Telehealth vs State Rules: Whose Rights Win in Abortion Access?
Analysis reveals 8 key thematic connections.
Key Findings
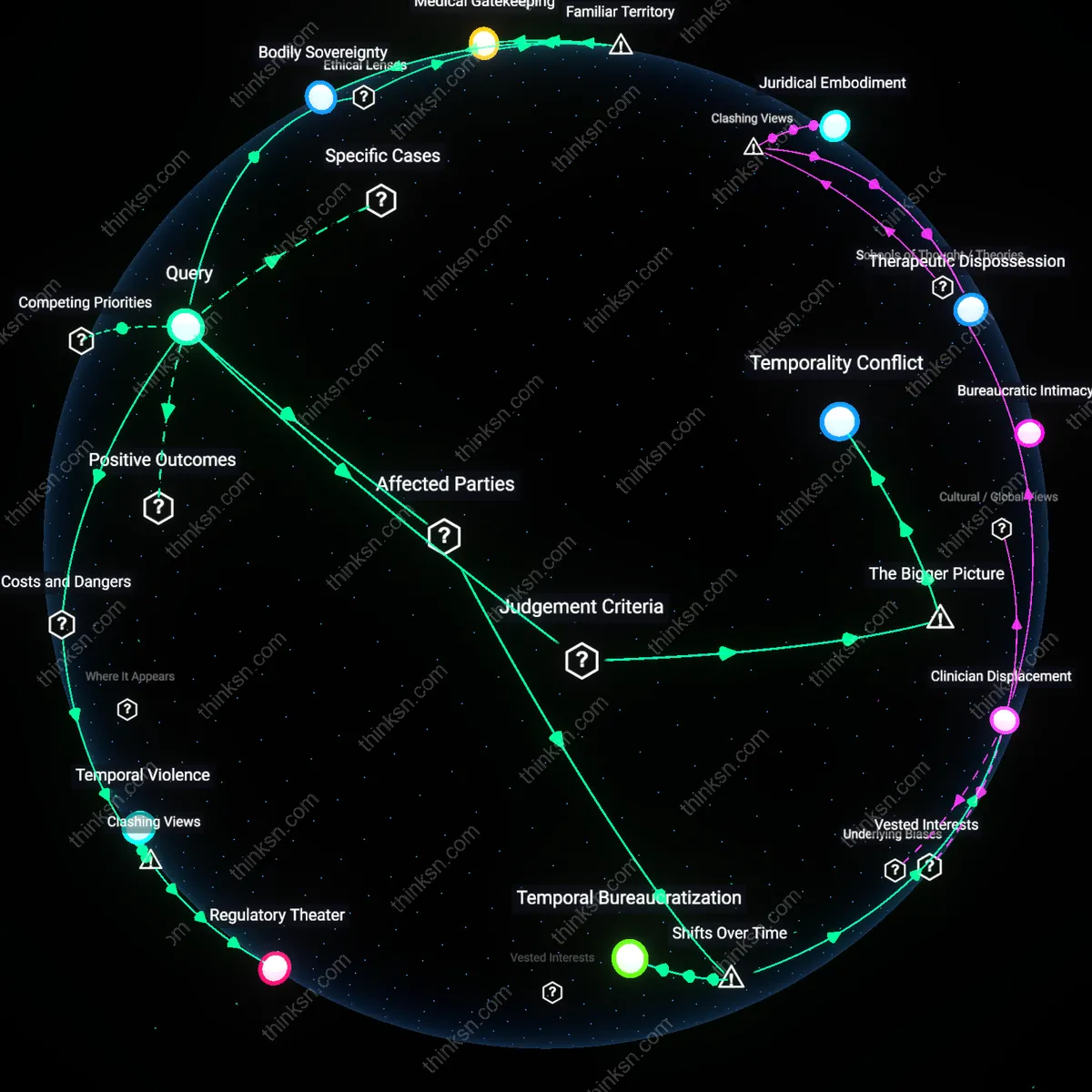
Clinician Displacement
The expansion of telehealth for medication abortion after 2020 decentralized clinical gatekeeping from in-person providers to digital platforms, shifting authority from local obstetricians to centralized telemedicine startups and regulatory compliance officers who now arbitrate access under state-specific waiting period mandates. This reconfiguration emerged as FDA restrictions on mifepristone were temporarily lifted during the pandemic, revealing how emergency public health logic eroded longstanding geographic and procedural controls—yet exposed how state-level waiting periods were repurposed not to protect patients, but to reassert jurisdiction over newly mobile clinical decisions, thereby diminishing the role of frontline clinicians in favor of bureaucratic compliance mechanisms.
Temporal Bureaucratization
State-mandated waiting periods evolved from being framed as patient protection measures in the 1990s into temporally enforceable procedural barriers by the 2010s, crystallizing through laws that required in-person visits 24–72 hours before abortion administration, thus transforming time itself into a regulatory instrument. The emergence of telehealth after 2020 disrupted this model by compressing geographic and temporal distance, forcing states to either suspend waiting requirements temporarily or shift enforcement onto asynchronous verification systems—such as mandatory video confirmations or timestamped digital consent forms—revealing how the medical encounter has been replaced by a compliance ritual whose primary function is to produce audit-ready temporal evidence rather than clinical benefit.
Regulatory Friction
Mandated waiting periods create systemic delays that undermine the time-sensitive efficacy of medication abortion, especially when telehealth enables immediate consultation—this contradiction reveals a structural misalignment between clinical urgency and bureaucratic oversight. State legislatures impose waiting periods based on paternalistic assumptions about decisional capacity, while telehealth platforms governed by federal medical standards prioritize rapid triage and access, generating jurisdictional friction. This tension is not merely procedural but reflects deeper conflicts between state-level moral governance and medical professionalism operating across state lines, an underappreciated consequence of federalism in health policy. The non-obvious insight is that waiting periods function as temporal gatekeeping, not just informational requirements, directly disrupting the operational logic of telemedicine.
Temporality Conflict
The mandated waiting period assumes a temporal model of decision-making that requires physical presence and deliberative pause, whereas telehealth operates on an immediacy-driven temporal logic that prioritizes timely pharmacological intervention within narrow clinical windows. Clinicians using telehealth must reconcile real-time patient needs with arbitrary legal deadlines, creating a procedural dissonance between medical timing and legal timing. This conflict is structurally produced by the decoupling of clinical authority from jurisdictional enforcement, where federal telecommunications policy enables rapid care delivery that state laws cannot consistently delay. The overlooked insight is that time itself becomes a contested domain through which autonomy and regulation are operationalized differently.
Regulatory Theater
Mandated waiting periods function not to enhance patient safety but to create the appearance of oversight, thereby legitimizing political control over reproductive decisions under the guise of medical caution. This ritualized delay operates through state legislatures imposing medically unnecessary hurdles—such as 24- or 72-hour waits—despite telehealth platforms enabling immediate risk assessment and drug delivery; the mechanism is performative regulation, where compliance with arbitrary timelines substitutes for actual clinical evaluation. The non-obvious consequence is that the system prioritizes documentation of delay over continuity of care, transforming administrative adherence into a proxy for safety while exacerbating access deserts—particularly in rural and low-income regions—where time off work, travel, and childcare compound the burden. This reveals how the state enacts governance through visible proceduralism rather than measurable health outcomes.
Temporal Violence
Waiting periods impose psychological and physiological harm by deliberately disrupting the time-sensitive context of abortion care, leveraging delay as a tool of coercion that aligns with carceral logics rather than medical ethics. The mechanism functions through state-enforced temporal disjunctions—forcing patients to interrupt treatment arcs established via telehealth consults—thereby increasing anxiety, logistical collapse, and gestational progression that may push individuals beyond legal limits. The non-obvious effect is that time itself becomes a weaponized regulatory instrument, where the damage is not solely in denied access but in the systematic production of helplessness and eroded agency; this reflects a deeper conflict in which clinical autonomy is subordinated to bureaucratic timelines that mirror punitive systems rather than healing ones. The result is a medical environment where the act of waiting constitutes an institutionalized injury.
Bodily Sovereignty
Restrictions on telehealth abortion undermine the principle that individuals have ultimate authority over medical decisions affecting their own bodies, particularly when waiting periods—rooted in paternalistic consent doctrines—override telehealth’s capacity to expand access in rural or underserved regions. This dynamic reflects a conflict between utilitarian public health regulation and deontological respect for personal autonomy, where state-mandated delays treat patients as subjects of oversight rather than rights-bearing agents. The non-obvious insight within familiar concerns about 'choice' and 'government intrusion' is that waiting periods function not just as informational pauses, but as regulatory acts that materially reconfigure who controls the timeline and location of care.
Medical Gatekeeping
Mandated waiting periods institutionalize a clinical checkpoint model where physicians and state agents serve as moral intermediaries between patient desire and treatment access, even when telehealth could bypass traditional care hierarchies. This preserves a Hippocratic tradition where medical expertise legitimizes access, countering telehealth’s emergent logic of decentralized, self-directed care. What gets overlooked in common debates about 'trust' and 'safety' is that waiting periods are less about medical necessity than about preserving professional authority against the democratizing potential of virtual platforms.