Long-Term Care Costs Rising: Insure or Invest?
Analysis reveals 5 key thematic connections.
Key Findings
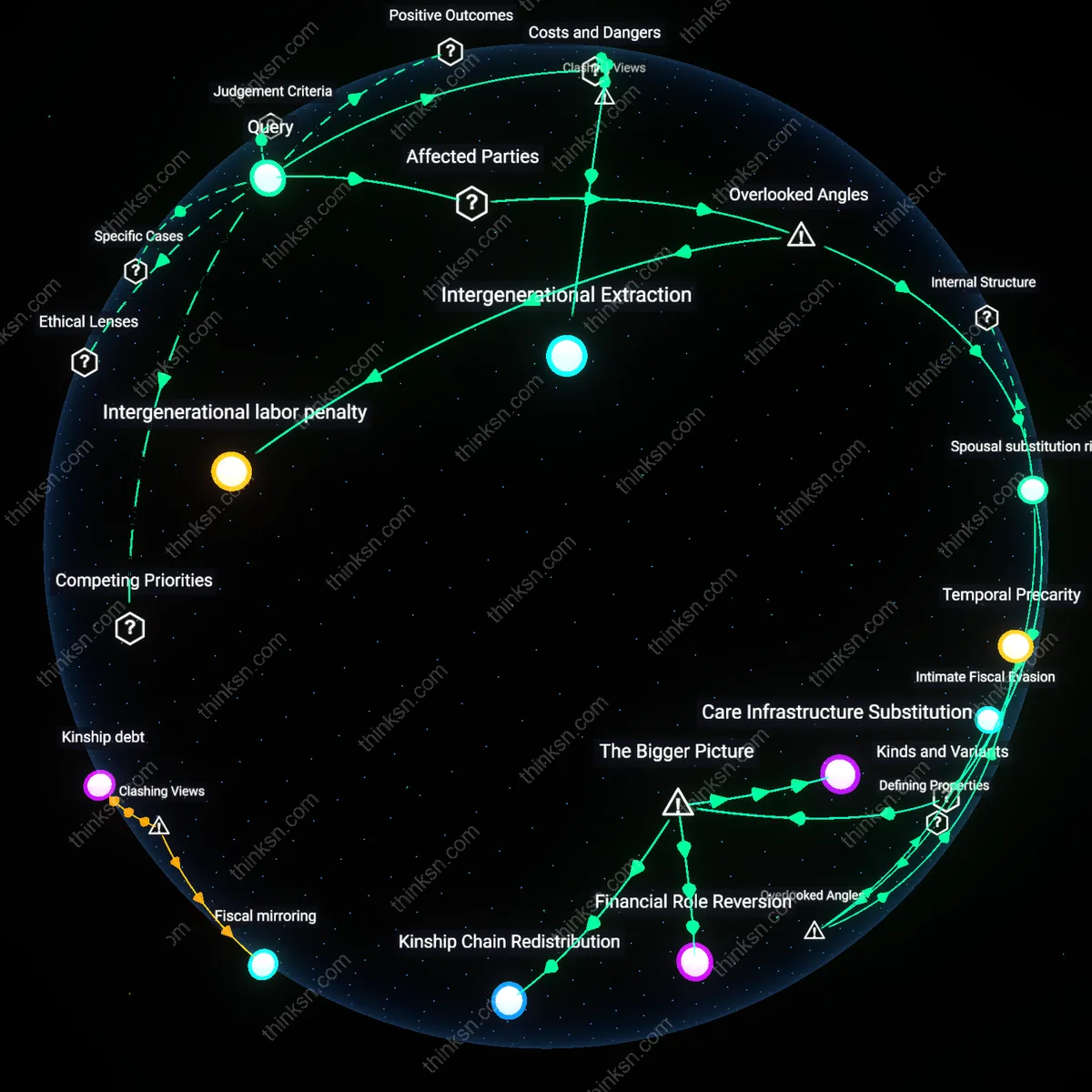
Spousal substitution risk
A 45-year-old should prioritize long-term care insurance over increasing retirement investments because the primary risk is not personal incapacity but the sudden dependency of a spouse, which disproportionately strains mid-life earning capacity. Most analyses focus on the individual’s future care needs, but the overlooked mechanism is the statistically common scenario where one partner incurs long-term care needs in their 60s or 70s, forcing the still-working 45-year-old to reduce hours, exit employment, or redirect active income—eroding both current cash flow and future retirement accruals. This spillover effect on the partner’s labor force participation, especially in dual-income households with limited extended family support, creates a larger financial disruption than personal care costs alone, yet it remains absent from standard insurance prioritization models, which assume care events are isolated and later in life.
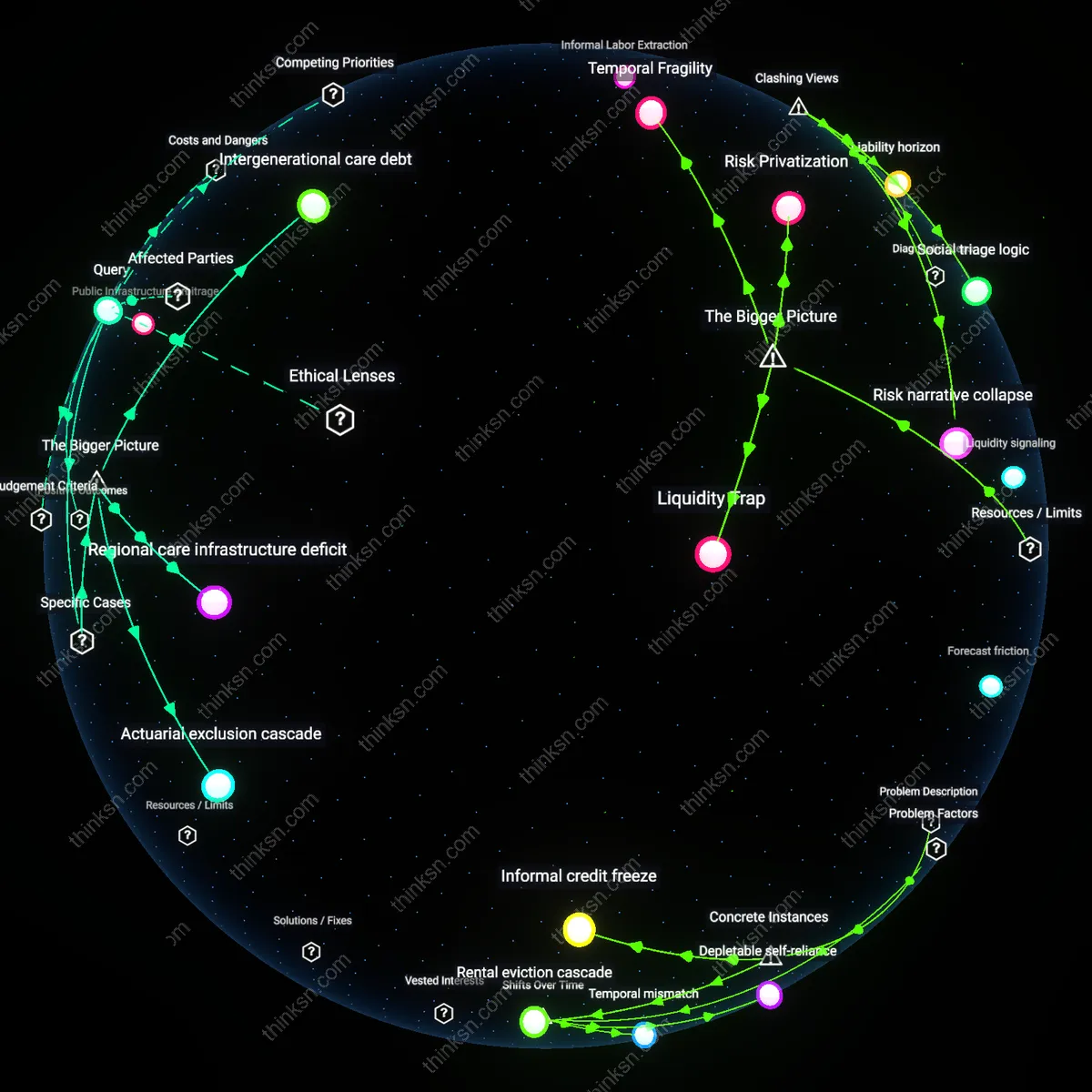
Municipal fiscal drag
A 45-year-old should prioritize long-term care insurance because future public care infrastructure—particularly at the county and municipal level—is likely to deteriorate due to unfunded liabilities and demographic strain, shifting costs to individuals regardless of personal planning. While most discussions assume a stable backdrop of public safety nets or Medicaid availability, the overlooked reality is that local governments in states like Illinois and New Jersey are already deferring maintenance on public elder-care facilities and reducing home health aide programs due to pension obligations and declining tax bases. This municipal fiscal drag means that even middle-class individuals may find state-assisted care unavailable or substandard by the time they need it, making private insurance a hedge not just against health risk but against institutional decay.
Intergenerational labor penalty
A 45-year-old should prioritize long-term care insurance because the hidden cost of underinsurance falls not on the individual but on their adult children, who absorb caregiving labor and associated income loss—a transfer that destabilizes the next generation’s financial trajectory. Standard analyses ignore that by age 75, 68% of care hours come from adult children, particularly daughters, who reduce work hours or exit careers, creating a measurable intergenerational labor penalty that undermines retirement security across two age cohorts. This dynamic reframes long-term care not as a personal financial tradeoff but as a familial resource extraction, where lack of insurance today converts into lost wages, eroded 401(k)s, and delayed home ownership for the 30-something children—making the 45-year-old’s insurance decision a form of intergenerational harm reduction.
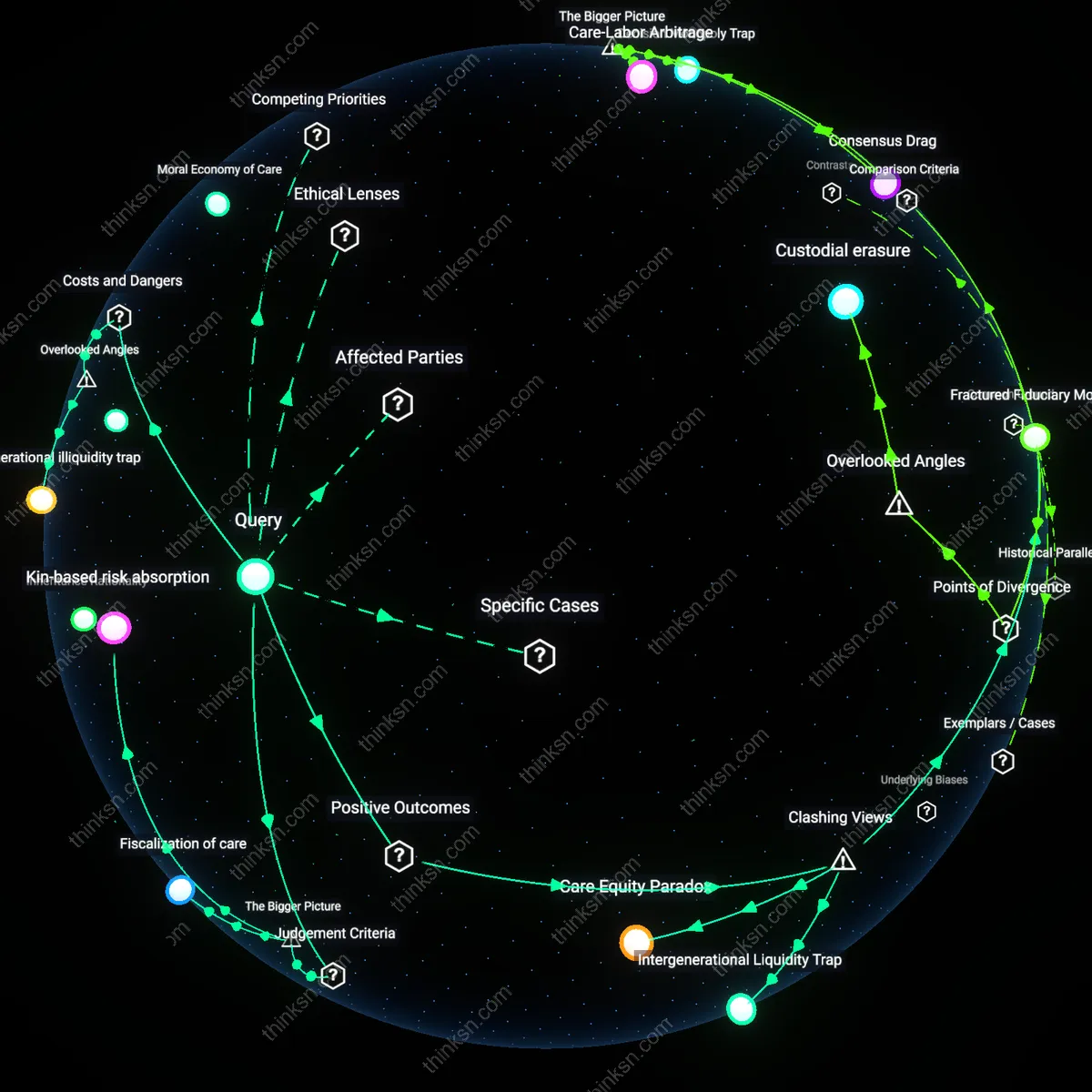
Actuarial Illusion
No, a 45-year-old should not prioritize long-term care insurance over retirement investments because the pricing of long-term care policies is structurally skewed by persistent adverse selection and insurer withdrawal from the market, making future coverage unreliable regardless of current premiums. Insurers like Genworth have raised rates dramatically after underestimating longevity and utilization risks, while younger cohorts face shrinking product availability as companies exit unprofitable lines—this creates a false sense of security where paying today may not guarantee protection tomorrow. The non-obvious reality is that the private long-term care insurance market functions less as a reliable risk pool and more as a speculative bet on insurer solvency and regulatory tolerance, undermining its core utility.
Intergenerational Extraction
No, because prioritizing long-term care insurance often functions as a covert transfer of wealth from middle-aged earners to already-privileged elderly populations who disproportionately receive the benefits of care labor, usually provided by underpaid women of color in home health and institutional settings. The economic model depends on cheap caregiving labor to justify actuarial projections, yet rising wages or regulation could destabilize the entire cost structure, exposing a dependency on systemic undervaluation of care work. This reveals that the financial logic of long-term care insurance relies not on sound risk management but on sustained social inequity, making its stability an ethical mirage.