Home or Nursing Home? Weighing Safety and Autonomy for Aging Parents?
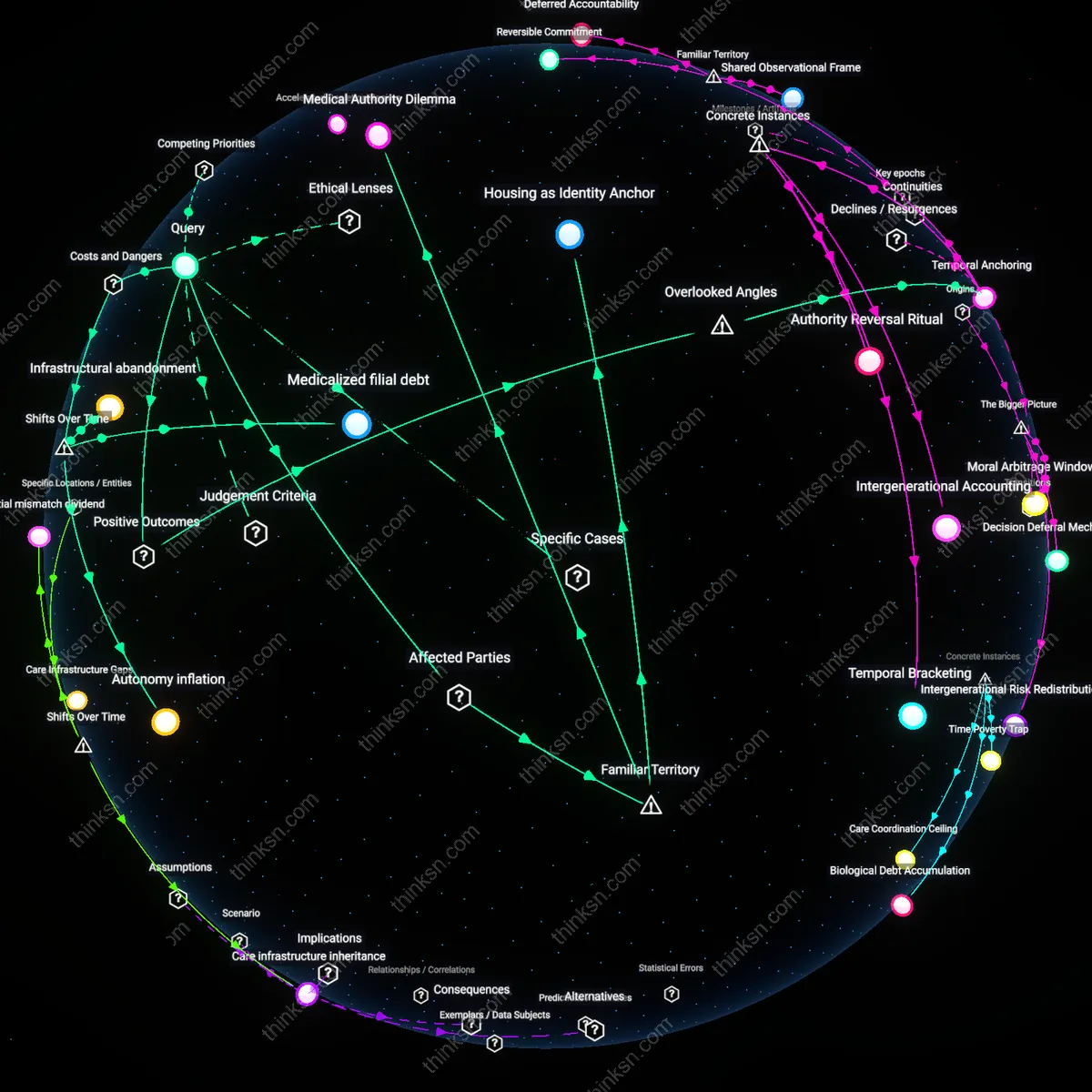
Analysis reveals 7 key thematic connections.
Key Findings
Family Caregiver Burden
Prioritize the emotional and physical toll on adult children by acknowledging their role as de facto care managers within the home, where familial duty intersects with limited medical infrastructure; this step activates the informal caregiving system that absorbs the gap between clinical recommendations and domestic reality, revealing how personal autonomy is often preserved at the cost of the caregiver’s well-being—a tradeoff rarely acknowledged in medical consultations but central to household decision-making.
Medical Authority Dilemma
Deflect clinical recommendations by invoking a parent’s legal right to refuse treatment, thereby positioning physicians and social workers as external authorities whose advice competes with familial loyalty and lived experience; this step exploits the boundary between medical expertise and civil rights, exposing how healthcare providers often lack enforcement power in home settings despite clear safety risks—a structural limitation that allows dangerous situations to persist under the guise of autonomy.
Housing as Identity Anchor
Frame the parent’s home as a repository of biography and continuity, where staying becomes less about physical safety and more about preserving a cohesive life narrative against institutional erasure; this step leverages the deep cultural association between place and personhood, revealing how the fear of losing identity in unfamiliar environments often outweighs rational assessments of care quality—making the house itself a silent participant in end-of-life decisions.
Temporal Anchoring
An adult child can reframe the transition to skilled nursing as a time-bound trial rather than a permanent surrender of autonomy, which preserves the parent’s sense of control while satisfying medical safety thresholds. This works because families often interpret medical recommendations as irreversible mandates, yet hospitals and nursing facilities routinely permit short-term placements that function as diagnostic periods for functional decline—during which the parent’s response to structured care can be evaluated objectively. What is typically overlooked is how the mere presence of a re-entry possibility transforms psychological resistance into conditional acceptance, not because the medical need diminishes, but because the perception of irreversible loss—the true driver of conflict—is mitigated. Temporal Anchoring surfaces the underappreciated role of time-contingent decisions in dissolving zero-sum autonomy-safety tradeoffs.
Medicalized filial debt
Insist that adult children institutionalize a parent to fulfill medical authority's safety mandates, because post-1980s liability frameworks have shifted elder risk management from familial discretion to clinical oversight, making home care negligence when professionals designate nursing needs. This reframing turns adult children into enforcers of institutional logic, where resisting medical advice risks legal and ethical censure, even when honoring parental autonomy; the non-obvious outcome is that filial duty is no longer defined by emotional or cultural loyalty but by compliance with healthcare-generated risk assessments anchored in post-1990s elder protection statutes and malpractice deterrence norms.
Autonomy inflation
Uphold the parent’s insistence on remaining home as inviolable, because from the 1970s onward, bioethical discourse elevated individual autonomy to a first principle, displacing older familial or communal decision-making models, particularly after the 1972 President’s Commission emphasized self-determination in care. This shift means that rejecting skilled nursing against medical advice is no longer seen as irrational but as an exercise of civil rights, creating a norm where safety concerns are downgraded if they contradict personal choice—producing a dangerous paradox where preserving autonomy undermines its preconditions, especially as home environments become de facto unregulated care sites.
Infrastructural abandonment
Delay relocation by retrofitting the home with safety modifications funded through piecemeal Medicaid waivers, because the 1999 Olmstead decision catalyzed a policy pivot toward community-based care, defunding institutional alternatives while underinvesting in robust home-care infrastructure. This creates a precarious compromise—older adults stay home not by choice but due to systemic avoidance of nursing beds, and adult children manage care gaps with informal labor and consumer-grade tech, exposing all to accumulated risks that formal care would mitigate; the overlooked outcome is that 'home safety' is sustained less by genuine support than by deflection of public responsibility onto families over decades of austerity-driven health planning.