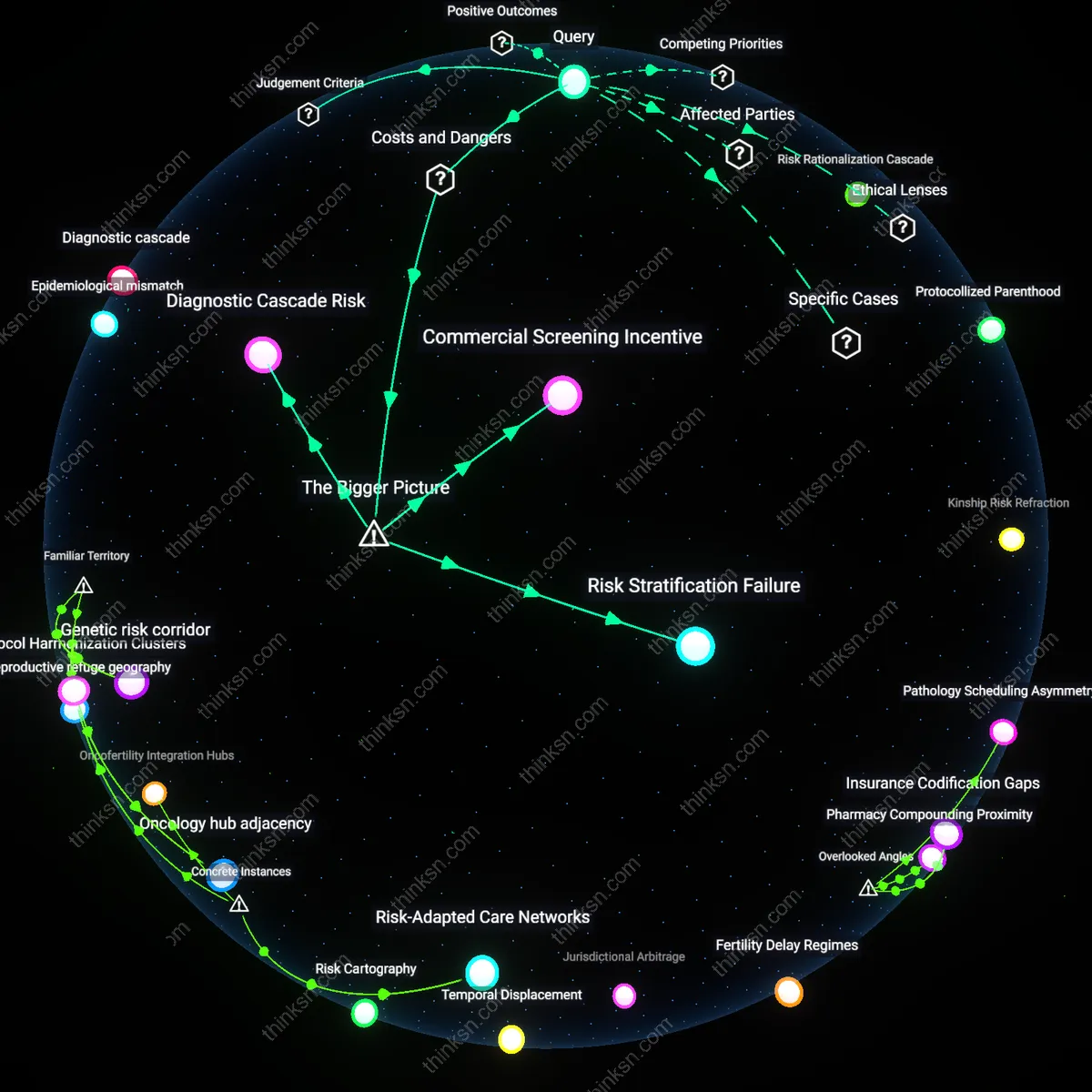
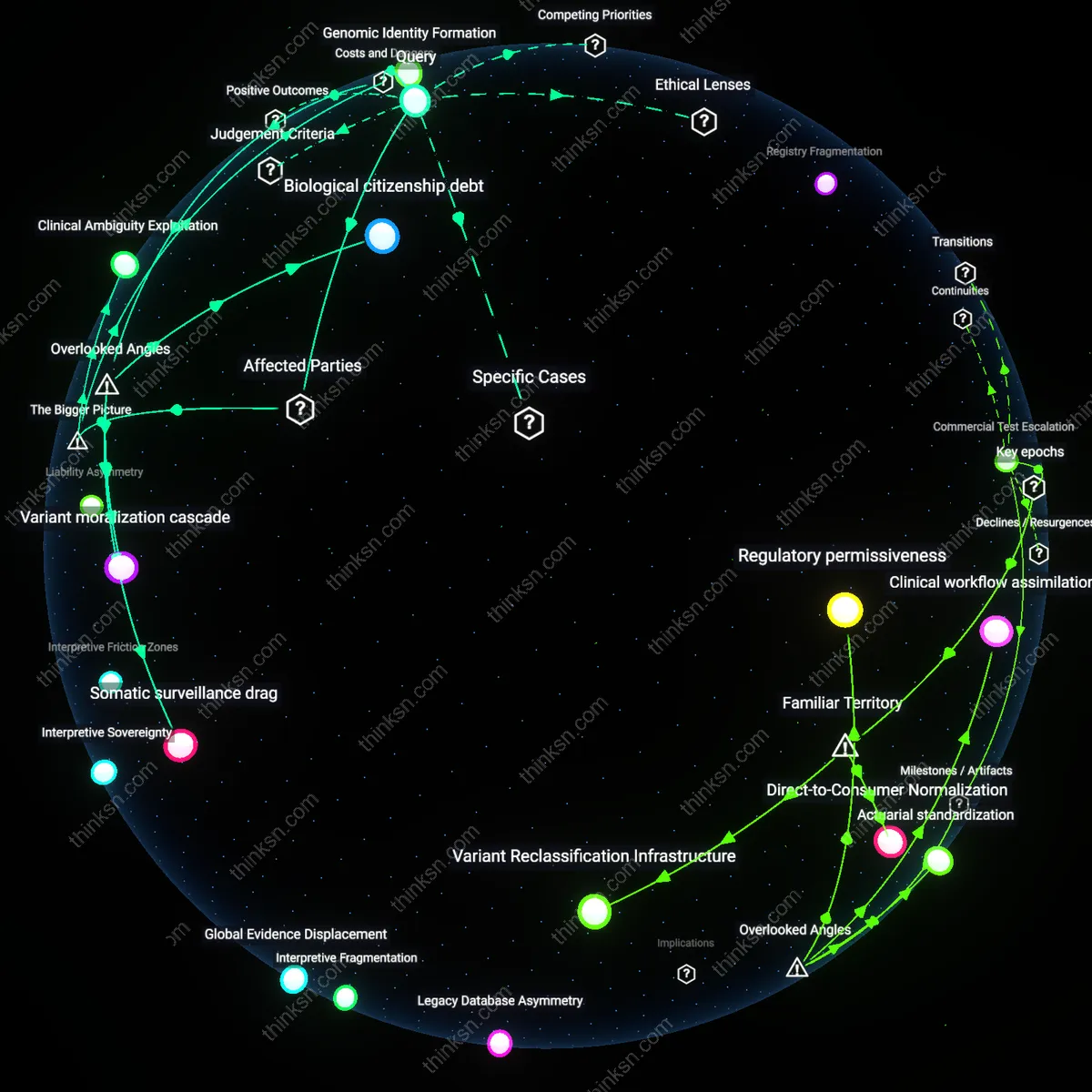
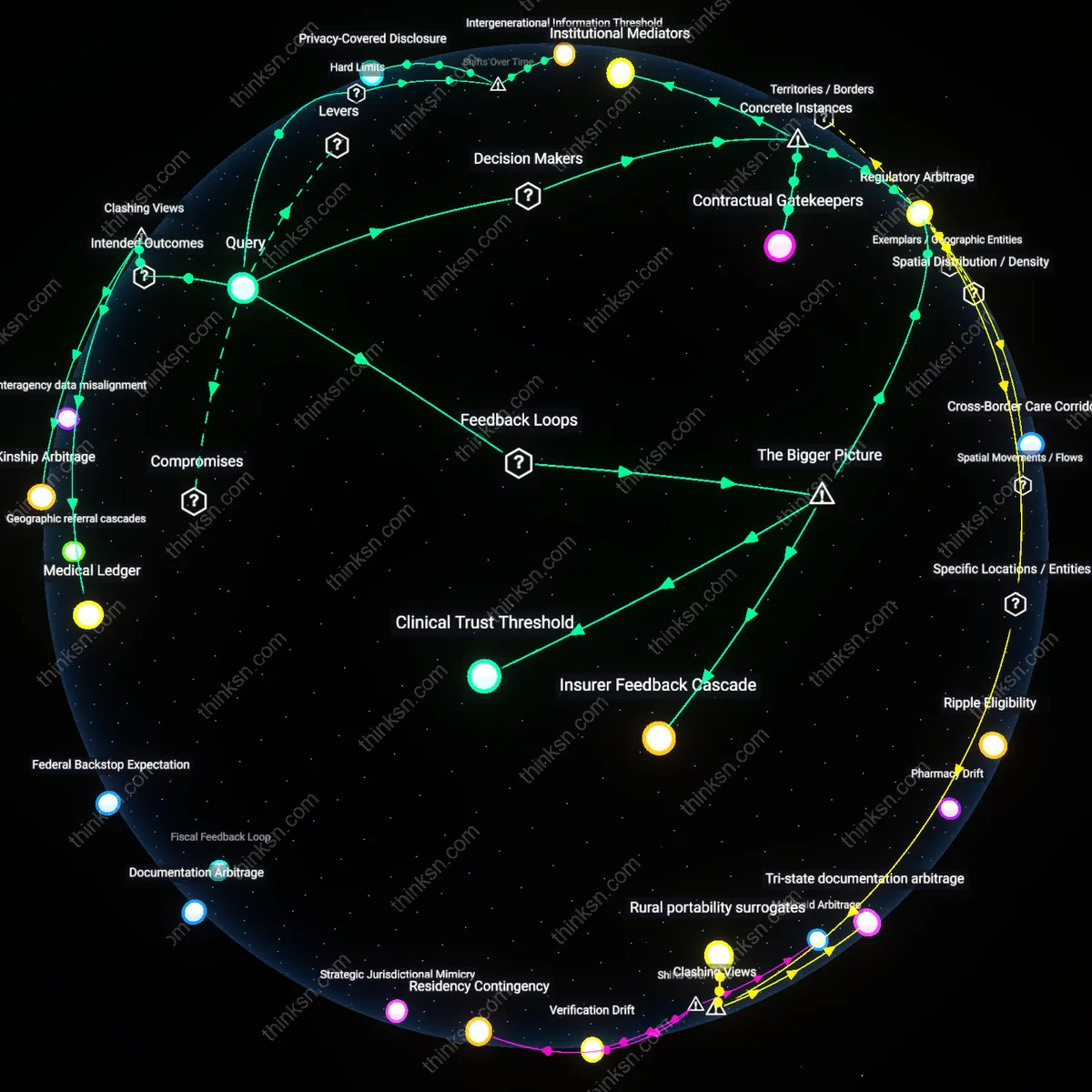
Can Insurance Cover Fertility Risks When Future Implantation Is Banned?
Analysis reveals 6 key thematic connections.
Key Findings
Regulatory Arbitrage
Insurance carriers began excluding fertility preservation coverage after 2015 state-level restrictions on embryo disposal emerged as a legal liability hedge, shifting risk assessment from medical necessity to jurisdictional compliance. As states like Louisiana and Indiana codified personhood frameworks that complicated embryo ownership and disposition, insurers recalibrated underwriting models to pre-empt litigation by treating implantation restrictions as de facto coverage voids. This pivot reflects an underappreciated shift from clinical actuarial logic to legal risk avoidance, where the insurability of medical services now depends on future legal enforceability rather than current treatment efficacy. The transformation reveals how reproductive medicine is increasingly governed not by health outcomes but by regulatory misalignment across state lines.
Jurisdictional Stratification
After 2020, national insurers began regionalizing fertility coverage tiers in response to divergent state laws on embryo status, adopting tiered risk pools that reflect legal geography more than medical risk. Carriers like UnitedHealthcare and Aetna reclassified patients not by diagnosis but by state of implantation eligibility, embedding future access barriers into underwriting algorithms as fixed risk multipliers. This evolution marks a departure from uniform clinical underwriting, exposing how reproductive risk is now stratified by legal destiny rather than biological potential, a transformation that institutionalizes geographic inequality within national insurance frameworks.
Regulatory Arbitrage Pressure
Insurance carriers restrict fertility preservation coverage in states with embryo personhood laws to preempt litigation exposure. By aligning benefit design with the strictest state-level legal interpretations—such as those in Alabama or Missouri where embryos are legally recognized as persons—insurers minimize the risk of future liability when implantation may be prohibited post-treatment. This preemptive narrowing of coverage reflects a systemic shift where legal risk, not medical need, determines benefit architecture, and it pressures self-insured employers and TPAs to replicate these restrictions across state lines even where not legally required. The non-obvious consequence is that national insurance products become de facto standardized to the most restrictive jurisdictions, amplifying legal exceptionalism into nationwide practice. Regulatory Arbitrage Pressure
Medical-Legal Misalignment
Clinical guidelines recommending immediate fertility preservation at cancer diagnosis conflict with insurance underwriting that delays approval until post-treatment legal status of embryos is clarified. Oncologists push for urgent cryopreservation to preserve reproductive options before gonadotoxic therapy, but insurers increasingly require legal affidavits or marital status verification to assess downstream implantation eligibility—creating treatment delays and coverage denials. This misalignment is systemically reinforced by ERISA’s fragmentation of health plan governance, allowing plan sponsors to impose moral clauses that medical bodies cannot override. The critical insight is that clinical urgency is being structurally disciplined by legal contingency, turning medical timing into a compliance metric. Medical-Legal Misalignment
Temporal Displacement Risk
Carriers assess fertility preservation risk not at the moment of cryopreservation but at an extrapolated future implantation date, because legal restrictions on embryo use invalidate the causal link between current intervention and future reproduction. For example, if a patient preserves embryos in California but anticipates living in a state with zygote personhood laws later, insurers may deny coverage by classifying preservation as futile or dissonant with intended outcomes. This temporal displacement—the decoupling of medical action from reproductive effect due to anticipated legal barriers—is rarely modeled in underwriting, yet determines whether a procedure is seen as causally generative of reproduction. The key overlooked factor is that insurers de facto project future legal environments onto present medical decisions, making prospective jurisprudence a covert actuarial variable.
Institutional Fertility Trajectory Mapping
Fertility clinics accredited by the Society for Assisted Reproductive Technology (SART) serve as de facto data gatekeepers whose reporting practices shape insurers’ risk evaluations, because carriers rely on clinic-mediated forecasts of post-treatment reproductive pathways to validate medical necessity. When clinics operate in multi-state networks like Reproductive Medicine Associates, they must navigate conflicting embryo disposition regulations, causing inconsistencies in how patient trajectories are documented—which in turn leads insurers to discount preservation claims where legal continuity is uncertain. The non-obvious dependency here is that insurance risk assessment is epistemically constrained by the granularity and legal awareness of clinical data entry, making administrative record-keeping standards an invisible but necessary precondition for reimbursement approval. Most analyses overlook how clinical bureaucracy mediates insurability.