Negotiating Cash-Pay: Empowerment or Insurer Control?
Analysis reveals 7 key thematic connections.
Key Findings
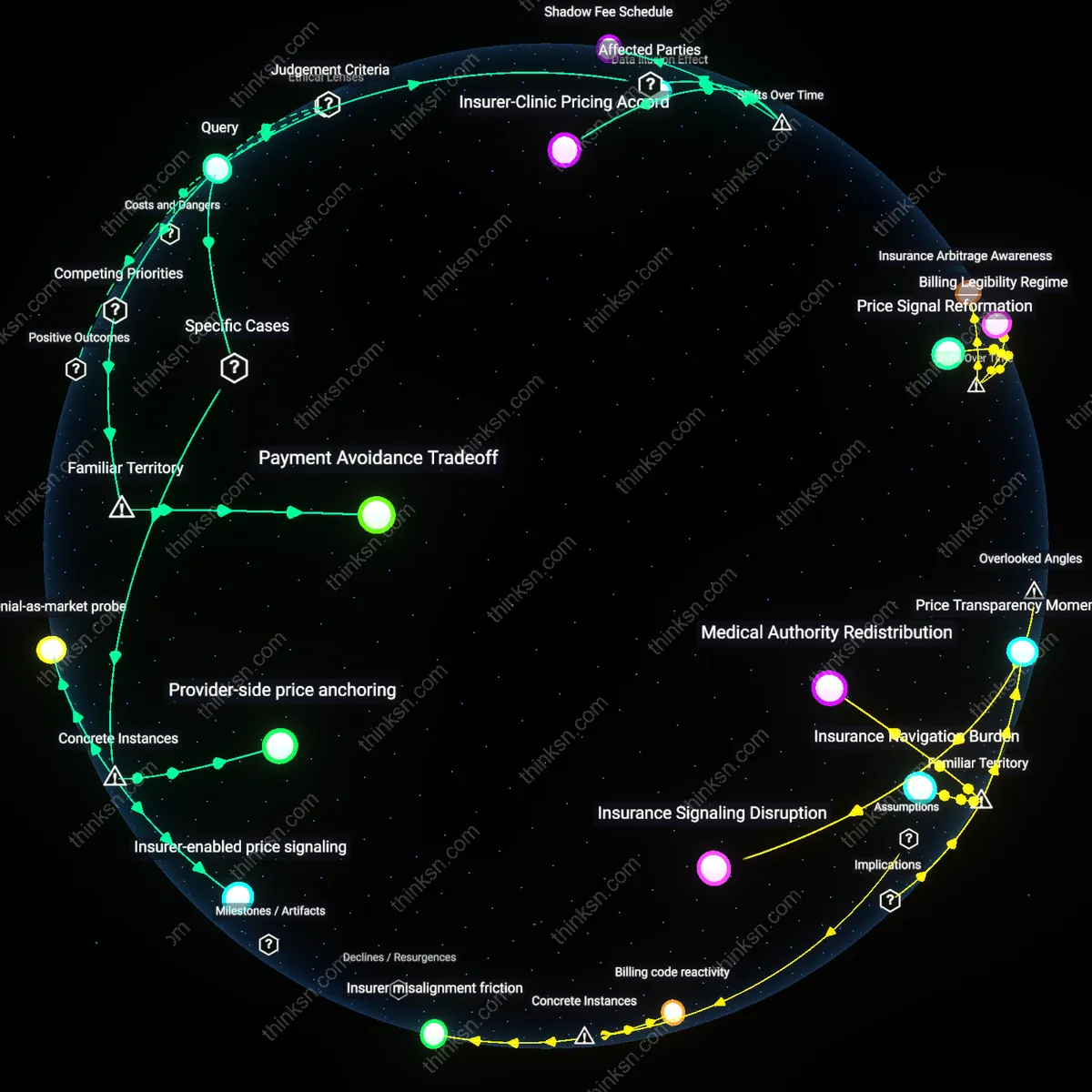
Insurer-Clinic Pricing Accord
Patients should negotiate cash-pay options after insurance denial because such negotiations reveal hidden price elasticity that clinicians leverage to bypass insurer fee schedules, a practice that intensified after the 2008–2010 shift from volume-based to value-based reimbursement, when clinics—facing higher revenue risk from bundled payments—began reserving self-pay slots to stabilize income. This dynamic embeds an informal 'Insurer-Clinic Pricing Accord' where out-of-network cash rates are tacitly calibrated to avoid undermining negotiated rates, exposing a post-reform equilibrium where pricing transparency is managed through exclusion, not disclosure. The non-obvious insight is that cash negotiations do not disrupt insurer control but instead reinforce it by creating off-balance-sheet pricing that sustains systemic opacity.
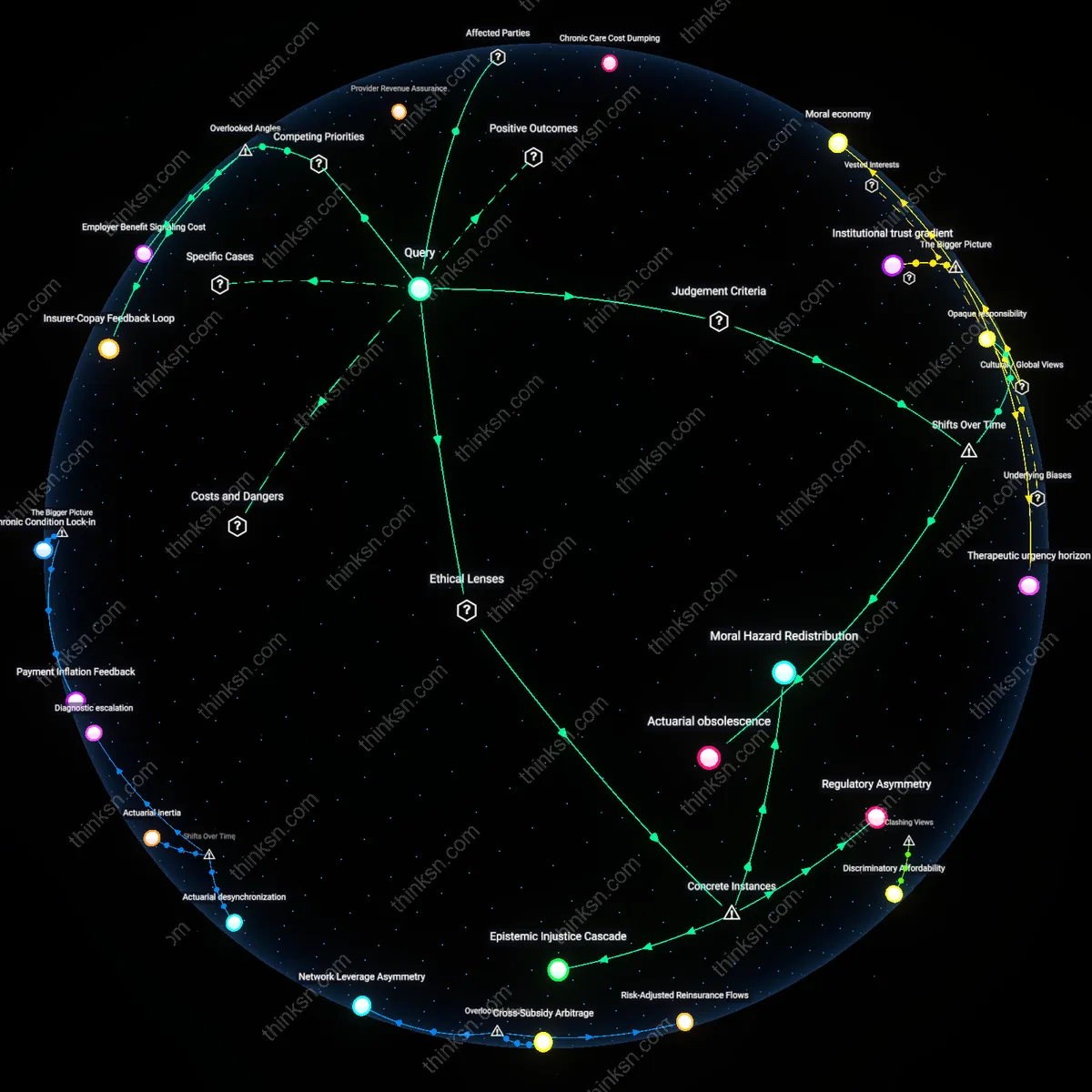
Patient as Revenue Arbitrageur
Patients began functioning as de facto revenue arbitrageurs after the 2014 expansion of high-deductible health plans (HDHPs), when cost transparency tools enabled individuals to compare insurer-negotiated rates against clinic list prices and selectively opt for cash payments when cheaper. This shift transformed patients from passive beneficiaries into active agents who, through fragmented payment choices, pressure clinics to publish or justify charges—yet simultaneously erode collective pricing data by generating non-insured transactions that evade claims reporting. The historically underappreciated effect is that this patient-driven arbitrage does not weaken insurers’ pricing authority but instead displaces transparency burdens onto individuals, preserving insurer dominance through distributed confusion.
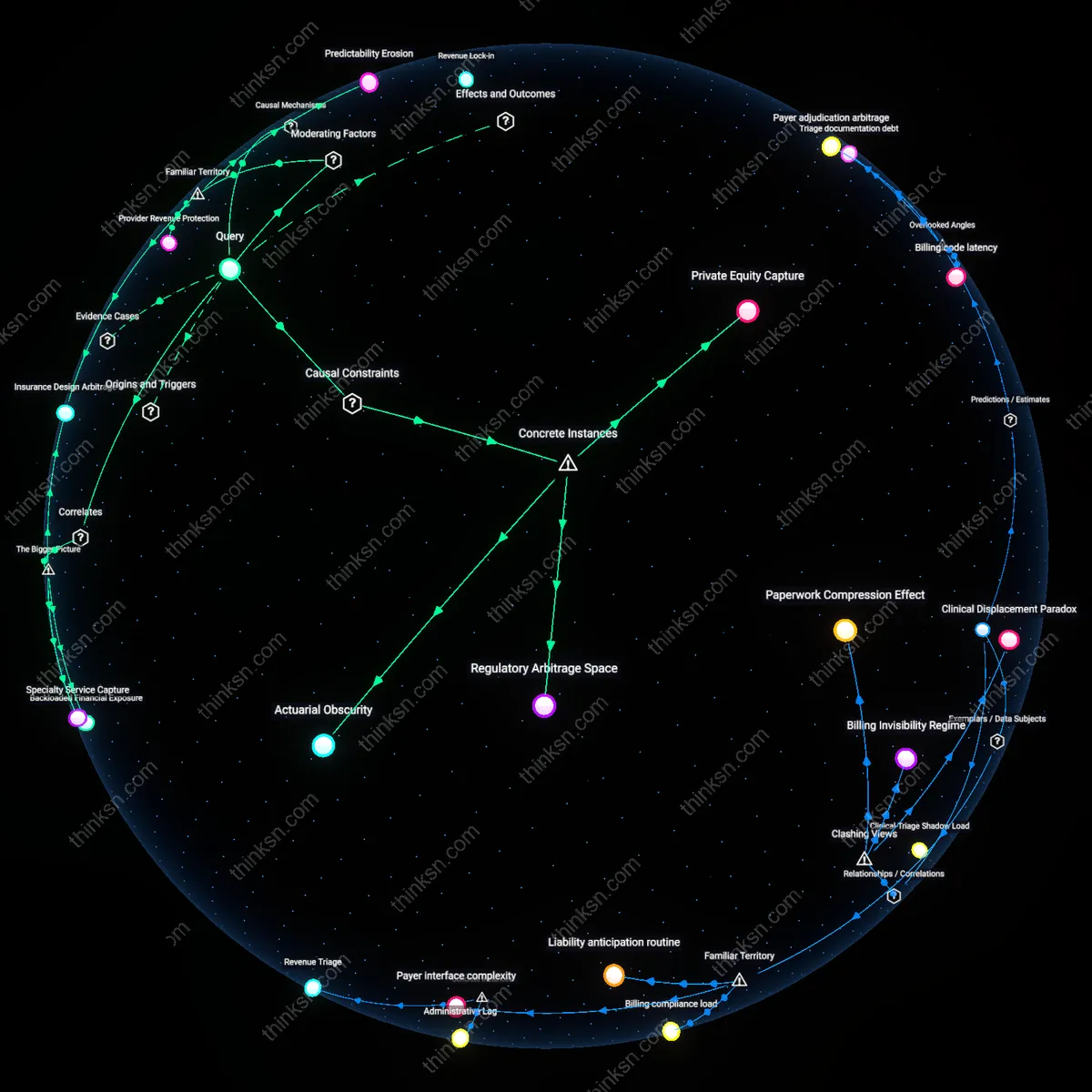
Shadow Fee Schedule
Cash-pay negotiations after insurance denial have hardened into a 'Shadow Fee Schedule' since the mid-2010s, as large physician groups and hospital systems began standardizing self-pay discounts (e.g., 30–50% off billed charges) in response to rising numbers of underinsured patients, a trend accelerated by the Affordable Care Act's coverage gaps. These standardized discounts emerged not from market competition but from institutional learning, where providers, having experienced revenue leakage from inconsistent cash pricing, codified internal rules to mimic insurer-style contracts—thereby replicating managed pricing logics outside insurance. The critical temporal shift reveals that this practice does not challenge insurer control but instead mimics it, producing a parallel structure that insurers can later reference to justify lower rates, thereby strengthening their downstream leverage.
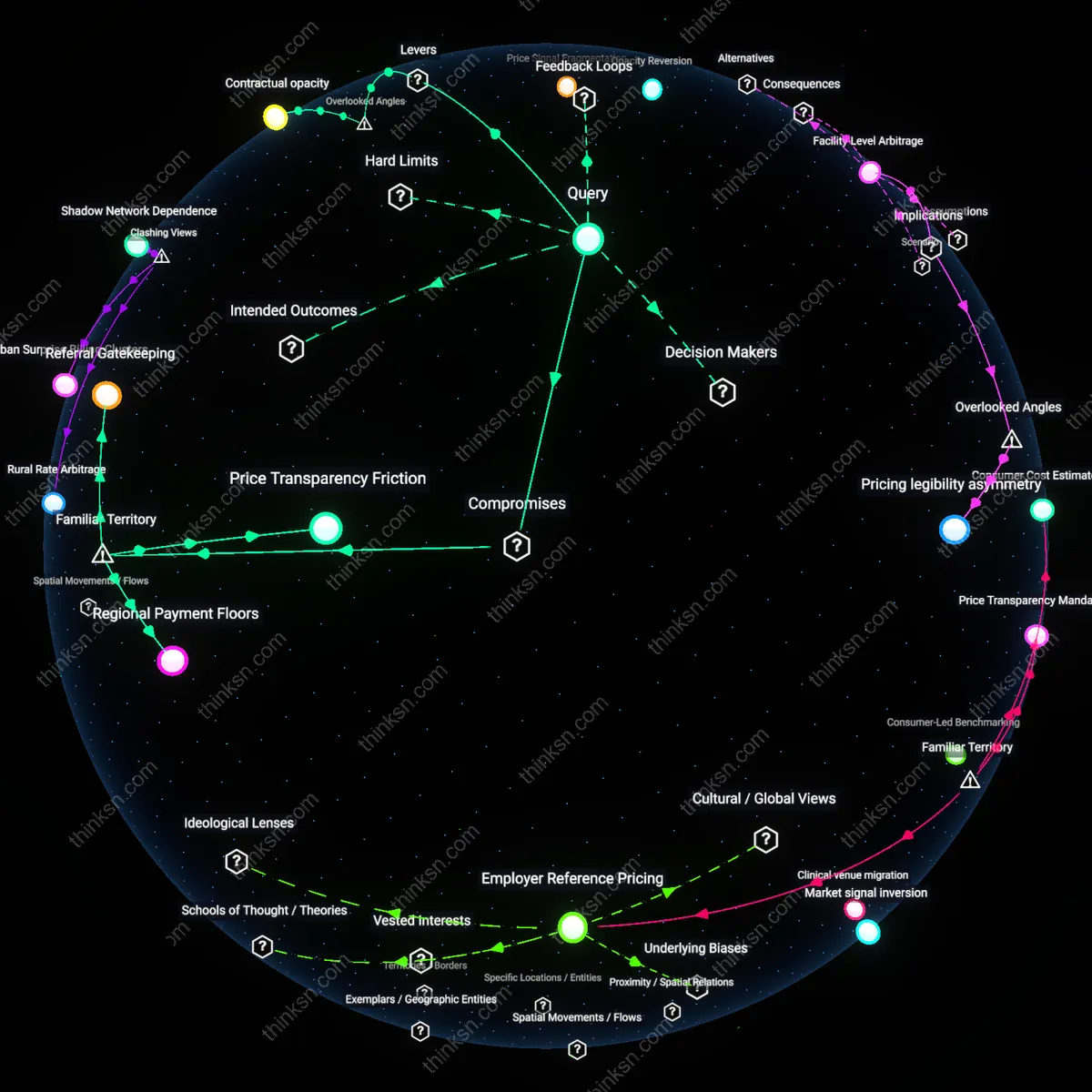
Payment Avoidance Tradeoff
Patients should negotiate cash-pay options after insurance denial because it shifts financial responsibility from insurers to individuals, leveraging providers’ willingness to bypass billing systems for immediate payment. This dynamic pits patient affordability against systemic cost containment, as providers gain short-term liquidity while insurers lose pricing influence and claims data. The non-obvious consequence under familiar assumptions—where cash negotiation is seen as personal financial relief—is that it erodes insurers’ ability to standardize and benchmark prices across networks, effectively creating a shadow pricing tier that undercuts negotiated rates.
Provider-side price anchoring
Montefiore Medical Center in New York routinely offers self-pay patients discounted cash rates after insurance denials, establishing a de facto reference price that undercuts billed charges and reveals the insurer's list price as artificially inflated—this practice entrenches hospitals as active price setters in the shadow of insurance opacity, demonstrating how cash negotiations inadvertently validate the insurer's pricing framework rather than challenge it. The mechanism works through differential pricing systems where cash rates are administratively set below chargemaster rates but remain invisible to insured patients, making Montefiore’s cash-pay option a tactical disclosure of hidden pricing tiers. This is non-obvious because it shows providers, not insurers, are the source of pricing opacity, yet their cash discounts reinforce insurers’ negotiated rates as the 'normal' benchmark—a dynamic rarely visible outside safety-net systems with high uncompensated care burdens.
Insurer-enabled price signaling
When UnitedHealthcare denied coverage for a spinal fusion procedure for a patient at Texas Health Resources, the hospital’s financial counseling team offered a $38,000 cash package—$22,000 less than the insured charge—demonstrating how denial-triggered negotiation creates a covert feedback loop where providers signal true cost to insurers through patient-facing prices. This operates through revenue cycle management systems that use cash-pay offers as loss-minimizing tools, yet the resulting data informs future payer contract bids, effectively letting self-pay pricing shape insurer reimbursement benchmarks. The underappreciated insight is that insurer denial policies don’t suppress cost transparency but instead trigger a backchannel data stream where out-of-pocket offers become informal market signals—making the denial event a pivot point for tacit pricing coordination, visible only where payer density is high and price variation extreme.
Denial-as-market probe
At Sutter Health in California, repeated insurance denials for outpatient imaging led patients to accept cash prices averaging 40% below contracted rates, turning denial events into real-time market tests that revealed demand elasticity and informed Sutter’s future payer negotiations—showing that patient-facing cash offers after denials function not as exceptions but as empirical pricing experiments. This mechanism runs through enterprise pricing offices that retrospectively analyze cash-pay uptake to refine charge master strategies, effectively using denied claims as low-risk opportunities to calibrate prices without breaching payer contracts. The non-obvious outcome is that insurer control is not weakened by transparency but strengthened by access to this behavioral data, as Sutter’s willingness to discount post-denial feeds back into UnitedHealthcare’s and Blue Shield’s rate negotiation models—a feedback loop evident only in integrated delivery systems with centralized pricing analytics.