Rare Disease Biologics on Specialty Tiers: Innovation or Inaccessibility?
Analysis reveals 8 key thematic connections.
Key Findings
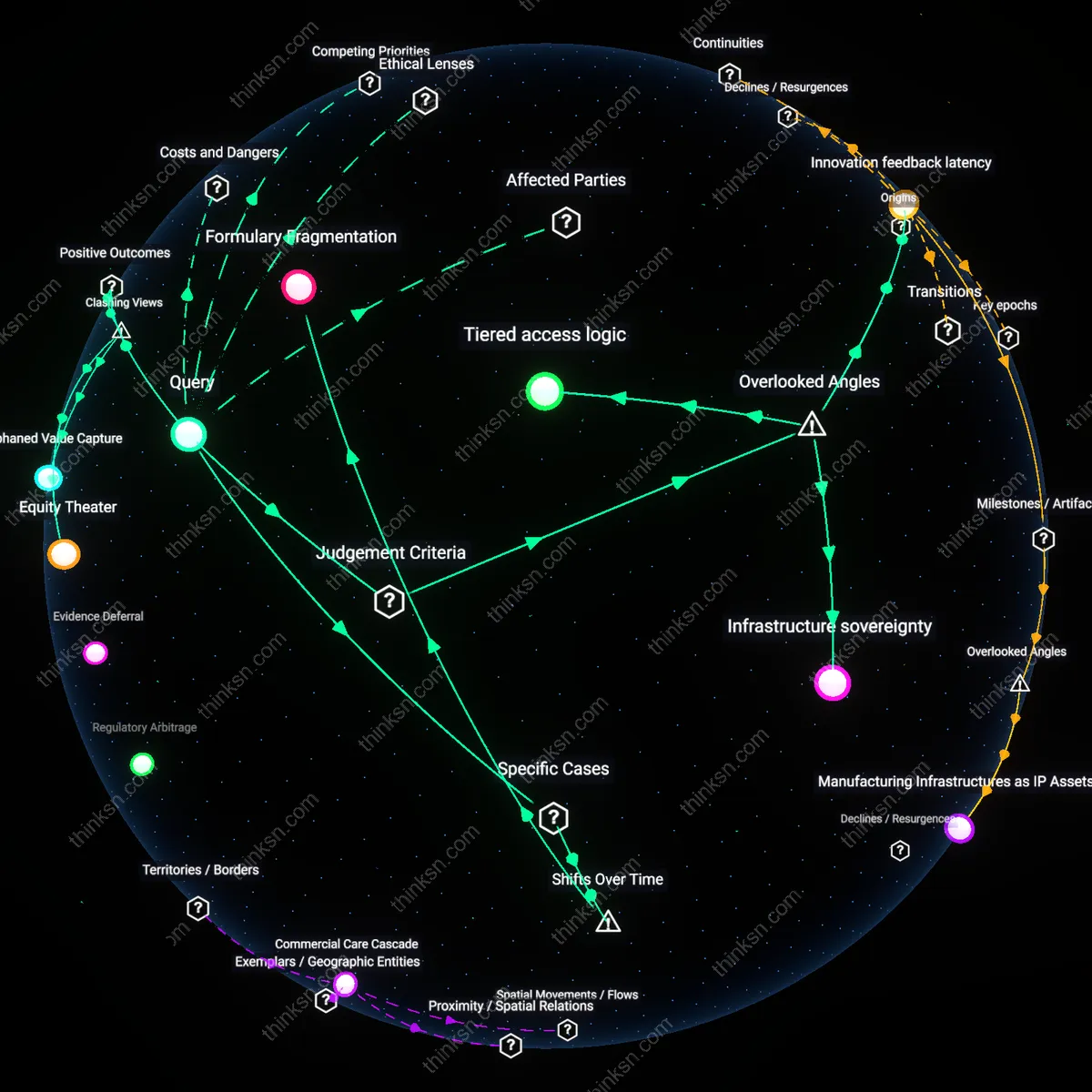
Tiered access logic
Placing a new biologic for a rare disease on a specialty tier reveals that payer formularies use tiered cost-sharing not merely as a financial tool but as a governance mechanism to delegate drug allocation decisions to prescribing physicians, thereby embedding clinical judgment within economic constraints. Specialty tiers function as a boundary object where insurers shift the burden of cost-benefit evaluation to prescribers—especially specialists—effectively making oncologists or geneticists the gatekeepers of access, despite those clinicians lacking direct economic accountability. This dynamic is overlooked because standard discourse frames tiering as a pricing outcome rather than a distributed decision-making architecture, obscuring how clinical authority is co-opted to absorb ethical trade-offs. The non-obvious implication is that equity concerns are not just fiscal but distributed across professional hierarchies, altering where moral responsibility is located.
Infrastructure sovereignty
The placement of rare disease biologics on specialty tiers reveals that equitable access is structurally constrained by the geographic concentration of specialized pharmacies and certified prescribers, often located in urban academic medical centers, which means the drug’s availability is mediated by logistical infrastructure more than insurance coverage alone. Patients in rural or underserved regions may have technically 'covered' access but face effective denials due to distributional bottlenecks—such as mandatory enrollment in proprietary hub systems or limited shipping networks—that are rarely included in access debates. This dependency on physical and digital distribution chains is typically ignored in moral and economic analyses focused on price or rationing, yet determines the actual usability of a benefit; the overlooked variable is that access infrastructure exerts a hidden sovereignty over who can be treated, reshaping the geography of therapeutic justice.
Innovation feedback latency
By assigning high-cost biologics to specialty tiers, payers create a delay between regulatory approval and real-world prescribing that distorts the innovation ecosystem, because manufacturers and researchers receive feedback about clinical utility only slowly and from a narrow, selected cohort of early adopters. This latency in usage data generation undermines iterative improvement cycles in rare disease research, where patient numbers are too small to absorb even minor delays or sampling biases. Most innovation incentives assume rapid knowledge accumulation, but tiering introduces a temporal friction that skews future investment—especially for next-generation therapies dependent on early clinical signals. The overlooked insight is that access barriers do not just constrain equity but corrode the epistemic foundation of future innovation, turning distributional delays into long-term cognitive costs for medical discovery.
Innovation Signaling
Placing a new biologic for a rare disease on a specialty tier accelerates insurer-driven recognition of clinical novelty, which in turn triggers faster formulary learning curves across health systems. This mechanism transforms payer categorization into a de facto validation signal that reduces information asymmetry among providers and pharmacy benefit managers, thereby streamlining off-label adoption for related conditions. The non-obvious outcome is that tier placement functions not as a barrier but as a dissemination engine—one where reimbursement policy becomes an underrecognized conduit for medical diffusion, challenging the assumption that specialty tiers primarily restrict access.
Equity Theater
Positioning a rare disease biologic on a specialty tier allows public and private payers to simulate equitable access while maintaining tight utilization controls, thereby satisfying stakeholder expectations of fairness without structural redistribution. The tier becomes a ritualized performance of inclusion, where the appearance of coverage deflects regulatory scrutiny and patient advocacy pressure even when actual dispensing remains constrained by prior authorization and narrow provider networks. This reveals that access architecture can be optimized for political legitimacy rather than clinical availability, contradicting the intuitive linkage between formulary placement and realized care.
Orphaned Value Capture
Assigning a new rare disease biologic to a specialty tier enables manufacturers to extend value extraction beyond the targeted patient cohort by anchoring future pricing benchmarks for more common indications. Because the tier isolates the drug from cost-effectiveness comparisons with mainstream therapies, it creates a protected pricing zone that severs the link between prevalence and price formation. The underappreciated mechanism is that rarity, when codified in tiering systems, becomes a regulatory loophole for value arbitrage—flipping the narrative of rare disease drugs as commercially risky into a strategic advantage for portfolio-level monetization.
Tiered Access Regime
Placing a new biologic for a rare disease on a specialty tier reveals the institutionalization of differential access as a normalized market mechanism following the shift from cost-based to value-based pricing models in the 2010s. As payers like UnitedHealthcare and Express Scripts adopted tiered formularies to manage expensive specialty drugs—such as Spark Therapeutics’ Luxturna (2018), priced at $850,000 per eye—their classification as 'specialty' functioned less as a reimbursement category and more as a gatekeeping apparatus that embedded actuarial risk assessments into patient eligibility. This system reframed equitable access not as a medical imperative but as a financial contingency calibrated to projected long-term savings, exposing a quiet transition where innovation incentives became structurally dependent on access restriction.
Formulary Fragmentation
The assignment of Vertex’s $2.2 million hemophilia B therapy, exagamglogene autotemcel (2024), to specialty tiers illustrates how the consolidation of pharmacy benefit managers (PBMs) like CVS Caremark and Cigna into vertically integrated gatekeepers since the mid-2010s has fragmented formularies along actuarial lines. Where uniform coverage was once the benchmark of insurance adequacy, the present system stratifies access by disease rarity, drug modality, and projected budget impact, converting the formulary from a transparency tool into a dynamic risk allocation device—highlighting a shift where innovation is sustained through intentional, institutionally sanctioned variability in access.