How Medicare Advantage Shifts Costs to Patients Long-Term?
Analysis reveals 9 key thematic connections.
Key Findings
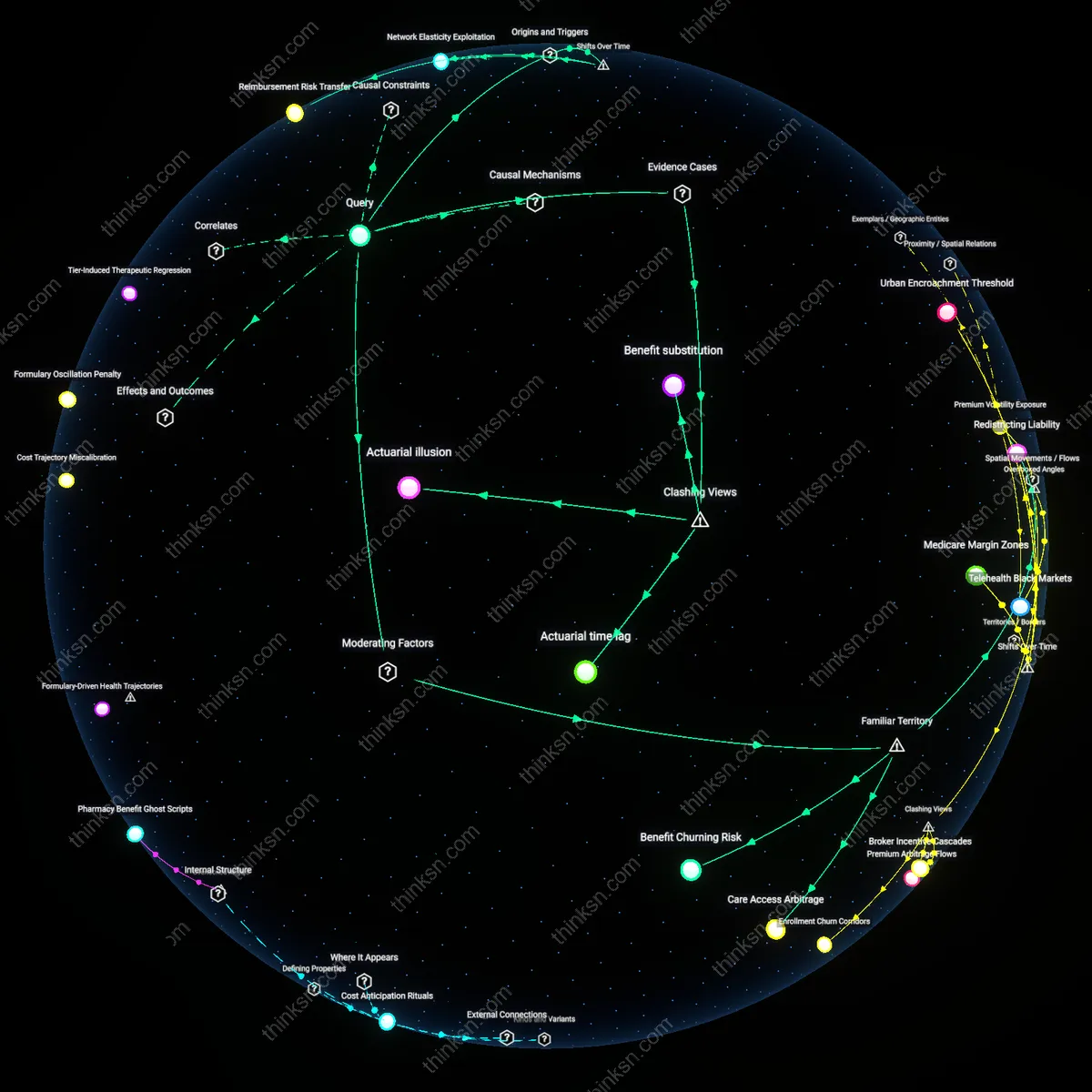
Reimbursement Risk Transfer
The shift to capitated Medicare Advantage reimbursement after the 2003 Medicare Modernization Act transferred financial risk from insurers to patients by design. Insurers receive fixed per-enrollee payments from CMS, creating incentives to limit services while shifting unmet care costs—via narrow networks, prior authorization, and formulary restrictions—onto beneficiaries, especially those with chronic conditions. This mechanism, amplified by post-2010 payment parity policies, reveals how systemic underfunding relative to fee-for-service Medicare has been monetized through patient assumption of access barriers, a dynamic obscured by the surface appearance of 'no premium' plans.
Actuarial Time Delay
Medicare Advantage plans compress actuarial timelines by front-loading profits while deferring patient costs, a shift cemented during the 2017–2020 phase of rapid plan consolidation. Insurers maximize margins by attracting healthier enrollees and minimizing early expenditures, knowing CMS overpays by 2–5% on average; the deferred financial burden manifests when patients face acute care gaps or disenrollment penalties in later years. This time-lagged cost imposition undermines long-term financial planning in a way invisible to standard actuarial models, which fail to track individual cost trajectories beyond annual cycles.
Network Elasticity Exploitation
The expansion of private plan networks under Medicare Advantage after 2010 enables geographic and specialty-based cost shifting by varying provider access without transparency. Insurers in sunbelt states, for example, design networks that exclude high-cost specialists—especially in cardiology and oncology—forcing patients into out-of-network care or early retirement relocation to maintain coverage. This spatial arbitrage, normalized under the guise of 'flexible benefits', reveals how reimbursement models exploit regional health system imbalances, turning patient mobility and household financial stability into de facto cost containment instruments.
Premium Volatility Exposure
Higher out-of-pocket costs emerge when Medicare Advantage plans shift premium fluctuations onto enrollees through tiered pricing and supplemental cost-sharing. Private insurers adjust monthly premiums based on local network renegotiations, formulary changes, and regional risk scores, making year-to-year budgeting difficult for fixed-income seniors. This mechanism is especially significant in suburban and rural markets where limited plan competition reduces price transparency and forces beneficiaries to absorb sudden increases. While most public discussion focuses on lower initial premiums, the underlying instability of those rates—driven by insurer profit optimization rather than public cost control—is rarely accounted for in household financial planning.
Care Access Arbitrage
Patients bear hidden costs when Medicare Advantage plans restrict provider networks to reduce reimbursement outflows, requiring beneficiaries to either pay out-of-network rates or forgo preferred clinicians. This cost-shifting occurs through prior authorization rules, narrow networks, and geographic service deserts, particularly affecting chronically ill seniors who require consistent specialist access. The public routinely associates 'more choices' with private Medicare plans, but the reality is that choice is conditional on compliance with administrative gates that increase time, travel, and indirect expenses. The financial impact isn't captured in premiums but in the compounded burden of delayed or denied care, which disrupts long-term health spending forecasts.
Benefit Churning Risk
Annual plan redesigns—common under Medicare Advantage—shift costs by altering covered services and pharmacy tiers each enrollment cycle, forcing patients to reevaluate care affordability every year. Insurers legally restructure benefits based on CMS bidding rules and regional risk pools, which incentivizes offering attractive initial packages that degrade over time to manage margins. Most seniors expect continuity in coverage once enrolled, but the system rewards churn in benefit design, making it difficult to project medication or service costs beyond 12 months. This creates a planning deficit rooted not in individual overspending but in structural unpredictability masked as customization and flexibility.
Actuarial illusion
The Medicare Advantage reimbursement model shifts costs to patients by incentivizing plans to attract healthier enrollees through enhanced benefits, which distorts risk adjustment payouts and inflates long-term financial burdens on those with chronic conditions who remain in traditional Medicare. Insurance giants like UnitedHealthcare exploit diagnostic upcoding—especially in Special Needs Plans in Florida and Texas—where capturing minor or historical conditions increases per-member payments without corresponding care, effectively reallocating system-wide costs into traditional Medicare and reducing its sustainability. This mechanism remains hidden from enrollees because enhanced premiums and reduced supplemental benefits appear generous initially, but destabilize public program solvency over time, contradicting the dominant narrative that MA plans save money for patients.
Benefit substitution
Medicare Advantage plans reduce patient cost exposure in premium terms only by reconfiguring out-of-pocket liabilities through non-standard benefit designs, effectively shifting long-term financial risk onto enrollees through mechanisms like capped coverage for home health or asymmetric drug formularies. In Pennsylvania, Highmark MA plans offer $0 premiums while imposing utilization limits on durable medical equipment, forcing patients with progressive diseases to absorb costs once their condition exceeds plan templates—often after irreversible care gaps occur. This contradicts the conventional view that lower premiums equate to greater affordability, exposing how cost shifting is masked as generosity through the strategic replacement of direct expenses with structural exclusions.
Actuarial time lag
The current Medicare Advantage reimbursement model accelerates short-term financial predictability for insurers while deferring patient cost exposure into later stages of illness through delayed denial mechanisms embedded in prior authorization regimes, as seen in Humana’s congestive heart failure protocols in rural Kentucky. These plans approve marginal treatments early but systematically reject escalating interventions over time, forcing patients to exhaust appeals processes or pay out-of-network rates when their condition deteriorates—costs that were never disclosed at enrollment. This dynamic disrupts the standard critique that cost shifting occurs primarily via copays or premiums, revealing instead how temporal manipulation of care approval functions as a deferred financial liability.