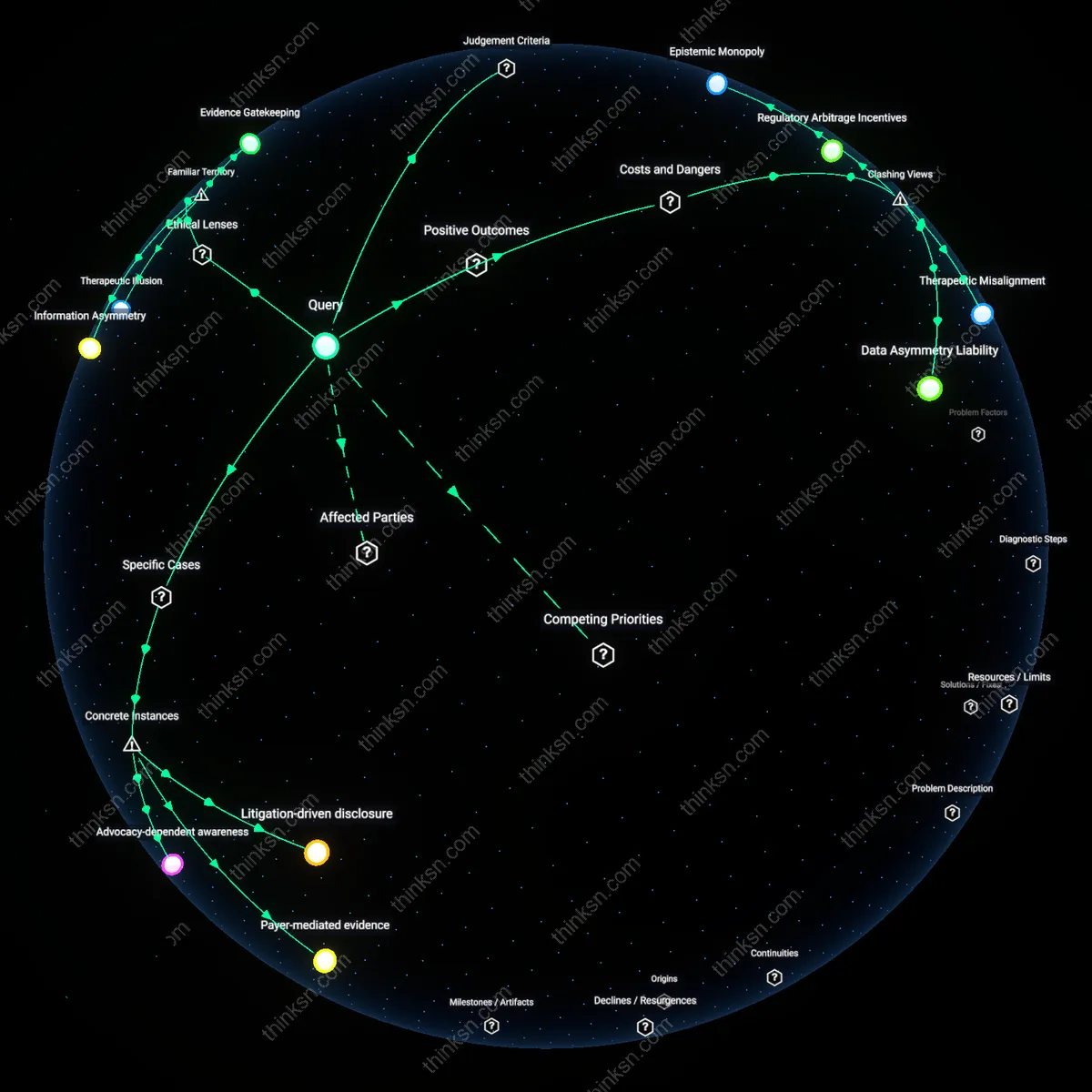
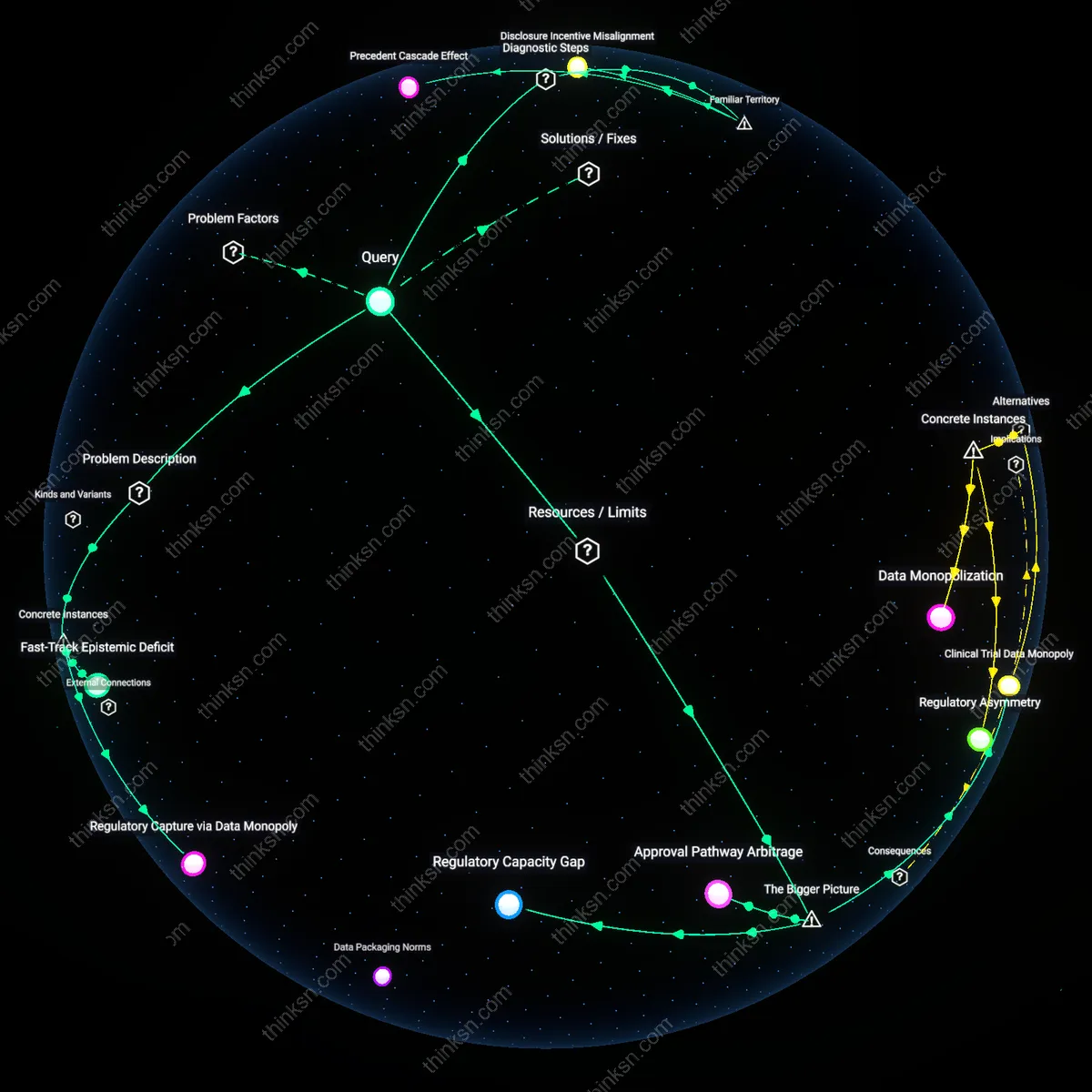
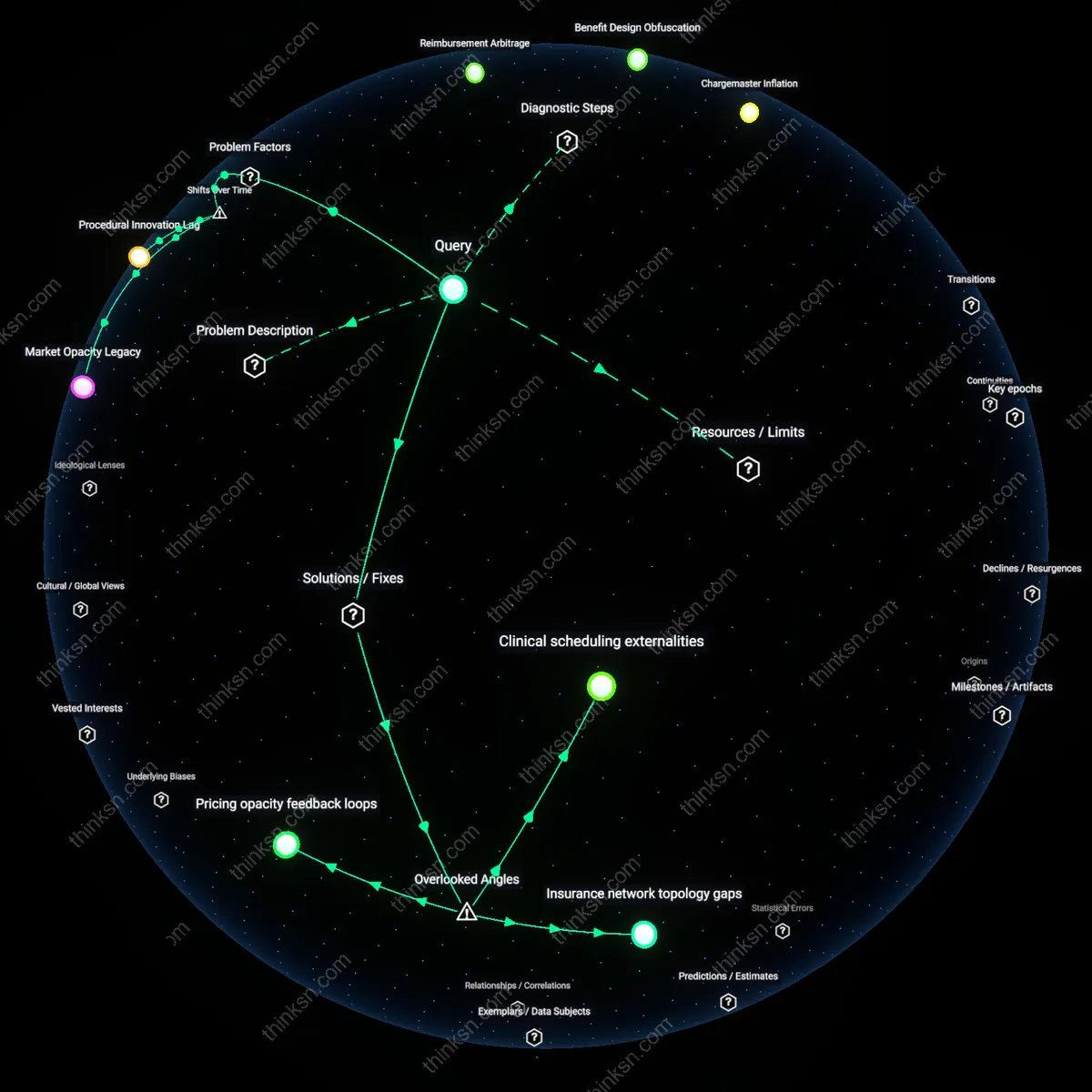
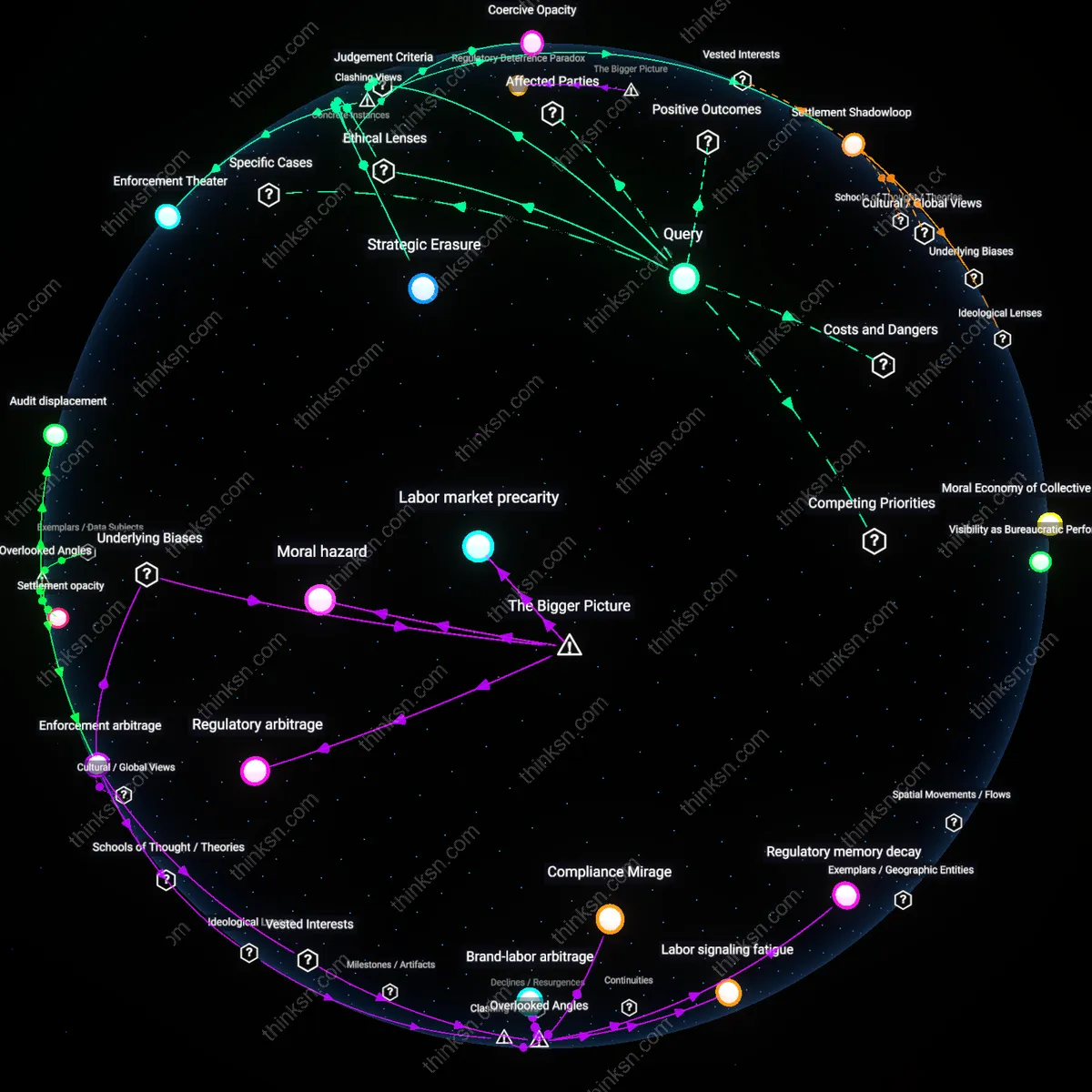
Is Limited Data Harming Evidence-Based Patient Decisions?
Analysis reveals 11 key thematic connections.
Key Findings
Regulatory Arbitrage Incentives
Restricting clinical trial data access for a specialty biologic incentivizes firms to conduct pivotal trials in jurisdictions with weaker transparency mandates, thereby reducing global comparability of safety outcomes. Multinational sponsors exploit regulatory fragmentation—such as conducting trials in countries without mandatory ClinicalTrials.gov registration—to anchor approval pathways in lenient regimes, then leverage reciprocity agreements to enter stricter markets without full data disclosure. This undercuts the principle of epistemic equity, as patients in transparent jurisdictions unknowingly rely on evidence bases contaminated by selectively disclosed, jurisdictionally gated findings—what matters is not just data withholding, but the strategic geographic choreography of trial execution that escapes current ethical scrutiny.
Therapeutic Substitution Distortion
Limited data access distorts off-label substitution patterns by obscuring comparative biomarker response curves, causing clinicians to misattribute efficacy to drug class rather than compound-specific mechanisms, particularly in autoimmune biologics with overlapping targets. Because pharmacoeconomic models and hospital formularies rely on published head-to-head trials—which are rare when data is restricted—providers use flawed proxy metrics like binding affinity or half-life to justify therapeutic substitution, leading to suboptimal patient outcomes that are then misread as patient-specific variability rather than systemic inference failure. The hidden dependency is the unsupervised extrapolation from partial pharmacodynamic data, which masquerades as clinical judgment but is actually a structural artifact of data containment.
Epistemic Monopoly
Restricted clinical trial data access entrenches an epistemic monopoly where regulatory agencies and originator manufacturers become the sole arbiters of evidence, preventing independent validation of a biologic’s efficacy or safety profile. This control enables selective interpretation of results through proprietary analytical models and unpublished endpoints, shielding methodological flaws or unfavorable outcomes from peer scrutiny—particularly in rare disease contexts where trial samples are small and statistical manipulation has outsized impact. The non-obvious danger is not mere opacity, but the systematic displacement of clinical uncertainty from scientific debate into patient risk, where off-label use proliferates without corrective counter-evidence.
Therapeutic Misalignment
When clinicians cannot access granular trial data for specialty biologics, treatment decisions default to marketing narratives and guideline algorithms that prioritize regulatory approval milestones over real-world patient heterogeneity, producing therapeutic misalignment. This misalignment manifests in oncology and autoimmune clinics where biomarker subpopulations showing no benefit—or harm—are obscured by aggregated response rates, yet insurers and institutions incentivize use via formulary placement. The clash lies in exposing that ‘evidence-based medicine’ in this context is less a scientific standard than a governance mechanism that offloads evidentiary risk onto patients, particularly those with comorbidities excluded from trials.
Data Asymmetry Liability
Pharmaceutical companies leveraging data access restrictions to delay generic or biosimilar competition convert clinical opacity into a financial instrument, where the liability of data asymmetry is borne not by the sponsor but by health systems and patients making irreversible treatment choices. By withholding individual participant data or complete safety datasets, sponsors exploit regulatory safe harbors to prolong market exclusivity under the guise of patient privacy or trade secrecy, even as meta-analyses and post-marketing surveillance remain impaired. The underappreciated consequence is that delayed access to disconfirming evidence functions not as a loophole but as a structural feature of biologic markets, embedding harm into the cost-effectiveness calculations of public payers.
Information Asymmetry
Restricted clinical trial data access entrenches a power imbalance between pharmaceutical developers and treating physicians by limiting access to raw efficacy and safety outcomes. Biologic manufacturers, protected by intellectual property doctrines like those in the U.S. Hatch-Waxman Act, control dissemination of full datasets, which the FDA accepts without public release—this institutionalizes asymmetric information flow where regulators and sponsors possess deeper evidence than clinicians. This mechanism contradicts the principles of deontological medical ethics, which demand full disclosure to enable informed consent, and undermines physicians’ capacity to interpret real-world applicability for individual patients. The underappreciated consequence is not just delayed knowledge transfer but the systemic design of opacity as a legitimate regulatory outcome, not a failure.
Therapeutic Illusion
When only summarized or redacted clinical trial results are released for specialty biologics, patient advocacy groups and media outlets often amplify isolated success stories, fostering a belief in transformative outcomes even when broader efficacy is marginal. This occurs through the normalization of anecdotal evidence in public discourse, especially in disease communities desperate for breakthroughs, where political liberalism's emphasis on individual autonomy amplifies the right to access unproven treatments despite incomplete evidence. The dynamic is reinforced by direct-to-consumer advertising norms in the U.S., which permit promotion based on partial data, legally sanctioned under commercial speech doctrines. The non-obvious risk is that transparency is symbolically satisfied—through press releases or abstracts—while substantive data remains sealed, creating a public impression of openness that masks evidentiary gaps.
Evidence Gatekeeping
Academic researchers denied access to full clinical trial datasets from biologic trials are prevented from conducting independent validation or subgroup analyses, effectively ceding epistemic authority to industry-sponsored authors. This gatekeeping is codified through contractual research agreements and data ownership clauses enforced by corporate legal teams, operating under neoliberal frameworks that prioritize private control over knowledge as a form of capital. Peer-reviewed journals, despite endorsing data-sharing policies, lack enforcement power, allowing selective publication to persist as the default. The underappreciated effect is that scientific reproducibility—the cornerstone of positivist medical research—becomes contingent on permission, transforming validation from a communal norm into a negotiated privilege.
Litigation-driven disclosure
The restricted access to clinical trial data for the biologic Avastin in metastatic breast cancer led to delayed patient awareness of its limited efficacy, which only became widely evident after legal battles forced data transparency through FDA hearings and congressional testimony. The mechanism here is that external legal and regulatory pressure—not voluntary industry disclosure—became the conduit for revealing efficacy gaps, illustrating how evidentiary opacity can persist until adversarial systems compel release. This is non-obvious because it reveals that transparency in biologics is not primarily a function of scientific norms but of institutional contestation.
Payer-mediated evidence
When NICE in the UK restricted reimbursement for the biologic Tysabri in multiple sclerosis due to incomplete long-term safety data, it effectively shifted the burden of evidence generation post-market, altering how patients perceived risk in treatment decisions. The mechanism operates through health technology assessment bodies substituting for comprehensive pre-approval data access, thereby embedding payer logic into clinical judgment. This case illustrates that limited data availability can reposition third-party payers as de facto interpreters of evidence, a role rarely acknowledged in patient consent processes.
Advocacy-dependent awareness
The limited availability of comparative trial data for the biologic Soliris in atypical hemolytic uremic syndrome meant that patient understanding of its benefit-risk profile emerged primarily through disease-specific advocacy groups like the aHUS Alliance, which negotiated access to redacted summaries. The mechanism here relies on civil society organizations to decode and redistribute restricted scientific information, revealing that patient decision-making becomes contingent on the presence and capacity of activist intermediaries. This is underappreciated because it shows that transparency is unevenly distributed across disease communities based on organizational density, not data availability per se.