Do Biologics Offer Too High a Cognitive Cost for Autoimmune Patients?
Analysis reveals 6 key thematic connections.
Key Findings
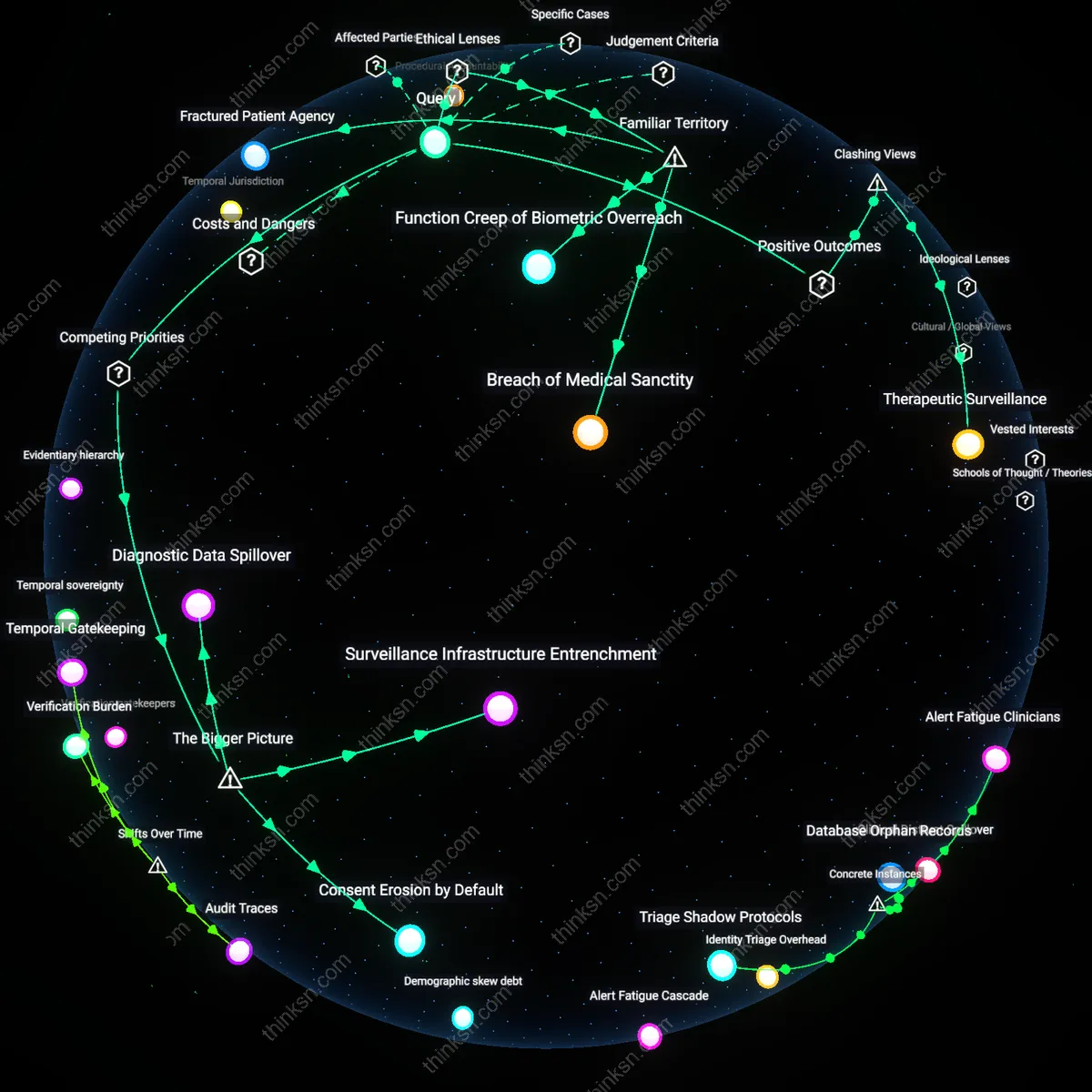
Therapeutic Surveillance Trap
Biologic therapies demand monthly blood tests to detect immune suppression, imposing a cognitive and logistical toll on patients managing chronic conditions like rheumatoid arthritis; these tests, while intended to prevent life-threatening infections, often trigger anxiety-driven non-adherence when patients equate lab frequency with disease severity. The system assumes compliance with monitoring as a proxy for safety, but in practice, it generates decision fatigue among working-age patients juggling treatment with employment and caregiving, undermining the very adherence it seeks to enforce. What’s underappreciated is that the public sees frequent monitoring as evidence of therapy seriousness, not as a hidden barrier to sustained use—this familiarity masks its role in patient burnout and early discontinuation.
Clinical Invisibility Tax
Autoimmune patients on biologics face invisibility in primary care settings where providers lack expertise in interpreting complex immunology panels, leading to delayed response when flare signals emerge between scheduled infusions; this creates a false sense of control where lab compliance substitutes for clinical vigilance. The reliance on numerical biomarkers encourages dismissal of subjective symptoms, particularly in women and minorities whose pain reports are historically underweighted, resulting in preventable hospitalizations. The unspoken cost is not just the blood draw schedule, but the systemic deferral of authority to data over patient voice—a risk normalized because labs feel like progress, even when they displace clinical judgment.
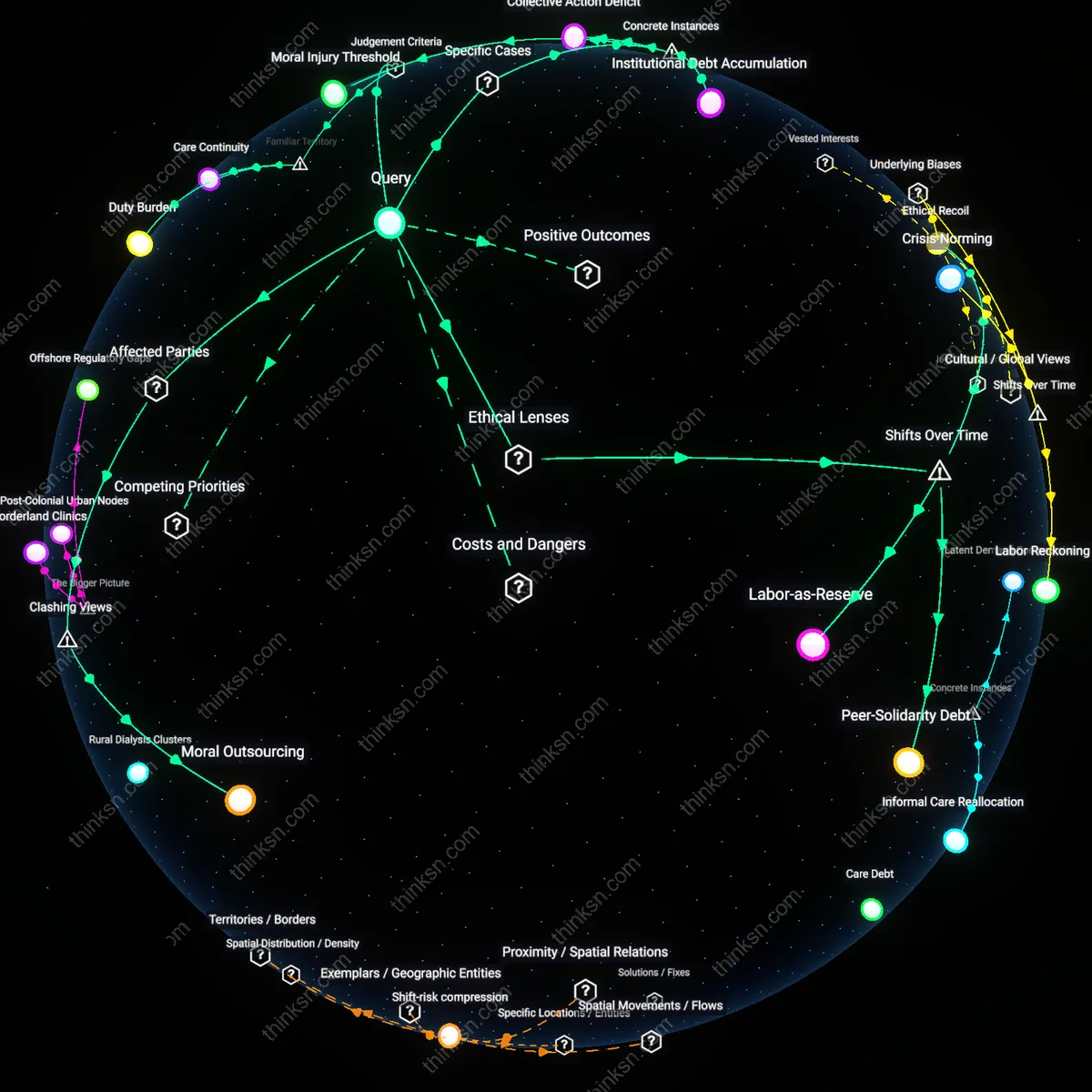
Inflammation Discounting
Reducing flare frequency through biologics is valorized in patient education materials and drug advertising as ‘returning to normal,’ but this narrative discounts the cumulative toll of vigilance required to sustain remission, particularly when monitoring schedules clash with inflexible work or transportation constraints. Patients internalize flare reduction as personal responsibility, framing missed labs as moral failure rather than systemic mismatch, which silences critique of therapy design. The danger lies in conflating biochemical stability with wellness, a simplification so embedded in public discourse that the attrition of mental bandwidth becomes invisible—even to clinicians who measure success solely by C-reactive protein levels.
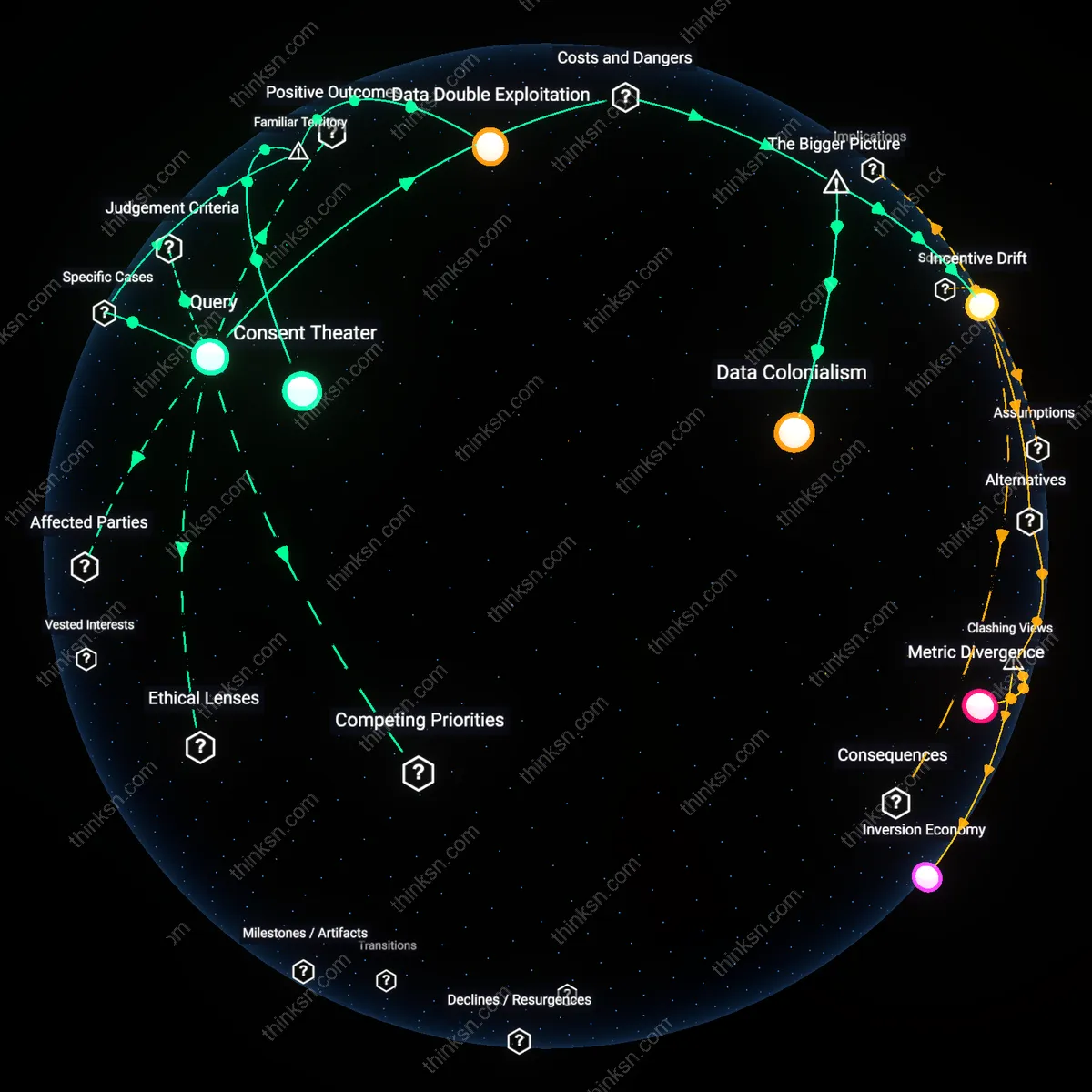
Monitoring labor economy
Biologic therapy regimens that reduce flare frequency disproportionately increase the cognitive and temporal burden of lab monitoring on patients managing autoimmune conditions, creating an invisible labor economy where clinical gains in disease control are offset by the unpaid work of tracking appointments, interpreting results, and coordinating care across fragmented systems—particularly for low-income, elderly, or geographically isolated patients who lack digital literacy or care coordination support. This burden operates through decentralized healthcare infrastructures like community labs and electronic patient portals, where the responsibility to act on results shifts from clinicians to patients, privileging those with social bandwidth to manage complexity while silently excluding others. Most risk-benefit assessments ignore this redistribution of labor because they measure outcomes in clinical metrics, not in enacted patient effort, misrepresenting equity in treatment access.
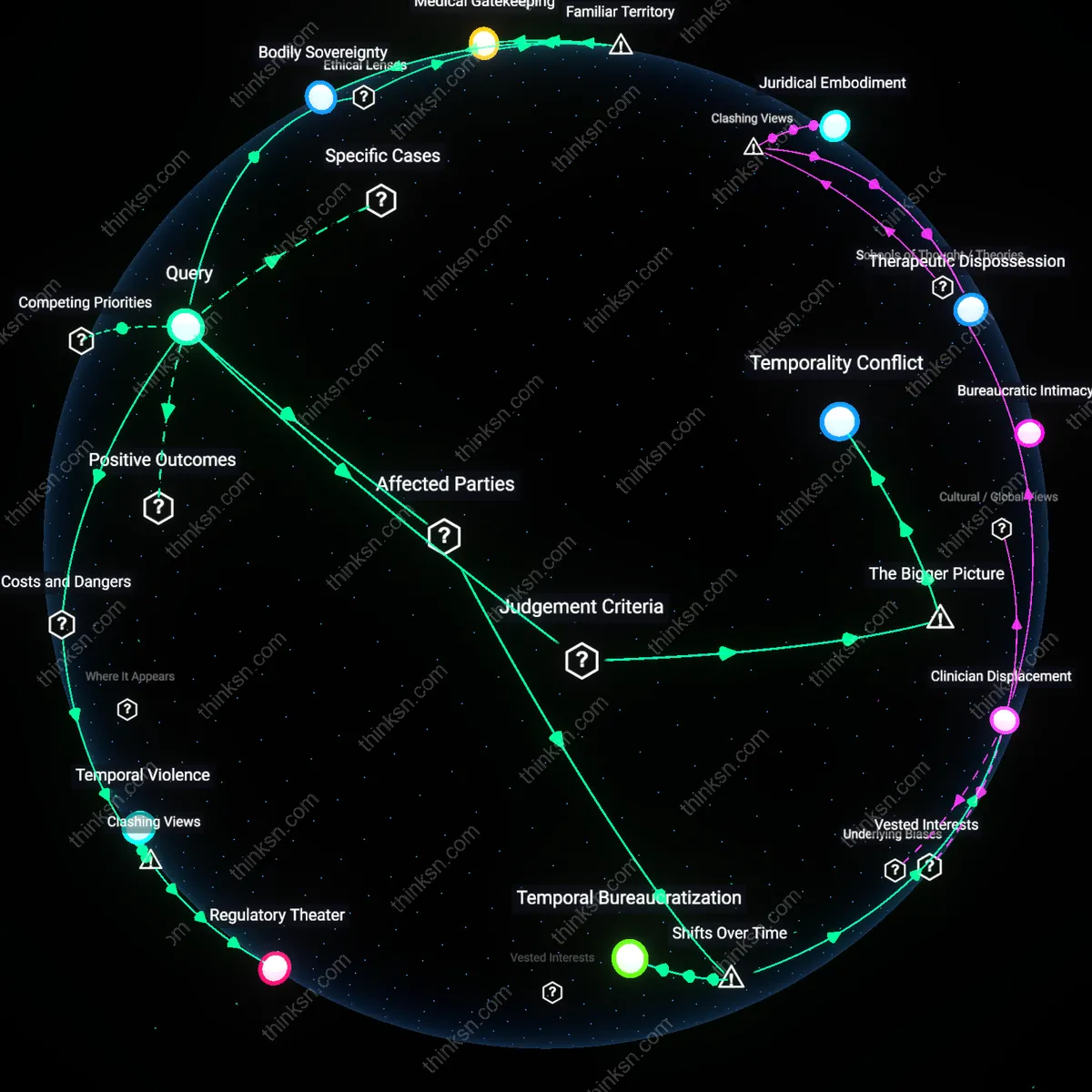
Temporal invisibility of decay
The justifiable trade-off between flare reduction and monitoring burden is skewed by the temporal invisibility of disease decay—patients and clinicians perceive the acute pain of flares immediately but systematically underestimate the cumulative cognitive erosion caused by years of recurring monitoring demands, which degrade executive function and treatment adherence over time. This dynamic operates through episodic healthcare models that assess safety at discrete intervals without modeling the longitudinal attrition of mental bandwidth, especially among neurodiverse or mentally fatigued patients whose coping reserves are already taxed. Standard cost-benefit analyses miss this because they treat monitoring as a neutral procedural step rather than a chronic psychological exposure, leading to overprescription of therapies that are unsustainable at scale.
Institutional tolerance for risk migration
Health systems justify frequent monitoring for biologics not based on patient-level cognitive trade-offs, but by migrating risk from institutional actors (hospitals, insurers) to individual patients, who absorb the uncertainty and labor of detection so that providers can maintain regulatory compliance and avoid liability for adverse events. This risk migration operates through protocols designed by committee-driven oversight bodies like institutional review boards and formularies, which reduce organizational exposure by mandating surveillance but do not track the downstream cognitive costs borne by patients across multiple chronic conditions. The overlooked dynamic is that monitoring frequency reflects institutional risk aversion more than clinical necessity, meaning the 'justifiable' trade-off is often predetermined by legal and bureaucratic incentives, not patient-centered deliberation.