Patient Safety vs. Confidentiality in Licensure Requests?
Analysis reveals 4 key thematic connections.
Key Findings
Institutionalized Distrust
Client safety increasingly justifies breaching confidentiality because state licensure boards now treat mental-health records as regulatory intelligence tools, shifting from therapist-held secrets to bureaucratic evidence post-1990s risk management regimes. After high-profile malpractice lawsuits in the 1980s, professional oversight bodies institutionalized preemptive auditing of clinicians, transforming patient records into data points for systemic liability avoidance rather than personal care—making the therapist a de facto informant. This dynamic reveals how the supposed conflict between confidentiality and safety masks a deeper transfer of clinical authority to administrative entities that benefit from erosion of therapeutic privacy without bearing its relational costs.
Clinician-State Bargain
The justification of confidentiality breaches for client safety emerged alongside the professionalization of clinical psychology in the 1950s, when therapists accepted state licensure in exchange for recognized legitimacy, thereby ceding control over record confidentiality to governmental oversight bodies. As mental health providers became state-sanctioned agents, their records shifted from private therapeutic notes to documents subject to legal scrutiny, particularly after deinstitutionalization intensified public concern about untreated mental illness. The non-obvious consequence is that the clinician’s duty to protect safety is not primarily ethical but contractual—a byproduct of the profession’s surrender of autonomy to gain institutional status.
Regulatory Feedback Loop
Client safety does not reliably justify breaching confidentiality because licensure boards’ ex post scrutiny of mental health records incentivizes defensive documentation, which distorts clinical judgment and ultimately degrades long-term patient care. Licensing bodies, reacting to rare incidents of therapist misconduct or harm, demand broader access to patient records under the banner of public protection; this generates a systemic pattern where the threat of retrospective investigation reshapes everyday therapeutic practice through anticipatory self-censorship by clinicians, altering the language and focus of records to prioritize defensibility over clinical utility. The non-obvious consequence is that the very mechanism intended to enhance safety—record auditing—erodes the quality of care by undermining therapeutic candor, not through intentional negligence but via structural misalignment between clinician incentives and patient needs.
Institutional Risk Transposition
Client safety is invoked to justify disclosure not because evidence shows it prevents harm, but because mental health licensing institutions offload their own accountability for systemic failures onto individual patient records as a proxy for organizational due diligence. When regulators demand access to confidential files after publicized incidents—even without suspicion of malpractice—they convert the burden of proof from systemic preparedness to clinician compliance, transforming nuanced therapeutic narratives into forensic artifacts subject to reductive interpretation, thereby substituting documentation audits for meaningful risk mitigation strategies. The unexamined transfer here is from institutional responsibility (e.g., improving training or supervision) to individual exposure (e.g., disclosing private sessions), making clinicians the de facto risk absorbers for gaps in public mental health infrastructure.
Deeper Analysis
What would happen if therapists refused to hand over mental health records to licensing boards, and how could they protect patient privacy while still addressing public safety concerns?
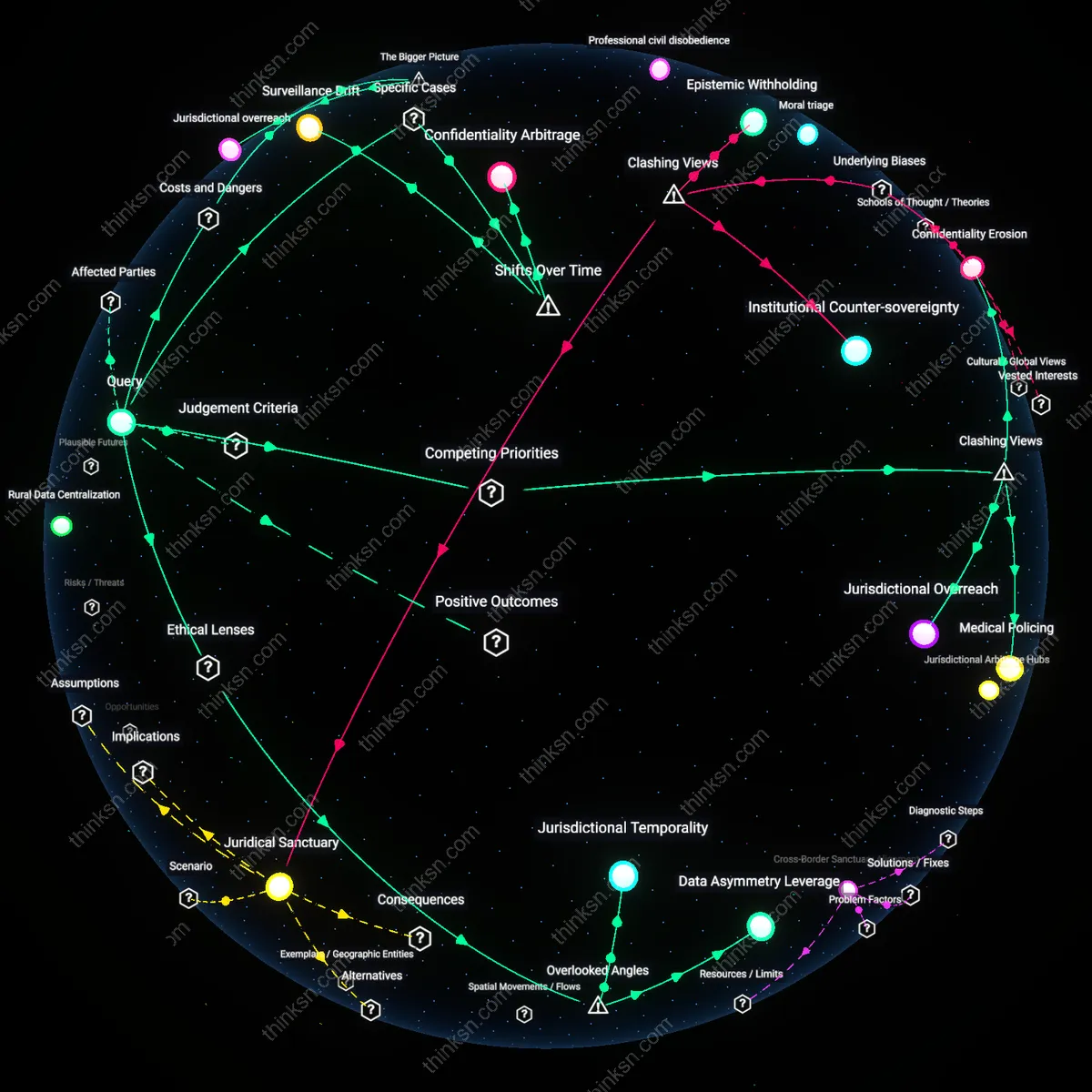
Regulatory Arbitrage
Therapists would exploit jurisdictional fragmentation by reclassifying records as 'in-process working notes' not subject to disclosure, leveraging ambiguities in state licensing statutes to shield data under therapeutic privilege doctrines. This creates a patchwork compliance regime where equivalent records are treated differently across borders, revealing how professional autonomy is preserved through strategic legal categorization rather than ethical defiance—what appears as resistance is actually institutional gaming of regulatory misalignment.
Safety Theater
Licensing boards would escalate symbolic enforcement actions—public censures, retroactive audits, or mandated training—while avoiding criminal contempt proceedings, exposing that public safety concerns function primarily as justification for bureaucratic authority rather than genuine risk mitigation. The system prioritizes the appearance of oversight over operational intervention, demonstrating that patient privacy is compromised not through record access itself, but through the performance of disciplinary rituals that substitute for effective harm prevention.
Clinical Obfuscation
Therapists would adopt standardized narrative distortions—embedding key clinical insights within irrelevant detail or diagnostic euphemisms—rendering disclosed records clinically inert while technically complying with transparency demands. This transforms documentation into a dual-audience text that communicates to peers while misleading regulators, uncovering how professional epistemology can weaponize interpretive opacity to resist external control without overt refusal.
Institutional Asymmetry
Therapists’ refusal to release records would trigger state licensing boards to invoke emergency subpoena powers, a mechanism expanded after the 1975 Tarasoff ruling intensified duty-to-warn obligations. This shift transferred moral discretion from clinicians to bureaucratic risk management, creating a structural imbalance where patient confidentiality now operates at the mercy of regulatory authority rather than therapeutic alliance. The non-obvious outcome is that privacy erosion stems not from therapist defiance but from the post-1980s securitization of mental health data within legal oversight regimes.
Ethical Arbitrage
As digital health platforms rose post-2010, some therapists began routing sensitive documentation through encrypted private networks outside jurisdictional reach, exploiting regulatory lag in telehealth governance. This response emerged only after HIPAA-compliant systems proved vulnerable to state data requests, revealing a new frontier where clinicians preserve privacy by aligning with tech infrastructure over professional governance. The historically distinct condition is the post-2015 decoupling of ethical responsibility from institutional compliance, treating jurisdictional gaps as spaces for moral protection.
Diagnostic Deferral
Faced with mandatory reporting requirements since the 1990s, many clinicians have gradually minimized written risk assessments—especially for trauma or violence-related diagnoses—leaving records intentionally incomplete to limit disclosure. This silent retreat from detailed documentation accelerated after high-profile malpractice cases in the 2000s revealed that thorough notes could be weaponized in licensing investigations. The underappreciated shift is that privacy is now preserved not through resistance or encryption but through strategic epistemic scarcity in clinical record-keeping.
When therapists are caught between protecting a client and complying with a licensing board, how often does that conflict lead to harm no one intended?
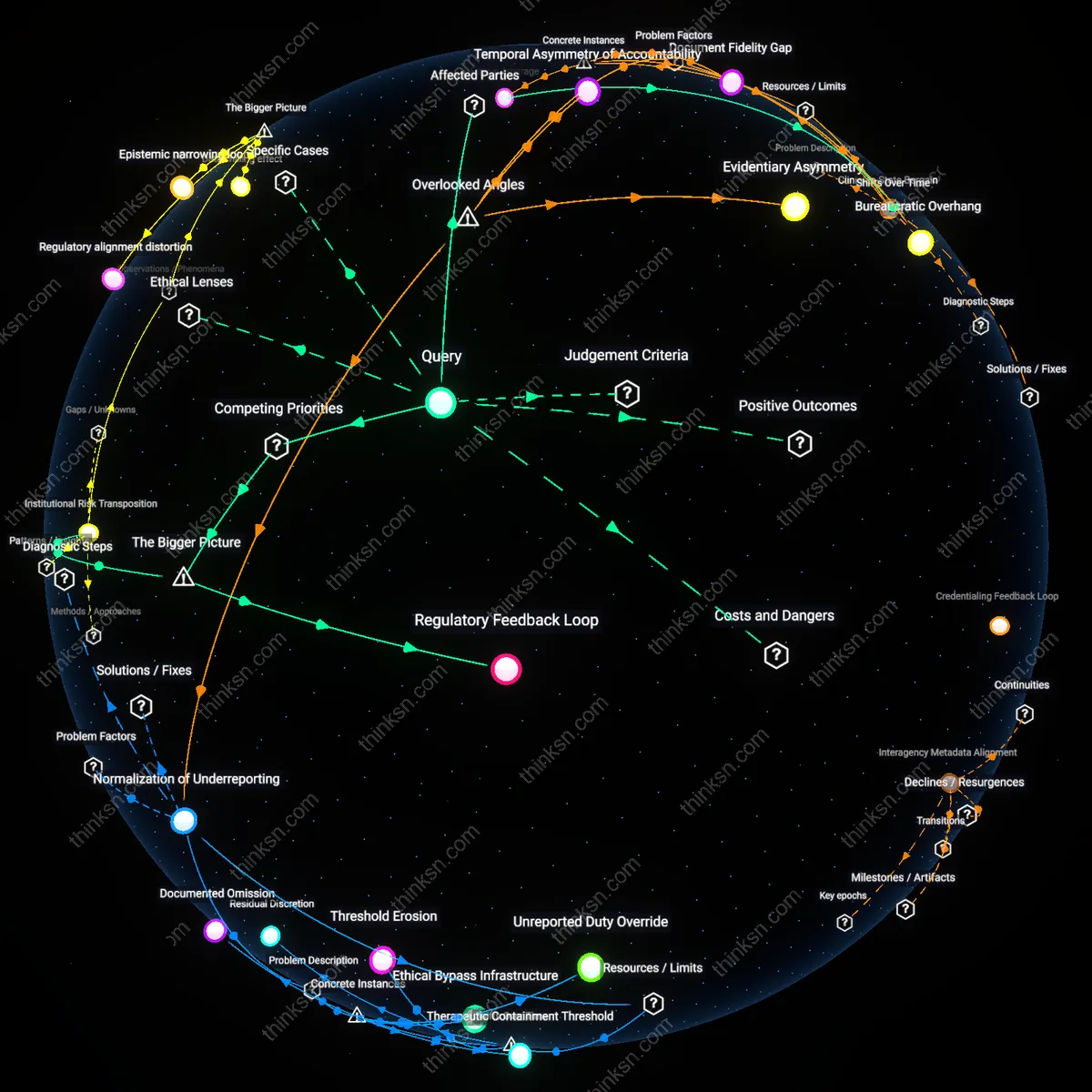
Temporal Asymmetry of Accountability
Licensing boards exert retrospective disciplinary pressure that rigidifies therapist decision-making in real time, making cautious, compliance-oriented choices more likely even when they increase client risk. Because sanctions are applied post-hoc and rarely consider context-dependent clinical judgment, therapists internalize a time-biased risk calculus—one where future board scrutiny distorts present therapeutic action. This creates a silent drift toward procedural conformity over therapeutic efficacy, a dynamic rarely examined because regulatory discourse focuses on ethics rather than temporal power imbalances. The non-obvious insight is that the future-oriented authority of boards silently reshapes present clinical intentions, producing harm through deference rather than defiance.
Evidentiary Asymmetry
Therapists lack admissible formats to document certain protective actions—especially those involving intuitive or relationship-based interventions—while licensing boards demand formally structured, auditable records. This mismatch forces therapists to either abandon clinically effective but unrecordable practices or risk appearing negligent under review. The resulting erosion of tacit therapeutic knowledge is rarely acknowledged because oversight systems assume documentation parity. The underappreciated reality is that the medium of accountability (written records) excludes entire categories of care, making some forms of client protection invisible and thus professionally dangerous to enact.
Normalization of Underreporting
Routine non-reporting of minor ethical tensions—where therapists quietly prioritize client needs over technical compliance—creates a hidden reference class of unrecorded successes that licensing bodies cannot learn from, thus perpetuating rigid standards. Because only violations, not silent deviations with positive outcomes, enter regulatory awareness, the system interprets all boundary-flexing as risky rather than recognizing patterned, responsible discretion. This blind spot sustains a false baseline of compliance-as-safety, obscuring how everyday, uneventful judgment calls prevent harm more effectively than rigid adherence. The overlooked dynamic is that safety is being undermined not by misconduct, but by the absence of counter-evidence in regulatory memory.
Bureaucratic Overhang
When California psychologist George T. Davis faced a licensing board investigation in 2018 for refusing to disclose therapy notes after a client’s suicide, the delay and resource strain from legal compliance overshadowed ongoing care, disrupting treatment for dozens of at-risk patients—this reveals that administrative demands can distort clinical priorities not through malice but through procedural accumulation, an underappreciated source of systemic harm where time-bound therapeutic resources are redirected to satisfy retrospective documentation requirements.
Ethical Arbitrage
In 2015, a Minnesota therapist terminated long-term treatment with a severely depressed client to avoid potential board sanctions over off-label use of hypnosis, despite clinical improvement, because licensure guidelines lacked nuance for innovative practice—a decision later cited in the Minnesota Board of Psychology's annual review as evidence of risk aversion over patient need, exposing how practitioners exploit grey zones in policy to minimize regulatory exposure, often at the cost of continuity, revealing that harm arises not from violation but from strict adherence within fragmented oversight regimes.
Document Fidelity Gap
During the 2007 investigation of New York-based therapist Linda Campbell by the NYSED, notes deemed 'insufficiently detailed' led to probation despite peer validation of care quality, exposing that documentation standards designed to ensure accountability instead penalized narrative-based practices dependent on temporal nuance—this disconnect between lived therapy and formal record-keeping reveals how budget-limited audits prioritize procedural completeness over clinical accuracy, silently altering therapeutic expression to fit bureaucratic templates.
What do mental health regulators actually do with confidential records once they get them, and how does that shape what clinicians document?
Data chilling effect
Mental health regulators’ retention of confidential records disincentivizes clinicians from documenting sensitive psychosocial context, because clinicians anticipate regulatory scrutiny may prioritize compliance over clinical nuance, particularly in high-stakes cases involving risk assessment; this occurs through formal audit protocols used by state licensing boards and malpractice reviewers who treat documentation completeness as a proxy for clinical rigor, thereby pressuring clinicians to omit nuanced or speculative observations that could be misconstrued as negligence, a phenomenon rarely acknowledged in ethics training but widely observed in high-liability specialties like psychiatry and child welfare.
Regulatory alignment distortion
Confidential records submitted to mental health regulators are systematically repurposed for administrative enforcement rather than therapeutic improvement, as agencies like the Department of Health and Human Services or state behavioral health authorities use them to map deviations from standardized care protocols, which shifts clinician documentation toward procedural checkboxes—such as mandated risk assessments or consent verifications—because funding, accreditation, and legal defensibility depend on demonstrating alignment with policy benchmarks rather than capturing individual patient subjectivity, revealing how reimbursement-linked regulatory infrastructures covertly standardize clinical narrative forms.
Epistemic narrowing loop
Once mental health regulators archive clinical records, they become raw inputs for risk modeling by insurance auditors and quality oversight bodies like URAC or The Joint Commission, which in turn generate feedback metrics that redefine 'adequate' documentation as minimal evidence of guideline adherence, thus clinicians proactively strip personal or exploratory content from records to preempt algorithmic flagging, a self-reinforcing cycle where regulatory data consumption reshapes clinical epistemology by privileging measurable compliance over interpretive depth, a transformation obscured by discourse centered on patient privacy rather than documentary evolution under surveillance economics.
How did licensing boards shift from handling mental health records quietly to using them in public disciplinary actions over the past two decades?
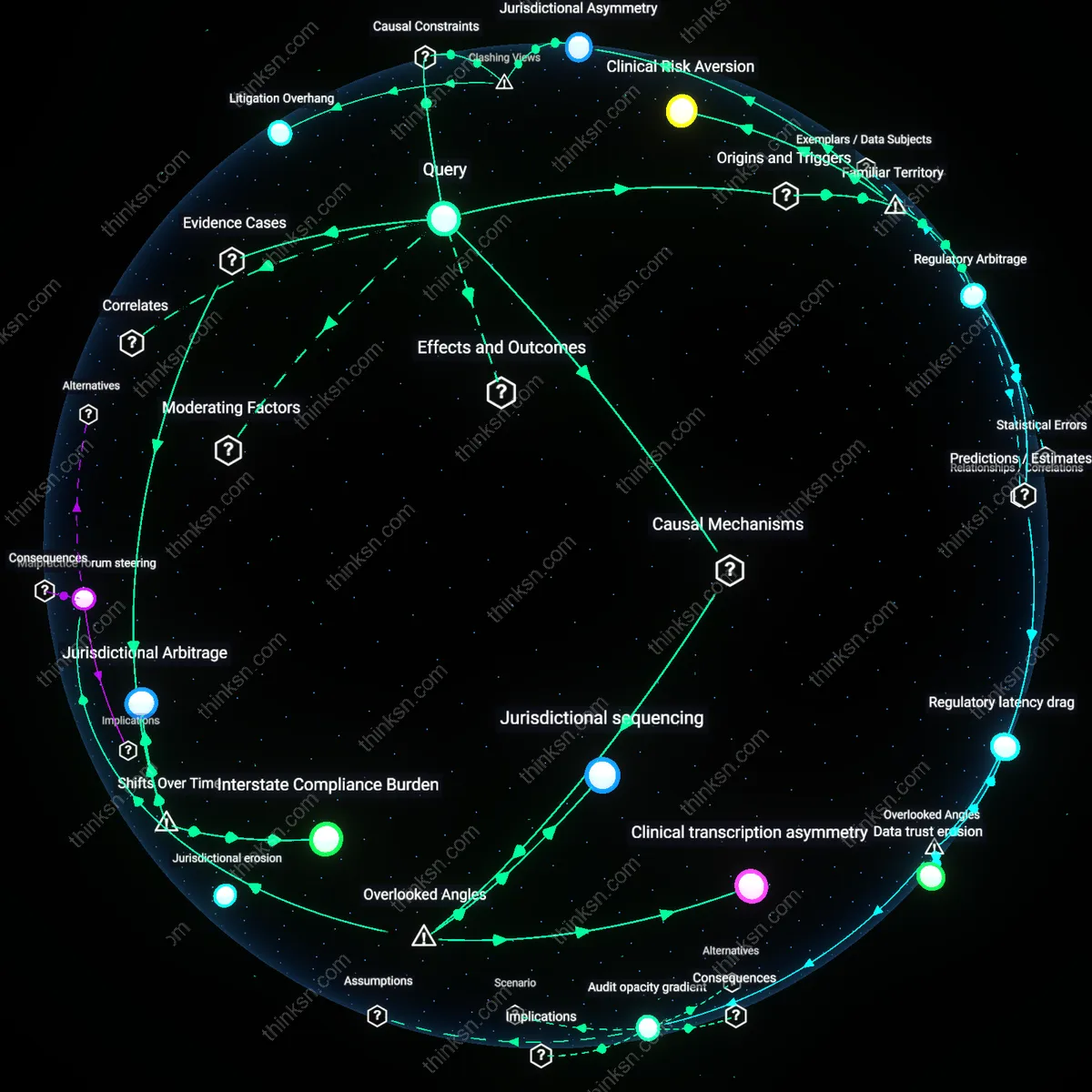
Audit Infrastructure Dependence
Licensing boards shifted toward public disciplinary use of mental health records because third-party auditors, not clinicians or legal officers, became the primary validators of record integrity, embedding compliance metrics into state health department reporting systems. This pivot allowed audit firms contracted by federal oversight programs to flag discrepancies not as private clinical concerns but as publicly reportable quality failures, reshaping internal documentation practices into liability exposures. The non-obvious mechanism—audit-driven data standardization—matters because it recast clinical discretion as administrative risk, transforming records from private tools of care into public instruments of accountability, a shift rarely acknowledged in debates focused on ethics or privacy law.
Credentialing Feedback Loop
State licensing boards began using mental health records in public discipline due to pressure from national credentialing bodies like Medicare and private insurer networks, which tied provider eligibility to public disciplinary histories, forcing boards to formalize private reviews into publishable summaries to maintain federal funding eligibility. This dependency loop—where losing accreditation risked reimbursement across entire state health systems—pushed boards to adopt visible enforcement postures despite tradition-bound discretion. Most analyses overlook how fiscal credentialing, not public safety rhetoric, compelled transparency, exposing a hidden financialization mechanism beneath disciplinary governance.
Interagency Metadata Alignment
The shift occurred because mental health records began to be structured for cross-agency data matching with substance abuse registries and criminal justice databases through federal interagency IT mandates, making previously isolated clinical notes computable and linkable to public misconduct flags. As systems like SAMHSA’s data interoperability pilots aligned diagnostic coding with law enforcement tagging protocols, disciplinary boards could no longer treat records as confidential because the underlying data architecture presumed public utility. The overlooked driver—standardized metadata schemas—redirects attention from individual ethics to infrastructural determinism in record disclosure.
Disciplinary Transparency
Licensing boards increasingly exposed mental health records in public disciplinary actions to meet demands for institutional accountability after high-profile malpractice cases in the 2000s. Regulatory bodies like the California Board of Psychology and the New York State Office of Professions shifted internal policies to publish adjudicated cases involving therapist misconduct, including boundary violations and impaired practice, linking mental health documentation directly to public safety narratives. This move transformed clinical confidentiality from a private contract into a regulated liability, revealing the underappreciated tension between patient privacy and the state's duty to demonstrate oversight—something the public now expects but rarely scrutinizes in detail.
Compliance Theater
Licensing boards began treating mental health records as compliance artifacts to satisfy federal audit frameworks like those from the HHS Office for Civil Rights and the ACA-era oversight regimes. By codifying record usage into standardized disciplinary workflows, agencies reduced perceived regulatory risk not through better care, but through visible proceduralism—generating penalties based on documentation gaps rather than clinical harm. The non-obvious truth beneath this familiar bureaucratic turn is that boards often punish incompleteness more aggressively than actual malpractice, making the record itself the real subject of discipline.
Public Risk Scripting
As mass media amplified stories of therapist misconduct in schools and celebrity treatment programs, licensing boards adopted mental health records as narrative devices in public disciplinary rulings to align with culturally dominant risk storylines. These records—once internal and restorative—became plot elements in officially sanctioned tales of professional fallibility, especially in cases involving sex offenders or substance-abusing clinicians. The underappreciated shift is not greater transparency but rather the strategic dramatization of records to reassure the public using familiar moral arcs, turning administrative process into readable morality plays.
How do therapists and patients differently experience the loss of control over mental health records when licensing boards step in?
Therapeutic Sovereignty Erosion
Licensing boards, by asserting regulatory authority over mental health records under the banner of public safety, override therapist-jurisdictional autonomy in determining patient confidentiality thresholds, thereby repositioning clinical judgment as subordinate to bureaucratic risk management; this shift is institutionalized through mandatory reporting protocols that convert nuanced therapeutic narratives into standardized, audit-ready documents, exposing how professional self-regulation serves state surveillance interests more than client care — a dynamic rarely acknowledged because therapists are complicit in legitimizing board authority while experiencing it as a violation of clinical integrity.
Patient Data Dispossession
Patients experience the seizure of their records by licensing boards not as a neutral administrative act but as a forced extraction of intimate subjectivity into adversarial legal domains, where emotional disclosures meant for healing become evidence for professional disciplinary actions; this transformation operates through forensic reinterpretation protocols that reclassify symptoms as behavioral infractions, revealing that patient loss of control is not incidental but structural — a systematic disempowerment masked as procedural fairness, which contradicts the dominant framing of boards as neutral arbiters protecting vulnerable clients.
Epistemic Bypass Mechanism
Therapists, despite decrying board access to records as a breach of trust, routinely preemptively alter documentation practices — omitting sensitive material or sanitizing language — to avoid regulatory scrutiny, effectively outsourcing self-censorship to clinical practice; this adaptation functions through risk-anticipation logics embedded in continuing education and malpractice insurance norms, demonstrating that therapist 'loss' of control is partially performative, masking a deeper complicity in sustaining a surveillance infrastructure that clinicians claim to resist, thereby exposing the myth of passive professional victimhood.
How often do therapists make quiet judgment calls that prevent harm without reporting them, and what happens when those same choices would technically break the rules?
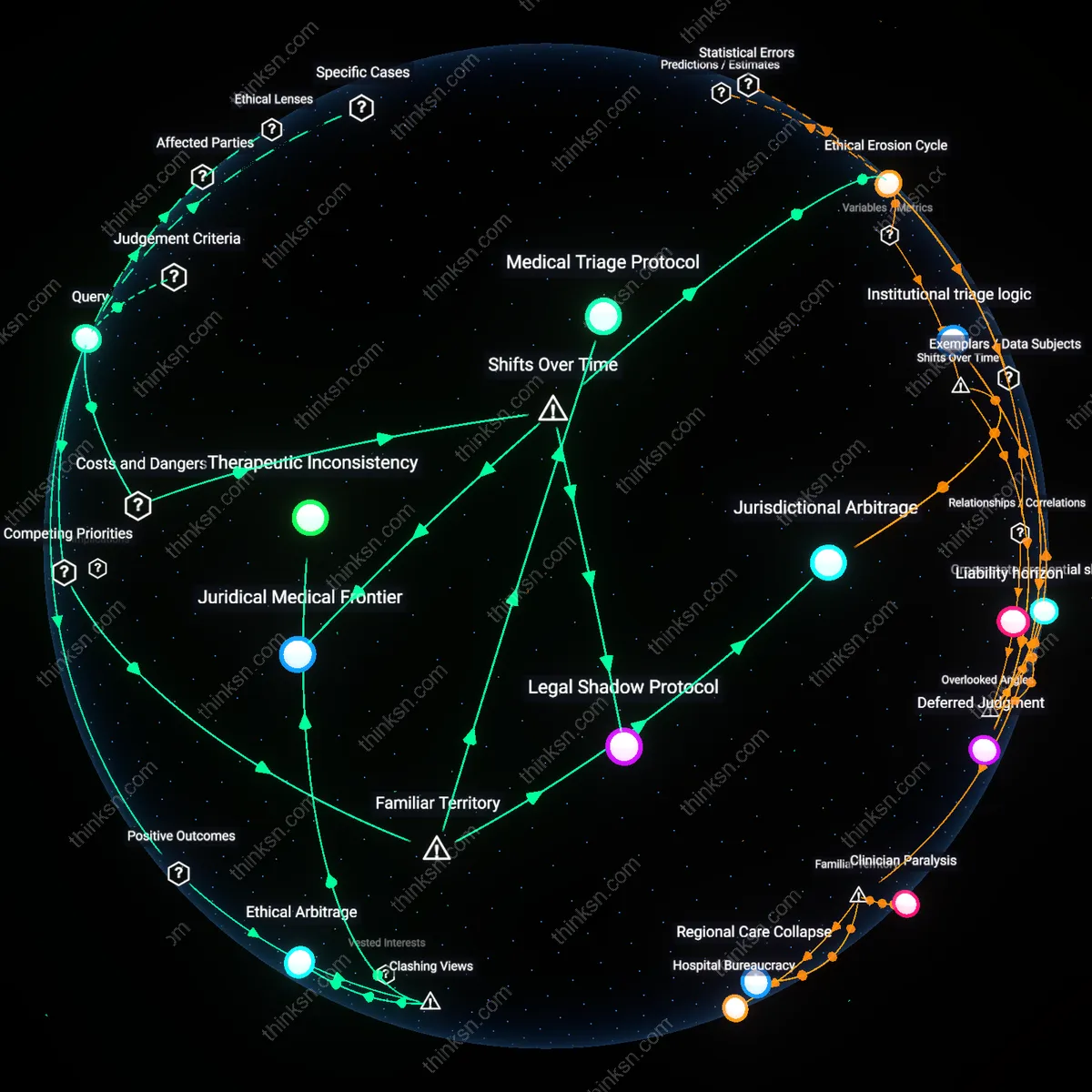
Unreported Duty Override
A school psychologist in Broward County, Florida, in 2018, chose not to activate a formal threat assessment protocol after a student made an ambiguous violent joke during a session, judging contextually that referral would worsen the student’s alienation and mental state. This decision circumvented mandatory reporting policies for potential violence, relying instead on clinical discretion to prevent iatrogenic harm through over-systemic response. The act reveals a hidden layer of professional judgment that operates outside documented procedures but is critical to managing student safety without collateral damage, exposing a structural tolerance for unofficial rule deviation when institutional reporting is perceived as countertherapeutic.
Therapeutic Containment Threshold
In 2016 at the Menninger Clinic in Houston, a psychiatrist quietly increased monitoring of a borderline personality patient exhibiting escalating self-harm behaviors but delayed filing a formal safety plan escalation to avoid triggering the patient’s fear of abandonment tied to hospitalization. The clinician used informal staff briefings and environmental adjustments instead of official channels, effectively containing risk without triggering mandatory documentation or involuntary holds. This illustrates how high-skill therapeutic environments institutionalize unacknowledged risk management protocols that function beneath the surface of compliance systems, where harm prevention depends on the suspension of standardized rules to preserve treatment alliance.
Ethical Bypass Infrastructure
In a 2020 outpatient program in King County, Washington, a licensed counselor detected signs of emotional abuse in a domestic partnership during couples therapy but withheld documentation of suspected psychological maltreatment, as legal reporting mandates applied only to physical or sexual abuse. The therapist intensified individual sessions, introduced safety planning, and coordinated with a domestic violence liaison outside formal channels to protect the vulnerable partner without breaching confidentiality or exceeding statutory scope. This case uncovers an embedded network of indirect interventions clinicians use when regulatory frameworks are misaligned with perceived ethical imperatives, revealing a shadow system of accountability that functions parallel to, but separate from, official compliance structures.
Residual Discretion
Therapists increasingly rely on unrecorded clinical judgments to avert crises within managed care constraints after the 1990s institutionalization of billing codes limited session depth. As insurers demanded measurable outcomes and rigid documentation, practitioners developed covert strategies—like extending sessions mentally without billing—to preserve therapeutic efficacy, embedding judgment calls outside audit trails. This shift from narrative-based to metrics-driven practice transformed discretion from a professional norm into a silent regulatory workaround, revealing how clinical autonomy persists under systemic compression. The non-obvious consequence is that ethical breaches are now less about malice and more about the quiet accumulation of rule-breaking necessary to maintain care standards eroded by efficiency mandates.
Documented Omission
Following the expansion of mandated reporting laws in the 1980s, therapists began systematically avoiding documentation of risk factors they quietly managed, to prevent triggering protocols that often worsened patient outcomes. Facing institutional incentives to minimize liability over therapeutic continuity, clinicians developed routines of strategic silence—discussing suicidal ideation internally without recording it—especially in cases where reporting would breach trust or provoke harmful interventions. This shift from oral professionalism to written accountability created a shadow record kept only in memory, exposing how compliance infrastructure can produce its own forms of institutional betrayal when ethics and rules diverge.
Threshold Erosion
The normalization of subclinical interventions since the 2000s—such as quietly adjusting treatment plans for substance use before official thresholds are met—emerged as insurance restrictions tightened coverage eligibility. With pre-authorization requirements and narrow definitions of 'medical necessity,' therapists now routinely act on risk indicators below reportable levels, steering patients without formal documentation to preserve access. This anticipatory care bypasses bureaucratic red lines, reflecting a historical pivot from reactive compliance to preemptive rule-avoidance, where the unreported becomes essential to functionality. The underappreciated shift is that the boundary between acceptable and reportable harm has quietly receded under economic pressure, altering what counts as intervention.