Do Insurance Complaints Override Cardiac Surgeon Recommendations?
Analysis reveals 9 key thematic connections.
Key Findings
Regulatory enforcement
Filing a complaint immediately mobilizes the state insurance commissioner's investigation power, enabling the commissioner to overturn or negotiate coverage and thus shift bargaining power away from the insurer. Under state law, the insurer must undertake a formal appeal before declining coverage; the commissioner can issue enforcement actions for violations, which forces the insurer to reassess its decision rather than simply refuse coverage. The significance is that the complaint turns a unilateral insurer denial into a regulated dispute that the insurer cannot ignore, a nuance often missed by patients who assume the process ends at the insurer level.
Market adequacy
Complaints serve as a trigger for the commissioner's market adequacy reviews, which can force insurers to conform to out‑of‑network coverage standards and alter the broader pricing power that insurers wield. In highly consolidated insurance markets, a single denial can prompt the state to investigate whether the insurer’s conduct violates network adequacy regulations, leading to enforcement or corrective action that affects all policyholders. The underappreciated consequence is that a complaint does not only resolve one patient’s issue but also initiates a systemic check on insurer practices, subtly shifting market dynamics in favor of patient access.
Public transparency
Complaints unlock the insurance commissioner’s public transparency mechanism, publishing denied claims and thereby mobilizing public pressure that can compel insurers to revise coverage policies. When the commissioner posts a denied recommendation on its website, media and patient advocacy groups can amplify local outrage, creating a reputational risk for the insurer that drives policy changes even without formal enforcement. Thus, a complaint can shift power by moving the battleground from private negotiation to public accountability, a dimension that most patients overlook when filing complaints.
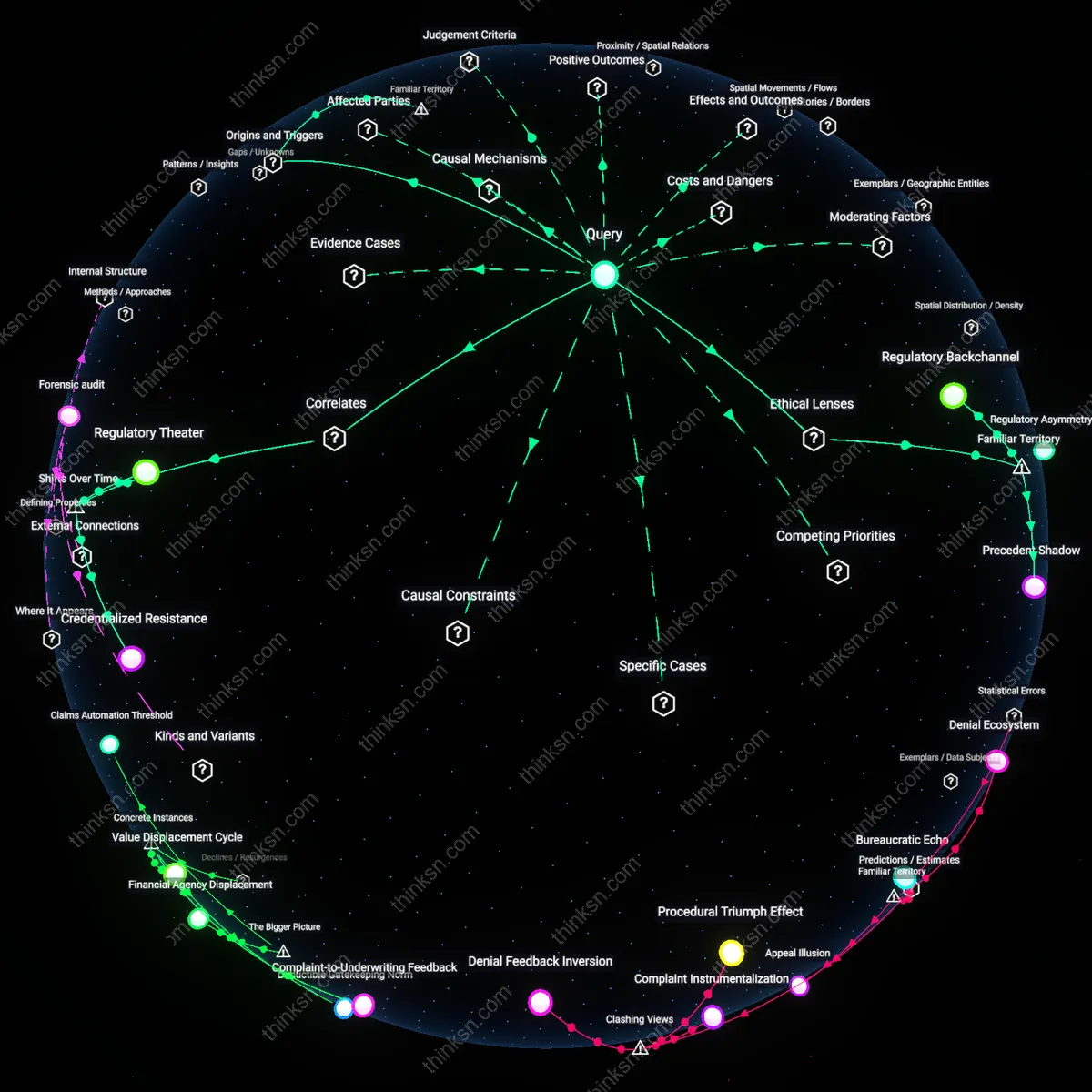
Regulatory Theater
Filing a complaint with the state insurance commissioner rarely alters insurer behavior but increasingly functions as a symbolic act that reflects post-1990s healthcare consumerism, where patients seek procedural validation even when structural power remains unchanged; this mechanism emerged as insurance appeals formalized in the 1990s, creating a performative avenue for redress that mimics empowerment without redistributing decision-making authority; what is non-obvious is that the act’s persistence relies not on efficacy but on its role in sustaining public trust in privatized health governance.
Asymmetric Accountability
The capacity of patients to influence insurer decisions via commissioner complaints diminished after the 2006 shift toward high-deductible health plans, which realigned insurer risk exposure and reduced sensitivity to individual appeals, embedding a new dynamic where regulatory scrutiny is statistically associated with complaint volume but not with reversal rates; this transformation reveals how market-based insurance designs have silently reconfigured responsiveness, making formal accountability mechanisms less consequential even as they remain publicly accessible; the underappreciated insight is that regulatory leverage eroded not through overt policy repeal but via incremental financial engineering of coverage.
Credentialized Resistance
Since the 2010s, cardiac surgeons' recommendations carry more weight in complaints filed with state commissioners when embedded within standardized clinical documentation, reflecting a shift from provider authority being granted by institutional affiliation to being contingent on bureaucratic legibility; this evolution marks the transition from medicine as profession-based trust to audit-ready evidence, where power accrues not to the clinician per se but to those who can translate medical judgment into administratively viable forms; the non-obvious consequence is that resistance to denials now depends less on clinical prestige than on adherence to documentation regimes shaped by insurance data systems.
Regulatory Backchannel
Filing a complaint with the state insurance commissioner gives patients access to a regulatory backchannel that bypasses the insurer’s internal appeals, leveraging state oversight to reframe clinical disputes as administrative failures. This process activates a formal accountability mechanism—an external review body with statutory authority to compel insurer justifications—inserting public scrutiny into a typically closed, privatized decision chain. The non-obvious force of this move lies in how it exploits bureaucratic procedure to convert medical marginalization into a case file, mobilizing institutional inertia against the insurer rather than relying on clinical persuasion, which most patients intuitively expect.
Moral Witnessing
Filing a complaint transforms the patient from passive claimant to moral witness, asserting ethical standing within a system that otherwise reduces care decisions to financial triage. This act invokes a public ethos of fairness rooted in deontological ethics, where the mere documentation of denial becomes a form of civic resistance against utilitarian cost-benefit logic dominant in managed care. What is underappreciated is that people remember this act not for its legal outcome but for its symbolic weight—how it aligns with widespread cultural narratives of 'being heard' by a higher authority, even when material redress is unlikely.
Precedent Shadow
Each complaint contributes to a precedent shadow that shapes future insurer behavior by aggregating isolated denials into actionable regulatory patterns, operating through the legal doctrine of administrative accumulation where repeated findings of questionable denials can trigger systemic audits or rule changes. This functions beneath individual awareness but within the logic of bureaucratic governance, where mass micro-complaints form invisible datasets that commissioners use to negotiate enforcement thresholds. The overlooked insight is that people associate complaints with personal outcomes, yet their real power often lies in collective statistical presence, not individual resolution.