Does Insurer Bias Taint Fairness in Medical Appeal?
Analysis reveals 11 key thematic connections.
Key Findings
Procedural Safeguards
The Minnesota Department of Health's external review program for Medicaid appeals reduced bias by mandating independent physician review when insurers deny care, demonstrating that structural independence in appeals directly increases fairness. This system requires that any contested denial be re-evaluated by a third-party medical expert unaffiliated with the insurer, thereby neutralizing financial incentives embedded in internal review processes. What is underappreciated is that fairness is not achieved through transparency alone, but through enforceable procedural separation between payer and evaluator.
Market Discipline
In the Netherlands, where health insurers operate under strict competition law and are prohibited from profiting on basic care, the threat of losing customers for repeated appeal denials incentivizes fairer initial coverage decisions, showing that competitive accountability can align financial motives with patient access. Insurers like CZ and Menzis have developed internal review protocols exceeding regulatory minimums to maintain public trust and market share, indicating that extramural financial pressures can counteract intramural cost-containment biases. The non-obvious insight is that financial incentives are not uniformly distorting—when applied at the market level, they can promote equity in appeals outcomes.
Regulatory Anchoring
California’s Department of Managed Health Care enforcement against UnitedHealthcare in 2021—fined $200 million for systematic delays and denials in autism therapy coverage—established that regulatory penalties can recalibrate insurer behavior more effectively than internal ethics policies, proving that external enforcement disrupts incentive-driven bias. The case revealed that financial penalties tied to appeal outcomes created a new cost calculus within UnitedHealthcare, leading to faster, more consistent approvals even before appeals were filed. The critical yet overlooked point is that fairness emerges not from eliminating financial incentives, but from imposing asymmetric consequence structures that make bias more costly than equity.
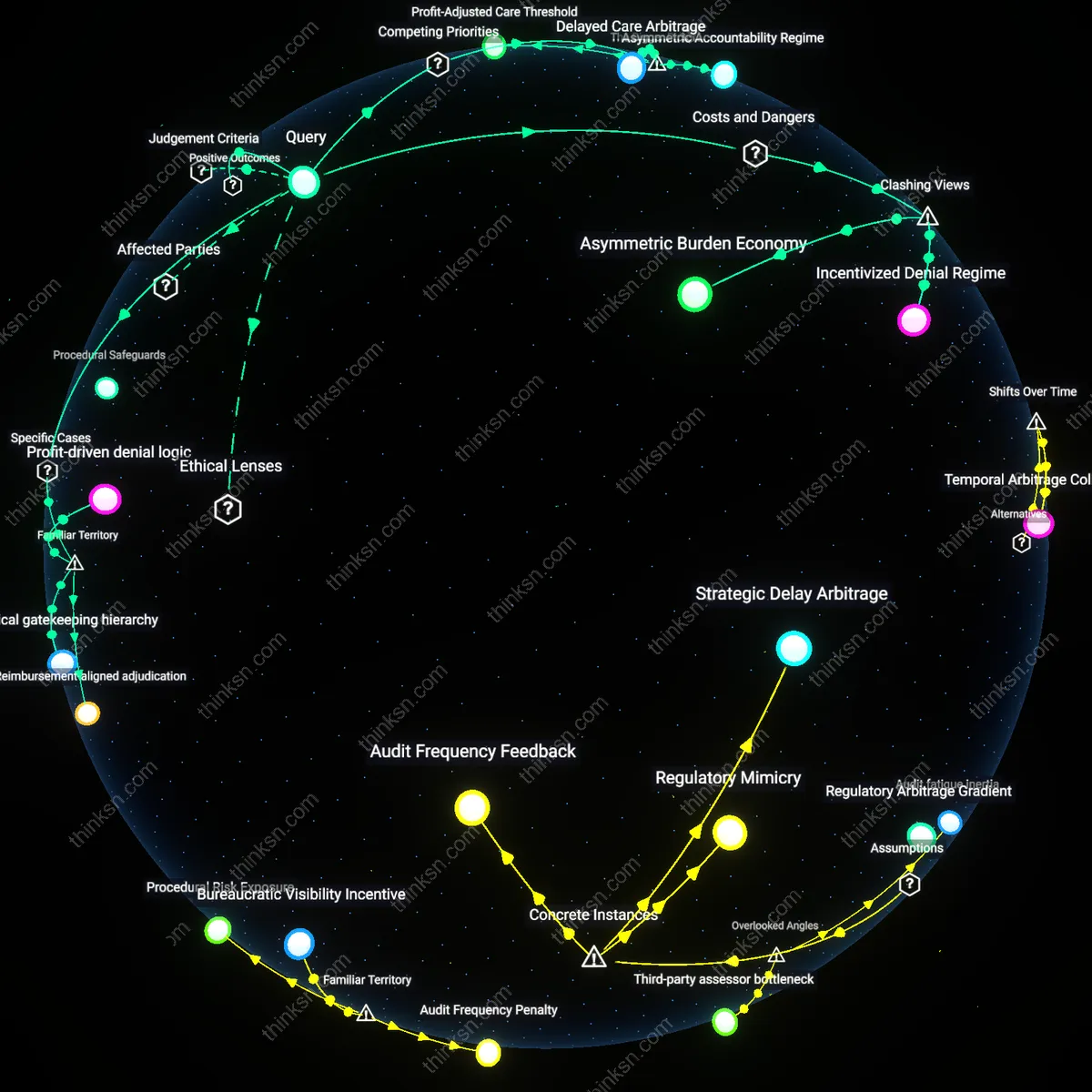
Incentivized Denial Regime
Financial incentives systematically increase the rate of denial in insurer-conducted medical appeals because insurance companies are structurally rewarded for minimizing claim payouts, creating a feedback loop where medical judgment is subordinated to cost containment metrics. This mechanism operates through internal performance benchmarks that tie claims adjuster evaluations to denial ratios, effectively transforming clinical appeals into procedural hurdles designed to exploit asymmetries in time and expertise—what is underappreciated is that the appeal process itself becomes a deterrent, discouraging even valid claims from being pursued, thus masking the true extent of withheld care.
Asymmetric Burden Economy
The fairness of insurer-conducted appeals is compromised not by overt fraud but by the deliberate construction of procedural complexity that leverages patients’ limited time, resources, and medical literacy. Insurers exploit differential access to documentation, specialist testimony, and legal support, making successful appeals feasible only for those with institutional backing or financial resilience, thereby institutionalizing inequity—this reveals that the system’s apparent neutrality masks a calculated transfer of burden onto the least empowered, turning fairness into a function of endurance rather than merit.
Profit-Adjusted Care Threshold
Financial incentives skew insurer medical appeals by institutionalizing cost-benefit analysis into clinical judgment, where profitability determines which treatments are deemed 'medically necessary' under appeal review. Insurers deploy actuarial models that weigh expected litigation costs against projected payouts, leading to strategic denial patterns that pressure providers into accepting suboptimal settlements—thereby reducing per-claim expenses but systematically disadvantaging complex, high-cost cases. This mechanism embeds economic triage within medical oversight, transforming appeals from clinical validations into fiscal risk calculations masked as peer review. The non-obvious consequence is that medical legitimacy becomes contingent on actuarial favorability, not just evidence-based standards.
Asymmetric Accountability Regime
Insurer-conducted medical appeals operate under a regulatory structure that mandates clinical justification for denials while insulating financial motivation from public scrutiny, creating a system where fiduciary duties to shareholders legally override patient equity in practice. Because state insurance commissioners lack uniform standards for auditing appeal outcomes, insurers face minimal penalties for patterns of economically driven rejections, enabling them to treat appeals as a compliance overlay rather than a restorative mechanism. This asymmetry allows profitability to be advanced through bureaucratic opacity, where the burden of proof falls entirely on patients or providers, not the entity controlling both payment and evaluation—revealing how institutional design enables mission drift under permissible oversight gaps.
Delayed Care Arbitrage
Insurers exploit time-cost imbalance in the appeals process by prolonging resolution periods for contested claims, effectively using procedural latency to induce medical obsolescence or patient withdrawal, thus avoiding payout without explicit denial. Because many treatments lose efficacy or urgency during months-long administrative reviews, the financial benefit arises not from superior medical judgment but from calculated procedural drag—particularly in oncology or neurology cases where timely intervention is irreversible. This transforms appeals from evaluative functions into instruments of de facto denial through delay, leveraging systemic inertia to align clinical timelines with fiscal advantages, a dynamic rarely captured in outcome audits focused only on final approval rates.
Profit-driven denial logic
Insurer-conducted medical appeals are systematically skewed toward denial when financial incentives are structurally embedded in utilization management, as seen in UnitedHealthcare’s UM protocols, where appeal outcomes consistently favor cost containment through standardized rejection templates tied to preauthorization algorithms. This mechanism functions through internal performance metrics that reward medical directors for aligning with corporate cost objectives rather than clinical reassessment, making the appeal process a procedural formality. The non-obvious insight is that these appeals are not neutral reviews but downstream enactments of upstream financial design, despite public perception framing them as corrective safeguards.
Clinical gatekeeping hierarchy
Medical directors at Anthem Blue Cross routinely override treating physicians’ recommendations during appeals, privileging internal clinical guidelines shaped by actuarial models rather than individual patient trajectories, demonstrating how financial incentive bias manifests through institutionalized medical authority. This operates via a hierarchical system in which corporate-employed clinicians, insulated from patient contact, adjudicate care based on protocol efficiency and risk stratification. The underappreciated reality is that the appeal process mimics clinical deliberation but functions as a legitimacy screen for financially motivated decisions, reinforcing the public’s mistaken belief in physician-led impartiality.
Reimbursement-aligned adjudication
At Aetna, appeal outcomes for high-cost specialty drugs show statistically significant correlation with plan-level profitability, revealing that financial incentive bias distorts fairness through covert adjustment of medical necessity criteria during internal reviews. This dynamic is operationalized via formulary design teams that retrospectively calibrate appeals to protect margin thresholds under Medicare Advantage contracts. The overlooked mechanism is that the appeal is not a remedial function but a feedback loop enforcing reimbursement strategy, contradicting the common assumption that it serves as an independent corrective to initial errors.