State Reporting on Out-of-State Abortions: Legal or a Breach of Privacy?
Analysis reveals 9 key thematic connections.
Key Findings
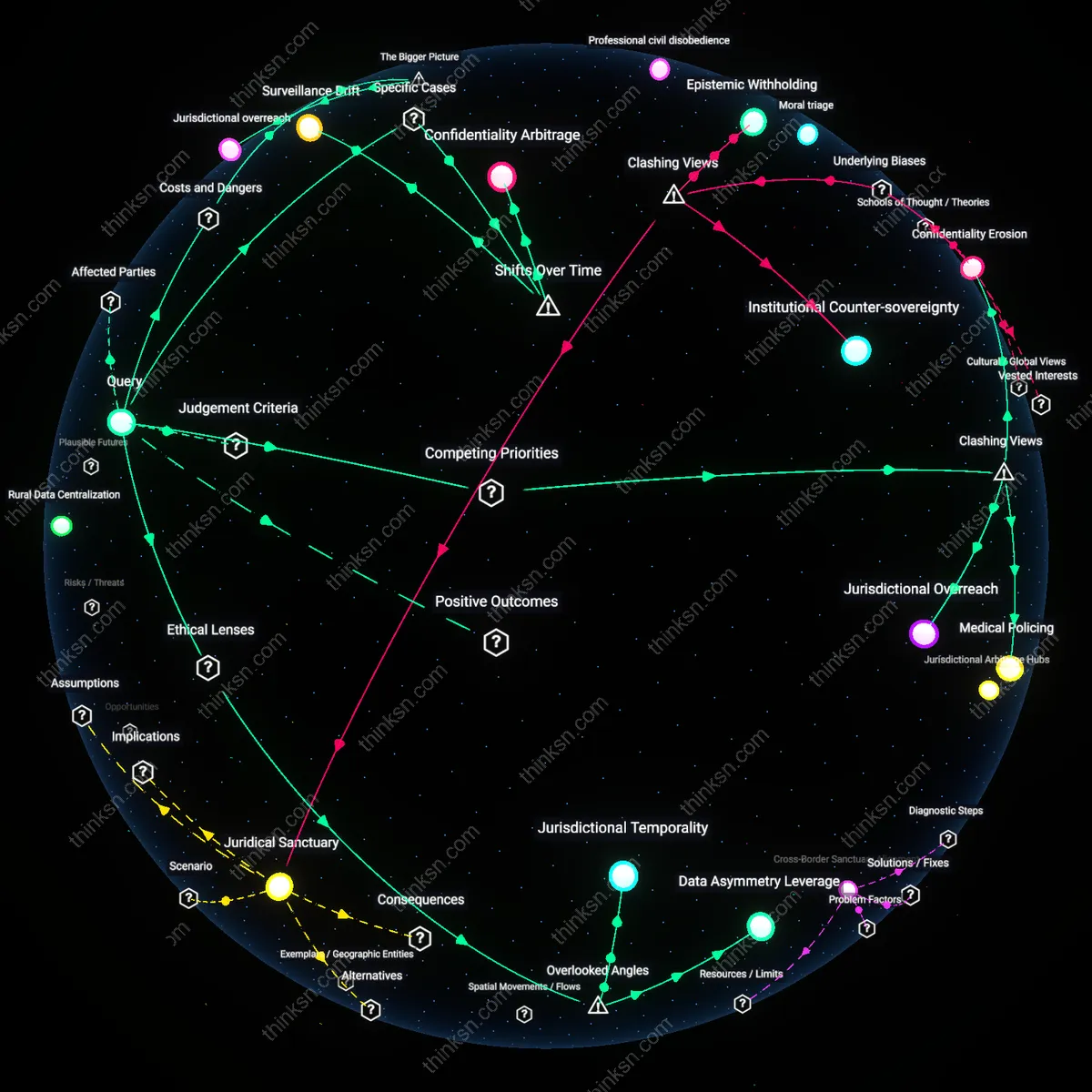
Jurisdictional overreach
A state cannot legally compel healthcare providers to report suspected out-of-state abortions because such mandates exceed the state’s territorial jurisdiction and conflict with dormant Commerce Clause principles and federal preemption in medical regulation, triggering unenforceability. Courts have consistently limited state authority to conduct occurring beyond borders, especially when it interferes with rights recognized in other jurisdictions, as seen in post-Dobbs interstate legal conflicts. This creates a destabilizing feedback loop where states attempt to project regulatory power across borders, eroding mutual recognition in federalism and provoking retaliatory legal measures. The non-obvious risk is not merely legal invalidation but the systemic erosion of interstate comity, as states begin treating neighboring jurisdictions as adversarial regimes rather than co-equal members of a shared legal order.
Regulatory arms race
When one state mandates reporting of out-of-state abortions, it provokes reciprocal legislation in other states criminalizing cooperation with such reporting, igniting a regulatory arms race that fragments national healthcare administration. This dynamic is already visible in states like California and Massachusetts passing laws shielding providers who assist out-of-state patients, directly countering bills in Texas or Missouri seeking extraterritorial enforcement. The mechanism is inter-state legislative retaliation operating through statutory counter-deterrence, where legal protections become territorial weapons. The systemic cost is the balkanization of medical record systems and care coordination, as electronic health networks must build jurisdiction-specific routing protocols, increasing overhead and error risk across the U.S. health IT infrastructure.
Jurisdictional Overreach
A state cannot legally compel healthcare providers to report suspected out-of-state abortions because such mandates violate the dormant Commerce Clause and the constitutional principle of extraterritoriality, which prohibit states from regulating conduct wholly occurring in other jurisdictions. This legal boundary exists because medical actions performed in another state fall beyond the regulatory authority of the referring state, regardless of the referring state's moral or legislative stance. The non-obvious implication is that even aggressive state anti-abortion regimes are structurally constrained by federalism’s invisible architecture, not just by privacy rights—an underappreciated check on state power that operates silently beneath the visibility of constitutional rights discourse.
Confidentiality Erosion
Mandating reporting of suspected out-of-state abortions inherently breaches patient confidentiality not as a side effect but as a designed function of the policy, because the state positions healthcare providers as de facto law enforcement informants, thereby redefining the clinician-patient relationship through surveillance rather than care. This shift undermines the ethical foundation of medical practice by inserting state investigative logic into clinical settings, making trust a systemic casualty rather than an incidental loss. The dissonance lies in recognizing that confidentiality is not merely weakened but actively dismantled as a condition of compliance, exposing how regulatory mandates can weaponize professional obligations against the individuals they are meant to serve.
Medical Policing
Requiring providers to report suspected out-of-state abortions transforms routine clinical judgment into a mechanism of cross-jurisdictional policing, where diagnostic discretion—such as interpreting bleeding as potential abortion—is coerced into serving penal objectives rather than health outcomes. This creates a shadow legal duty that overrides medical neutrality, turning obstetric and gynecological care into a site of investigatory risk, particularly in border regions like Texarkana or Cincinnati where proximity to abortion-accessible states increases surveillance pressure. The underrecognized reality is that medicine itself becomes a frontier of legal enforcement, revealing how reproductive regulation extends not by expanding criminal statutes but by repurposing existing medical infrastructure for compliance tracking.
Data Asymmetry Leverage
A state can legally compel reporting of suspected out-of-state abortions only insofar as federal health data protections are selectively underenforced in cross-jurisdictional reproductive care, a mechanism exemplified by states like Texas instrumentalizing HIPAA’s narrow exceptions to justify mandatory disclosure regimes. This turns on the fact that HIPAA permits disclosure to law enforcement under vague conditions of ‘suspected criminal activity,’ which states reframe to include conduct legal elsewhere—exploiting the federal government’s uneven auditing of such disclosures, particularly in politically aligned jurisdictions. What is overlooked is not the conflict between state and federal law per se, but how asymmetries in health data governance—where federal oversight is reactive rather than preventive—enable states to normalize surveillance under the guise of compliance, thereby shifting the burden of resistance onto individual providers and eroding de facto confidentiality even when de jure protections exist.
Jurisdictional Temporality
States cannot legally mandate reporting of abortions that occur outside their borders, but they can redefine the temporal boundaries of medical acts to claim jurisdiction—for instance, by treating prenatal consultations or travel arrangements as in-state components of an abortion process, thus creating a legal predicate for reporting requirements under laws like Missouri’s SB 8. This exploits a blind spot in medical ethics frameworks, which assume jurisdiction is spatially bound to the location of procedure, not temporally extended to preparatory care; by stretching jurisdictionality across time, states convert care coordination into reportable conduct. The significance lies in how medical temporality, typically neutral in ethical analysis, becomes a covert legal instrument that detaches provider obligations from the site of care and attaches them to the patient’s history, undermining the integrity of confidential pre-procedure consultations.
Surveillance Drift
State health departments in Texas post-2022 Dobbs decision have activated dormant reporting mandates, repurposing public health infrastructure originally designed for infectious disease tracking to capture out-of-state abortion referrals by requiring licensed providers to report 'unlawful' procedures suspected in patients—this marks a shift from clinical confidentiality as a medical norm to a legally enforceable state surveillance conduit, where healthcare becomes an extension of investigative capacity. The mechanism operates through statutory redefinition of professional duty, leveraging existing licensure oversight by medical boards to compel compliance, with penalties for non-reporting now mirroring those for statutory violations. This transformation is analytically distinct not because of new laws, but because it repurposes pre-existing bureaucratic systems originally insulated from criminal enforcement, revealing how medical governance can quietly pivot from care to control under changed legal conditions.
Confidentiality Arbitrage
Following the 2019 Missouri abortion restrictions, certain interstate provider networks began routing patient data through HIPAA-compliant channels in states like California to avoid disclosure mandates, exploiting jurisdictional gaps in enforcement—a shift from uniform national expectations of privacy to a fragmented, geography-dependent regime of data shielding. This work-around emerged only after states began testing extraterritorial enforcement of abortion bans, transforming HIPAA from a baseline privacy standard into a strategic shield, where providers selectively invoke federal preemption to resist state overreach. The significance lies not in outright defiance but in the normalization of legal stratagems that treat patient records as mobile assets to be jurisdictionally sheltered, exposing how temporal divergence between federal inaction and state activism creates new operational logics in clinical practice.