Is Financing Med School for Kids a Risky Bet on Shortage Hype?
Analysis reveals 10 key thematic connections.
Key Findings
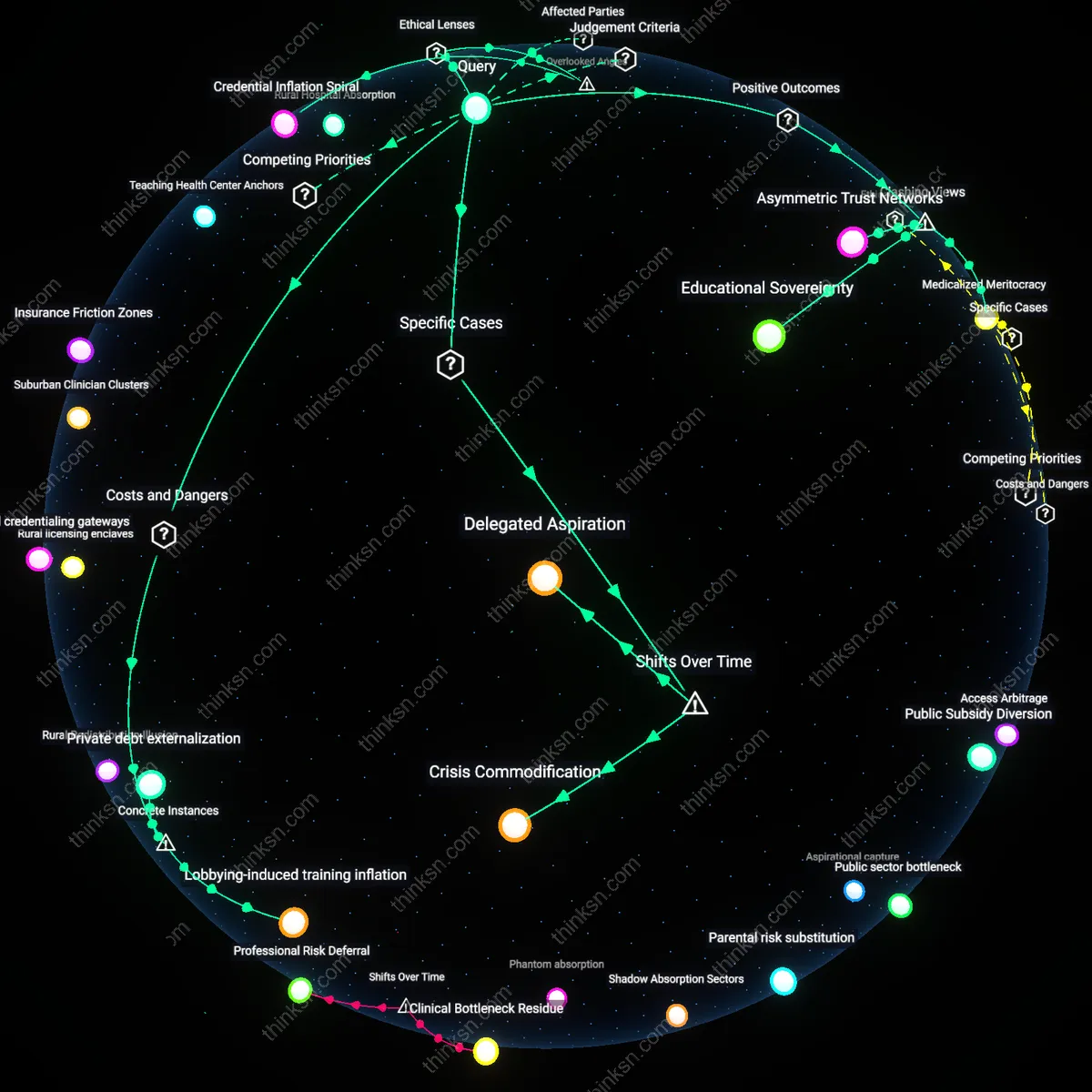
Educational Sovereignty
A parent’s investment in medical education remains justified because it functions as a form of household-level agency that resists centralized health labor planning, regardless of national physician supply claims. Families operating in jurisdictions like the U.S., where medical training is privatized and future practice locations are decentralized, exercise autonomy in human capital development without reliance on state or industry projections; this bypasses the influence of organizations such as the AAMC, whose repeated warnings of shortages correlate with increased medical school enrollment but not with primary care accessibility in rural regions. The non-obvious insight is that individual investment acts as a counterweight to institutionalized forecasting—often shaped by teaching hospital lobbies—thereby preserving familial discretion in upward mobility strategies under conditions of information asymmetry.
Medicalized Meritocracy
Funding medical school can be rational even if physician shortages are inflated, because the credential itself redistributes social status and intergenerational stability more reliably than general economic indicators suggest. In urban centers like New Delhi or São Paulo, where medical degrees confer professional insulation from labor market volatility, parents treat the degree as a positional good—distinct from actual clinical need—enabling access to elite networks and bureaucratic authority within public health systems. This reveals that the decision is less about healthcare delivery gaps and more about navigating rigid class hierarchies, challenging the assumption that such investments respond to public utility rather than structural inequality disguised as merit.
Asymmetric Trust Networks
Parental funding persists despite questionable shortage narratives because trust in localized medical authority—such as that of family physicians or community hospitals—overrides skepticism toward national policy discourse, particularly in regions like rural Appalachia where federal health reports are viewed with suspicion. The mechanism operates through kinship-embedded knowledge systems where personal experience with healthcare access outweighs statistical claims from Washington-based think tanks funded by hospital associations. This dynamic exposes a hidden resilience in decentralized medical legitimacy, where individual decisions to fund education are sustained not by accuracy of supply-demand forecasts but by the social credibility of neighborhood health providers.
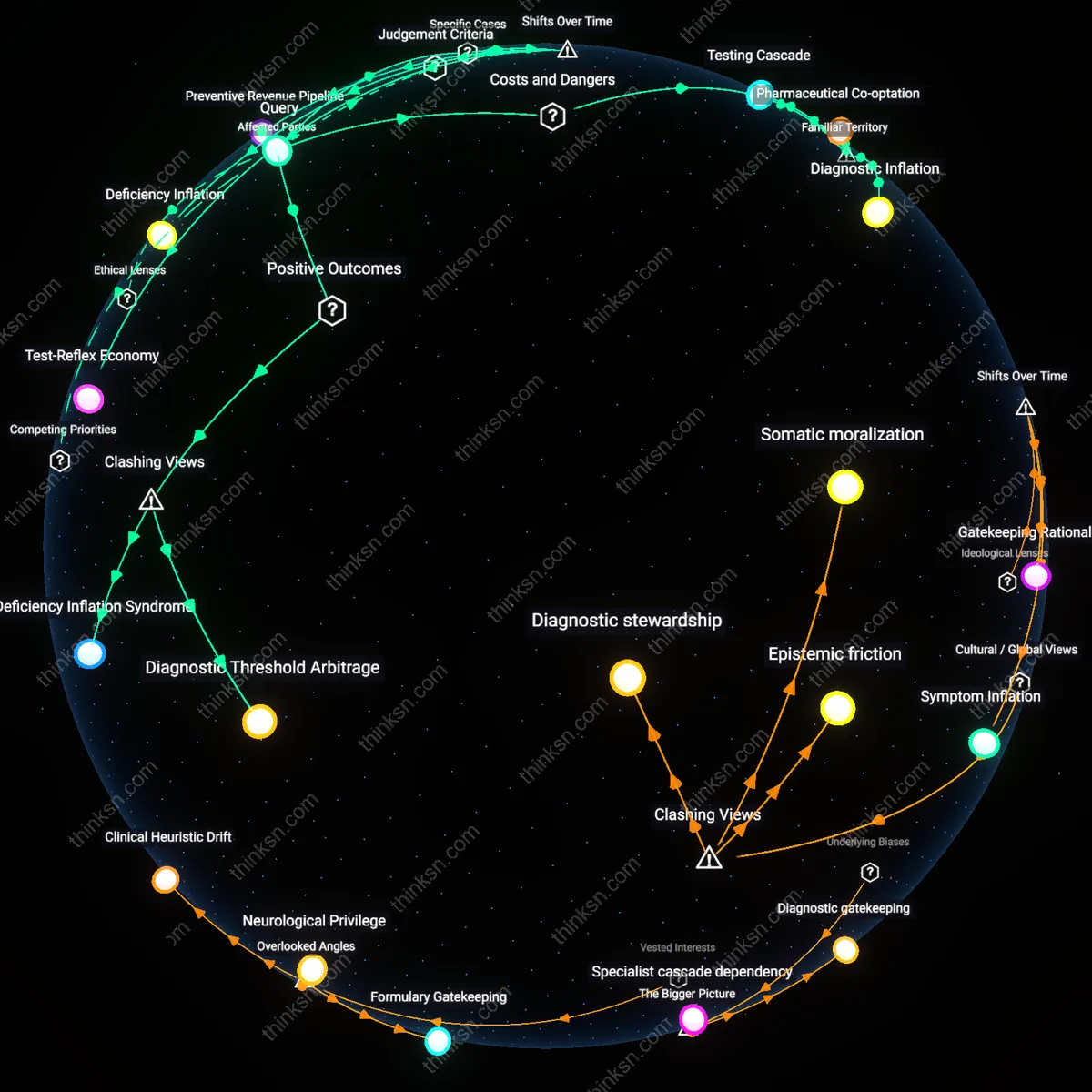
Lobbying-induced training inflation
The American Medical Association’s sustained lobbying to restrict residency slots while amplifying physician shortage narratives directly caused medical schools to raise tuition and expand enrollment without corresponding clinical training capacity, as seen in the 2010–2020 proliferation of for-profit medical schools in the Caribbean that rely on U.S. graduate demand; this mechanism exploits parental investment in response to manufactured scarcity, shifting systemic training costs onto families while entrenching access inequity. The non-obvious consequence is that the shortage narrative does not merely mislead—it actively structures a financial pipeline from households to underregulated institutions by simulating future demand.
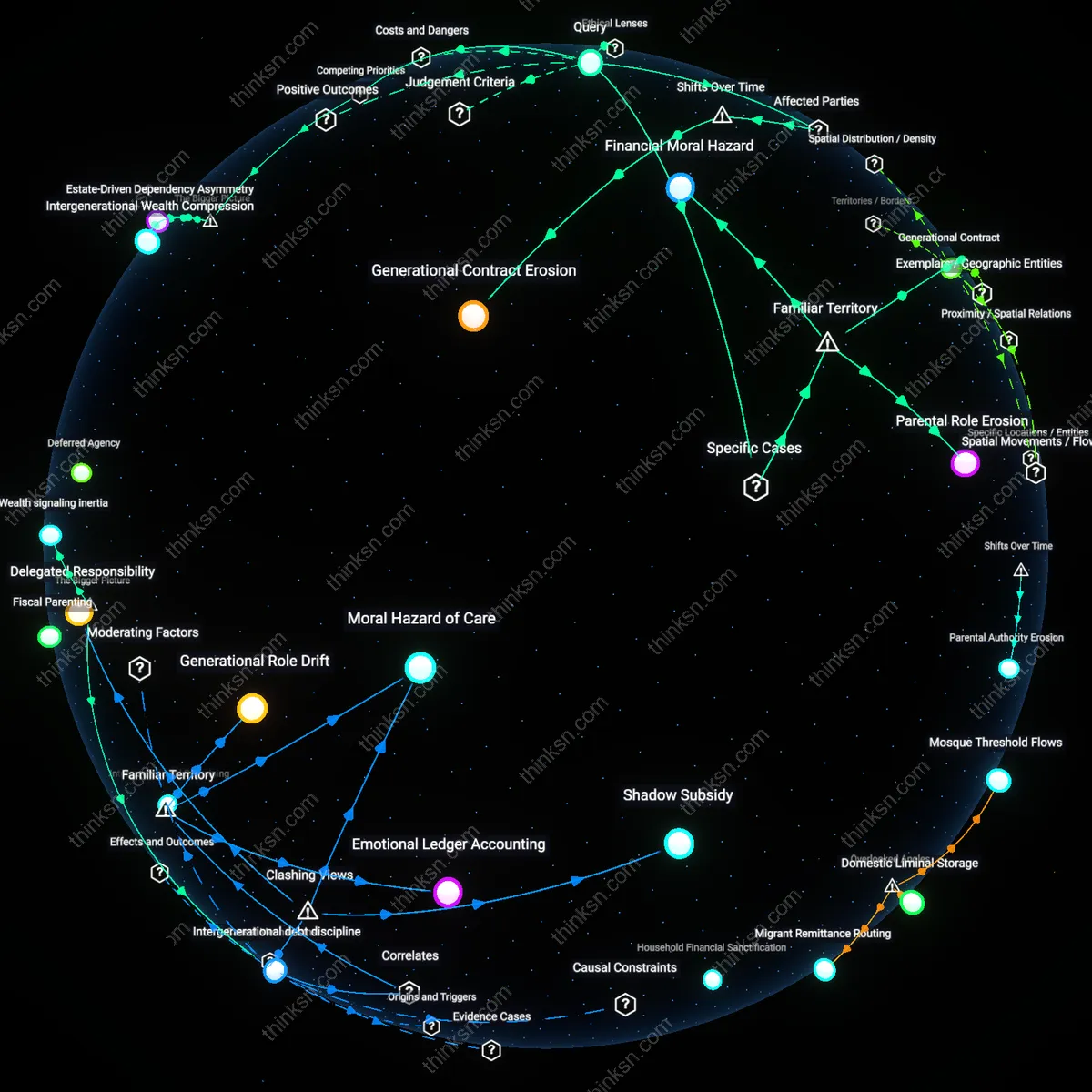
Private debt externalization
In the wake of the 2003 Graduate Medical Education funding freeze in the U.S., teaching hospitals increasingly offloaded resident labor costs onto medical students’ future earning potential, a shift exemplified by the rapid tuition surge at institutions like New York Medical College, where family-funded education became a de facto subsidy for clinical service delivery; this dynamic reveals that parental financing inadvertently absorbs public cost-shifting masked as workforce development, normalizing private assumption of what should be publicly managed infrastructure. The underappreciated risk is that familial investment legitimizes disinvestment in public health systems by redefining physician production as a consumer purchase.
Credential-dependent labor traps
The 2018 expansion of osteopathic (DO) programs, heavily promoted by AOA-aligned institutions citing shortage projections, led to a saturated primary care market where graduates—many from middle-income families who depleted savings to fund education—now face diminished hiring power and contract precarity, as seen in the oversupply crisis in states like Pennsylvania; this illustrates how parental capital fuels entry into a labor tier designed to absorb excess supply while protecting MD-dominated specialty sectors. The overlooked mechanism is that inflated training pipelines create credentialized underemployment, turning family wealth into risk-bearing collateral for professional caste insulation.
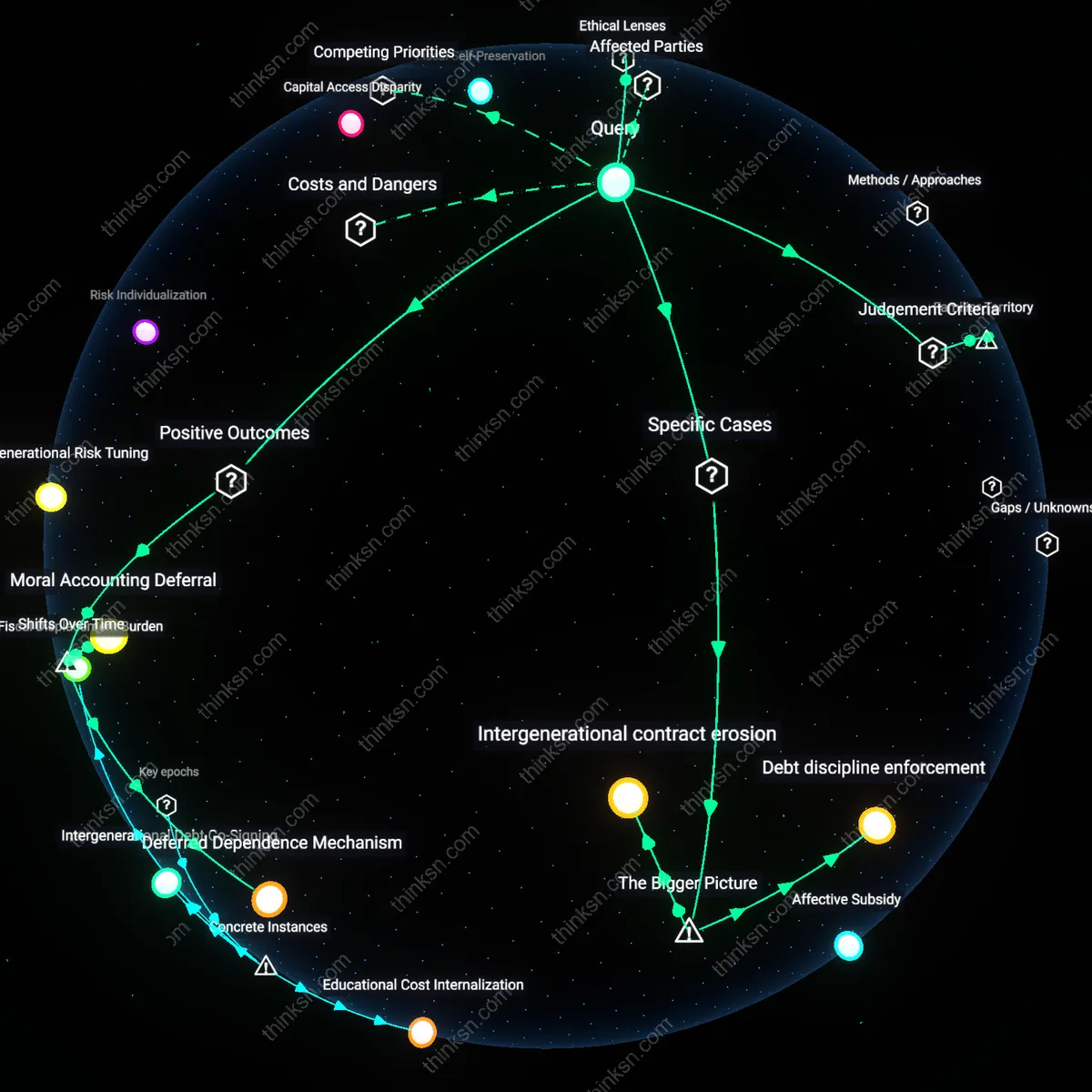
Intergenerational Debt Entanglement
Yes, because the parent’s funding decision embeds the child in a lifelong fiscal and moral dependency structured by medical education’s opaque loan architecture, which systematically binds family wealth to corporate hospital networks via residency placement and debt servitude. This hidden financialization of familial obligation operates beneath ethical debates about physician supply, where the real coercion lies not in labor shortages but in the capture of family assets through credentialing bottlenecks controlled by nonprofit academic medical centers that rely on resident labor. The overlooked mechanism is how private household investment in medical training functions as a backdoor subsidy to publicly funded teaching hospitals, distorting both familial autonomy and labor markets in medicine.
Credential Inflation Spiral
Yes, because the justification for funding shifts when viewed through the lens of status competition rather than labor economics—parents invest not in response to actual shortages but to secure class reproduction in a field where medical degrees function as elite social credentials, irrespective of workforce data. The underappreciated force here is how professional licensing bodies and elite universities collude to sustain the symbolic capital of the MD degree even as telemedicine and nurse practitioner expansion erode its functional monopoly, making parental investment less about future income than about insulating children from downward mobility. This transforms medical education into a positional good, where value is derived from exclusion, not societal need.
Delegated Aspiration
A parent's decision to fund medical education remains justified when viewed through the historical transformation of professional medicine into a familial legacy project, exemplified by the rise of physician dynasties in urban academic medical centers like Massachusetts General Hospital, where multi-generational affiliation since the 1980s has shifted motivation from economic return to identity preservation, making individual career choices subordinate to intergenerational continuity. This shift from vocational investment to kinship reproduction reveals how parental funding insulates against perceived labor market volatility by treating medical training as a rite of belonging rather than a financial gamble, thereby masking the influence of lobbying-driven shortage narratives. The non-obvious insight is that the persistence of such investments is less responsive to workforce data than to the erosion of medicine’s meritocratic ideal over the late 20th century in elite institutions.
Crisis Commodification
Funding medical education is sustained as a private responsibility due to the post-2000s discursive reframing of physician shortages by industry actors like the Association of American Medical Colleges, whose persistent lobbying after the Balanced Budget Act of 1997 constructed scarcity as a permanent feature despite uneven regional saturation, transforming parental investment into a privatized solution to a publicly manufactured crisis. The key shift occurred in the 2010s when workforce models became policy instruments rather than predictive tools, enabling medical schools to expand tuition-based enrollment while attributing gaps to 'planning failure' rather than misaligned incentives. The underappreciated consequence is that parents, observing this constructed perpetual emergency, treat expenditures not as speculative but as morally obligatory—revealing how lobbying-induced narrative persistence has rescheduled individual time horizons around institutional crisis cycles.