Balancing Social Isolation and Lung Health in Asthma Management?
Analysis reveals 9 key thematic connections.
Key Findings
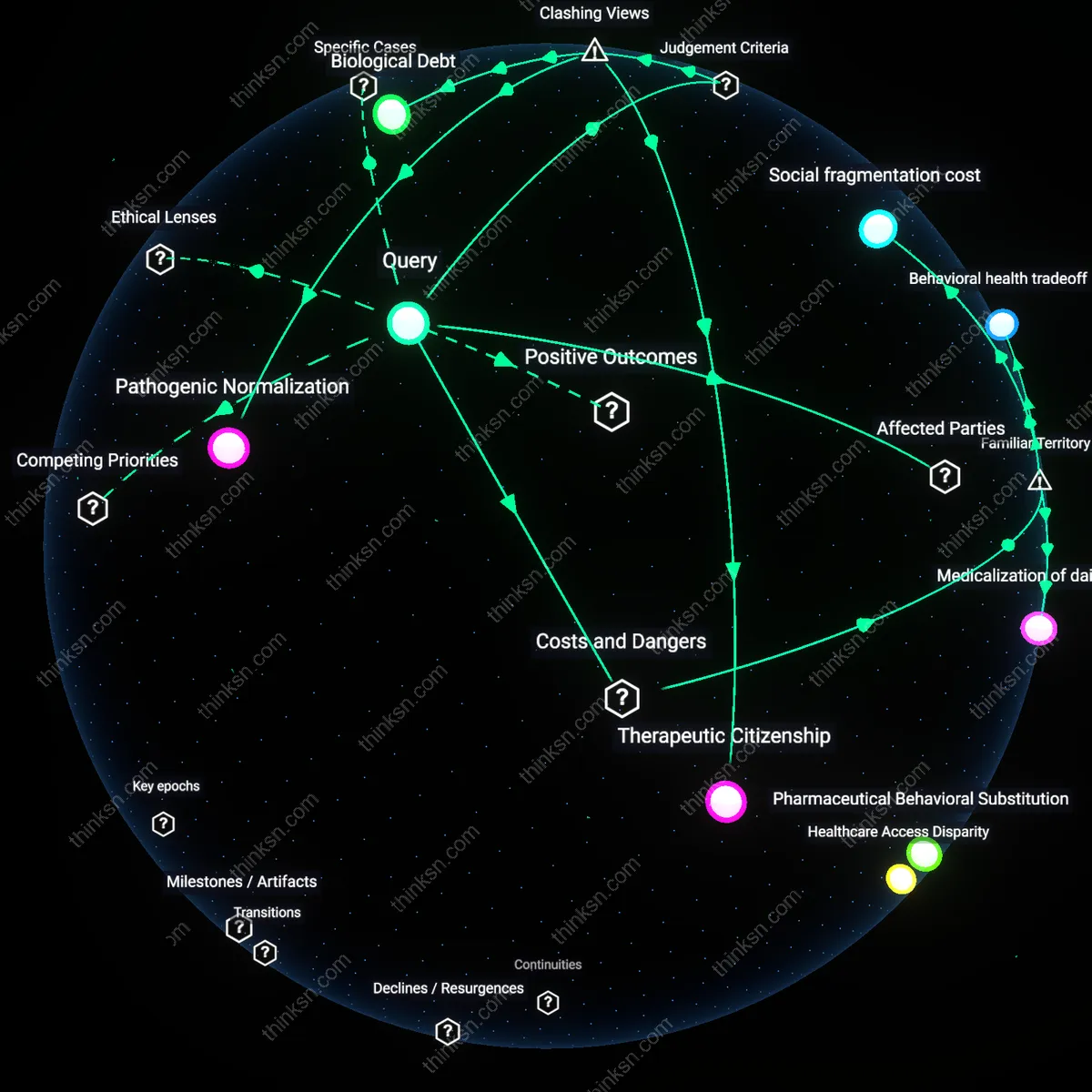
Healthcare Access Disparity
Medical guidance on strict asthma trigger avoidance disproportionately prescribes social withdrawal to low-income urban populations, whose housing and neighborhood conditions concentrate pollutants and limit control over environmental exposures. Clinicians in overwhelmed public health systems often default to individual behavioral adjustments—like staying indoors—because structural interventions such as housing remediation or urban air quality regulation are outside their reach, placing the burden of systemic failure on patients’ isolation. This dynamic reinforces a hidden clinical triage where marginalized patients absorb social costs to achieve physiologic stability, revealing how healthcare rationing operates through environmental constraint rather than explicit resource denial.
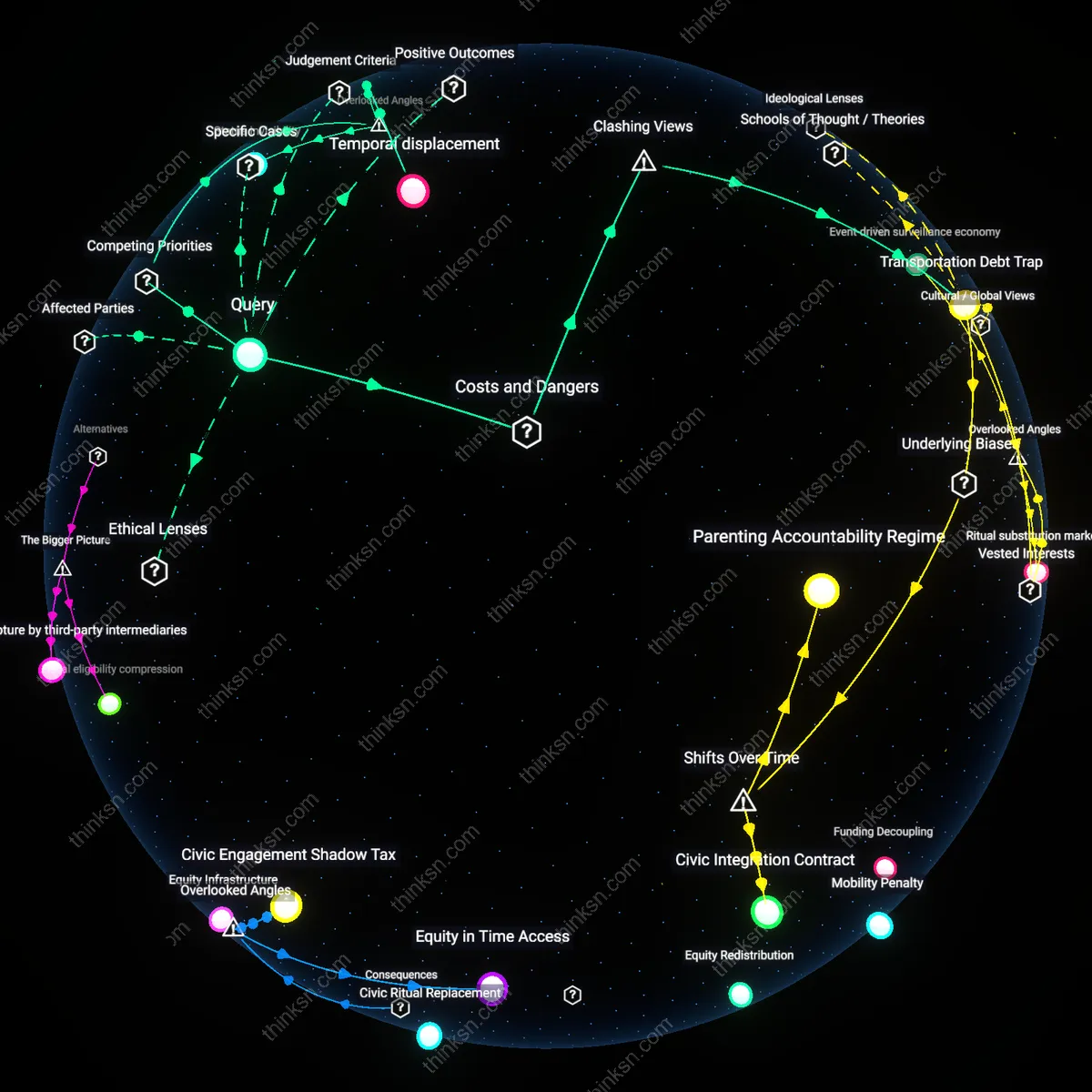
Parental Risk Attribution Shift
Parents of asthmatic children internalize strict avoidance protocols as moral imperatives, escalating social disengagement not due to medical instruction alone but in response to school administrators’ liability aversion and the absence of enforceable accommodations under federal disability law. The mechanism emerges when institutions offload risk management onto families by failing to implement clean-air policies or train staff in asthma response, transforming parental caution into enforced isolation to prevent public episodes that could trigger reputational or legal consequences. This shifts accountability from collective institutional preparedness to individual family discipline, making social withdrawal a covert compliance strategy within fragmented educational and healthcare systems.
Pharmaceutical Behavioral Substitution
Aggressive promotion of long-acting bronchodilators and biologics by pharmaceutical firms recasts strict trigger avoidance as a temporary phase rather than a sustained lifestyle, subtly devaluing social resilience in favor of biochemical control. By positioning medications as complete risk mitigants, drug marketing alters patient and clinician perception of environmental management as burdensome and obsolete, thereby weakening advocacy for urban planning reforms or workplace protections that would reduce exposure collectively. This creates a feedback loop where pharmacologic solutions undermine political will for environmental justice, turning isolated behavior change into a biologically managed substitute for social integration.
Therapeutic Citizenship
One should prioritize long-term lung health over immediate social integration because medical adherence constitutes a civic duty that reconfigures individual autonomy as collective resilience in public health systems. This reframing treats disciplined self-management not as social withdrawal but as an act of therapeutic citizenship—where patients become de facto public health agents reducing strain on emergency care and aerosolized transmission risks in dense urban clinics, a mechanism especially consequential in high-prevalence areas like inner-city asthma belts. The non-obviousness lies in rejecting the assumption that isolation inherently undermines well-being, instead positioning strict avoidance as a socially generative practice that redistributes care-labor from overwhelmed institutions to informed individuals.
Pathogenic Normalization
One should reject the trade-off entirely because framing asthma trigger avoidance as socially isolating reproduces pathogenic normalization—where chronic exposure to preventable pollutants is treated as socially inevitable, thereby legitimizing environmental injustices in low-income neighborhoods near industrial zones. This lens reveals that 'isolation' is not caused by avoidance itself but by blaming individuals for systemic failures, such as lax air quality enforcement in cities like Houston or Detroit, where refineries and highways produce disproportionate particulate exposure. The dissonance emerges when the moral weight shifts from personal sacrifice to collective accountability, exposing how biomedical decisions are falsely detached from spatialized political economy.
Biological Debt
One should discount future lung health benefits because the accumulation of biological debt—in which short-term social impoverishment erodes neurodevelopmental and immune pathways critical in adolescence—outweighs delayed pulmonary gains, especially among children in segregated school districts. Peer interaction isn't ancillary but metabolically formative; cortisol dysregulation from loneliness can amplify bronchial hyperreactivity more than occasional allergen exposure, undermining the very physiological goals of trigger avoidance. This reframing disrupts the intuitive primacy of organ-specific outcomes by showing how relational health operates as foundational infrastructure for biological integrity.
Social fragmentation cost
Strict asthma trigger avoidance forces individuals to withdraw from communal spaces like schools, workplaces, and social gatherings where allergens or pollutants are present, thereby eroding their social support networks. This isolation is not incidental but structurally enforced by institutional environments that prioritize operational convenience over accommodation, such as schools that use scented cleaning products or offices with poor ventilation. The damage lies not in the act of avoidance itself but in how it codifies exclusion through normative environmental design, making respiratory safety incompatible with participation—an underappreciated contradiction in public health policy that disproportionately impacts low-income asthmatics who lack private, controlled environments.
Behavioral health tradeoff
Avoiding asthma triggers to the point of social withdrawal amplifies risks for anxiety, depression, and hypervigilance, particularly in children who internalize their condition as a marker of fragility. The mechanism operates through chronic stress response systems activated by both physiological fear of attack and social stigma tied to being 'the sick one' who must leave the room or skip activities. What's rarely acknowledged in public discussions—despite widespread recognition of mental health struggles—is that trigger avoidance regimes often mirror phobic conditioning, where safety behaviors inadvertently reinforce avoidance, turning environmental caution into psychological constraint.
Medicalization of daily life
Rigid adherence to asthma trigger avoidance transforms routine human interactions—such as hugging someone who wears perfume or attending a family barbecue with smoke—into potential health threats, thereby medicalizing ordinary social behaviors. This shift is institutionalized through clinical guidelines that emphasize individual control over environmental exposure without addressing collective responsibility for shared air quality. The underappreciated consequence is that patients become de facto regulators of public behavior, absorbing the labor and interpersonal friction of enforcement, which re-frames care as personal burden rather than civic obligation.