Why Does U.S. Lack National Drug Price Negotiation?
Analysis reveals 9 key thematic connections.
Key Findings
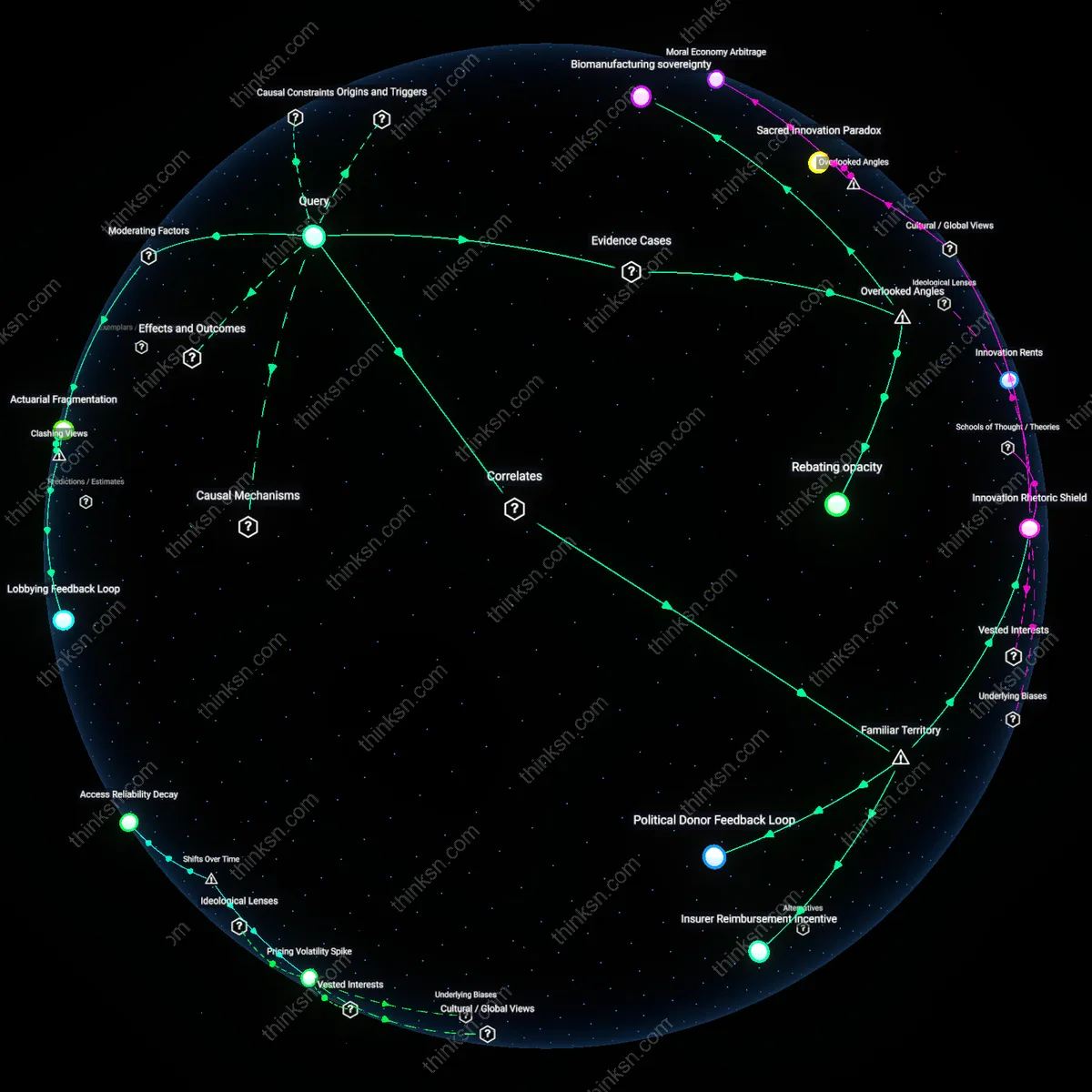
Lobbying Feedback Loop
Pharmaceutical companies sustain the absence of national drug price negotiation by converting political risk into legislative protection through targeted campaign financing in swing districts, which hardens resistance in Congress even when public opinion favors reform. This mechanism operates through the alignment of PAC donations with committee assignments—particularly in the House Energy and Commerce Committee—where members receiving the highest industry contributions are least likely to co-sponsor negotiation bills, irrespective of party. The non-obvious insight is that it is not broad anti-regulation ideology but geographically concentrated financial incentives that pivot legislative behavior, revealing how localized political economy conditions override national health policy imperatives.
Actuarial Fragmentation
Insurers benefit from the lack of national price negotiation because fragmented formulary design allows them to extract rebates and steerage profits from differential access tiers, which would collapse under uniform pricing. This operates through private Medicare Part D plan bidding dynamics, where risk corridors and reinsurance thresholds create profit incentives to maintain variable drug costs across regions. Contrary to the assumption that insurers seek cost control, their actuarial models are calibrated to volatility in drug prices, making them covert opponents of standardization—a dissonance that exposes how payment complexity, not care delivery, anchors insurer market power.
Federalism Arbitrage
State-level innovation in drug pricing programs—such as Montana’s insulin affordability cap or California’s state-run procurement pilot—actively undermines federal negotiation efforts by creating a false dichotomy between 'local solutions' and 'national overreach,' which pharmaceutical firms exploit to deflect systemic reform. This dynamic is institutionalized through industry-funded think tanks that amplify state exceptions as evidence that federal intervention is unnecessary, thereby shifting the policy burden to jurisdictions with limited fiscal capacity. The overlooked reality is that decentralized experimentation isn’t impeding federal action—pharma is weaponizing it, revealing how subnational heterogeneity functions as a strategic disruption tool rather than a policy laboratory.
Political Donor Feedback Loop
Pharmaceutical companies fund congressional campaigns to block national drug price negotiation. This financial entanglement operates through PAC contributions and lobbying expenditures concentrated in Washington, D.C., particularly targeting key committee members in the House Energy and Commerce Committee and Senate Finance Committee. While the public often cites 'lobbying' generally, the non-obvious mechanism is the self-reinforcing cycle where elected officials depend on drug industry donations to win elections, making systemic reform structurally inhibited regardless of public support.
Insurer Reimbursement Incentive
Private insurers benefit from the current lack of federal price controls because they maintain flexibility to negotiate rebates and formularies that generate revenue under spread pricing models. This system allows pharmacy benefit managers (PBMs) to profit from the difference between negotiated drug prices and reimbursement rates paid by insurers. The underappreciated reality is that insurers and PBMs are complicit enforcers of price opacity, as their profitability depends on a fragmented, non-transparent pricing regime that a centralized negotiation system would collapse.
Innovation Rhetoric Shield
Government agencies and policymakers invoke the narrative that free pricing protects biomedical innovation to justify non-intervention in drug markets. This claim operates through public discourse and testimony before Congress, where pharmaceutical CEOs and trade associations equate price regulation with reduced R&D investment. The non-obvious truth is that this rhetorical frame—deeply embedded in media and political rhetoric—functions not as a predictive model but as a prophylactic justification, pre-empting reform by associating it with risk to future cures regardless of empirical evidence on R&D spending patterns.
Legislative arbitrage
The federal government avoids direct drug price negotiation to preserve the fiscal autonomy of Congressional committees controlling Medicaid and Medicare funding, as seen in the exclusion of Medicare Part D from the 2007 Medicare Modernization Act’s negotiation provisions. This mechanism, structured through jurisdictional separation between the House Ways and Means Committee and the Energy and Commerce Committee, creates a check on consolidated executive control over pricing that pharmaceutical lobbies exploit by fragmenting opposition. The non-obvious dimension is that inter-committee institutional rivalry—not just industry lobbying—enables pricing opacity, reframing stalemate as a feature of federal legislative design rather than a failure. This residual logic of jurisdictional deadlock is rarely acknowledged in public discourse focused on corporate greed.
Rebating opacity
Private insurers maintain complex rebate systems with pharmaceutical companies that obscure actual drug prices, exemplified by UnitedHealth Group’s OptumRx division structuring formularies to prioritize high-rebate drugs over lower-cost generics. This dynamic depends on the invisibility of post-rebate net prices to employers and patients, allowing both insurers and manufacturers to profit while deflecting political accountability for high list prices. What is underappreciated is that insurers are not passive conduits but active architects of pricing confusion, using rebates to extract value without reducing patient costs—a feedback loop that undermines public support for federal negotiation.
Biomanufacturing sovereignty
The absence of national drug price controls is sustained by defense and economic security rationales tied to maintaining domestic pharmaceutical production capacity, visible in the Department of Defense’s reliance on U.S.-based manufacturers like Meridian Medical Technologies for epinephrine auto-injectors. Because certain drug classes are treated as strategic reserves akin to munitions, aggressive price negotiation is avoided to protect fragile, high-cost domestic supply chains from offshoring. This national security framing, rarely discussed in health policy debates, positions drug pricing not just as a market or moral issue but as a contingency of industrial policy essential to military readiness—reshaping the political calculus around intervention.