Is Requesting Mental Health Diagnostics for Accommodations Unethical?
Analysis reveals 4 key thematic connections.
Key Findings
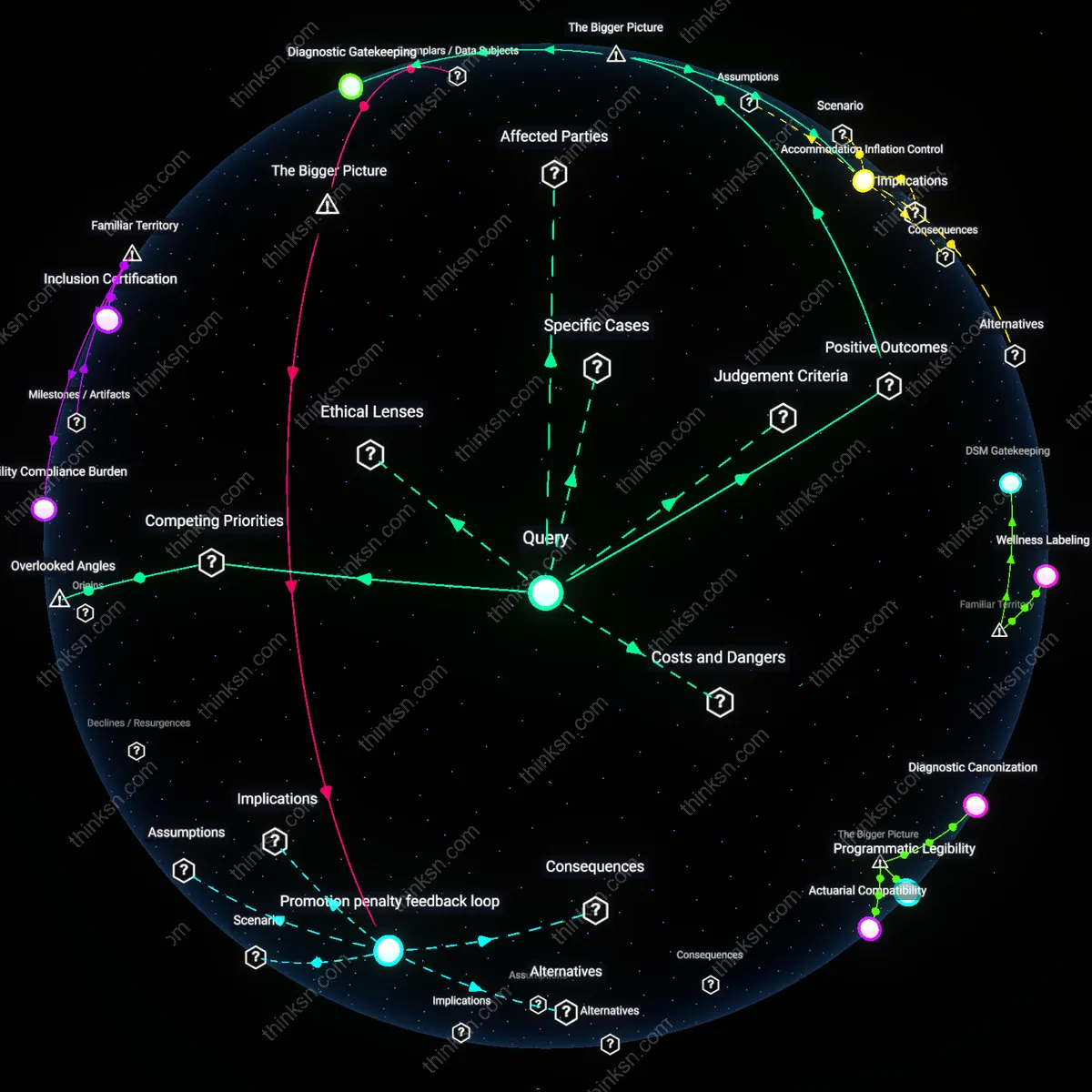
Diagnostic Gatekeeping
Requiring mental-health diagnoses for accommodations strengthens institutional accountability by aligning workplace adjustments with clinically validated criteria, ensuring that resources are allocated where they are most likely to yield measurable functional improvements. This process leverages established medical frameworks—such as DSM-5 classifications and psychiatrist evaluations—enabling employers to standardize requests across jurisdictions and avoid arbitrary or unverifiable claims. The non-obvious consequence is that diagnostic gatekeeping creates a feedback loop where only medically codified conditions become legible to organizational systems, thus reinforcing the authority of clinical psychiatry in defining workplace disability.
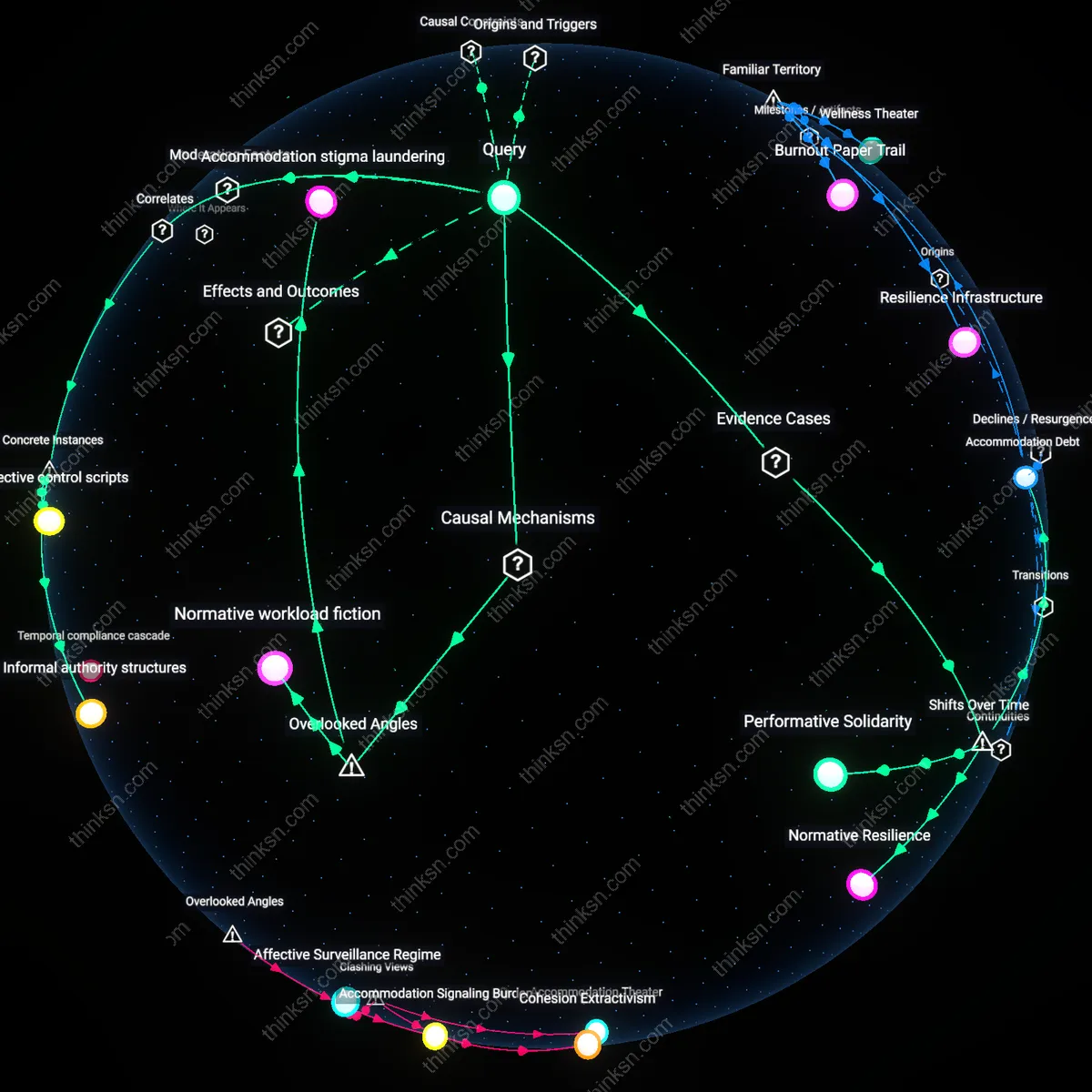
Stigma Codification
Mandating formal diagnoses converts private psychological experiences into official records, which paradoxically legitimizes mental health concerns within corporate bureaucracy while embedding stigma into personnel data systems. When HR departments treat diagnosed conditions as administrative categories, they inadvertently classify employees through medical labels that can influence performance evaluations or promotion trajectories, even when accommodations are granted. This reveals how the procedural need for documentation activates structural stigma—not through individual prejudice, but via routine data management practices in large organizations that reify diagnostic status as a permanent attribute.
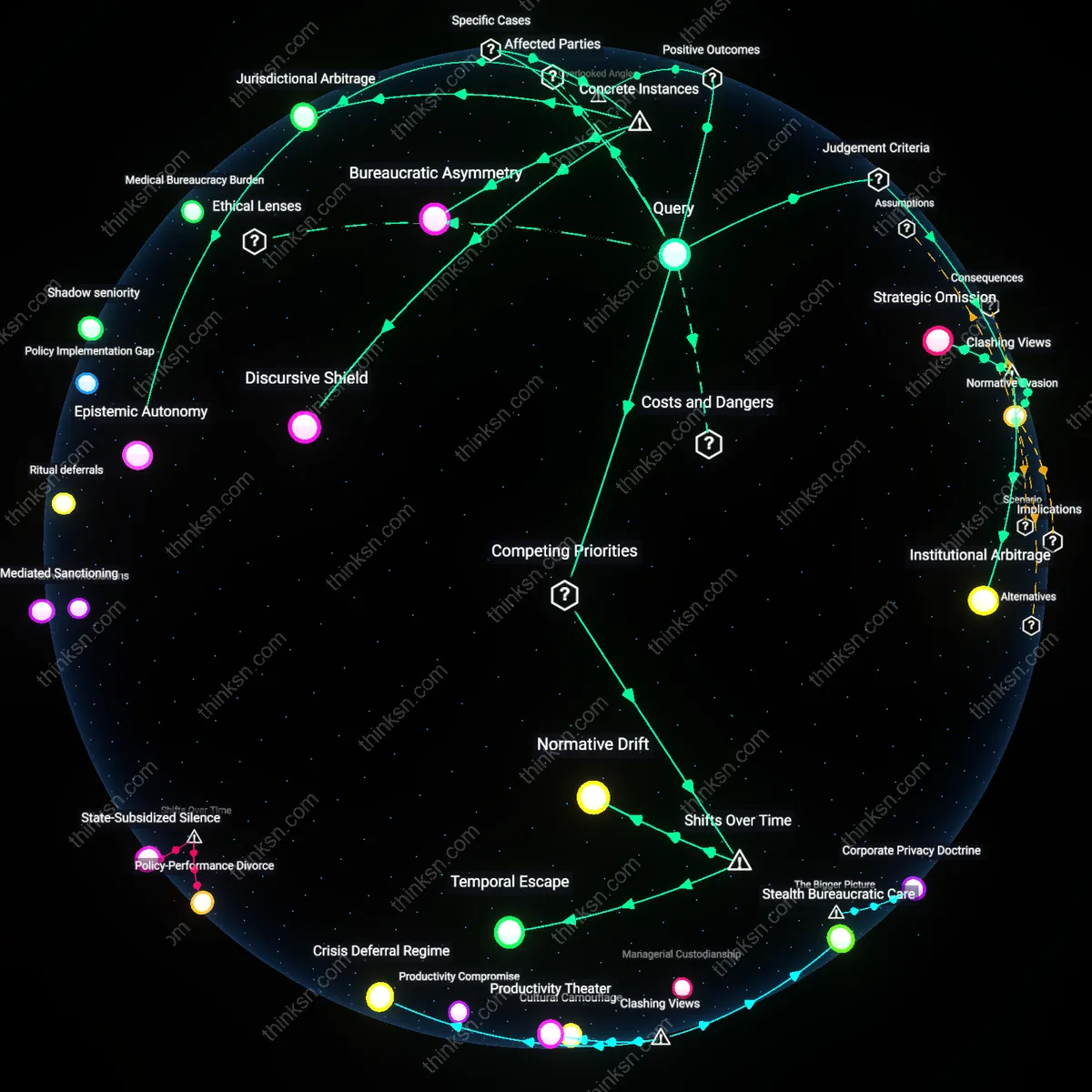
Accommodation Inflation Control
Employers who require diagnoses prevent the dilution of accommodation resources by ensuring that interventions are tied to verifiable impairments, preserving the effectiveness of support systems for those with severe conditions. In environments like multinational corporations or public-sector agencies, where accommodation budgets and staffing ratios are fixed, unchecked requests could overwhelm capacity and reduce overall program sustainability. The underappreciated mechanism is that diagnostic requirements function not as obstacles per se, but as rationing tools embedded in equitable distribution systems, calibrated by legal risk management and insurance underwriting standards.
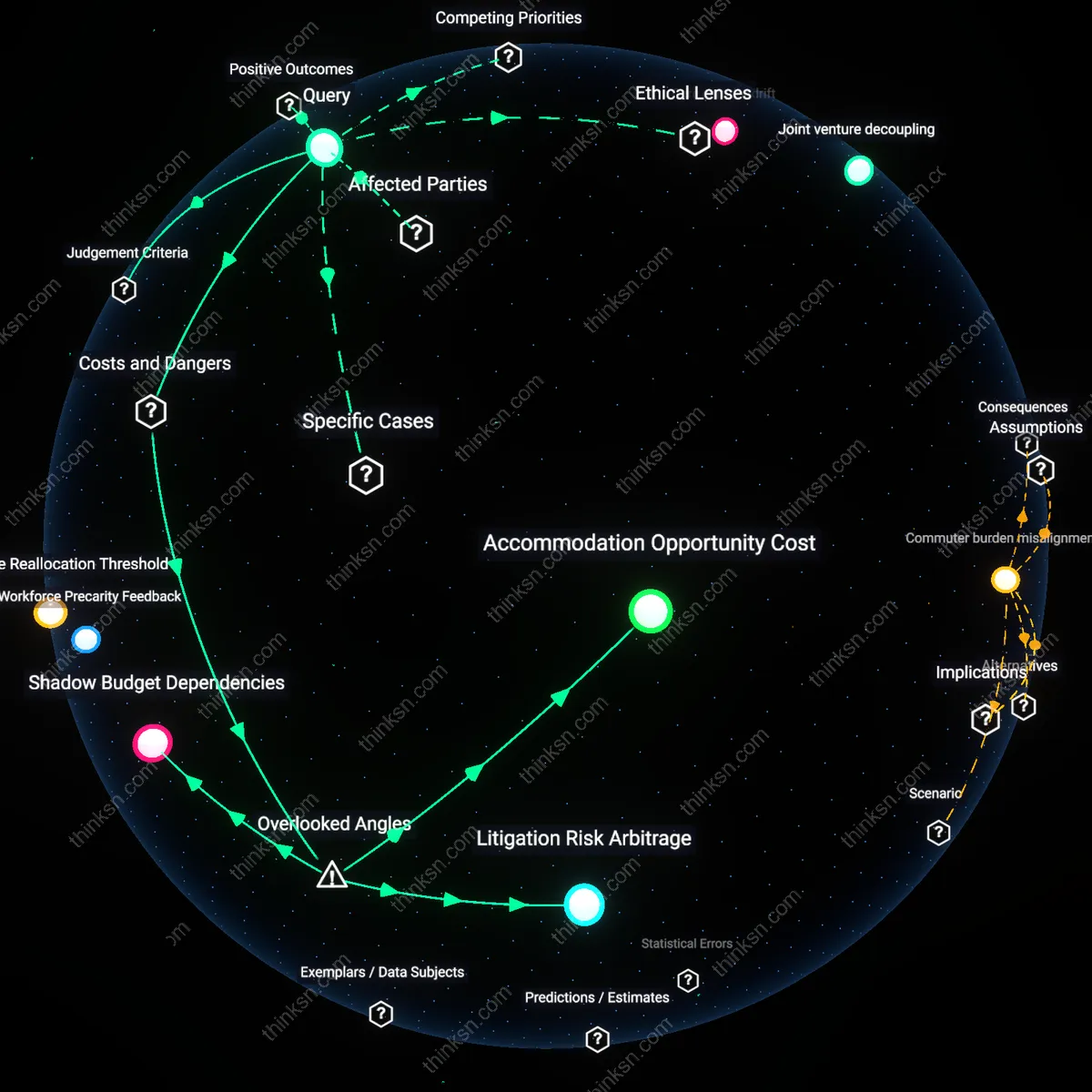
Accommodation Inflation
Mandating diagnoses unintentionally inflates the perceived rarity and cost of accommodations, making routine adjustments seem like exceptional medical privileges rather than standard workplace flexibility. This happens because diagnostic gatekeeping frames all mental health support as medically exceptional, which triggers heightened scrutiny, legal documentation, and managerial resistance—turning simple schedule shifts or noise-reducing headphones into high-stakes medical transactions. The overlooked dynamic is that requiring diagnosis doesn't just protect employer boundaries; it actively reshapes organizational culture to treat baseline human variability as pathological, thereby increasing the social and procedural cost of asking for help even when no real resource burden exists. This transforms the ethical question from one of individual fairness to a systemic distortion of normative workplace norms.