Do Rebates Lower Patient Costs or PBM Profits?
Analysis reveals 10 key thematic connections.
Key Findings
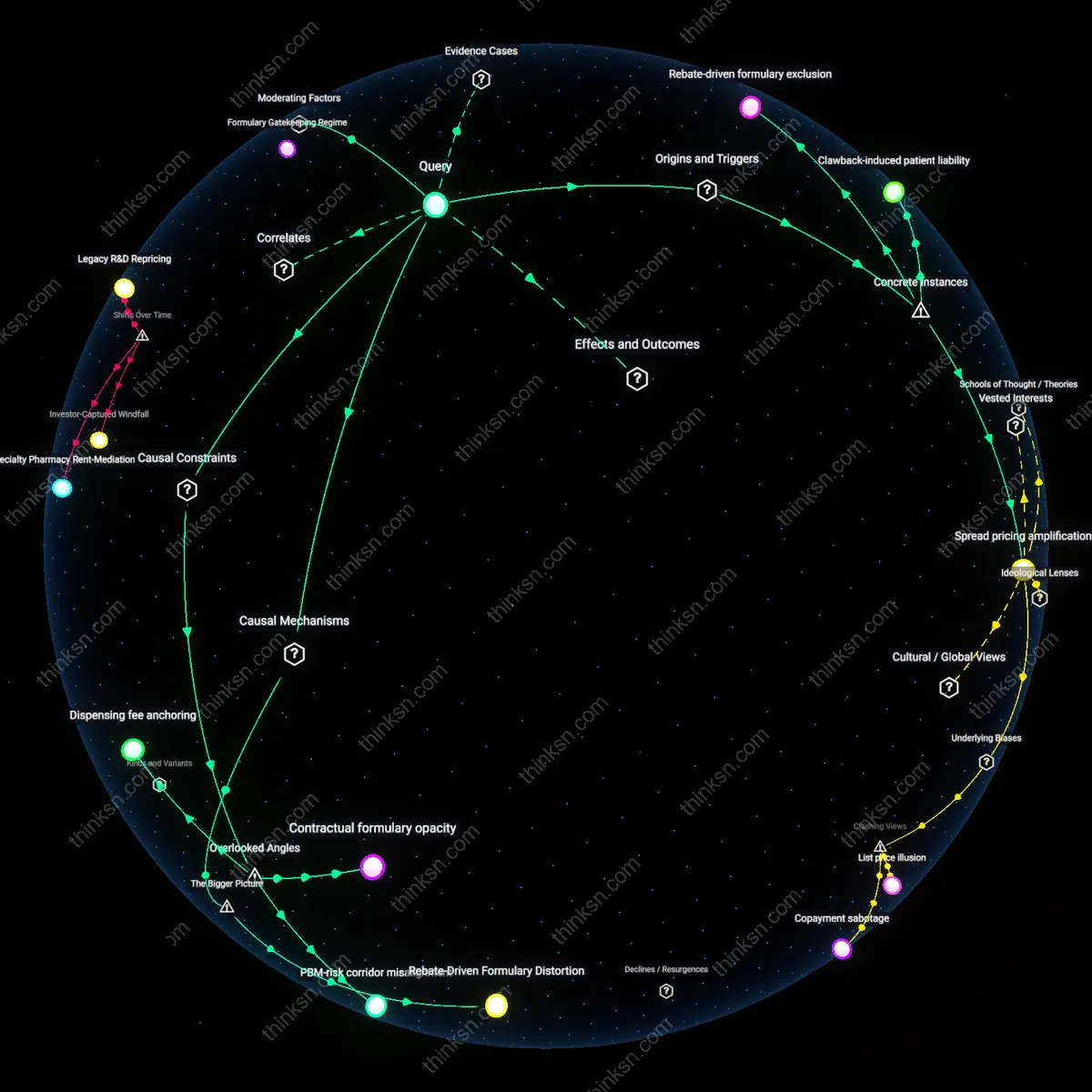
Rebate-driven formulary exclusion
Drug manufacturer rebates to insurers reduce out-of-pocket costs for low-income patients only when the drug is on formulary, but often lead to higher patient costs when rebated brand-name drugs displace lower-cost generics, as seen in the case of insulin formulary manipulation by Express Scripts in 2017, where preferred insulins with high rebates were promoted despite minimal clinical superiority, increasing patient cost sharing when alternatives were excluded; this reveals how rebate structures prioritize PBMs’ profit capture over affordable access, a dynamic rarely visible to patients or prescribers.
Spread pricing amplification
Pharmacy benefit managers increase their profit margins through spread pricing—charging insurers more than pharmacies are paid—while rebates from manufacturers allow PBMs to justify higher baseline prices, exemplified by Arkansas’ 2015 litigation against MedImpact and others, which exposed how PBMs retained both rebates and spread profits without passing savings to Medicaid patients; this demonstrates that rebate flows legitimize opaque pricing architectures that systematically inflate PBM margins at the expense of public payers and low-income enrollees.
Clawback-induced patient liability
Insurers and PBMs use rebates to lower premium costs but maintain high list prices, leading to elevated out-of-pocket spending for low-income patients on high-deductible plans, as occurred under Cigna’s pharmacy strategy in 2019, where rebated specialty drugs like Eliquis remained priced at list while patients paid deductibles based on undiscounted amounts; this mechanism—where rebates are clawed back by PBMs and insurers rather than reducing cost sharing—reveals how financial benefits bypass patients entirely, embedding cost burden within pricing opacity.
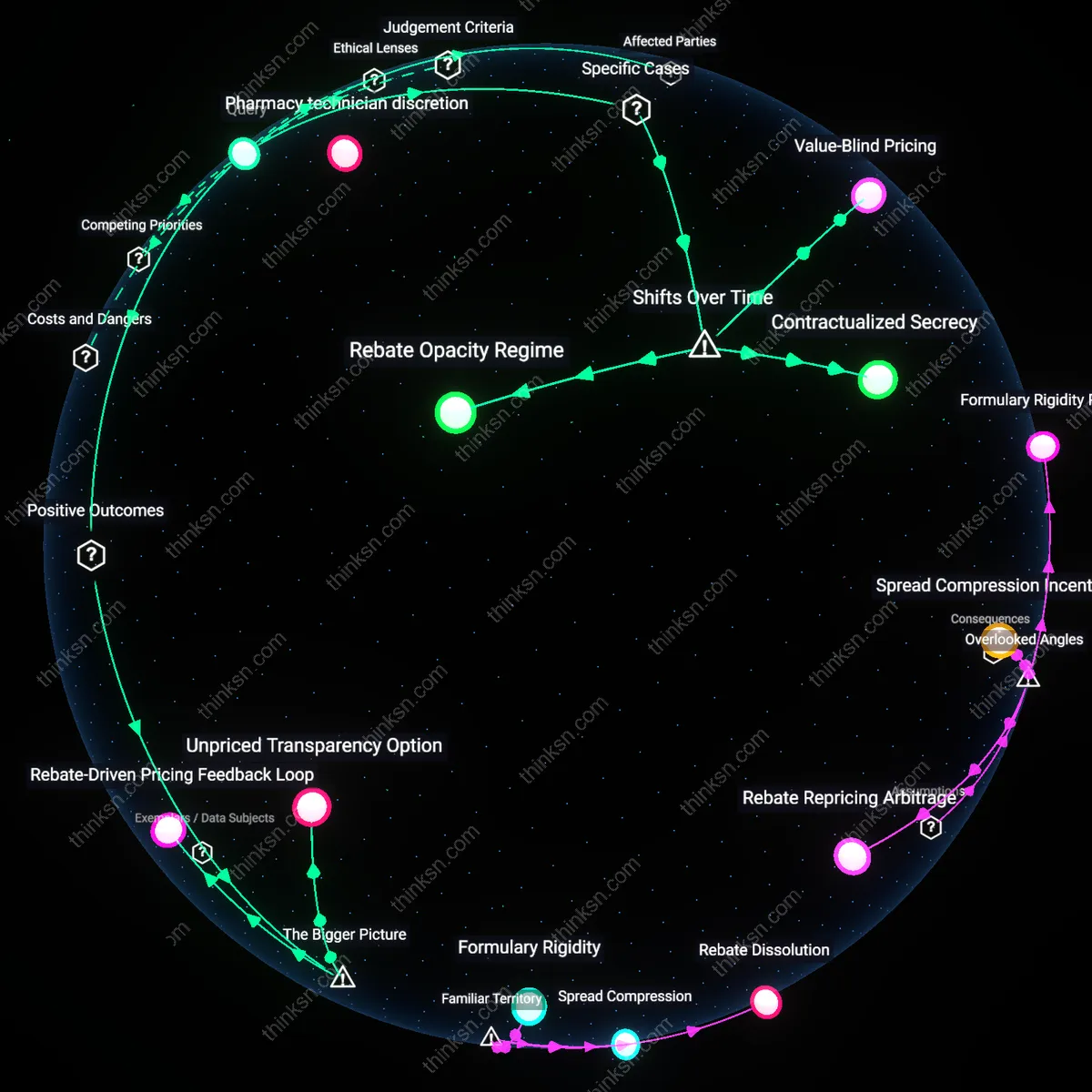
Rebate-Driven Formulary Distortion
Drug manufacturer rebates cause insurers to place higher-cost branded drugs on preferred formulary tiers, which suppresses generic utilization and increases low-income patients’ out-of-pocket costs despite lower PBMs’ direct profit margins. Because pharmacy benefit managers (PBMs) are paid rebate-sharing fees based on list price, insurers prioritize drugs with the largest rebates—often originator brands—over clinically equivalent, lower-cost generics, shifting financial risk onto cost-sensitive patients. This mechanism thrives inside the structural opacity of PBM contracting, where rebate amounts are undisclosed and tier placement is decoupled from net price; the non-obvious consequence is that rebates, intended to lower system costs, actually inflate patient spending by distorting competitive market signals through insurer formulary design.
Subsidized List Price Inflation
Manufacturer rebates enable sustained increases in drug list prices, which disproportionately burden low-income patients on high-deductible plans or with capped benefits, while simultaneously boosting PBM profits tied to percentage-based fee structures on gross invoice values. Since PBMs earn administrative fees and rebate compensation calculated as a percentage of list price, both manufacturers and PBMs gain financially from price escalation—even when net prices post-rebate decline—creating a misaligned incentive system where higher sticker prices generate more revenue upstream regardless of downstream patient harm. This perverse dynamic is entrenched in the U.S. pharmaceutical distribution chain, where fee-for-service PBM models commodify list price volatility rather than therapeutic value, revealing how pricing rituals favor intermediaries over equity in access.
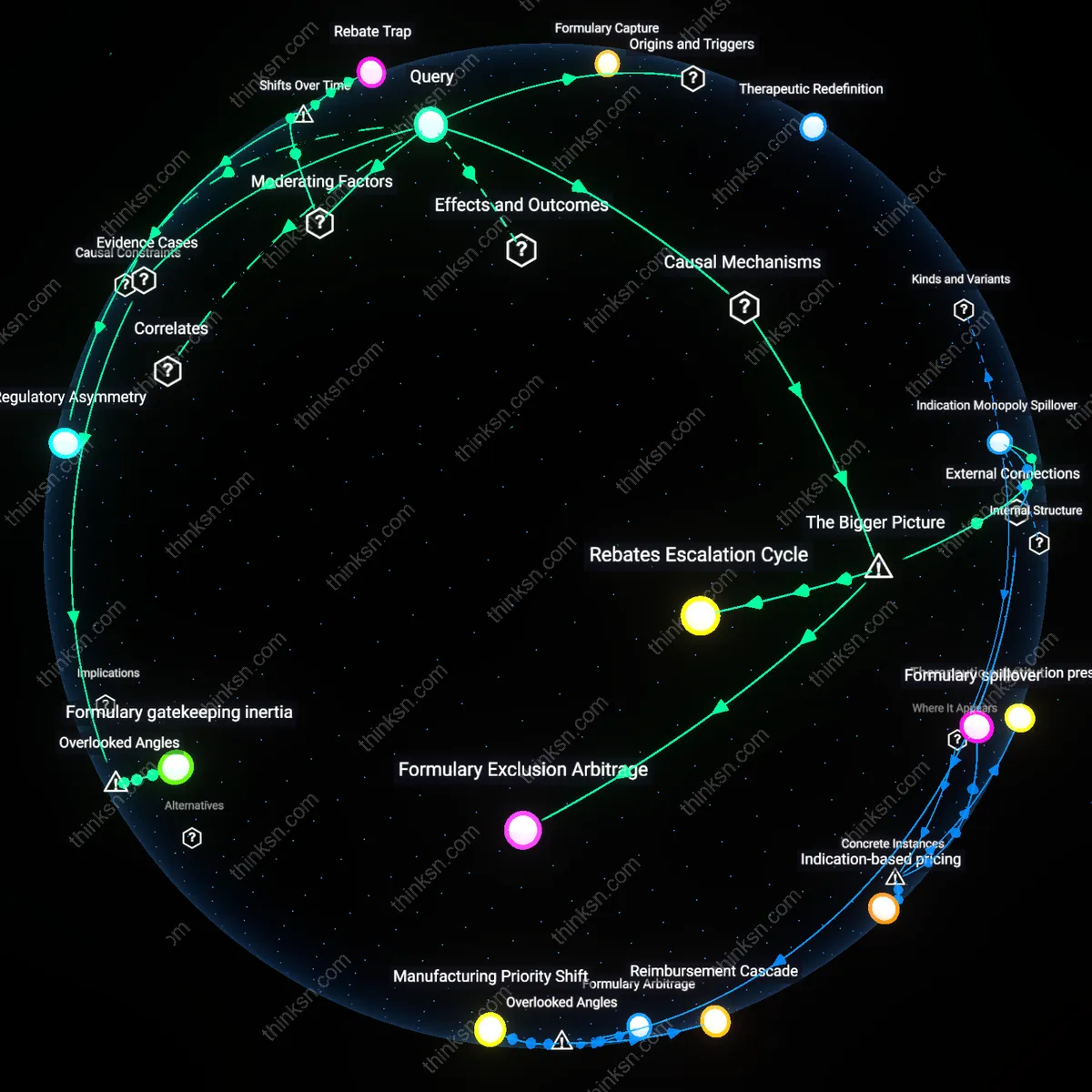
Rebate Escalation Trap
Drug manufacturer rebates to insurers increase out-of-pocket costs for low-income patients and widen pharmacy benefit manager (PBM) profit margins by inflating list prices, a dynamic that intensified after the 2003 Medicare Modernization Act allowed PBMs to retain spread pricing and rebate clawbacks. As rebates became a dominant form of negotiated pricing in the mid-2000s, manufacturers raised list prices to preserve net revenue, causing cost-sharing calculations—tied to list price—to rise for patients even as PBMs and insurers captured more rebate value. This mechanism, embedded in formulary placement incentives and opaque PBM contracts, systematically shifted financial risk onto patients least able to bear it, revealing how post-2003 market design amplified regressive cost burdens under the guise of managed care efficiency.
Formulary Gatekeeping Regime
Rebates reduce out-of-pocket costs only for low-income patients whose insurers place preferred drugs on favorable formulary tiers, a shift that crystallized between 2010 and 2015 as high-deductible health plans proliferated and Medicaid adopted managed care models emphasizing rebate-maximizing drug selection. As formulary segmentation hardened during this period, patient access became contingent on PBM-administered tier assignment, which prioritizes drugs with higher rebates over lower list prices, effectively making cost-sharing a function of rebate leverage rather than therapeutic value. This transition entrenched PBMs as gatekeepers of affordability, where profit margins grew not from service fees but from strategic control over which rebates patients could practically access—unveiling a tiered affordability system masked as cost containment.
Contractual formulary opacity
Drug manufacturer rebates increase out-of-pocket costs for low-income patients and widen pharmacy benefit manager (PBM) profit margins because rebate contracts are structured to prioritize gross drug price inflation over net cost reductions, which remain invisible at the point of sale. PBMs negotiate rebates behind closed formulary contracts with manufacturers, but these savings are rarely passed through to patients, especially in Medicaid or Medicare Part D plans where cost-sharing is based on list price rather than net price after rebates. The bottleneck preventing rebates from lowering patient costs is the lack of mandatory pass-through clauses in state or federal regulations, enabling PBMs to retain a portion of rebates as performance-based fees. This dynamic is rarely accounted for in policy debates, which focus on list prices while ignoring how contractual design insulates patients from rebate-driven savings, making the rebate system a hidden driver of cost burden for vulnerable populations.
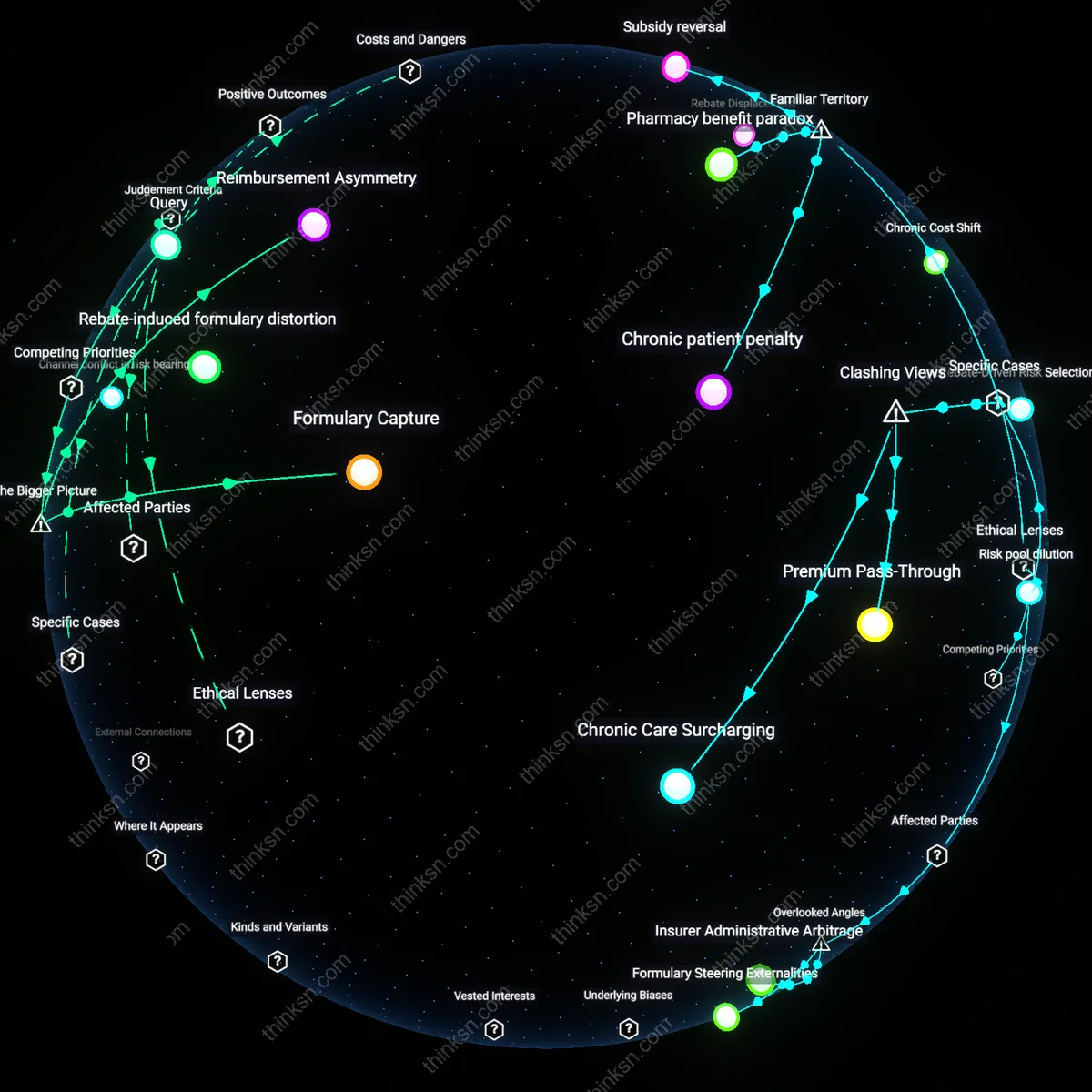
PBM-risk corridor misalignment
Rebates inflate PBM profit margins while worsening cost exposure for low-income patients because PBMs operate under risk-sharing agreements with insurers that financially reward them for rebate volume rather than patient cost reduction. In commercial and Medicare plans, PBMs are often compensated through a spread between the negotiated net price (list price minus rebate) and the reimbursement they pass to pharmacies, creating a direct incentive to favor high-list-price, high-rebate drugs even when cheaper generics exist. The causal prerequisite—PBM compensation tied to rebate capture rather than outcomes—is rarely altered by payer contracts, locking in perverse incentives. Most analyses miss that the risk corridors intended to stabilize insurer finances inadvertently subsidize PBM behavior by absorbing upward cost shocks from inflated list prices, decoupling financial accountability from patient affordability.
Dispensing fee anchoring
Drug manufacturer rebates indirectly increase out-of-pocket costs for low-income patients by distorting pharmacy reimbursement structures, particularly through the anchoring of flat dispensing fees in PBM-pharmacy contracts. Because rebated drugs maintain high list prices, pharmacy reimbursement from PBMs is often compressed to offset PBM rebate payments to plans, leading independent and rural pharmacies to rely more heavily on fixed dispensing fees to break even. This creates downward pressure on access for low-income patients, as pharmacies in underserved areas may stop carrying high-rebate specialty drugs due to narrow margins, forcing patients to travel or pay cash. The overlooked mechanism is that dispensing fees—often invisible in rebate discourse—become structurally essential income when net pharmacy reimbursements fall, revealing a hidden dependency of patient access on ancillary revenue streams that rebates quietly undermine.