How Quick-Fix Meds Shape Anxiety Care and Doctor Choices?
Analysis reveals 7 key thematic connections.
Key Findings
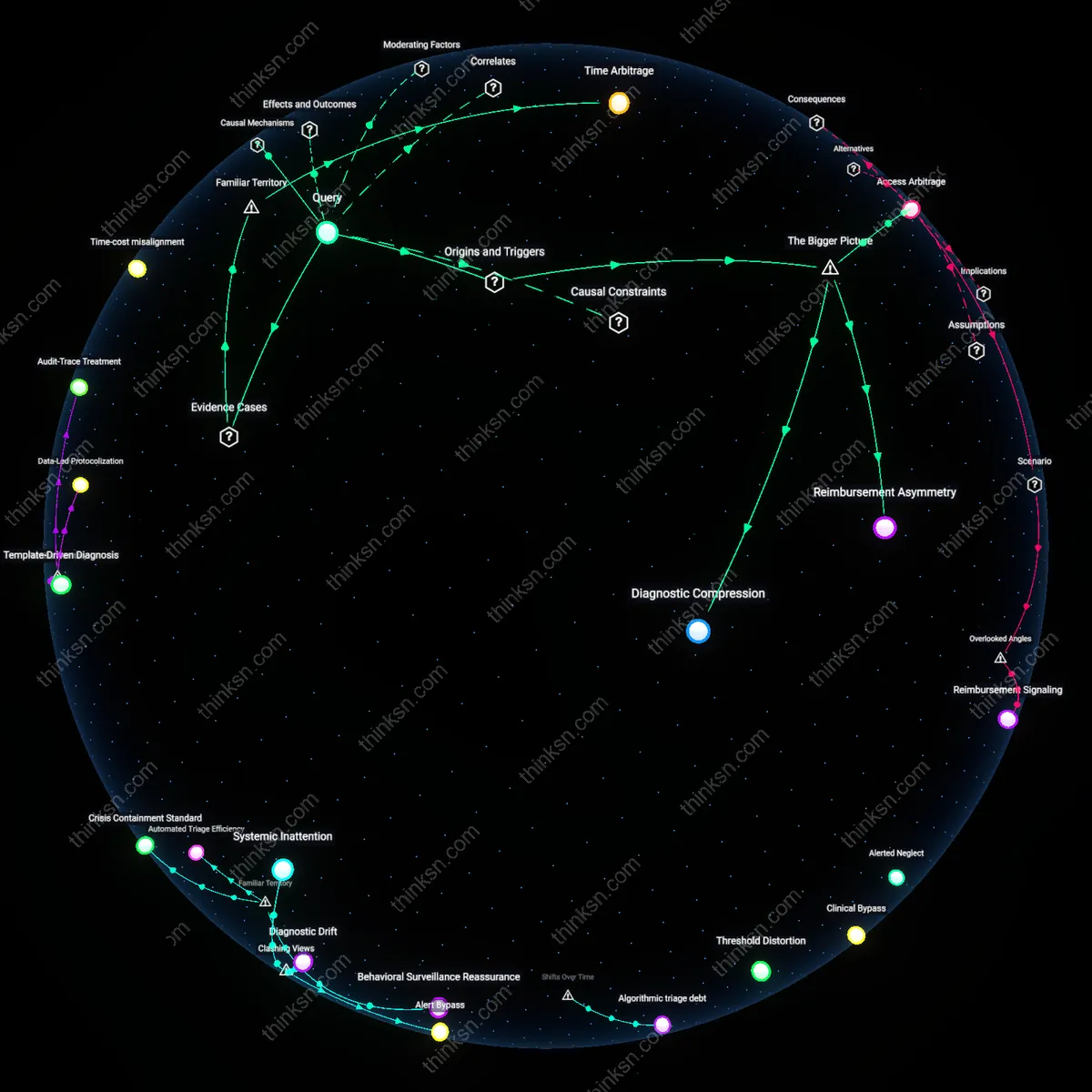
Reimbursement Asymmetry
Fee-for-service payment models in U.S. primary care directly incentivize shorter consultations over time-intensive interventions, making pharmacological management of anxiety more economically viable than behavioral referrals or longitudinal support. Clinicians operating within constrained visit windows—often 15–20 minutes—routinely prescribe anxiolytics because insurance systems reimburse medication visits similarly to psychoeducation but do not compensate the extended coordination required for cognitive behavioral therapy or social work engagement. This misalignment between clinical efficacy and financial sustainability embeds a structural preference for quick fixes, an effect that persists even when physicians are aware of superior non-pharmacological options. The underappreciated consequence is that cost-efficient care is conflated with expedient care, not value-based care, reinforcing treatment patterns that serve financial architecture more than patient outcomes.
Diagnostic Compression
Primary care settings systematically compress complex mental health presentations into treatable categories under pressure from productivity metrics like patient volume quotas and electronic health record (EHR) documentation demands, leading physicians to prioritize rapid symptom suppression over etiological exploration. Faced with high caseloads and templates oriented toward check-box diagnostics, clinicians are more likely to assign generalized anxiety disorder and prescribe first-line SSRIs than to explore trauma histories, socioeconomic stressors, or cultural contexts that might explain distress. This procedural reductionism is amplified by EHR design, which facilitates medication ordering far more than referral tracking or narrative documentation. The overlooked outcome is that diagnostic efficiency becomes a proxy for clinical adequacy, normalizing pharmacological solutions as the only tractable response within overburdened systems.
Access Arbitrage
The scarcity of mental health specialists in rural and safety-net urban clinics forces primary care physicians to function as de facto psychiatrists, resulting in reliance on medications because they are the only scalable tool available within existing workforce and referral infrastructures. In regions with fewer than one psychiatrist per 30,000 residents, GPs routinely initiate benzodiazepines or SSRIs not due to therapeutic preference but because community mental health programs are oversubscribed, Medicaid panels are thin, and care navigation support is absent. This structural workaround treats medication as a substitute for access, transforming temporary expediency into standard practice. The unrecognized systemic effect is that geographic and economic disparities in mental health infrastructure get internalized as clinical decision-making norms, even when those choices contradict guideline-based care.
Time-cost misalignment
Primary care physicians disproportionately prescribe anxiolytics because visit reimbursement structures reward speed over depth, making pharmacological interventions more economically rational than extended behavioral counseling. The mechanism operates through insurance billing codes that reimburse a 15-minute medication check-in at the same rate as a 45-minute psychosocial assessment, effectively pricing out longer discussions. This creates a hidden economic logic in clinical decisions—one rarely visible in patient-physician interactions—where time becomes a scarcer resource than medication, shifting treatment toward fast-acting drugs even when suboptimal. The overlooked dimension is not physician bias or patient demand, but the way reimbursement structures silently shape medical calculus by penalizing time investment.
Diagnostic simplification pressure
Physicians rely on quick-fix medications for anxiety because fragmented electronic health record systems incentivize rapid diagnostic coding over longitudinal symptom mapping, folding complex distress into billable ICD-10 categories like F41.1. Since EHR workflows prioritize billing-ready diagnoses over process notes, physicians convert ambiguous, evolving emotional states into discrete disorders to maintain workflow continuity, which then triggers standardized pharmacological pathways. This procedural necessity—misaligned with the messy reality of mental suffering—channels treatment toward pills because drugs are easier to document and renew than open-ended psychosocial support. The underappreciated factor is how administrative software design, not clinical judgment, steers treatment by making some responses bureaucratically 'lighter' than others.
Script Efficiency
Primary care physicians in high-volume U.S. clinics rely on prescribing SSRIs during brief anxiety consultations because reimbursement structures prioritize visit throughput over extended behavioral health integration, making medication a default procedural response. This occurs in settings like Medicaid-serving community health centers where 15-minute appointments and EHR documentation burdens incentivize discrete, actionable outputs—like prescriptions—over longitudinal coping strategies. What is underappreciated is that the script itself becomes a documentation and billing artifact, not just a clinical intervention, reinforcing its use even when suboptimal.
Time Arbitrage
In corporate-owned primary care chains like CVS MinuteClinic, providers prescribe benzodiazepines or SSRIs for anxiety because standardized protocols and algorithm-driven workflows reward resolving patient complaints within preset time envelopes, treating symptom suppression as closure. The system conditions this via performance metrics tied to patient turnover and satisfaction scores, where 'solving' anxiety quickly—often without referral options—aligns with operational efficiency. The underappreciated reality is that clinical autonomy is reshaped not by malice but by embedded temporal economics that redefine 'care' as expedient resolution.