Why Small Claims Courts Fail Victims of Defective Medical Devices?
Analysis reveals 5 key thematic connections.
Key Findings
Judicial Capacity Ceiling
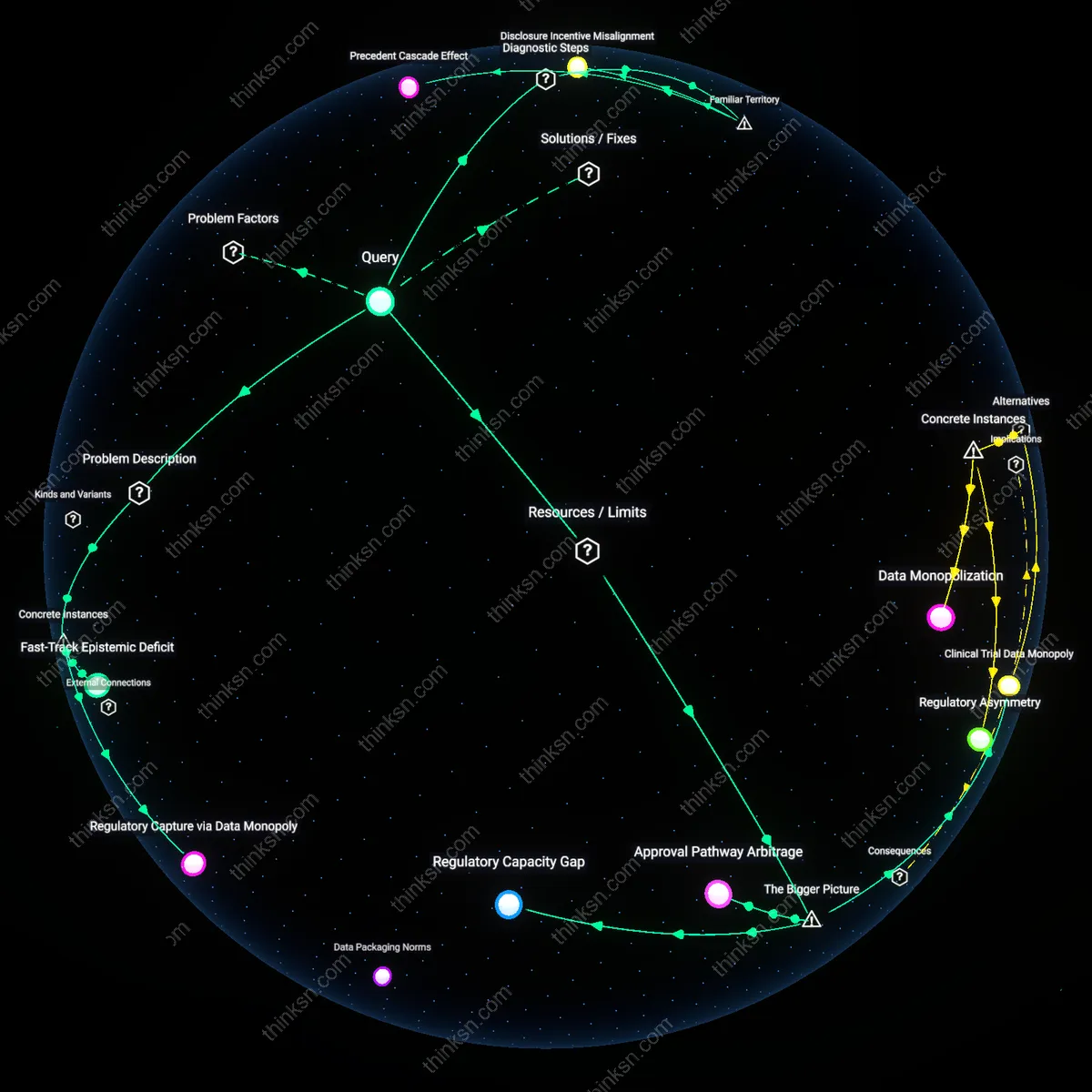
Small-claims courts cannot fully compensate victims of defective medical devices because their statutory damage caps arbitrarily truncate compensation relative to the severity of systemic harm, which severs the economic feedback loop that would otherwise incentivize manufacturers to improve device safety. These courts are designed for speed and accessibility, not complex causation or high-stakes liability, constraining awards to amounts that fail to reflect lifelong medical costs or corporate accountability—enabling manufacturers to treat payouts as routine cost-of-business rather than corrective signals. This structural design insulates device makers from full financial exposure, making FDA oversight the only actor with preemptive authority to detect and halt hazardous patterns before litigation, despite its resource limitations. The non-obvious insight is that courts’ procedural efficiency creates a liability blind spot that systematically underprices harm, redistributing risk from firms to patients.
Regulatory Preemption Trap
FDA preemption of state tort claims for federally approved medical devices legally denies small-claims courts the authority to award damages when devices comply with federal standards, even if those standards lag behind emerging safety data or clinical outcomes. This doctrine, rooted in Supreme Court interpretations of the Medical Device Amendments, prioritizes regulatory consistency over local accountability, effectively immunizing manufacturers from liability for harms that fall within approved specifications. As a result, victims cannot achieve redress through decentralized legal channels, reinforcing dependence on the FDA as the sole legitimate source of corrective action. The underappreciated dynamic is that judicial deference to federal regulation creates a monopoly of oversight responsibility, disabling compensatory systems from serving as adaptive checks on regulatory inertia.
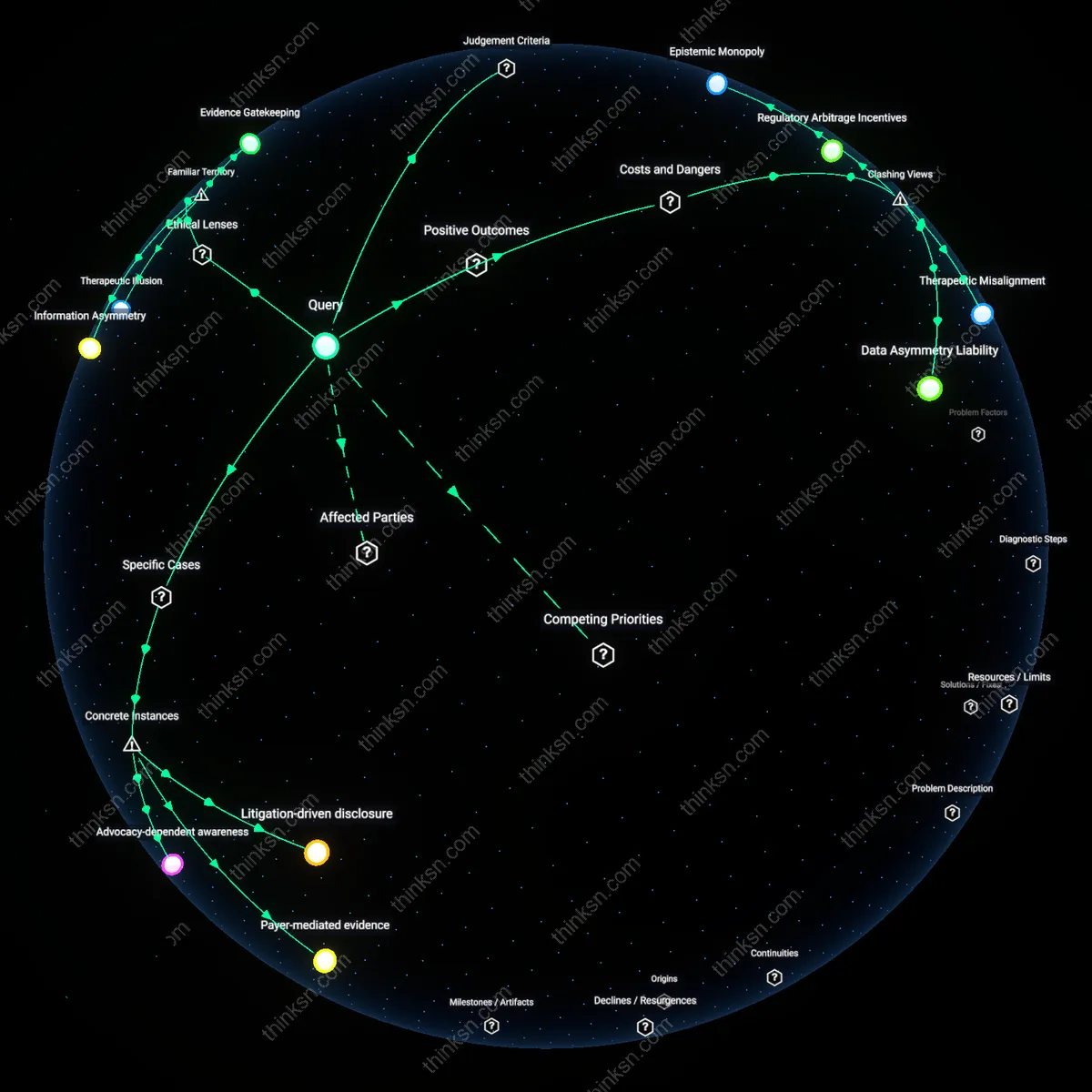
Asymmetric Information Infrastructure
Manufacturers possess proprietary clinical trial data, post-market surveillance analytics, and engineering specifications that are inaccessible to small-claims courts, preventing judges from linking device failure to corporate conduct without third-party validation—thus rendering compensation contingent on FDA public reporting or whistleblowers. This information asymmetry allows firms to obscure causality and delay accountability, while courts lack subpoena power or technical staff to independently verify defects, especially in cases involving software-driven or implantable devices. Consequently, victims must await official FDA determinations even when harm is evident locally, entrenching agency dependence. The overlooked reality is that the absence of a shared evidentiary platform transforms the FDA into a gatekeeper of truth, not just safety, effectively monopolizing the conditions for legal redress.
Compensation Lag
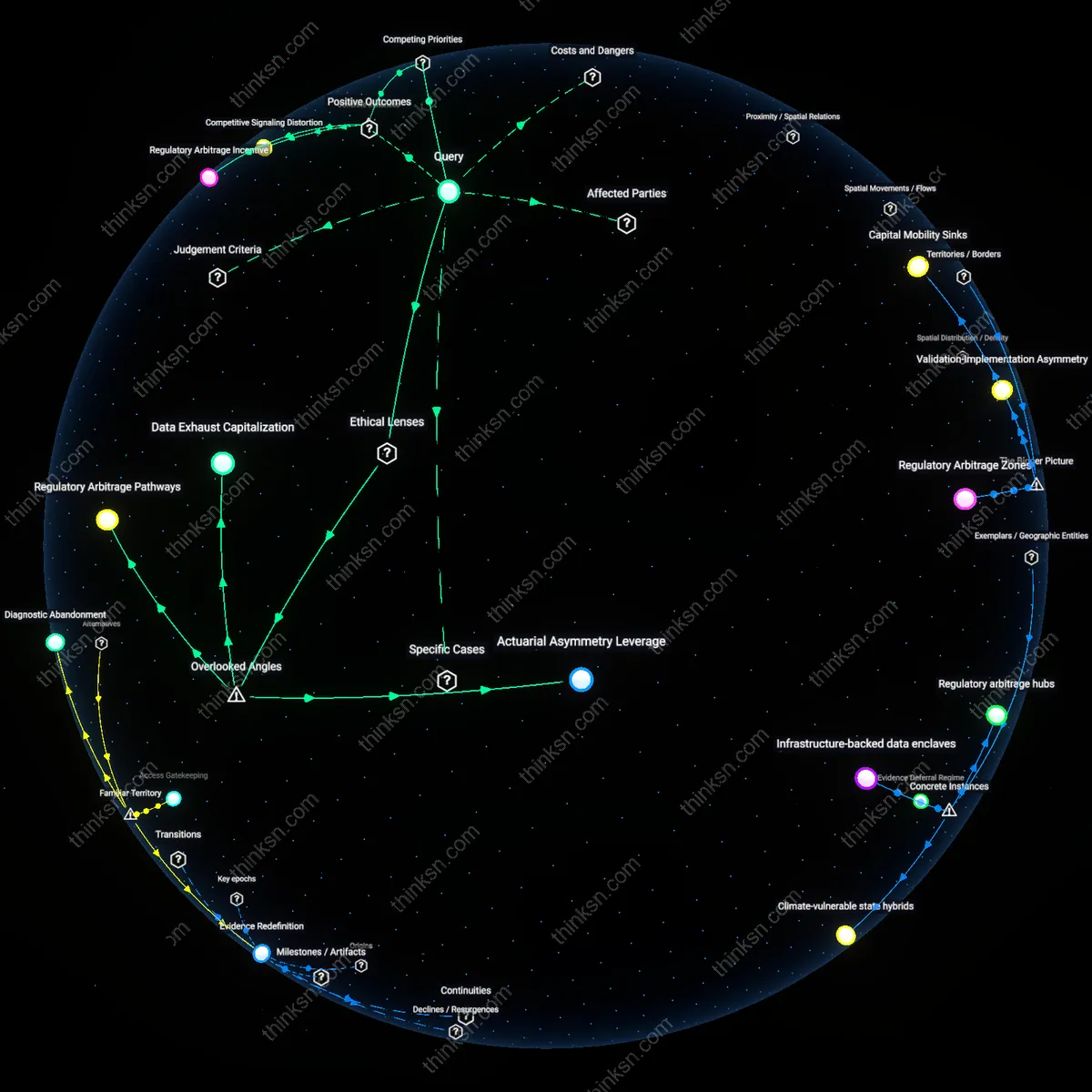
Small-claims courts cannot keep pace with the rapid diffusion of new medical devices because their adjudication cycles are measured in months or years, while device deployment and harm manifestation now occur on faster technological timelines. Post-1990s FDA fast-track approvals, especially under the 510(k) clearance pathway, enabled widespread market entry of devices without longitudinal safety data, creating a disconnect between injury occurrence and legal recognition of defect. This temporal misalignment means courts rely on evidence that lags behind real-world use, making compensation reactive rather than preventative. The underappreciated consequence is not just delayed justice but systemic failure to signal risks in time to prevent subsequent harms, revealing compensation as temporally decoupled from risk emergence.
Fragmentation Penalty
Since the 1980s expansion of tort reform and federal preemption doctrines, small-claims litigation for medical devices has been systematically fragmented across jurisdictions, limiting the aggregation of harm patterns that could establish defectivity. Unlike product categories with mass-injury visibility (e.g., pharmaceuticals), defective devices like faulty infusion pumps or pelvic mesh dispersed geographically produced isolated claims too minor for coordinated class action, yet cumulatively significant. Courts handling individual cases cannot generate generalizable rulings due to doctrinal limits on precedent scaling in minor tribunals. The historical shift toward decentralized litigation after the 1990s preemption rulings thus penalized victims of low-volume, high-variability harms, forcing reliance on centralized regulatory bodies to identify systemic flaws that fragmented courts cannot see.