Privacy vs Documentation: Family Struggles with Medical Information Transparency?
Analysis reveals 10 key thematic connections.
Key Findings
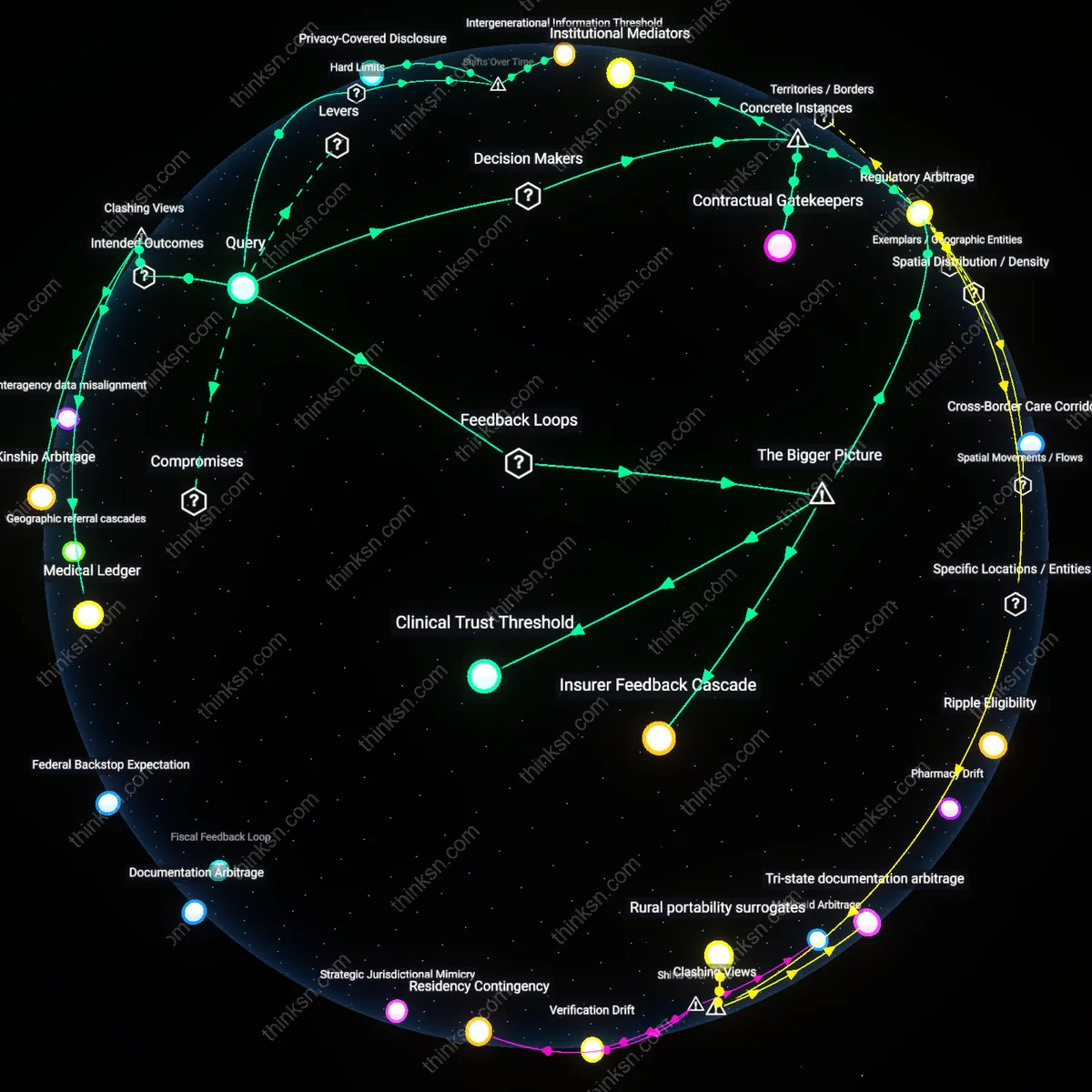
Privacy-Covered Disclosure
Families balance medical privacy and insurance transparency by restricting disclosure to data strictly necessary for adjudicating claims, a boundary solidified after the 1996 HIPAA regulations formalized minimum necessary standards in health information sharing. This mechanism involves insurers, healthcare providers, and family members negotiating access within legally defined zones of permissible use, operating through tiered authorization forms that evolved from post-HIPAA administrative simplification rules. The non-obvious insight is that the parent’s privacy is not overridden but reconfigured into a procedural right—dependent on timing, form, and scope—revealing how 1990s regulatory formalization shifted privacy from absolute control to conditional, context-bound permissions.
Intergenerational Information Threshold
Families manage privacy and transparency by deferring disclosure until a child reaches an age of recognized medical autonomy, a threshold that crystallized in the 2010s as state policies began uniformly recognizing adolescent consent for mental health and reproductive services. This shift reframed family decision-making around developmental milestones, embedding disclosure within pediatric care transitions managed jointly by parents, pediatricians, and insurers through graduated consent protocols. The underappreciated dynamic is that privacy is no longer a singular parental right but a phased transfer across time, exposing how post-2010 medicalization of adolescence has produced a new temporal boundary in insurance governance.
Claim-Contingent Consent
Families navigate privacy and documentation demands by tying parental consent to specific insurance claim events rather than blanket authorization, a practice institutionalized after the Affordable Care Act expanded dependent coverage to age 26 and increased audit scrutiny on family-based claims. This event-triggered model involves discrete, time-limited disclosures coordinated through patient portals and insurer verification systems, operating within post-2010 claims validation frameworks that require dated justification for data release. The overlooked dimension is that privacy is now episodically negotiated rather than statically assigned, revealing how regulatory stress on claims integrity has transformed consent into a transactional checkpoint rather than a continuous status.
Regulatory Arbitrage
Institutionalizing dual-tier documentation systems within regional health networks creates a buffer between parental privacy rights and insurer transparency demands. By formalizing distinct clinical record pathways—one for insurers requiring auditable care justification, another for private use—health systems in states like Massachusetts under Chapter 221 regulations enable families to submit minimally invasive data while preserving autonomy. This governance duality stabilizes feedback because it acknowledges payer accountability cycles without triggering privacy escalation loops, a mechanism often overlooked when compliance is assumed to erode patient rights uniformly. A subtle enabling condition is state-level variation in medical confidentiality statutes, which providers can leverage to resist data overreach without violating federal transparency mandates.
Insurer Feedback Cascade
Implementing tiered claims review protocols based on disclosed diagnosis sensitivity alters how payers influence medical privacy thresholds. When private insurers like UnitedHealthcare deploy risk-adjusted adjudication tiers—where mental health or genetic conditions undergo lighter documentation scrutiny—they reduce systemic pressure on families to over-disclose, thus weakening a key reinforcing loop between stringent verification and privacy erosion. This mechanism emerges from the interplay between actuarial fairness norms and litigation risk, which insurers are incentivized to balance regionally, particularly in markets with concentrated provider networks like Minnesota’s HealthPartners system. The underappreciated insight is that insurance adaptability, not just regulation, can initiate balancing loops in privacy-transparency conflicts.
Clinical Trust Threshold
Shifting care documentation initiation from insurers to trusted primary care entities, such as federally qualified health centers in rural Oregon, relocates authority over medical disclosure and disrupts the self-reinforcing cycle of invasive verification. By embedding documentation roles within longitudinal patient-clinician relationships, these centers cultivate threshold levels of trust that permit selective data release—neither fully opaque nor universally transparent—and align with both HIPAA allowances and state insurance codes. The key systemic dynamic is that proximity to care determines data consent stability, an often-ignored spatial determinant of privacy policy effectiveness. This repositioning sustains balance by making transparency contingent on clinical, not financial, validation cycles.
Institutional Mediators
Healthcare systems like Kaiser Permanente have established internal ethics boards that adjudicate conflicts between HIPAA-protected patient privacy and insurer requests for medical documentation, allowing families to withhold sensitive information while still satisfying audit requirements through redacted summaries reviewed by a third-party clinical panel. This mechanism shifts resolution from legal confrontation to clinical governance, revealing that intermediary bodies within integrated care networks can function as binding arbiters without requiring family members to directly disclose or deny information, a role often overlooked in privacy debates dominated by court-centric models.
Contractual Gatekeepers
In 2018, UnitedHealthcare revised its group insurance policies for corporate clients like Amazon, introducing a clause that requires employers—not employees—to verify medical necessity before releasing documentation, thereby positioning the employer as a contractual buffer between parent, insurer, and healthcare provider. This reconfiguration transfers the burden of transparency compliance away from the individual family and embeds privacy protection within employment-based insurance architecture, exposing how liability-shifting in private insurance contracts can quietly rewire access without legislative change.
Medical Ledger
Families can reconcile medical privacy and insurance transparency by designating a trusted third-party health fiduciary—a role increasingly available in states like California and Massachusetts—who receives, redacts, and forwards only clinically and legally necessary data to insurers; this creates a boundary object that satisfies claims requirements without exposing sensitive diagnoses or treatment histories to family members or insurers. The mechanism operates through HIPAA-compliant data stewardship frameworks used in integrated delivery networks such as Kaiser Permanente, where audit trails and role-based access control limit exposure—what is underappreciated is that privacy is not breached by disclosure per se, but by unstructured access, and the non-intuitive solution is not withholding information but routing it through a regulated intermediary. This reframes the conflict not as a moral dilemma between transparency and confidentiality, but as a systems design problem in information architecture.
Kinship Arbitrage
Families maintain privacy by strategically assigning the insured role to the parent with the least medical vulnerability, leveraging asymmetries in plan enrollment rules across employer-sponsored policies—such as those offered by the University of Michigan or Intel—to minimize disclosure burden while retaining coverage integrity. This exploits a misalignment between insurance underwriting logic, which assesses individual risk, and family benefit structures, which pool access; the result is that privacy becomes a resource allocated to the most exposed member by shifting administrative visibility onto the healthier parent. The underappreciated reality is that privacy in family medicine is not equally distributed but is actively traded—challenging the assumption that transparency demands are uniformly binding, and instead showing they can be navigated through tactical kinship positioning within regulatory loopholes.