Is Society Undervaluing Home Health Care for Elders?
Analysis reveals 5 key thematic connections.
Key Findings
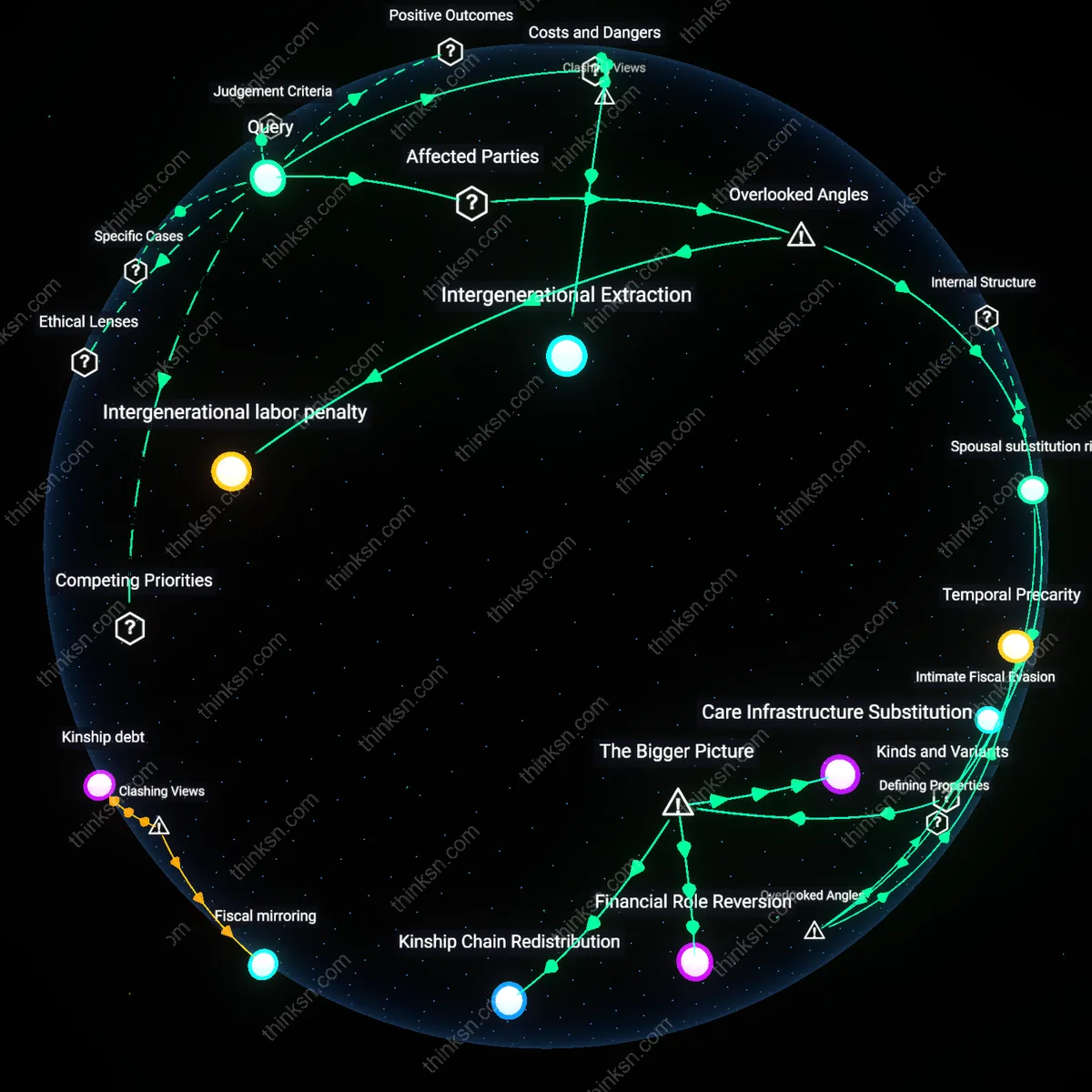
Burden Transfer
The gap between Medicare's restricted home-health coverage and growing demand for in-home care indicates that families, especially middle-income adult children, are expected to absorb the financial and labor-intensive responsibilities of elder care. Medicare’s narrow eligibility—limited to skilled nursing or therapy following hospitalization—excludes long-term personal care like bathing or meal prep, forcing households to privately finance or personally deliver services that clinical systems exclude. This reflects a systemic deference to familial obligation over public responsibility, where the absence of universal support infrastructure outsources eldercare to kin networks, particularly women and lower-wage relatives. The non-obvious implication is that this informal care economy is not an anomaly but a designed pressure valve, sustaining cost-constrained public programs by relying on unpaid or underpaid domestic labor.
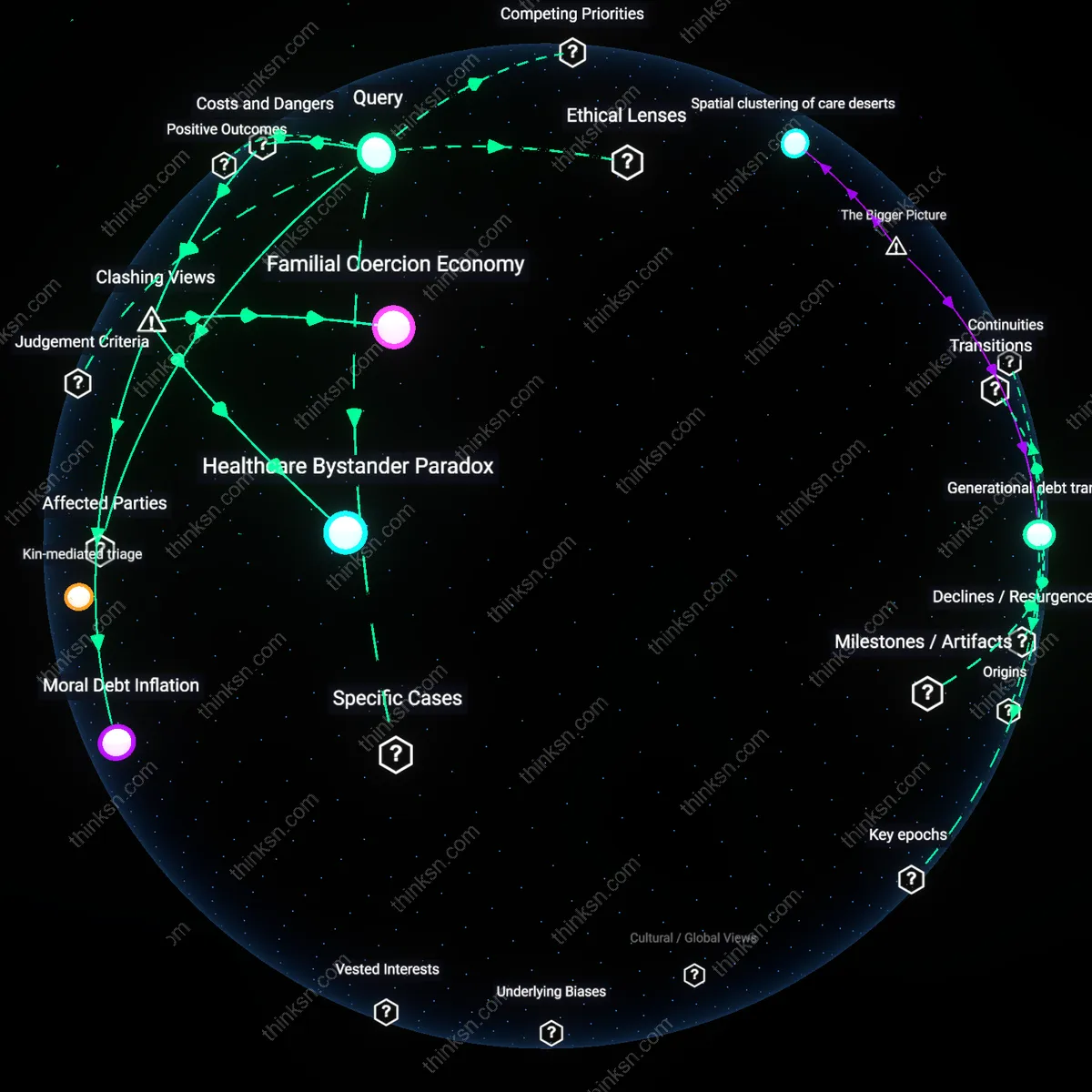
Welfare Hierarchy
The coverage gap signals that American society stratifies careworthiness, privileging institutional care and acute medical treatment over dignified, community-based aging, thereby reinforcing a caste-like differentiation in how elder lives are valued. Nursing homes receive robust Medicaid reimbursement, while home-based support—often preferred and more cost-effective—is rationed through strict clinical criteria and income-based eligibility, disproportionately disadvantaging those who lack family caregivers or reside in rural areas. This tiered system reflects a broader ideological preference for containing aging within professionalized, clinical spaces rather than investing in social models of care that sustain autonomy and place attachment. The underappreciated mechanism is that this hierarchy isn’t accidental but actively maintained through budgetary choices that valorize medical intervention over daily living support.
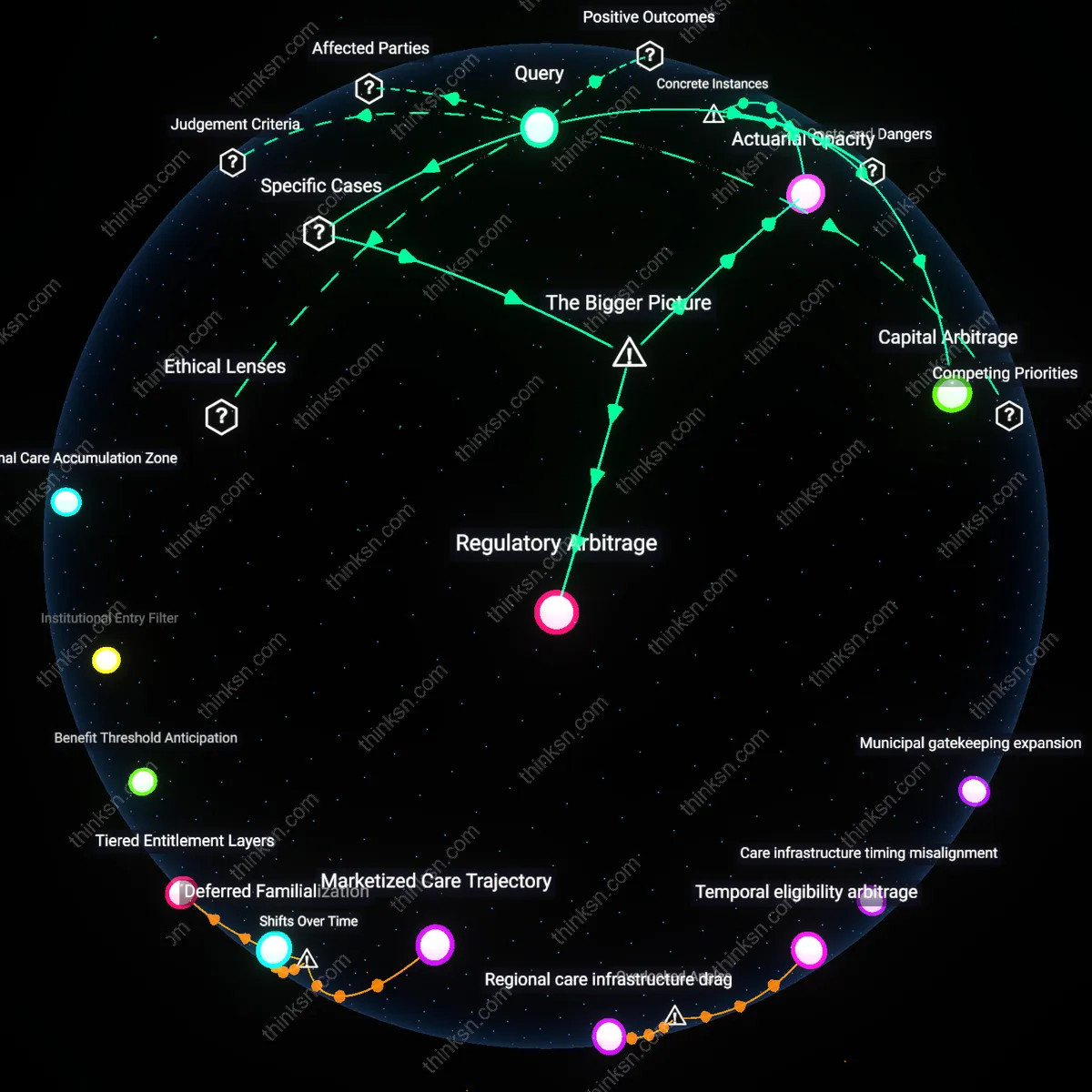
Care Deflection
Medicare’s limited home-health benefits reflect a systemic preference for institutional over in-home care, privileging clinical efficiency and cost containment within a framework of allocative justice shaped by utilitarian cost-benefit calculus. Federal reimbursement rules restrict ongoing home care to patients who are homebound and require skilled nursing, effectively excluding long-term functional support for aging adults with chronic but stable conditions—thereby transferring responsibility to families, particularly women and low-income caregivers, who absorb unpaid labor under familial obligation norms. This mechanism reveals how public policy, underpinned by neoliberal fiscal discipline and actuarial rationality, shifts social risk onto private networks, normalizing the invisibility of care work while preserving budget neutrality. The non-obvious insight is that the coverage gap is not a policy failure but a calculated alignment of actuarial governance with gendered and racialized caregiving infrastructures.
Temporal Disinvestment
The mismatch between Medicare’s narrow eligibility and rising demand for in-home care signals a deeper political economy that devalues late-life dependency, treating aging not as a phase requiring robust public infrastructure but as a private contingency managed through fragmented markets. Because Medicare is structured around episodic medical events rather than continuous social support, its design reflects a developmental time model that equates health with productivity and views old age as decline rather than a legitimate stage of human flourishing—aligning with liberal individualism and life-course paradigms prevalent in U.S. social policy. As longevity increases and the senior population diversifies, particularly in urban centers like Miami-Dade and Harris Counties with growing elderly minorities, the pressure on informal systems intensifies, exposing how institutional temporality excludes non-acute, protracted needs. What is underappreciated is that this temporal misalignment is not incidental but constitutive of a system that only recognizes dependency during clinical crises, not as a foreseeable social condition.
Spatialized Care Rationing
The restriction of Medicare home-health benefits functions as a geographic mechanism of care rationing, where federal reimbursement criteria produce uneven access along urban-rural and racialized lines, thereby inscribing spatial hierarchies into eldercare equity. In rural counties across Appalachia and the Delta, where hospital closures and transportation barriers limit clinical access, the lack of covered in-home services forces reliance on under-resourced local networks, while federally qualified health centers lack capacity to compensate—this reflects a distributive model shaped by federalism and localism that delegates care responsibility to failing local infrastructures. Regulatory logic treats home health as a medical supplement rather than a social necessity, enabling state and municipal underfunding under the guise of federal constraints, thus reinforcing regional disparities. The overlooked insight is that the coverage gap operates not just financially but cartographically—making care availability contingent on zip code, not need.