Is Age-Based ICU Allocation Fair to Elderly Patients?
Analysis reveals 9 key thematic connections.
Key Findings
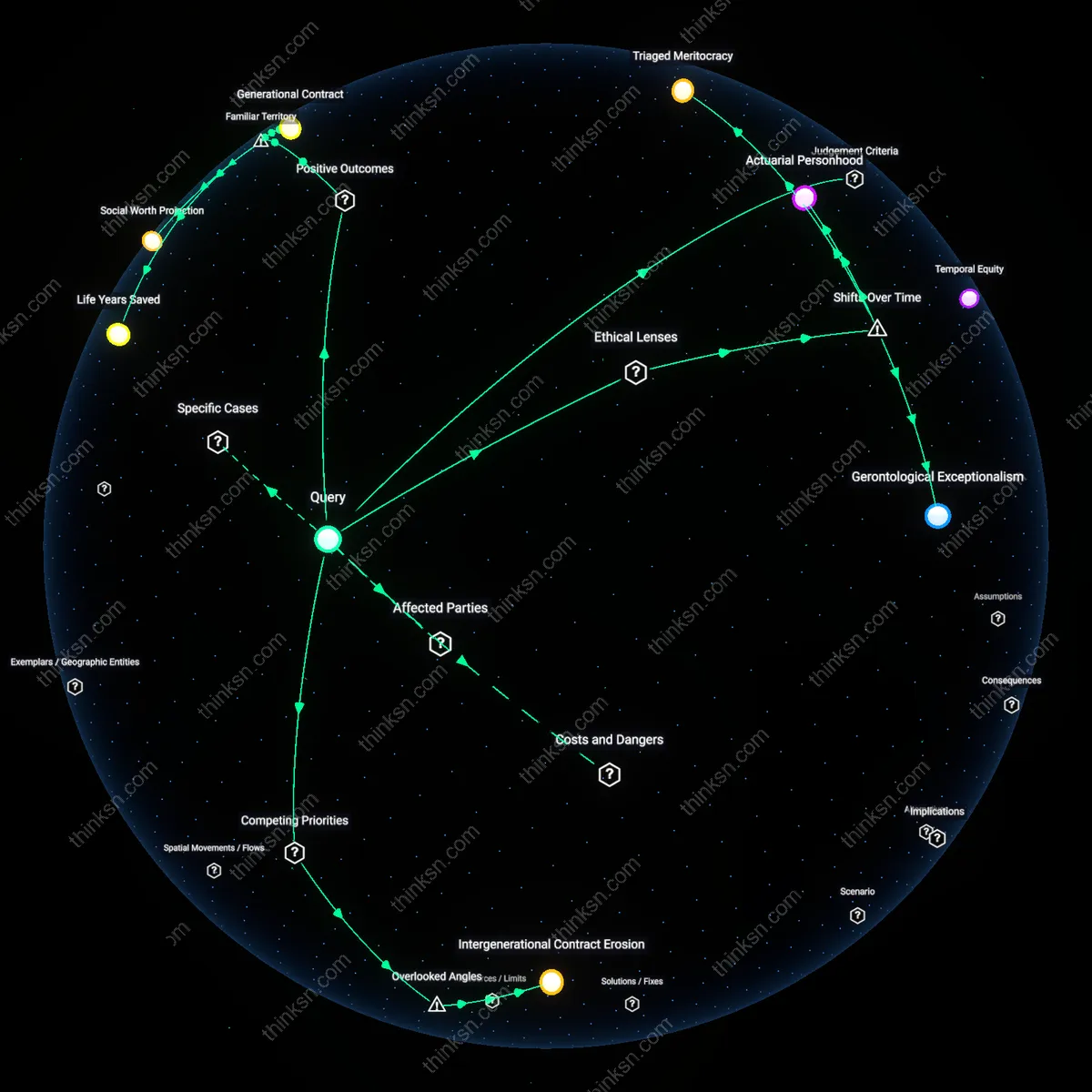
Temporal Equity
Using age-based triage protocols during Italy’s 2020 COVID-19 surge prioritized younger patients not on grounds of inherent worth but on the principle that limited ICU resources should maximize life-years saved, reflecting a utilitarian calculus that treats future time as a distributive metric. Italian medical associations endorsed guidelines that de facto deprioritized adults over 80 based on predicted survival duration, not immediate clinical need—operating through regional health boards in Lombardy where decision trees incorporated age as a proxy for resilience. This reveals how crisis standards of care can normalize temporal equity, where fairness is indexed to anticipated longevity rather than present vulnerability, subtly recasting age as an actuarial destiny.
Institutional Abandonment
In the 2009 H1N1 pandemic in Mexico City, public hospitals delayed ICU access for older adults due to fragmented insurance coverage and ageist assumptions about 'natural decline,' leading to disproportionate mortality—an outcome not mandated by policy but emergent from systemic neglect. Public-sector hospitals under Seguro Popular treated elderly patients as low-priority relative to younger, formally employed citizens, reinforcing classed and gerontological hierarchies through triage bureaucrats who lacked protocols but applied implicit discounting of older lives. This instance exposes how institutional abandonment occurs when resource allocation is left to discretion in inequitable systems, where fairness is compromised not by explicit rules but by the invisibility of older adults in design.
Life Years Saved
Prioritizing younger patients for ICU beds maximizes the number of life years preserved, aligning with public health goals during crises like the COVID-19 pandemic when hospitals in Lombardy or New York faced triage decisions. This approach reflects a widely accepted intuition that saving younger lives yields greater aggregate survival benefit, operating through utilitarian frameworks embedded in crisis standards of care. What’s underappreciated is how this familiar appeal to 'more years' subtly shifts ethical weight from individual dignity to population-level efficiency, naturalizing age as a proxy for future contribution.
Social Worth Projection
Allocating ICU access by age implicitly ties medical value to perceived societal productivity, echoing common narratives that associate older adults with dependency and youth with economic or familial future-building. This mechanism functions through culturally reinforced assumptions visible in media portrayals and policy debates, where saving a younger person is framed as 'saving a mother' or 'a worker' rather than an elder with accumulated wisdom. The non-obvious effect is how routinely invoking these roles legitimizes covert rationing by social utility, masked as clinical pragmatism.
Generational Contract
Using age in ICU triage activates an implicit intergenerational bargain where society protects the young now in expectation they will support future elders, mirroring pension systems or educational investment seen in countries like Japan or Germany. This dynamic operates through reciprocal expectations embedded in social institutions, not just medical ethics guidelines. The underrecognized insight is that public comfort with age-based triage may stem less from devaluing older lives and more from upholding a deeper, unstated norm of cyclical care across life stages.
Intergenerational Contract Erosion
Allocating ICU beds by age undermines intergenerational reciprocity because older adults' prior contributions to social infrastructure are rendered invisible when they become dependent on it during crises. Healthcare rationing based on life-years saved privileges future productivity over past investment in societal systems—such as tax payments, caregiving labor, and civic participation—which older adults have cumulatively provided. This shift is particularly pronounced in aging societies like Japan or Italy, where retiree-to-worker ratios strain pension systems, yet those same retirees are excluded from critical care on grounds of diminished future output. The overlooked dynamic is that fairness in triage does not just reflect competing lives but competing temporal claims on society’s obligations, altering how moral weight is assigned across generations.
Triaged Meritocracy
Allocating ICU beds by age is fair under a utilitarian calculus that emerged prominently during the 2020 COVID-19 pandemic, when clinical guidelines in regions like Lombardy and New York shifted toward maximizing life-years saved. This approach institutionalized a form of medical triage that privileges younger patients not on individual merit but on projected biological productivity, embedding a consequentialist ethic into emergency allocation protocols. The non-obvious outcome of this shift is that it redefined fairness as demographic efficiency, revealing how crisis conditions can normalize a temporally coded hierarchy—where value is indexed to expected duration of life—within healthcare systems that otherwise reject age discrimination.
Actuarial Personhood
Age-based ICU allocation became ethically legible through a historical pivot in the late 20th century, when actuarial models migrated from insurance industries into bioethics and public health policy, particularly after the 1980s cost-containment era in U.S. medicine. This mechanism transformed the patient into a risk profile, where clinical decisions are increasingly mediated by statistical life expectancies rather than moral status, with older adults rendered as actuarially depleted subjects. The significance lies in how this shift concealed ethical judgment within technical rationality, making age-based deprioritization appear value-neutral even as it encoded a quiet devaluation of aging bodies.
Gerontological Exceptionalism
The fairness of age-based ICU allocation unravels when viewed through the rise of geriatric medicine as a counter-discourse since the 1990s, which challenged the assumption that advanced age necessarily implies poor outcomes by demonstrating heterogeneous resilience among older adults. This medical shift exposed the fallacy of age as a proxy for frailty, revealing how triage protocols reliant on chronological metrics reproduce a biologically deterministic view that older patients lack recoverability. The underappreciated consequence is that such protocols instantiate a new form of ageism—one masked as clinical pragmatism—despite growing evidence that societal investment in aging populations demands recognition of their variable, not diminished, human potential.