HSAs vs Roth IRAs: Balancing Future Health and Wealth?
Analysis reveals 5 key thematic connections.
Key Findings
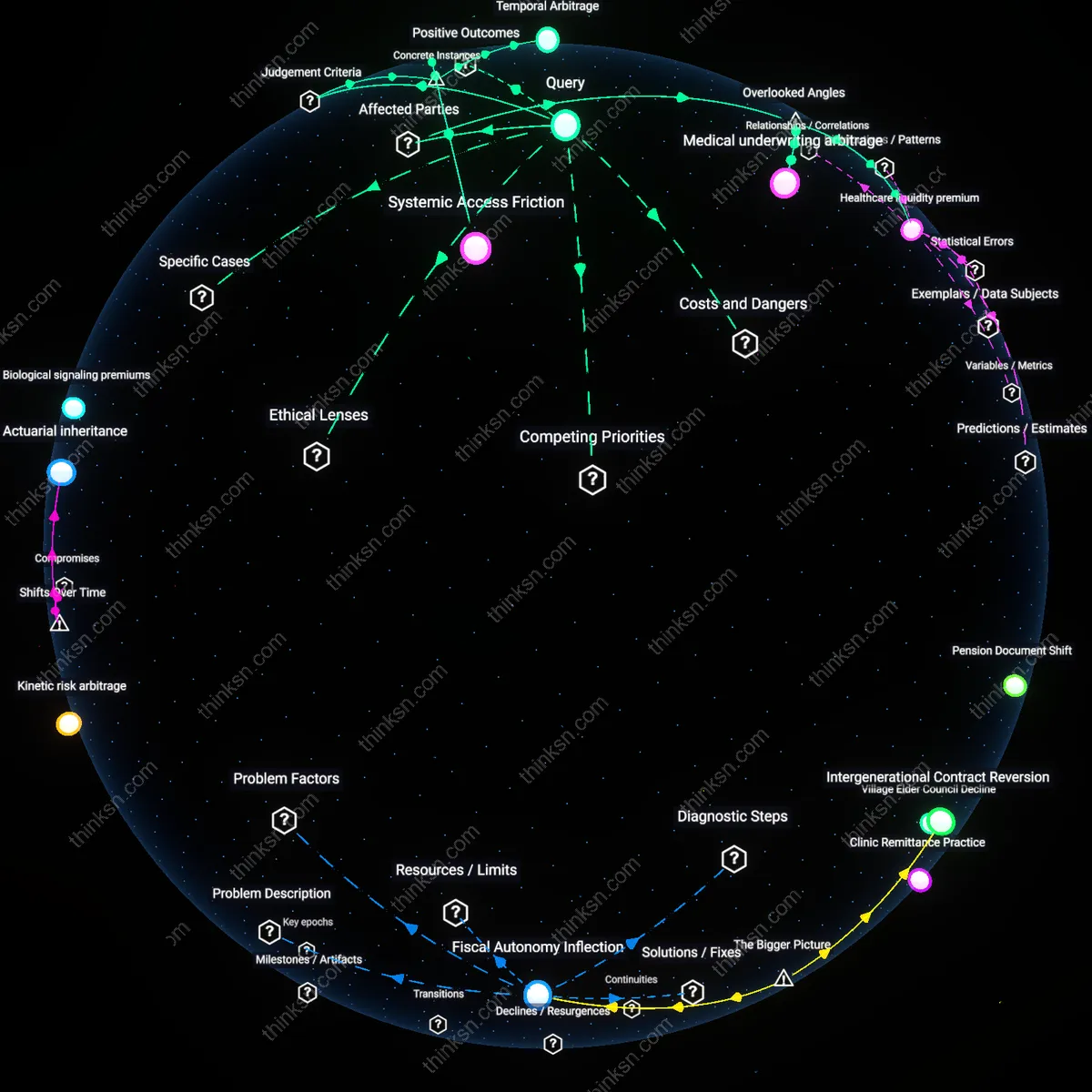
Medical underwriting arbitrage
Front-load HSA contributions even at the expense of Roth IRA savings if one anticipates future eligibility for subsidized insurance programs like ACA marketplaces or Medicaid. Because HSA eligibility requires enrollment in high-deductible health plans (HDHPs), individuals who strategically time their HSA funding during periods of private HDHP coverage can later transition to public or subsidized plans without forfeiting accumulated funds, creating a backdoor tax-free savings channel. This dynamic is invisible in conventional advice, which treats account choices as static, yet it enables financially literate lower-middle-income households to exploit regulatory gaps between private savings incentives and public benefit thresholds, effectively gaming the boundary between personal responsibility and state support.
Healthcare liquidity premium
Allocate incrementally to the HSA before the Roth IRA when residing in states with weak emergency medical protections and punitive debt enforcement, such as Texas or Florida. In these jurisdictions, even insured patients face high out-of-network billing risks and aggressive collection practices, making HSA funds a form of localized financial self-insurance that preserves creditworthiness and avoids cascading household instability. Standard models ignore that healthcare costs function not just as retirement risks but as acute liquidity shocks, and that tax-free access to HSA balances serves an immediate protective function akin to a high-yield emergency fund—especially where legal and institutional supports are thin, reframing the account as a survival mechanism rather than a long-term investment.
Temporal Arbitrage
Prioritize Roth IRA contributions when early-career income is low because future tax rates are likely higher than current ones, as demonstrated by physicians in training who deferred taxation during residency only to face higher marginal rates in practice; this mechanism exploits the irreversibility of time in tax liability scaling, revealing that income trajectory asymmetry makes Roth conversions a form of intertemporal financial optimization often overlooked in static models of retirement planning.
Medical Uncertainty Premium
Allocate more to a Health Savings Account when facing a diagnosis with uncertain progression, such as early-stage multiple sclerosis in a 38-year-old software engineer in Oregon who maximized HSA contributions post-diagnosis to exploit triple tax advantages amid unpredictable future care costs; this response embeds a hidden insurance function against idiosyncratic health shocks, exposing how personalized risk profiles can rationally tilt asset allocation toward medical liquidity over generalized retirement growth.
Systemic Access Friction
Direct limited funds to HSAs over Roth IRAs for low-income service workers in Texas lacking employer-sponsored plans, where Medicaid eligibility caps penalize IRA asset accumulation but exempt HSA balances tied to HDHPs, revealing how structural policy misalignments create perverse incentives in which medical savings vehicles become de facto wealth preservation tools under means-tested systems, an effect rarely acknowledged in mainstream financial advice.