When Insurers Deny Before Treatment, Do Rural Patients Lose Options?
Analysis reveals 10 key thematic connections.
Key Findings
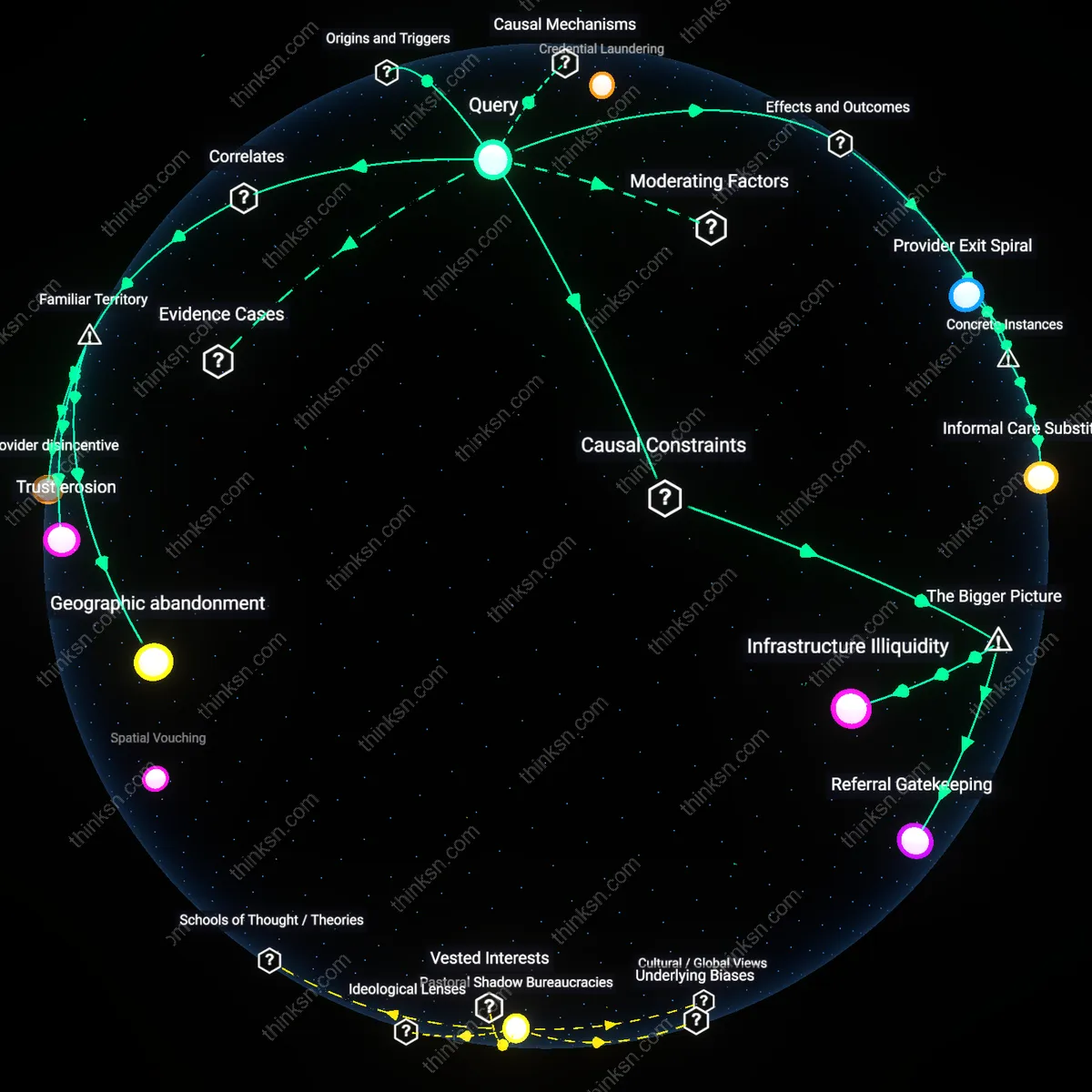
Preauthorization Sabotage
Early insurance denial restricts access to alternative healthcare providers in rural areas not because of patient income or geography, but because primary care gatekeepers exploit preauthorization protocols to consolidate control over specialist referrals. Rural clinics, often tied to regional health monopolies, weaponize early denials to prevent patients from seeking care outside their network—even when balance-billed options exist—by manipulating documentation requirements and delaying appeals until care becomes urgent or impractical. This reveals that the denial is less a financial filter than a territorial mechanism preserving provider dominance under the guise of cost containment, challenging the assumption that patients are excluded due to affordability alone.
Credential Laundering
Early insurance denial paradoxically expands access to unregulated alternative providers in rural areas by pushing patients toward practitioners who bypass insurance entirely and instead build legitimacy through community affiliations rather than medical accreditation. These providers—such as faith healers, traditional herbalists, or chiropractors operating cash-only—thrive because repeated denials discredit institutional medicine, allowing them to reposition themselves as liberatory alternatives despite lacking clinical oversight. This dynamic reframes denial not as a barrier but as a catalyst for delegitimizing biomedical gatekeeping, exposing how systemic failures are exploited to validate marginally recognized practices.
Carefronting
Early insurance denial forces rural patients to engage in carefronting—where they formally enroll with an approved provider solely to meet insurance criteria while covertly relying on alternative care from informal or distant networks coordinated through social ties, not medical institutions. This shadow system operates through kinship logistics, such as relatives in urban centers obtaining medications or telehealth access on their behalf, rendering official denial irrelevant but also rendering care invisible to public health tracking. It reveals that access is not lost but displaced into extralegal circuits, challenging the idea that denial equates to non-treatment and exposing the limitations of formal healthcare metrics in capturing actual care pathways.
Provider Exit Spiral
After Medicaid denials surged in 2017 for opioid treatment programs in McDowell County, West Virginia, clinics like the Appalachian Community Health Center reduced buprenorphine services due to uncollectable revenue, accelerating local physician burnout and practice closures. The withdrawal of providers following payer rejection illustrates how financial attrition operates faster than patient mobility, creating care deserts not from demand shifts but from eroded professional sustainability—revealing that denials trigger a self-reinforcing cycle where provider scarcity validates future payer underinvestment.
Informal Care Substitution
In the Navajo Nation’s Shiprock Chapter, early denials for diabetic wound care led patients to rely on traditional healers and community health aides after wound infections became unmanageable, transforming clinical pathways into hybrid systems where ceremonial and biomedical practices merge out of necessity. This adaptation demonstrates that when formal access breaks down, care does not vanish but reorganizes through culturally embedded substitutes—highlighting that insurance failure can quietly redirect medical dependence from licensed institutions to informal networks, a shift largely invisible in utilization metrics.
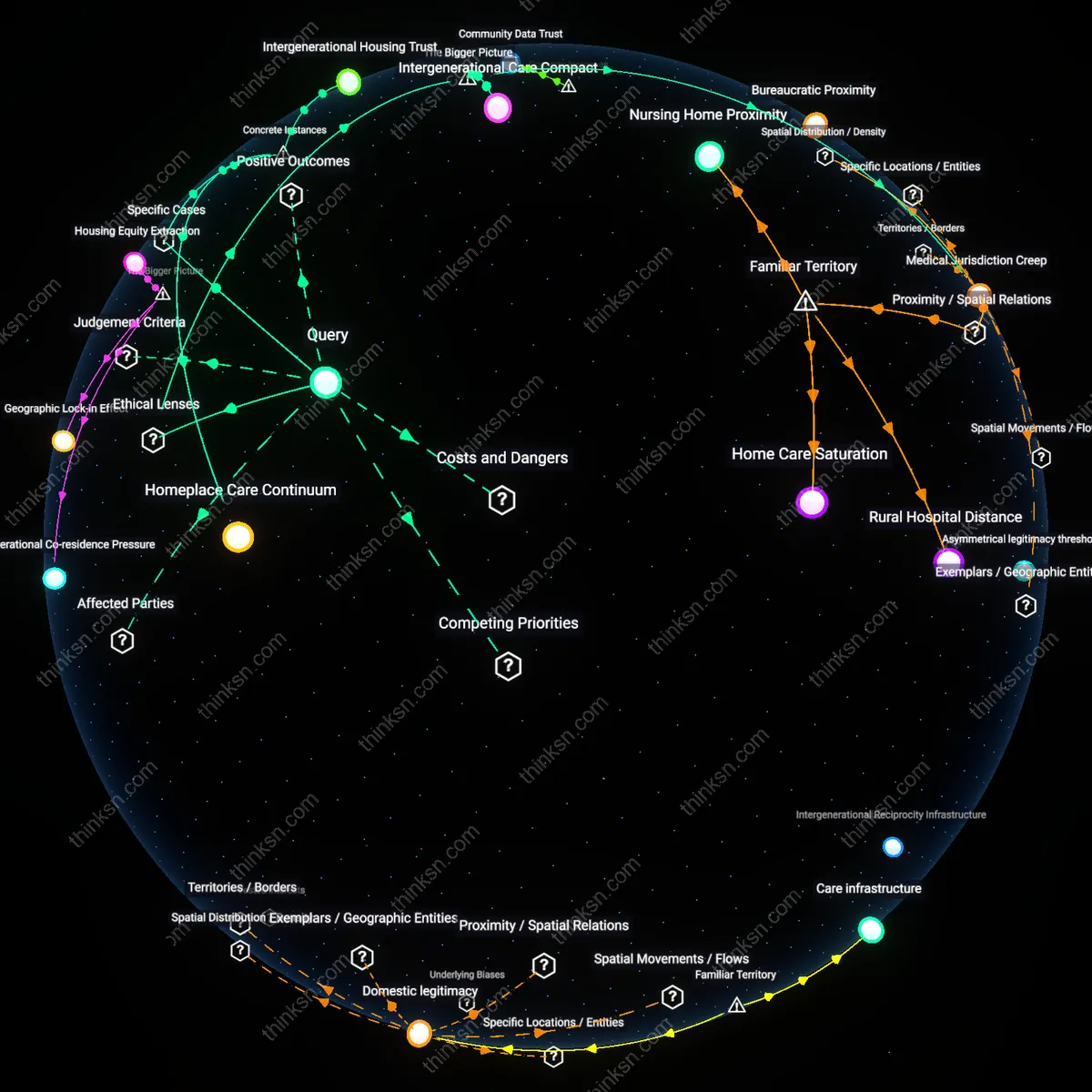
Geographic abandonment
Early insurance denial reduces patients’ ability to pay for care, which in turn decreases provider revenue in rural clinics, leading to clinic closures or service reductions. This occurs because rural healthcare facilities operate on thin margins and rely heavily on insured patient volume; when insurers reject claims early, providers lose anticipated income, forcing downsizing or exit. The non-obvious consequence under Familiar Territory is that denial doesn’t just block individual care but erodes the physical availability of care infrastructure itself—making distance to care a symptom, not a cause, of financial exclusion.
Trust erosion
Early insurance denial undermines patient confidence in formal healthcare systems, prompting reliance on informal or non-medical sources like community healers or family remedies. In rural areas, where personal networks are tightly woven and experiences with bureaucracy are uniformly negative, one denied claim becomes a shared cautionary signal. The underappreciated insight is that the denial doesn’t only limit financial access—it redefines the perceived legitimacy of providers, turning medical authority into just another unreliable institution.
Provider disincentive
When insurers deny claims early and frequently, healthcare providers in rural areas are less likely to join or remain in insurance networks, shrinking the list of accessible in-network options. This happens because the administrative burden and financial risk of pursuing appeals outweigh the benefits, especially in regions where provider shortages already limit competition. The overlooked reality is that insurance status doesn’t just affect patients—it actively shapes which providers are willing to serve them, making provider choice an artifact of payer policy, not local supply.
Referral Gatekeeping
Early insurance denial restricts patients’ access to alternative healthcare providers in rural areas by collapsing the referral cascade that funnels patients toward specialists or regional centers. Primary care providers in rural clinics often serve as gatekeepers to higher-level care, but without insurance pre-authorization, they cannot activate formal referral pathways—triggering an early breakdown in access. This bottleneck is enforced by payer-driven protocols that require documentation and approval before any downstream provider can bill, effectively disabling informal or urgent care workarounds. The non-obvious systemic tension here is that the gatekeeping role of rural physicians—intended to manage care—becomes a structural barrier when insurers withdraw financial sponsorship before care is even attempted.
Infrastructure Illiquidity
Early insurance denial freezes the latent supply of alternative healthcare providers in rural areas by making mobilization of spare or part-time clinical capacity economically infeasible. Rural regions often depend on visiting specialists, telehealth locum tenens, or mobile clinics—providers who require guaranteed reimbursement to justify travel and scheduling—but early denials remove revenue certainty and deter participation. This creates a liquidity crisis in care delivery infrastructure, where potential supply exists but cannot be activated without insurer signaling. The overlooked mechanism is that insurance approvals function as real-time market signals; their denial doesn’t just block payment—it suppresses provider entry into isolated care ecosystems.