Who Wins in Claims Triage? Prioritizing Equity in Insurance
Analysis reveals 6 key thematic connections.
Key Findings
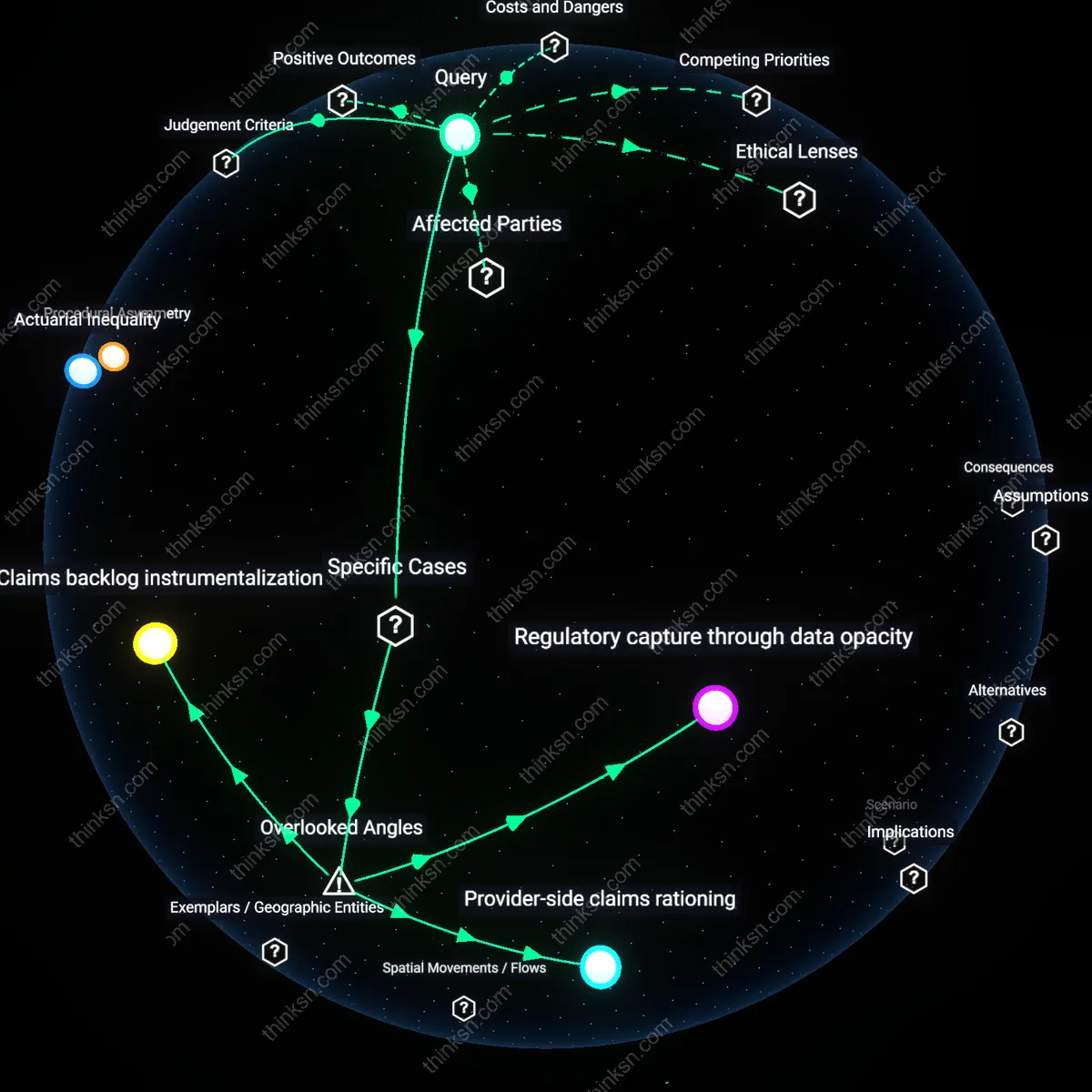
Actuarial Inequality
Insurers' claims triage privileges capital stability over equitable access, a shift from postwar social insurance norms to neoliberal risk segmentation after the 1980s deregulation wave. Under pressure to maximize shareholder returns, actuaries reclassified claimant behaviors as 'risk signals,' transforming medical necessity into actuarial probability—penalizing those with complex or recurrent needs not because they violate policy terms but because their predictability undermines portfolio efficiency. This recalibration reveals that fairness is no longer measured by need but by the cost of deviating from statistical baselines, a shift obscured by clinical justifications masking financial thresholds.
Procedural Asymmetry
Claims triage systematically advantages insurers by institutionalizing asymmetrical review timelines and evidentiary burdens, a transformation cemented during the managed care expansion of the 1990s when 'utilization review' became routine. Insurers deploy layered appeals processes that exploit patients’ temporal and informational disadvantages—denials are fast, appeals are slow, and reversals come after treatment delays that often negate medical urgency. This procedural imbalance reframes fairness not as outcome parity but as adherence to internal process rules, masking power differentials through procedural legitimacy that emerged precisely when external regulatory oversight receded.
Datafied Compliance
Insurers' triage practices now benefit from algorithmic governance systems adopted since 2010, which redefined compliance as data consistency rather than ethical consistency, shifting authority from clinicians to backend analytics teams. Under this model, claims are scored using natural language processing and historical adjudication data, privileging patterns of past denials as proxies for 'valid' claims—thus reinforcing existing biases as operational norms. The resulting feedback loop institutionalizes historical inequities as machine-learned standards, presenting them not as moral failures but as neutral compliance outcomes, thereby displacing ethical judgment into opaque technical systems.
Claims backlog instrumentalization
Insurers' triage practices disproportionately benefit third-party administrators (TPAs) like CoventryHealth or Optum who profit from delaying low-severity claims to create operational inefficiencies that are later monetized through 'efficiency consulting' contracts. These TPAs exploit triage algorithms to deliberately accumulate manageable backlogs, which then justify large-scale process overhauls sold back to insurers as cost-saving solutions—despite eroding timely care for patients in mid-tier diagnostic categories. The overlooked mechanism is not bias in triage per se, but the strategic under-processing of claims as a revenue-generating feedback loop, which reframes procedural delays as intentional infrastructure rather than system failure. This transforms administrative inertia into a billable asset class.
Regulatory capture through data opacity
State insurance departments in markets like Florida and Arizona indirectly benefit from insurers’ triage opacity because inconsistent adjudication generates a surge in appeal filings, which in turn inflates agency budget justifications and staffing mandates. By allowing triage criteria to remain proprietary, regulators create a self-sustaining cycle where poor initial decisions necessitate bureaucratic oversight, thereby expanding their institutional footprint. The underappreciated dynamic is that regulatory agencies may have an institutional interest in maintaining confusion at the claims level—not to favor insurers or patients, but to reinforce their own political relevance through crisis management. This reveals triage unfairness as a source of administrative power, not just economic distortion.
Provider-side claims rationing
Large hospital systems such as Northwell Health adapt to insurers’ triage thresholds by pre-screening patient claims for likely denial risk, then downgrading or suppressing submissions for marginally eligible treatments to preserve payer relationships and maintain bulk reimbursement rates. This creates an invisible layer of clinical rationing that occurs before claims even enter insurer systems, where fairness is compromised not by insurer decisions but by provider self-censorship to avoid administrative conflict. The overlooked cause of inequity is thus not the insurer’s adjudication logic but the anticipatory compliance of care providers who internalize triage expectations, shifting the locus of denigration from payer to provider and rendering access disparities logistically invisible.