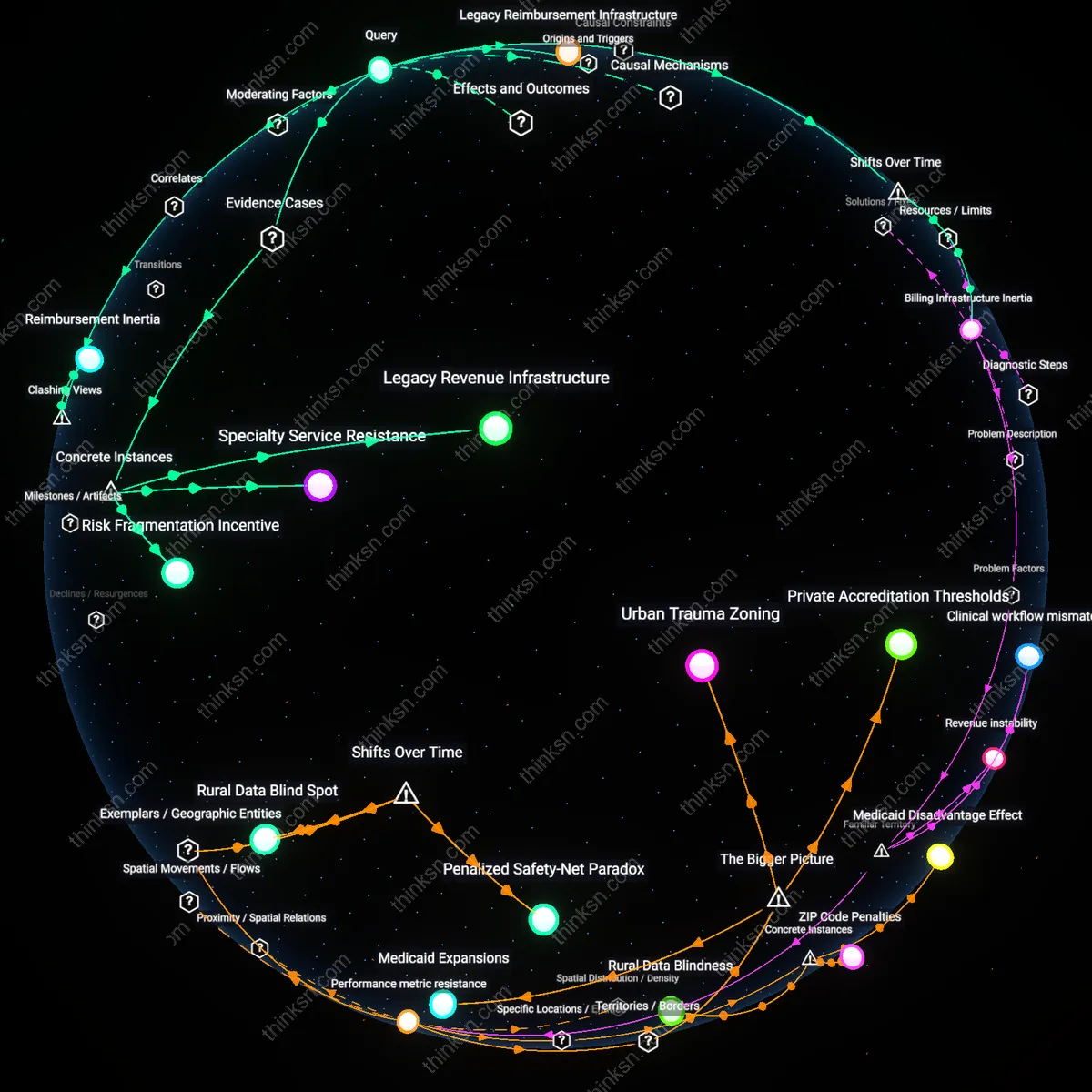
Legacy Reimbursement Infrastructure
The fee-for-service model persists because Medicare's historical establishment of volume-based reimbursement created an entrenched billing infrastructure that hospitals cannot economically abandon. Legacy systems—both technical and administrative—were calibrated to track discrete procedures rather than episodes of care, making the transition to bundled payments operationally disruptive and costly for providers, insurers, and billing vendors alike. The non-obvious insight is that the inertia stems not from preference, but from the sunk costs and interdependence of institutional workflows built over decades around transactional coding systems like CPT and ICD.
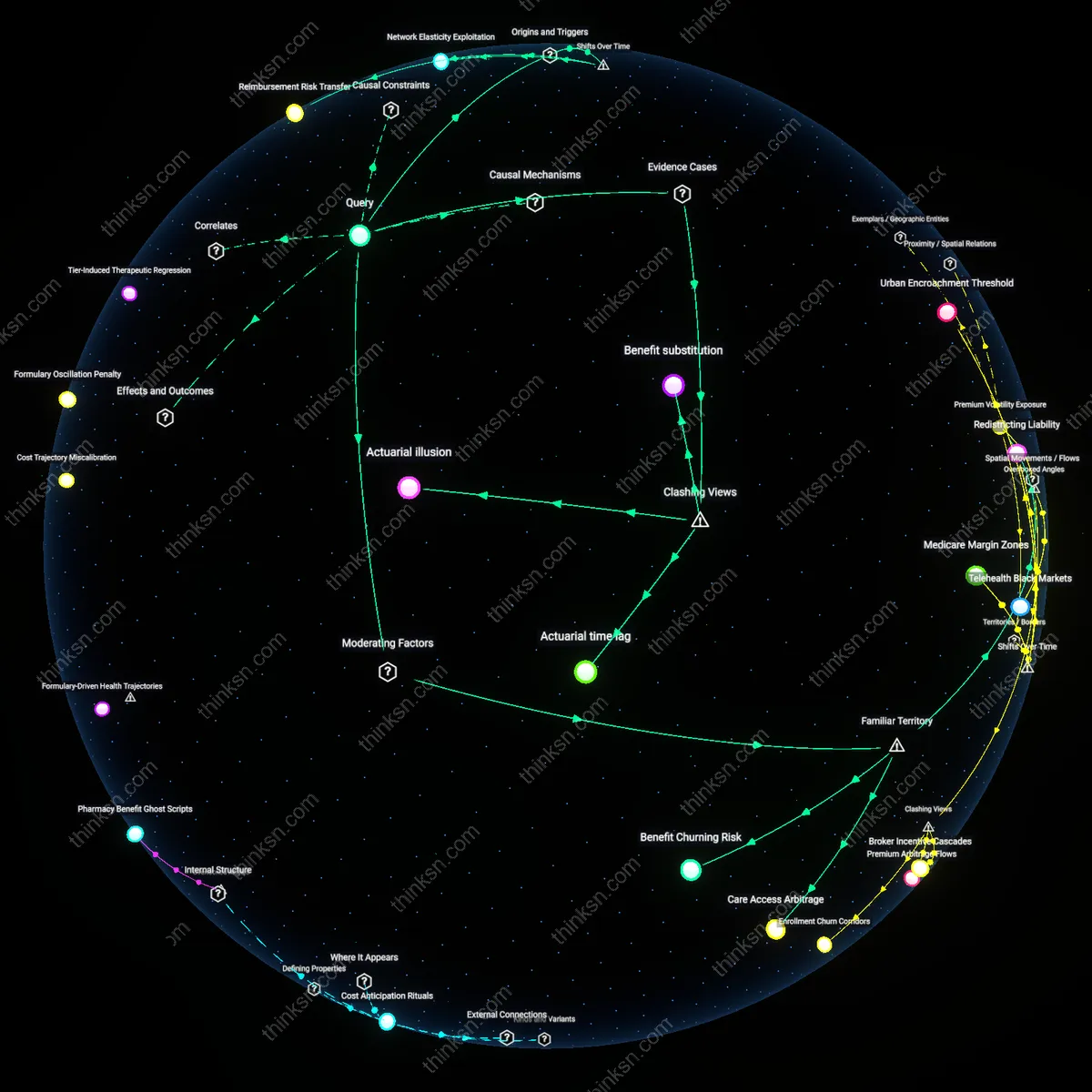
Fragmented Care Accountability
Hospitals continue relying on fee-for-service because the U.S. healthcare system distributes financial risk across disjointed actors—referral networks, specialists, post-acute providers—none of whom assume full accountability for episode-wide outcomes. Bundled payments require coordinated cost and quality management across these entities, but without contractual alignment or shared incentives, dominant players like hospitals default to maximizing revenue through billable units. This reveals that the true barrier is not payment design, but the lack of a unified risk-bearing entity capable of internalizing downstream consequences.
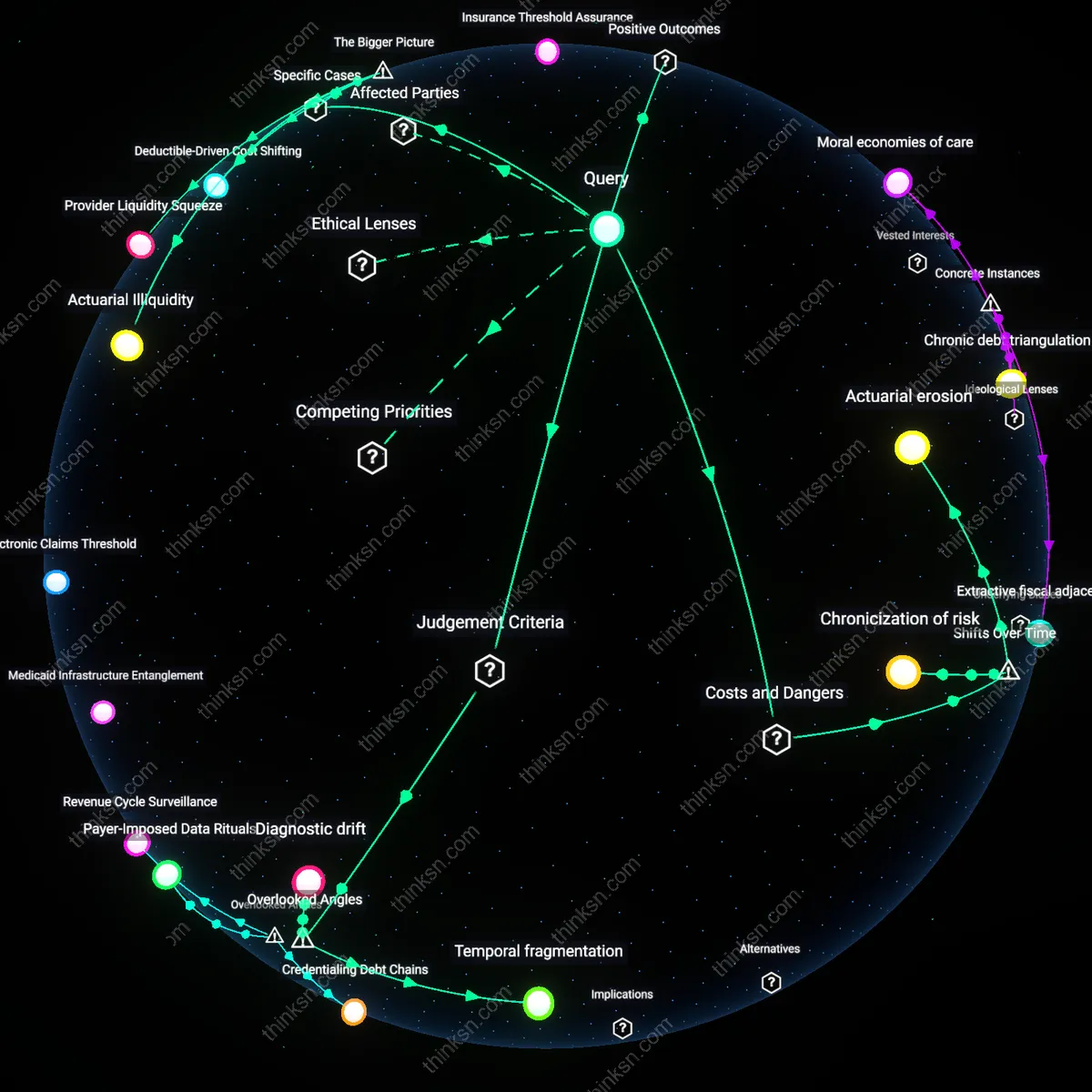
Regulatory Risk Aversion
Fee-for-service remains dominant because federal and state regulations have selectively enabled, but not mandated, bundled payment adoption, leaving hospitals exposed to financial downside without proportional upside assurances. Providers perceive bundled payments as risk-shifting mechanisms—especially under early mandatory pilots such as CMS's Bundled Payments for Care Improvement—sparking resistance rooted in budgetary uncertainty during periods of thin margins. The underappreciated dynamic is that regulatory half-measures have amplified provider risk aversion, making voluntary innovation unattractive even where evidence supports it.
Reimbursement Inertia
Hospitals maintain fee-for-service because legacy billing infrastructures at major health systems like HCA Healthcare and University of Pittsburgh Medical Center are too entrenched to displace, even when bundled payments reduce costs; converting would require overhauling coding protocols, renegotiating payer contracts, and retraining tens of thousands of billing staff—a coordination cost that outweighs potential savings. This reveals that organizational momentum, not clinical or economic logic, determines payment adoption, exposing how technical path dependency suppresses superior models even in evidence-rich environments.
Regulatory Asymmetry
Medicare’s Conditions of Participation still require line-item billing for federal audit compliance, forcing hospitals to retain fee-for-service as the legal baseline even when private payers offer bundled alternatives through initiatives like CMS’ Bundled Payments for Care Improvement. Because no parallel regulatory pathway legitimizes bundled accounting for oversight, hospitals cannot fully operationalize alternatives without dual-system redundancy, revealing that legal scaffolding—not market failure or resistance to innovation—preserves the status quo by making compliance costlier under reform.
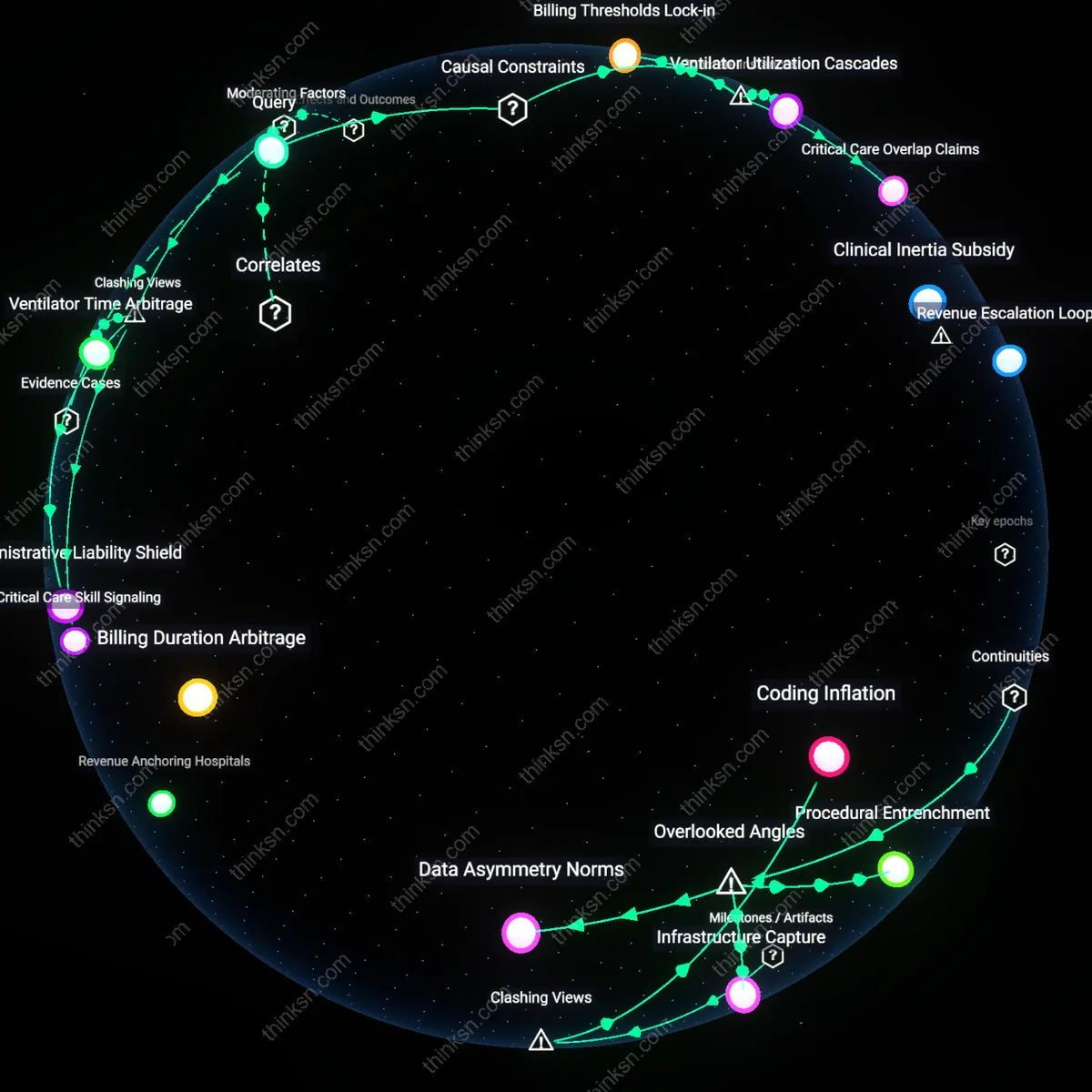
Billing Infrastructure Inertia
The fee-for-service model persists because hospital billing systems evolved over decades to standardize per-unit reimbursement, making large-scale systemic shifts to bundled payments operationally unviable without dismantling entrenched coding, auditing, and payer coordination mechanisms. Legacy IT systems, designed around CPT and ICD billing codes, are deeply embedded in finance and compliance workflows across U.S. hospitals since the 1980s expansion of private insurance and Medicare Part B, creating a technical and organizational bottleneck that predates and resists value-based reform experiments of the 2010s. This reveals how administrative path dependency—rather than clinical or economic logic—has become the central constraint on payment innovation, exposing a hidden infrastructural rigidity masked by policy discourse on outcomes.
Legacy Revenue Infrastructure
The U.S. Medicare program's persistent reliance on fee-for-service billing under Part B demonstrates that entrenched administrative systems favor familiar reimbursement pathways over innovation. Medicare processes over 1 billion fee-for-service claims annually through established systems like the National Claims History file, which hospitals, insurers, and fiscal intermediaries rely on for cash flow predictability; shifting to bundled payments would require overhauling core IT, auditing, and compliance architectures that have been reinforced for decades. This reveals how operational path dependence—not just financial incentives—anchors the healthcare system to fee-for-service, a constraint most acute in large public programs where system-wide coordination costs are prohibitive.
Specialty Service Resistance
At Massachusetts General Hospital, orthopedic surgery departments have selectively opted out of CMS Bundled Payments for Care Improvement (BPCI) initiatives despite favorable outcomes in pilot data, because high-volume joint replacements generate disproportionate revenue under per-procedure billing. Surgeons, anesthesia teams, and device vendors align around maximizing utilization, and bundled payments threaten to compress profits from implant markups and ancillary services; this microcosm reveals how clinically concentrated economic power can veto system-level reforms even when aggregate efficiency improves under alternative models.
Risk Fragmentation Incentive
In Florida’s for-profit hospital chains like HCA Healthcare, the retention of fee-for-service payments enables strategic risk offloading between providers and post-acute care facilities. By keeping payments episode-discrete, hospitals can discharge patients to skilled nursing facilities without bearing downstream complication costs—exploiting a loophole visible in Medicare data showing 20% higher readmission rates in BPCI-excluded markets. This demonstrates how fee-for-service supports a business model built on transactional risk avoidance rather than care integration, particularly where ownership structures incentivize volume over accountability.