Is Cheaper Care for Aging Parents Ethically Justifiable?
Analysis reveals 4 key thematic connections.
Key Findings
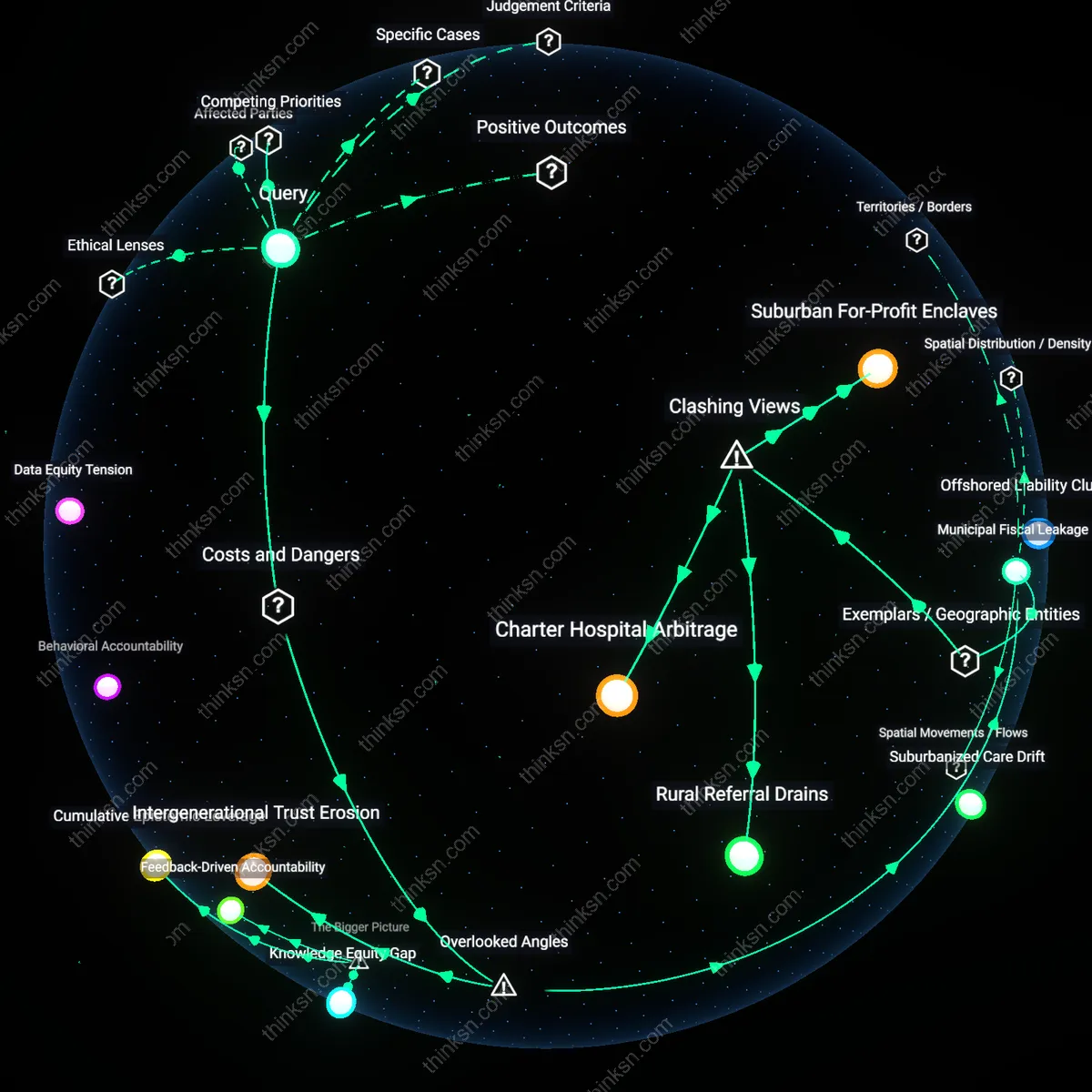
Intergenerational Trust Erosion
Choosing lower-cost, lower-quality elder care systematically undermines the tacit social contract between generations within families, as younger members’ financial calculations become visible and codified in ways that recalibrate expectations of reciprocity. When care decisions are perceived as cost-driven rather than need-driven, it signals to both current and future dependents—children and aging parents alike—that care is conditional, not categorical, altering long-term familial behavior. This shift weakens the unspoken assurance that support will be prioritized regardless of expense, ultimately eroding intergenerational trust, a dynamic rarely weighed in cost-benefit analyses of elder care but central to family cohesion over time. The non-obvious risk is not immediate harm to the parent, but the quiet redefinition of care as a negotiable commodity, which alters relational logic across decades.
Municipal Fiscal Leakage
Opting for substandard private elder care increases long-term municipal fiscal burdens by displacing state-supported high-quality services with care models that generate hidden public costs through emergency health interventions and social service overrides. When under-resourced facilities fail to manage chronic conditions or prevent falls and infections, the downstream burden falls on publicly funded hospitals and adult protective services, particularly in counties with strained safety nets like those in rural Georgia or upstate New York. Evidence indicates that cost-saving decisions at the family level often correlate with increased Medicaid utilization and first-responder callouts, shifting rather than reducing systemic costs. This fiscal leakage—where private savings generate public losses—remains invisible in household budgets but destabilizes municipal care infrastructure over time.
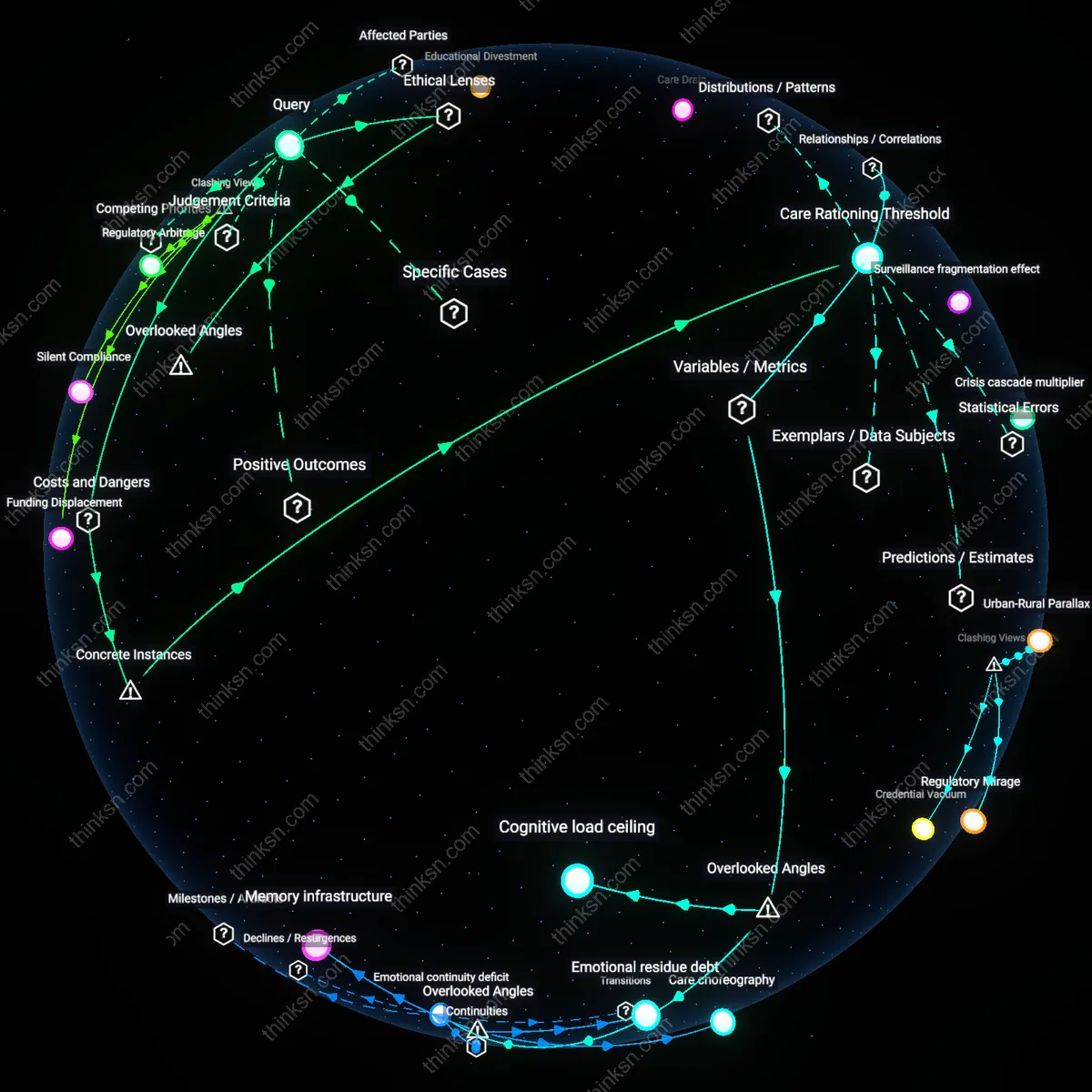
Clinical Data Distortion
Widespread adoption of lower-quality elder care settings skews population-level health data by underreporting comorbidities and treatment adherence, distorting clinical benchmarks used to design geriatric care standards and pharmaceutical dosing guidelines. Facilities prioritizing cost-efficiency often lack consistent monitoring tools or staff trained to document cognitive decline, pain levels, or medication responses with the rigor of accredited institutions, leading to systemic noise in datasets aggregated by hospital networks and research consortia. This data distortion particularly affects treatments for conditions like dementia and heart failure, where symptom progression models depend on accurate longitudinal input. The overlooked consequence is that family-level cost decisions contribute to degraded medical evidence, imperiling not just the individual parent but the validity of future care protocols for entire patient populations.
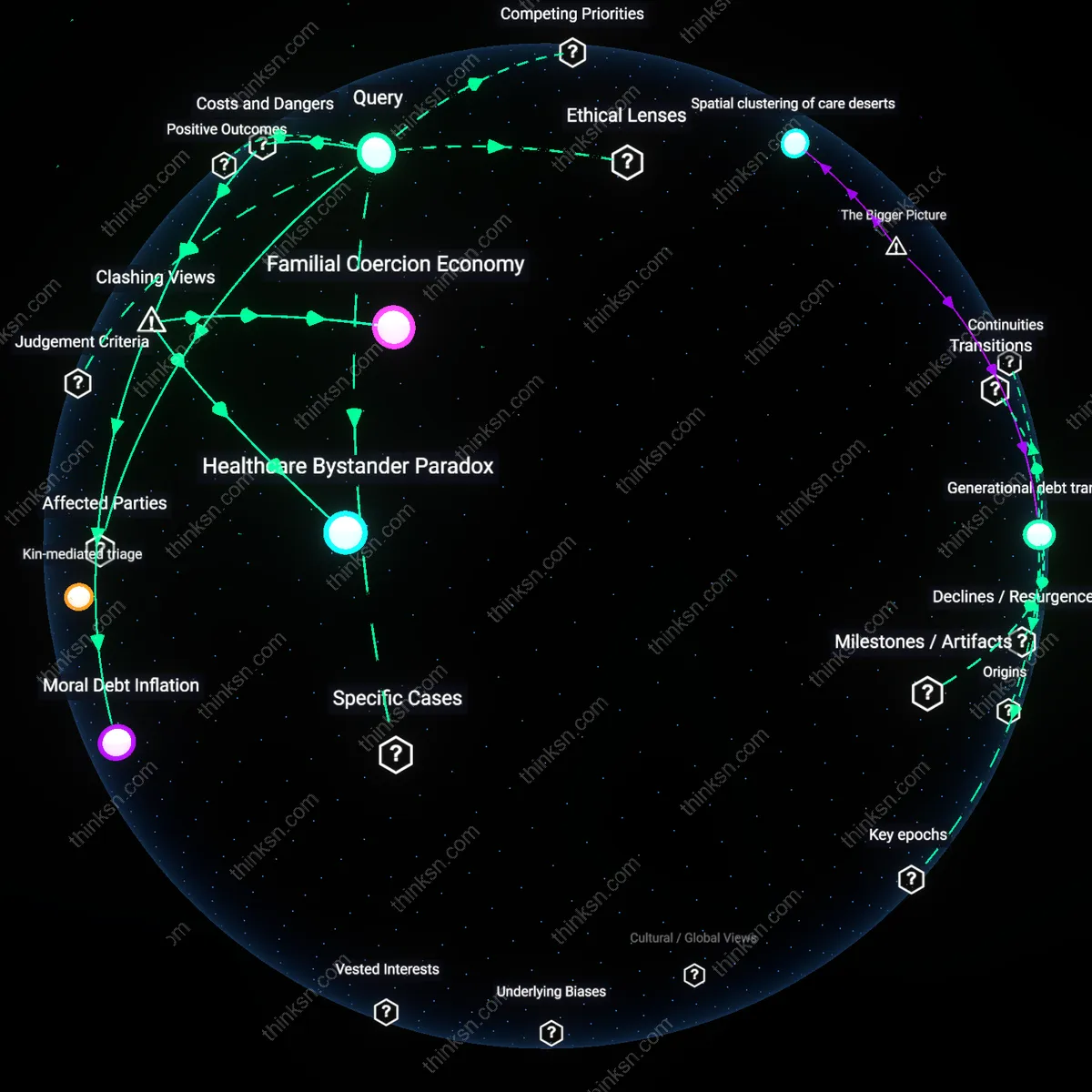
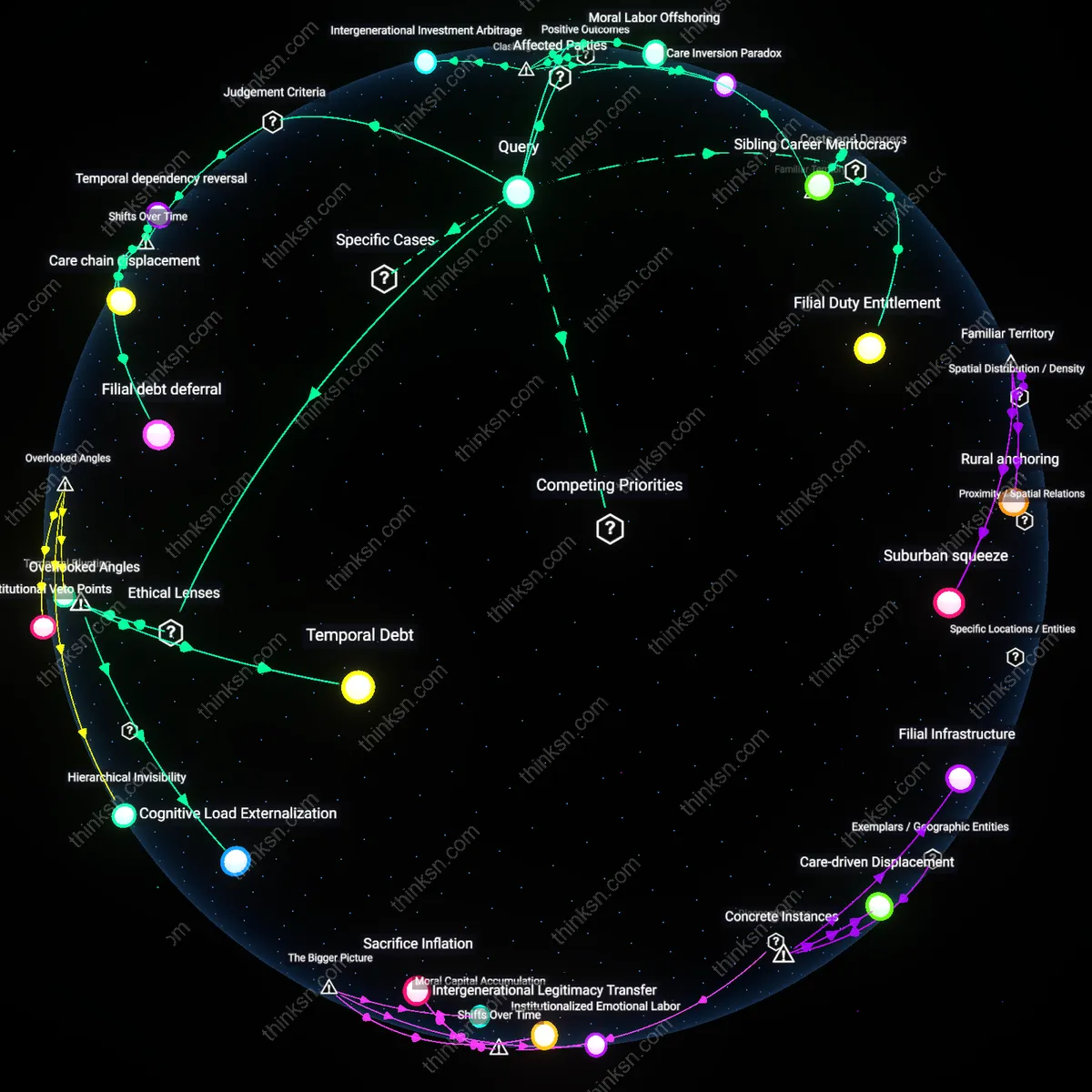
Kinetic Responsibility
The acceptability of choosing lower-cost elder care crystallized only after the 1990s expansion of privatized home care markets, which redefined filial duty not as direct physical attendance but as cost-effective management of externalized labor. As care shifted from institutional to fragmented, home-based service models, families could outsource bodily care while retaining moral credit for oversight—so long as budgets were optimized. This transition, driven by Medicaid managed care reforms and venture-backed eldercare platforms, decoupled moral worth from care quality and recoupled it to fiscal stewardship, making prudence a new form of filial virtue. The underappreciated dynamic is that moral justification now depends on demonstrating responsible navigation of market choices, not the quality of lived care experience.