How to Weigh Short-Term Recovery vs Long-Term Durability in Heart Valve Surgery?
Analysis reveals 10 key thematic connections.
Key Findings
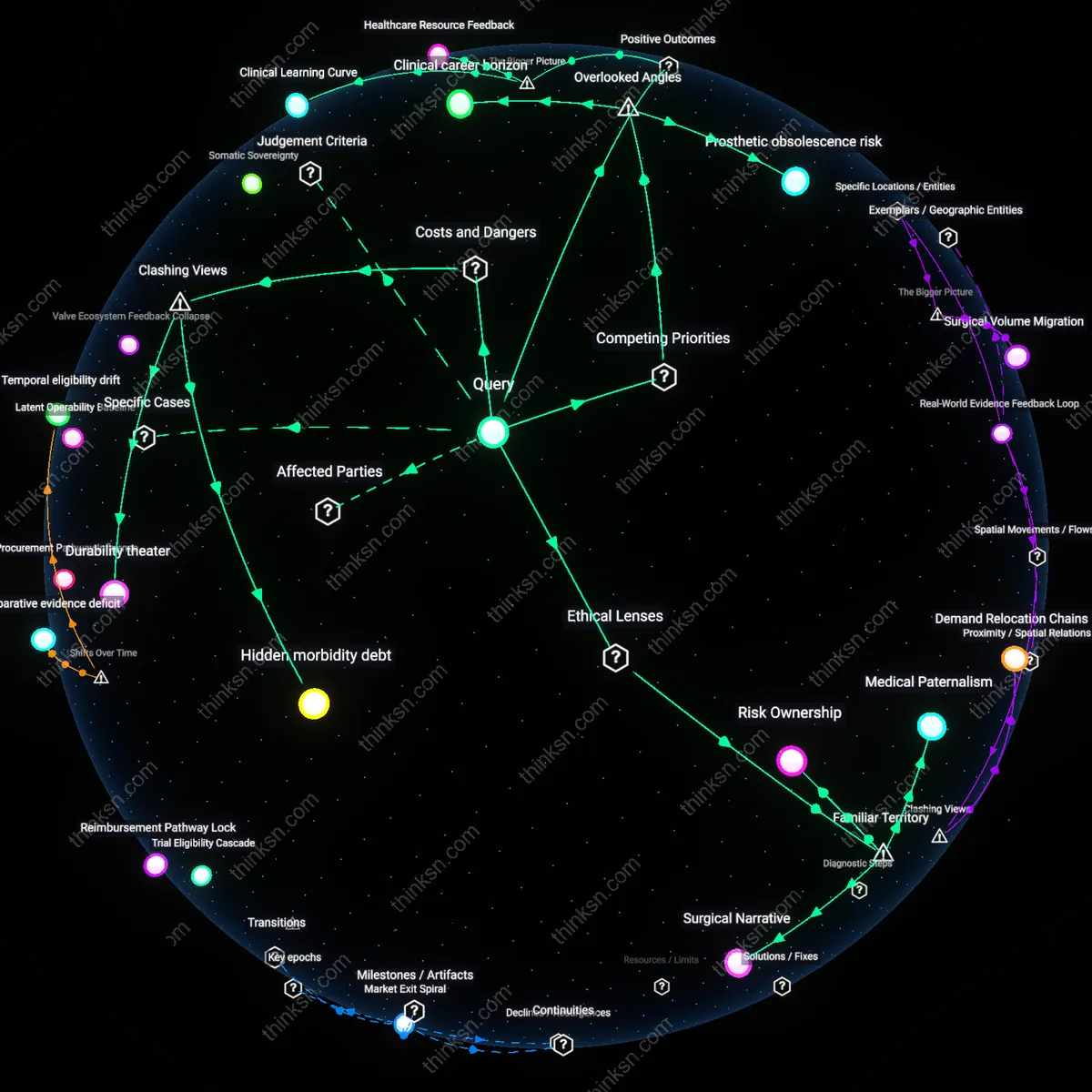
Clinical Learning Curve
Cardiovascular patients gain optimal long-term durability without sacrificing recovery time when treatment decisions align with center-specific surgical expertise because high-volume institutions accumulate procedural mastery that reduces complications in both minimally invasive and open approaches. This occurs through institutional feedback loops where repeated cases refine team coordination, perioperative protocols, and technological adaptation, enabling some centers to collapse the traditional trade-off between speed of recovery and longevity of repair. The underappreciated systemic driver is that outcomes depend not on the procedure type alone, but on the maturity of the surgical ecosystem performing it, which modulates risk independently of individual patient factors.
Healthcare Resource Feedback
Patients indirectly improve population-level access to durable, rapidly recoverable valve interventions when choosing minimally invasive repair at emerging centers, because their participation fuels procedural volume that accelerates institutional learning and justifies investment in specialized infrastructure. As more patients opt for these interventions, hospitals expand training, acquire refined tools, and develop protocols that eventually lower barriers to high-quality care across regions. The non-obvious mechanism is that individual choice functions as a market signal that reshapes resource allocation in cardiothoracic surgery, transforming localized innovation into widespread capacity.
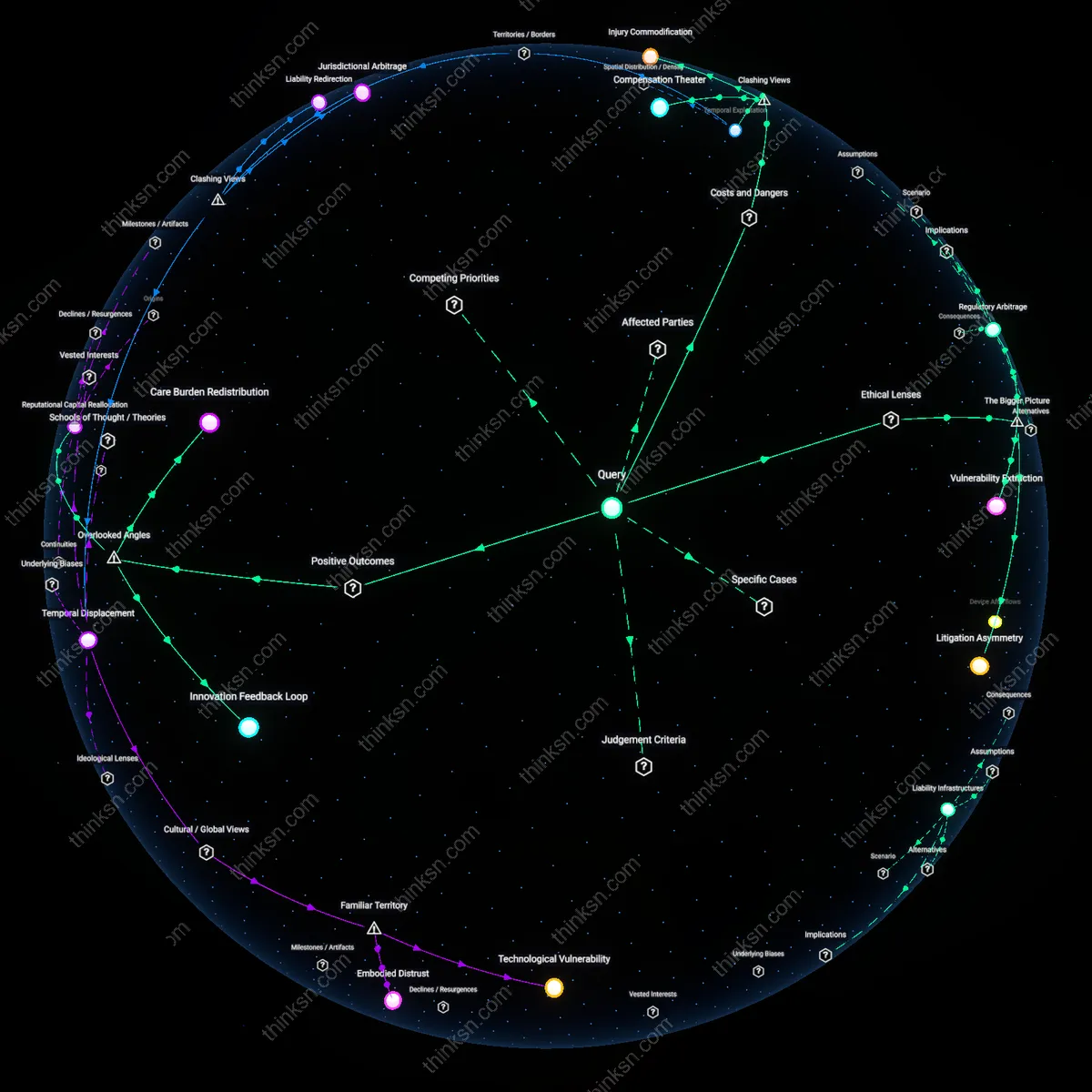
Longevity-Innovation Paradox
Selecting open surgery for its proven durability can unintentionally slow the advancement of minimally invasive techniques, depriving future patients of equally durable yet less invasive options, because delayed adoption reduces real-world data generation and industry incentive to refine devices and training programs. This creates a feedback delay where today’s risk-averse decisions preserve individual short-term safety at the cost of collective long-term innovation velocity. The systemic consequence is that patient evaluations rooted solely in personal outcome maximization may weaken the developmental pipeline for next-generation interventions, effectively trading known benefits against unrealized potential.
Hidden morbidity debt
Cardiovascular patients should prioritize open surgery over minimally invasive valve repair because the reduced initial recovery time of minimally invasive procedures creates a false economy that defers and obscures cumulative postoperative complications, increasing long-term morbidity. The mechanism operates through fragmented follow-up care in decentralized health systems, where early discharge and outpatient monitoring fail to detect subclinical hemodynamic deterioration, leading to late-stage reoperations with higher mortality. This dynamic is non-obvious because dominant clinical metrics emphasize 30-day outcomes, masking the true burden of deferred failure that accumulates outside acute care settings.
Durability theater
Patients should distrust long-term durability claims for open surgery because those data originate from historical cohorts managed in tightly regulated academic centers, creating an illusion of robustness that does not generalize to contemporary, heterogeneous practice. The durability advantage depends on surgical precision, postoperative anticoagulation compliance, and access to specialized echocardiographic surveillance—conditions often absent in community hospitals where most patients receive care. This challenges the intuitive view that open surgery’s track record reflects inherent superiority, revealing instead a performance artifact tied to selective, high-resource environments.
Clinical career horizon
Cardiovascular patients should prioritize open surgery over minimally invasive repair when the treating surgical team is within the last phase of their clinical career, because experienced surgeons nearing retirement have accumulated irreversible tacit knowledge in traditional approaches but limited adaptation to evolving best practices in durability assessment for new techniques. This creates a hidden misalignment between perceived expertise and actual long-term outcome optimization, as the surgeon’s career timeline—not just skill level—biases procedural recommendations toward what they mastered decades ago, a dynamic rarely factored into shared decision-making. Most risk-benefit analyses assume static expertise, overlooking how the diminishing time horizon of the clinician skews innovation adoption and distorts durability predictions.
Prosthetic obsolescence risk
Patients should discount the durability advantage of open surgery when living in regions with delayed access to transcatheter valve-in-valve technology, because the assumed permanence of surgical bioprostheses becomes a liability if future reinterventions are likely but only salvageable via advanced percutaneous methods not yet locally available. A durable initial repair may backfire by outlasting the window for safe reoperation, locking patients into eventual care deserts when structural valve deterioration occurs. This creates a temporal mismatch between surgical durability and technological accessibility, a hidden dependency where the geographic lag in adopting next-generation interventions inversely determines the optimal initial strategy—an inverse innovation gradient rarely acknowledged in risk calculators.
Medical Paternalism
Cardiovascular patients should defer durability assessments to clinical expertise because established hierarchies in cardiologic decision-making privilege physician judgment over patient interpretation of risk. This mechanism operates through institutionalized protocols in academic medical centers like the Mayo Clinic, where treatment pathways are codified under beneficence-driven frameworks rooted in Hippocratic ethics, making physician-led trade-off evaluation the norm. The non-obvious insight within this familiar framework is that patients often perceive autonomy as central to their choices, yet real-time decision architecture in high-volume surgical centers systematically embeds clinician authority, reinforcing a legacy of medical paternalism.
Surgical Narrative
Patients should prioritize open surgery when longitudinal outcomes dominate public discourse because lived experience and media portrayals—epitomized by televised recovery journeys and celebrity interventions—frame durability as victory. This narrative functions through cultural memory, where open-heart surgery is mythologized as the 'gold standard,' anchoring long-term survival to visible sacrifice, even as minimally invasive techniques improve. The underappreciated reality is that this trope obscures incremental innovation, making the dramatic recovery arc more cognitively available than the quiet efficacy of reduced invasiveness.
Risk Ownership
Patients must evaluate trade-offs by asserting personal responsibility for long-term outcomes, as neoliberal health policy in the United States transfers medical consequences from institutions to individuals through cost-sharing and patient activation mandates. This shift operates via accountable care organizations and value-based reimbursement models, which recast durability as a metric of consumer rationality rather than clinical consensus. The overlooked implication is that familiar appeals to 'informed choice' obscure how structural incentives shape risk tolerance, converting medical decisions into expressions of fiscal self-governance.