How Price Opacity in Medical Imaging Harms Uninsured Patients?
Analysis reveals 8 key thematic connections.
Key Findings
Revenue Cycle Obfuscation
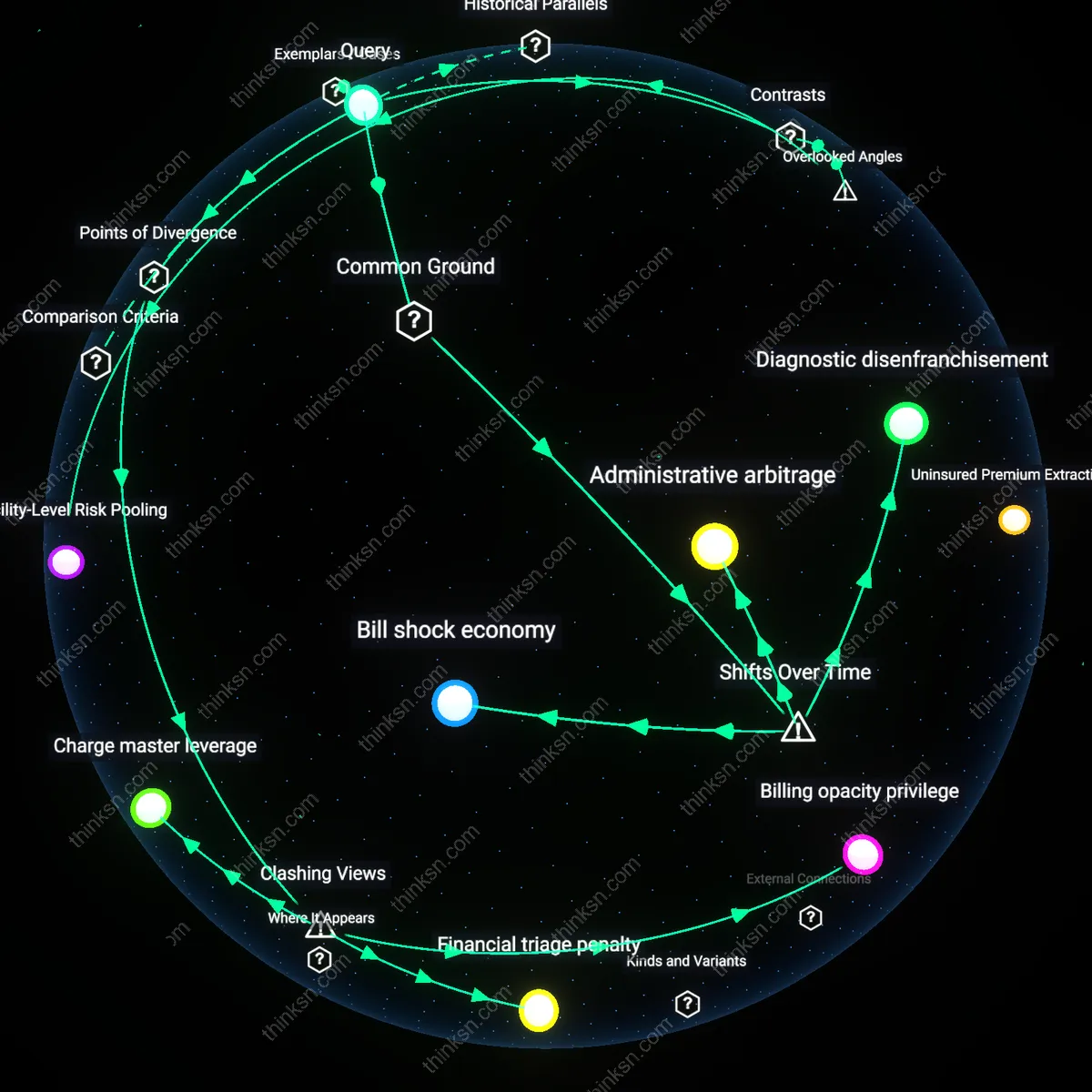
Uninsured patients bear disproportionate imaging costs because hospitals exploit opaque pricing to maximize revenue through aggressive post-service billing tactics, a mechanism insulated from market discipline by the absence of transparent fee schedules. Insurers negotiate fixed rates that cap provider returns, whereas uninsured patients—lacking negotiated rates or price signaling—trigger unfilled gaps in the hospital’s revenue cycle, prompting charge master inflation and collections escalation. This dynamic reveals that price opacity functions not as a neutral information gap but as an active instrument for balancing institutional financial risk at the expense of a vulnerable patient subgroup—a role rarely acknowledged in policy debates focused on insurer bargaining power.
Facility-Level Risk Pooling
Imaging facilities shift fixed operational costs onto uninsured patients because opaque pricing enables implicit cross-subsidization in reverse—where the uninsured effectively subsidize the predictability of insured payer streams rather than the other way around. Since insurers guarantee volume and timely payment, facilities treat insured patients as low-risk inputs and optimize workflows accordingly, while using opaque, inflated uninsured charges to hedge against underpayment risks and equipment overhead. This inverted subsidy structure—unseen in most equity discussions—means price opacity sustains system efficiency for insured populations by concentrating fragility on those outside formal risk pools.
Bill shock economy
Absence of price transparency in medical imaging entrenches a bill shock economy that emerged prominently after the 1990s managed care backlash, when deregulatory trends allowed providers to set prices without public benchmarks while insurers negotiated covert rate schedules. Hospitals and radiology groups began operating with highly variable, cost-plus pricing models that were shielded from scrutiny, and as employer-based insurance eroded in the 2000s, underinsured and uninsured patients—once hidden behind pooled risk structures—were exposed directly to these inflated charges. The mechanism is not mere lack of information but the historical collapse of price consensus post-HMO era, which made list prices arbitrary and decoupled from actual cost, rendering uninsured patients subject to first-point-of-contact price setting with no appeal or negotiation capacity, revealing a system designed for risk deflection, not cost clarity.
Administrative arbitrage
Insured patients are shielded from opaque imaging prices because insurers evolved, during the Medicaid expansion and ACA implementation phases (2010–2016), into arbitrage agents who negotiate rates based on volume and network access, a function that only works through exclusion. This created a dual-tier system where reimbursement schedules are internally transparent to payers but deliberately obscured from patients, especially those without coding literacy or benefit managers. The shift from fee-for-service dominance to managed competition embedded pricing opacity as a structural feature, not a flaw—providers now depend on differential pricing to balance margins, meaning uninsured patients, who cannot be leveraged for volume discounts, become default revenue absorbers, revealing administrative arbitrage as a normalized mechanism of financial extraction.
Diagnostic disenfranchisement
The lack of imaging price transparency entrenches diagnostic disenfranchisement, a condition that intensified after the 1980s commodification of radiology, when technological advances decoupled scan provision from physician judgment and recast imaging as a profit center. Prior to widespread MRI/CT availability, diagnostic access was gatekept clinically; now, it is gatekept financially, and without insurance acting as a proxy negotiator, uninsured patients face delayed or avoided care not due to availability but fiscal unpredictability. This shift from clinical to financial triage—evident in ER billing patterns since the 2000s—reveals that price opacity is not incidental but functionally sustains a rationing mechanism that operates invisibly for insured populations while imposing active harm on the uninsured, producing a class of medically marginalized whose exclusion is justified by administrative silence.
Billing opacity privilege
Uninsured patients are systematically excluded from negotiated rate structures that insurers access, forcing them into full sticker-price liability despite identical imaging procedures; hospitals and radiology groups maintain dual pricing tiers where insured patients benefit from opaque but discounted contractual rates, while uninsured patients face unadjusted charges that reflect list prices inflated to offset insurer discounts, a mechanism sustained by the absence of federal price transparency mandates for self-pay patients. This dynamic reveals that price opacity is not a market failure but a strategic feature preserving institutional revenue streams, privileging those with third-party payment capacity—a condition invisible when assuming all patients face the same pricing system.
Financial triage penalty
Uninsured patients experience delayed or fragmented imaging access due to upfront cost uncertainty, leading to downstream clinical worsening that increases total care intensity when treatment finally occurs, whereas insured patients navigate scheduling with predictable copays anchored to transparent cost-sharing tiers; this creates a divergence where the uninsured absorb not just higher per-unit prices but also compounded health and financial risks from deferral, driven by the absence of real-time price signals that might allow cost-avoidance or facility comparison. The non-obvious consequence is that price opacity functions as a de facto rationing mechanism that penalizes financial vulnerability, contradicting the assumption that imaging access barriers primarily stem from insurance status alone.
Charge master leverage
Hospitals leverage the lack of imaging price transparency to maximize disproportionate share hospital (DSH) subsidies and bad debt write-offs by inflating charges for uninsured patients, whose billed amounts—though rarely paid—serve as the baseline for calculating revenue loss and federal reimbursement adjustments; in contrast, insured patients' lower negotiated rates reduce reported losses and limit subsidy eligibility, meaning that the uninsured are instrumentally overcharged not for revenue capture but to sustain institutional financing mechanisms dependent on demonstrating high uncompensated care burdens. This inverts the expectation that opaque pricing harms providers' bottom lines, revealing instead that phantom prices perform a critical fiscal role in safety-net hospital economics.