Why Is a WHO Essential Drug Unaffordable in the US?
Analysis reveals 9 key thematic connections.
Key Findings
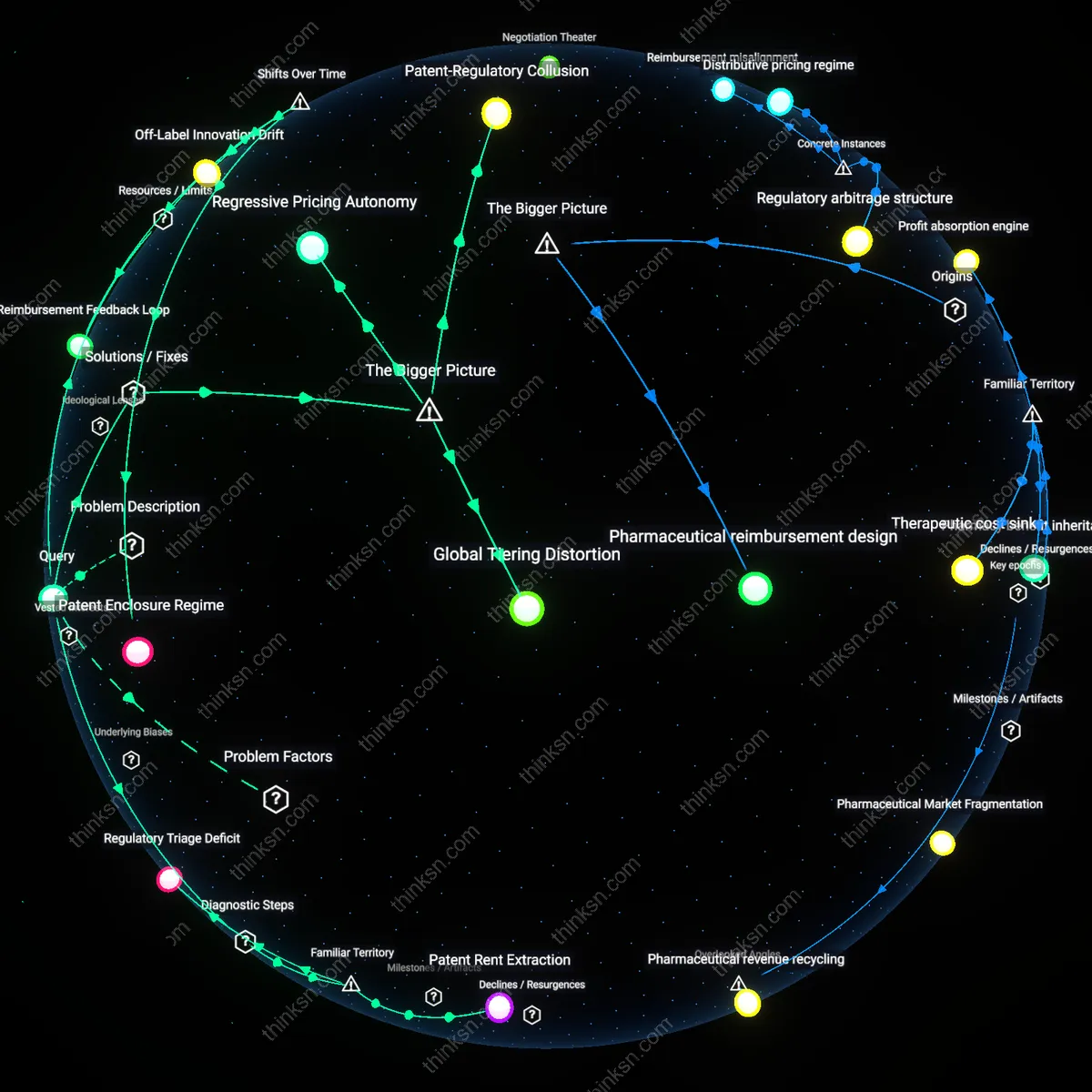
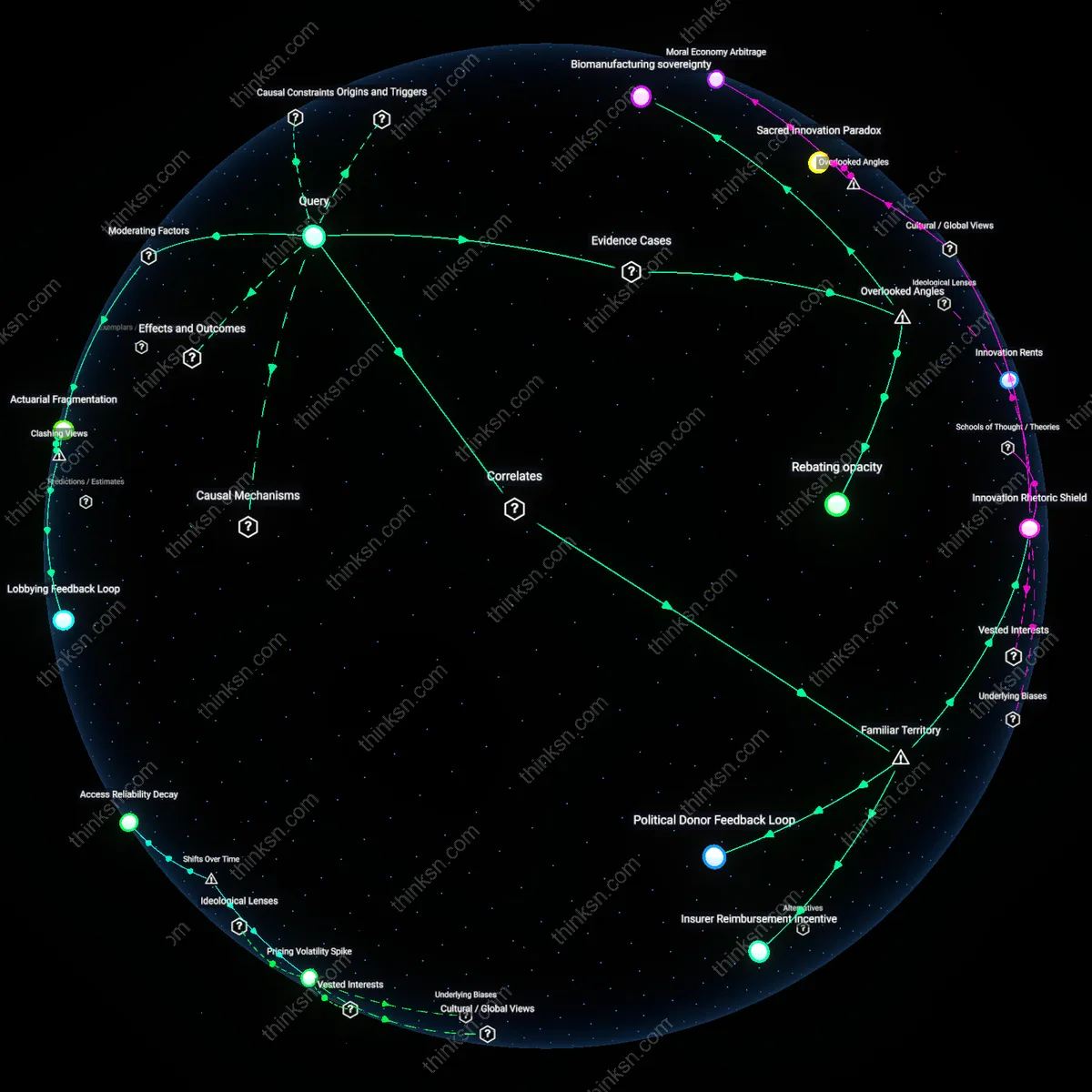
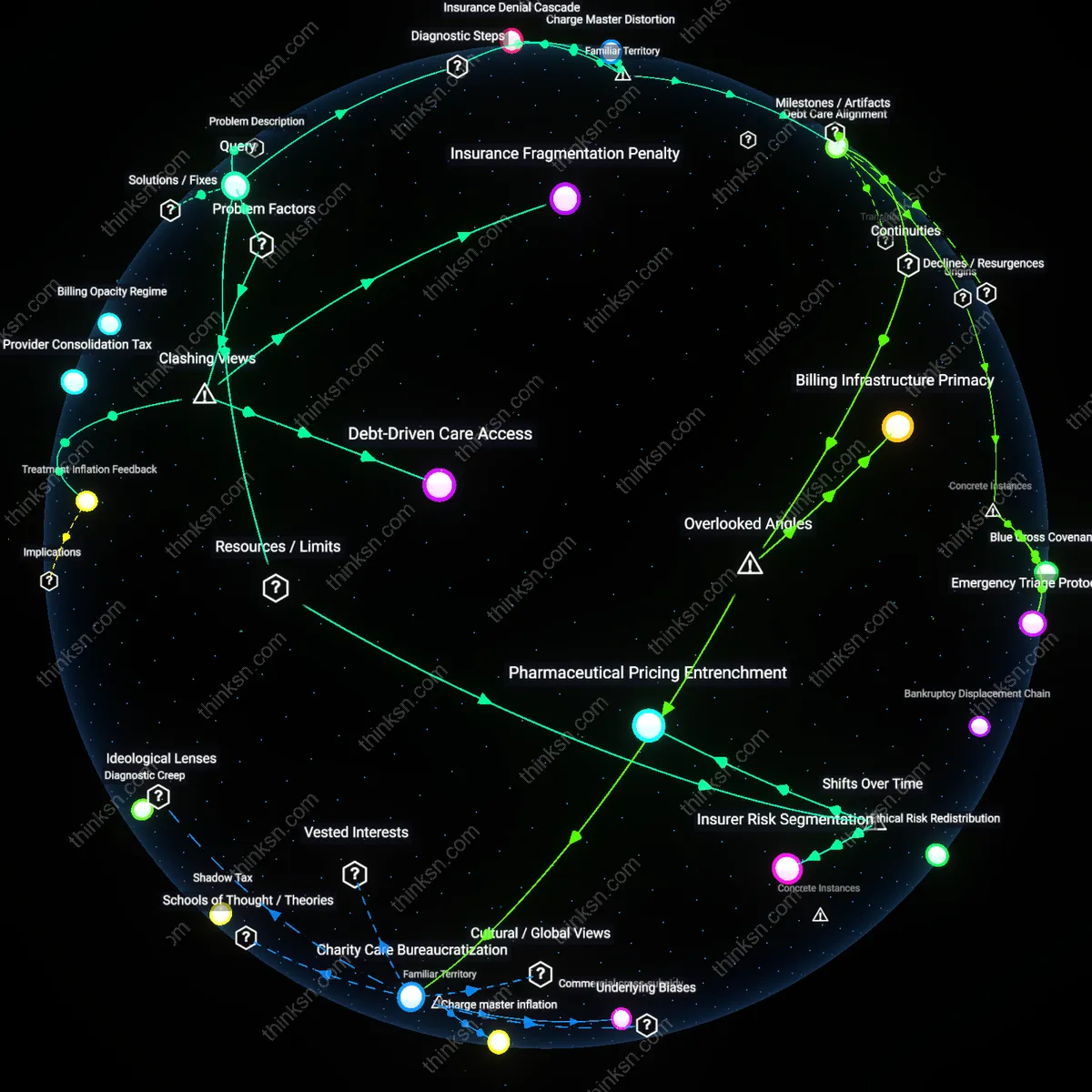
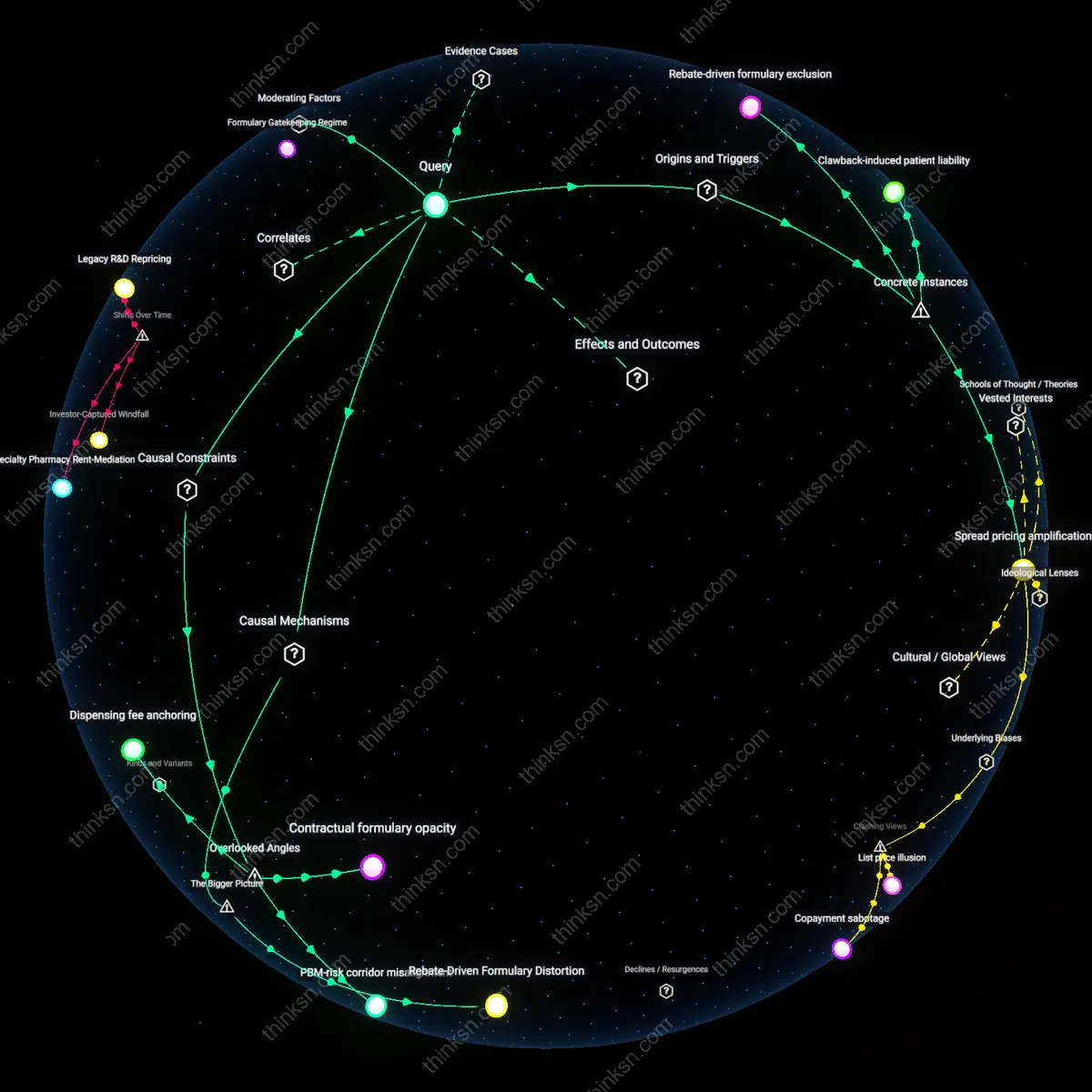
Patent Rent Extraction
Drug patents granted by the USPTO enable originator manufacturers to maintain monopolistic pricing on WHO-essential medications. This exclusivity prevents generic competition even when production costs are low, allowing firms like Pfizer or AbbVie to set prices far above marginal cost, particularly for insulin or antivirals. The non-obvious element within this familiar narrative of 'big pharma pricing' is that the mechanism is not merely corporate greed but a deliberate alignment of federal intellectual property law with private pricing autonomy, making affordability structurally deferred to patent expiry—assuming no evergreening.
Reimbursement Market Distortion
The dominance of private health insurers in the U.S. payment system creates a fragmented, opaque reimbursement environment where pharmacies and hospitals negotiate drug prices behind closed contracts. Unlike centralized procurement used in most countries, this system allows wholesalers like McKesson and PBMs like CVS Caremark to extract administrative rents while destabilizing bulk purchasing of WHO-essential drugs. The underappreciated point is that public outrage over 'high drug prices' often misses how the pricing burden is shifted and amplified through layers of third-party intermediaries who profit from complexity rather than therapeutic value.
Regulatory Triage Deficit
The FDA’s approval pathway prioritizes novelty and safety over cost-effectiveness or public health urgency, meaning life-saving generics for diseases like tuberculosis or rheumatic fever face the same development and inspection bottlenecks as new biologics. Because there is no parallel fast-track for WHO-essential off-patent drugs, manufacturers like Sandoz or Teva delay entry due to low expected returns amid high regulatory overhead. What people rarely recognize in the usual 'government failure' critique is that the agency’s design assumes market incentives will naturally align with health needs—a misfire when markets ignore unprofitable but essential medicines.
Regressive Pricing Autonomy
Decentralized procurement policies in the U.S. hospital systems allow individual institutions to negotiate drug prices independently, weakening collective bargaining power and enabling manufacturers to sustain high prices for WHO-essential drugs. This fragmentation is particularly harmful for low-volume but critical medications, where economies of scale could otherwise reduce costs; instead, the lack of centralized leverage entrenches price dispersion. The non-obvious insight is that localized cost-containment strategies—often seen as efficient—can systematically undermine affordability at the national level when they erode systemic price-setting counterweights.
Patent-Regulatory Collusion
The U.S. Food and Drug Administration’s (FDA) market exclusivity extensions for minor formulation changes in existing WHO-essential drugs enable manufacturers to legally block generic competition without meaningful innovation. This regulatory alignment with patent strategies transforms regulatory safeguards into profit-preserving tools, disproportionately affecting drugs where safety and familiarity justify continued use despite cost. The underappreciated dynamic is that the FDA, intended as a public health gatekeeper, becomes a structural enabler of pricing monopolies through procedural synergy with intellectual property regimes.
Global Tiering Distortion
U.S. pharmaceutical pricing policies indirectly destabilize international reference pricing models by establishing the highest benchmark price tier, which then disables cross-national cost equalization for WHO-essential drugs in lower-income countries. Because many governments base their reimbursement rates on U.S. market prices, the American inability to cap costs creates a floor effect that ratchets up global prices, even for off-patent medications. This reveals the paradox that domestic deregulation in a single high-income country generates a structural subsidy mechanism that reshapes pricing logic across interconnected health systems.
Patent Enclosure Regime
The consolidation of pharmaceutical patent ownership through mergers since the 1980s has systematically extended monopolies on WHO-essential drugs, preventing generic competition even after initial patent expiry. This shift—accelerated by the Bayh-Dole Act and reinforced by WTO-TRIPS compliance—transformed publicly funded research into privately controlled assets, enabling price inflation under legal exclusivity. The non-obvious outcome is that affordability is not undermined by isolated profiteering but by a structural enclosure of medical knowledge once treated as commons.
Reimbursement Feedback Loop
The Medicare Modernization Act of 2003 excluded direct federal negotiation of drug prices, entrenching a reimbursement model where private insurers and pharmacy benefit managers (PBMs) prioritize formulary placement over cost containment. As post-2000 market dynamics shifted pricing power to intermediaries who profit from list price spreads, manufacturers raised prices to maximize rebates—making even off-patent WHO-essential drugs unaffordable. The historical pivot reveals that unaffordability is not a supply failure but a perverse reward structure embedded in third-party payment systems.
Off-Label Innovation Drift
Since the 1990s, FDA regulatory incentives for novel indications have redirected pharmaceutical R&D away from generic production of essential medicines toward high-margin specialty drugs, even when molecularly similar. This therapeutic repositioning—where companies legally repurpose WHO-essential drug derivatives for niche conditions—exploits regulatory pathways like orphan drug status to reset exclusivity clocks. The underappreciated consequence is that essential drugs become unaffordable not due to scarcity, but because the innovation system actively devalues therapeutic equivalence in favor of market differentiation.