When Career Stress Threatens Health: Justifying a Costly Pivot?
Analysis reveals 5 key thematic connections.
Key Findings
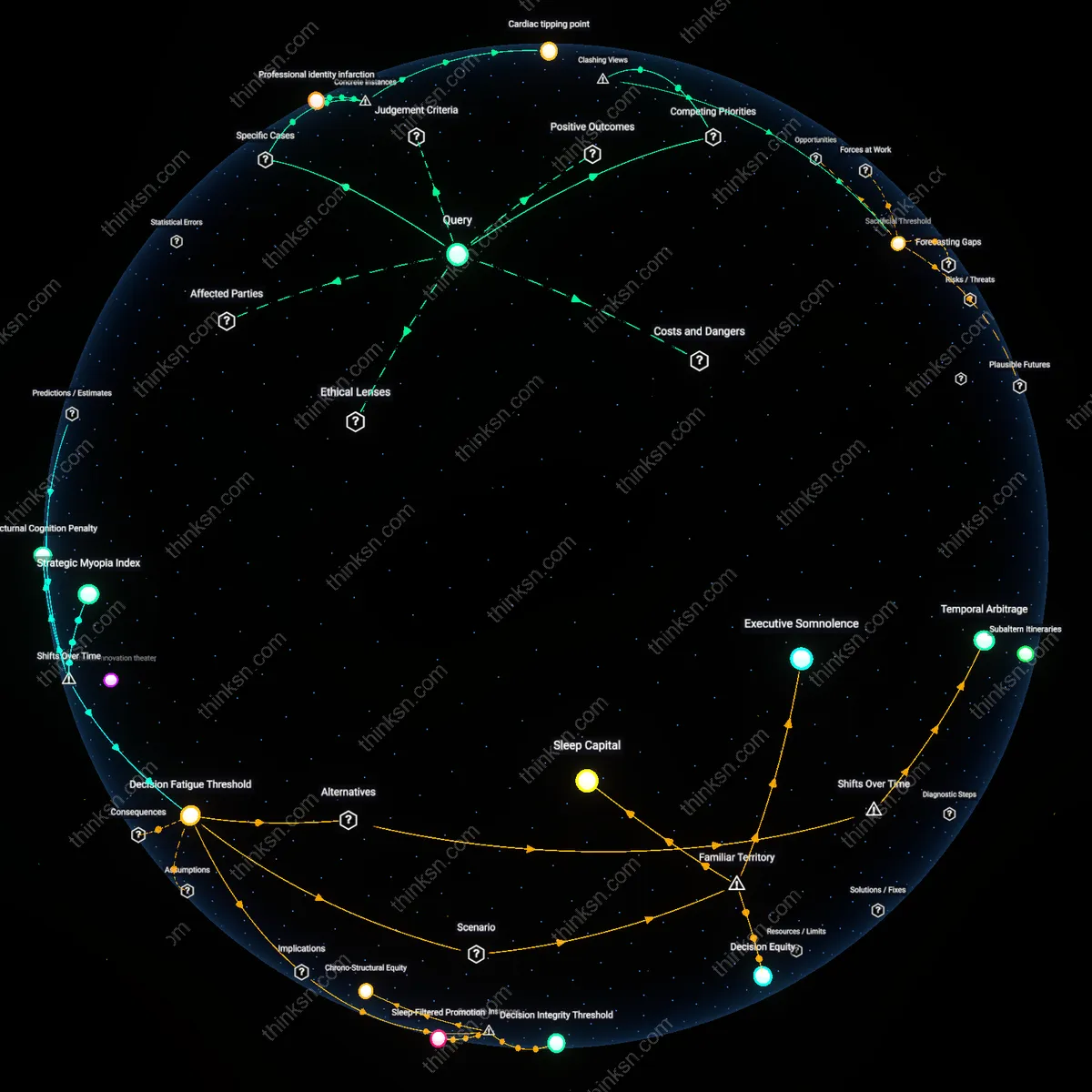
Sacrificial Threshold
A career change becomes medically necessary when prolonged cortisol elevation from job-related stress crosses into organ damage, detectable via biomarkers like C-reactive protein, because healthcare systems in industrialized nations only intervene after physiological collapse, not psychological erosion—this reveals that medicine treats the body as a salvageable machine post-failure, not a system to be preserved preventively, making the non-obvious claim that clinical thresholds, not lived suffering, determine actionable risk.
Aspirational Debt
The moment a career impedes circadian rhythm alignment—measured by melatonin onset disruption—a costly switch is justified, because chronic circadian misalignment degrades dopaminergic pathways essential for future planning, revealing that career decisions made under sleep deprivation systematically impair long-term judgment; this reframes 'ambition' as a cognitively compromised forecast, exposing how the pursuit of professional stability often depends on the erosion of neural foresight.
Cardiac tipping point
Prolonged stress from a misaligned career became a serious health risk necessitating change when journalist Sarah Ellison documented the 2011 collapse of David Carr, whose relentless work at The New York Times amid internal misalignment with digital media’s pace triggered a fatal heart attack at his desk, revealing how chronic cognitive dissonance in high-output newsrooms can catalyze irreversible cardiovascular events. The mechanism—sustained sympathetic nervous system activation due to identity-work mismatch in a prestige-driven institution—demonstrates that the body’s physiological threshold can mark the only definitive boundary for career recalibration, an outcome invisible until it is absolute.
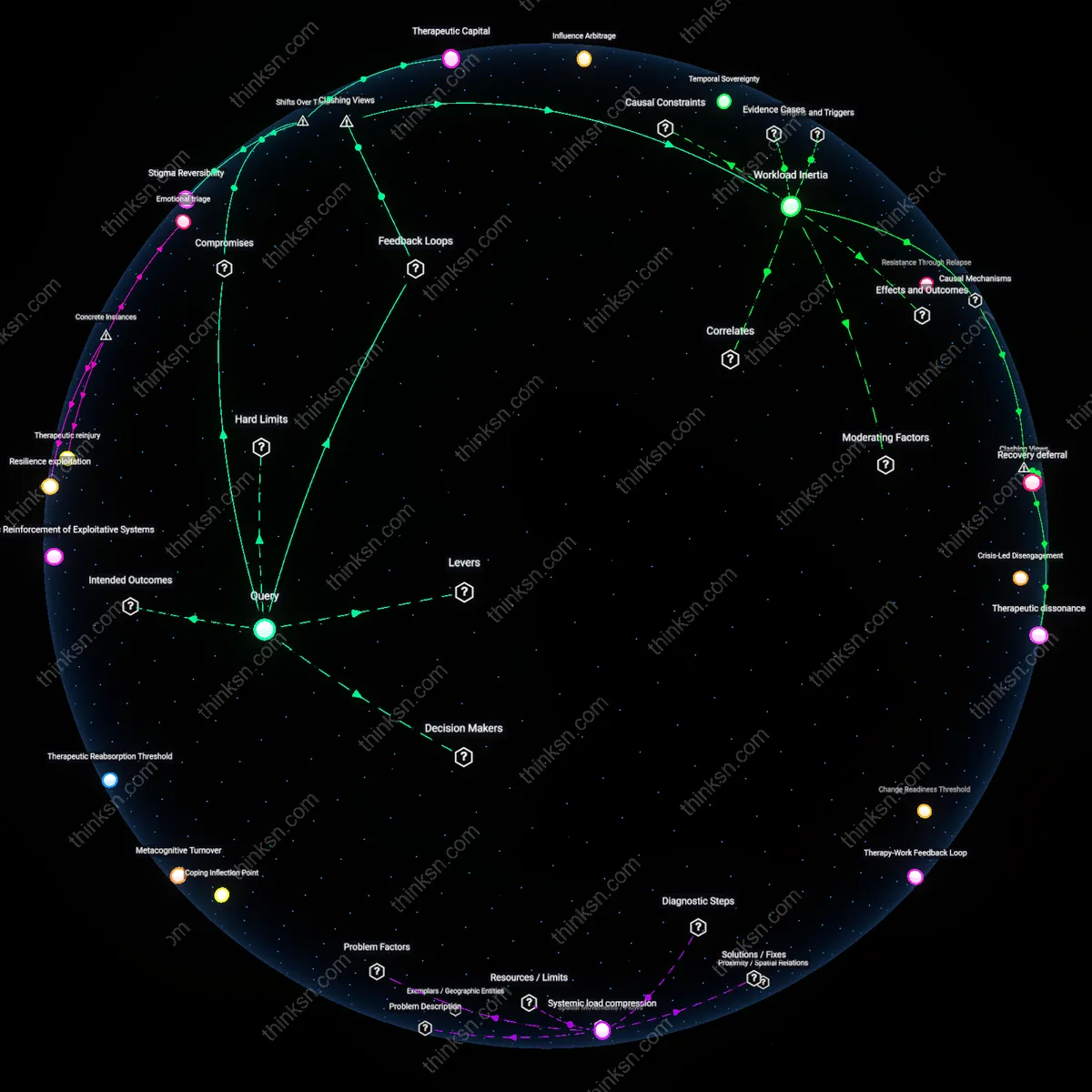
Institutional abandonment effect
At Enron, long-term employees in mid-level compliance roles experienced escalating psychological deterioration after repeatedly conforming to ethically misaligned directives, culminating in documented cases of clinical depression and liver disease that preceded mass resignations before the 2001 collapse, showing how systemic organizational decay transforms career misalignment into somatic illness when institutional loyalty outlasts moral coherence. This dynamic—where employees’ health degrades not from overwork but from sustained betrayal of professional identity under eroding governance—reveals that the body registers institutional corruption as chronic toxic exposure, making career change a survival mechanism rather than a choice.
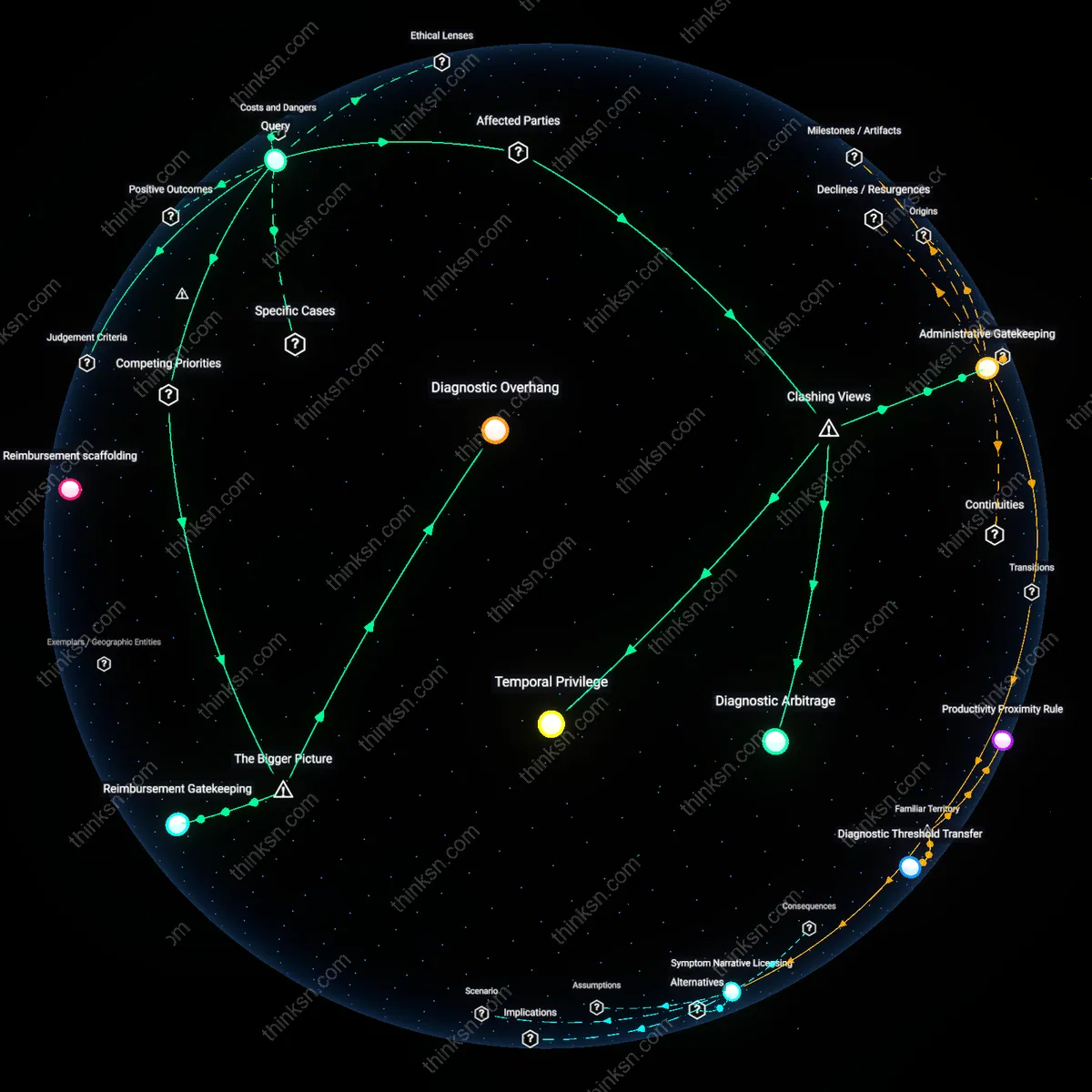
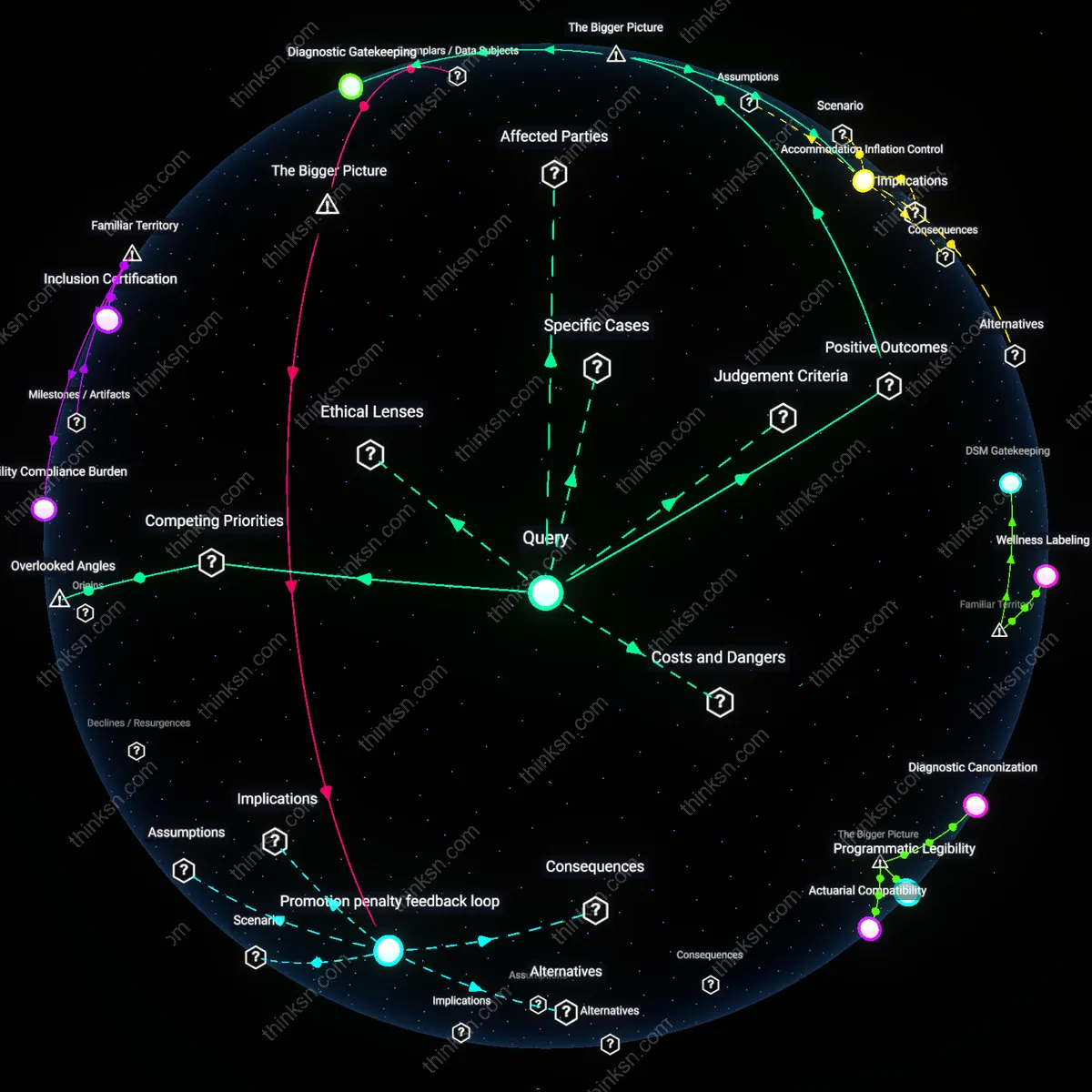
Professional identity infarction
In the NHS England case of Dr. Hadiza Bawa-Garba, the 2015 wrongful death conviction and subsequent erasure from the medical register led to a documented acute decline in her mental health, but the deeper crisis emerged from years of systemic misalignment between her clinical judgment and bureaucratic mandates, where repeated suppression of professional autonomy incubated treatment-resistant anxiety long before legal action, illustrating how career structures that nullify expert identity can induce a slow psychological infarction. This pattern—where the erosion of agency within a vocation becomes pathogenic independent of external crisis—demonstrates that alignment with professional ethos is as vital to health as workload or compensation.