Why Medical Necessity Narratives Disadvantage Unrepresented Patients?
Analysis reveals 7 key thematic connections.
Key Findings
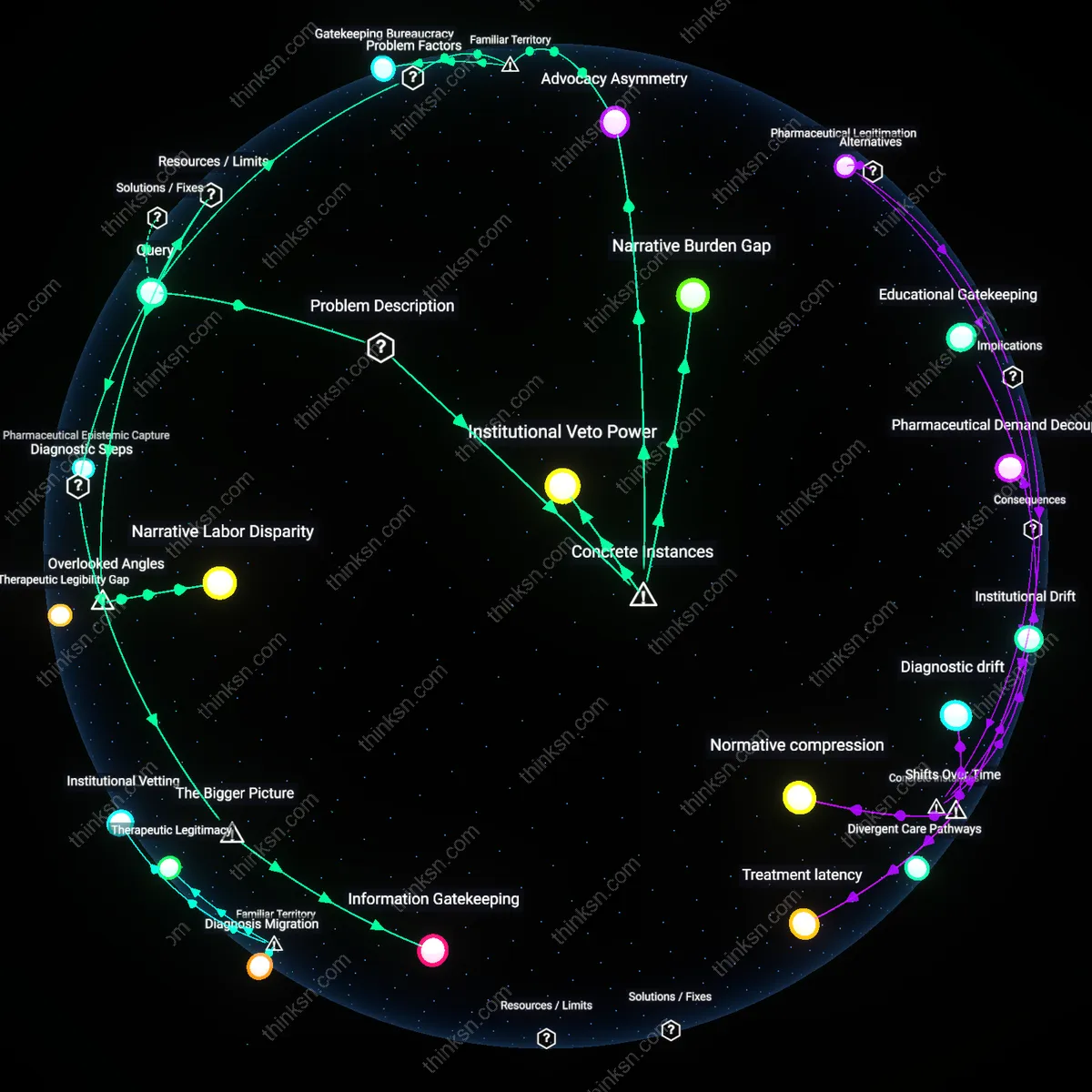
Advocacy Asymmetry
Patients with complex chronic conditions like sickle cell disease at Howard University Hospital in the 2010s frequently faced insurance denials for pain management regimens because their primary care providers lacked the institutional weight to justify prolonged opioid use as medically necessary, whereas similar narratives from oncologists for cancer patients were routinely accepted, revealing that the legitimacy of a medical necessity claim is unevenly distributed across specialties. The mechanism here is not clinical severity but perceived disciplinary authority—hematologists managing sickle cell care were systematically overruled by payors despite longitudinal patient relationships, while oncology’s narrative dominance in pain justification went unchallenged, making the disparity one of epistemic privilege rather than medical evidence. This case exposes the non-obvious reality that insurance validation systems rely on hierarchical credibility within medicine, not uniform clinical standards.
Narrative Burden Gap
In rural Kentucky clinics during the 2018 Medicaid prior authorization expansion, diabetic patients without endocrinology access were denied continuous glucose monitors because family physicians were neither trained nor compensated to write the detailed physiological trajectory narratives required by insurers, unlike urban specialists who routinely included such documentation. The system assumes narrative production capacity as a neutral professional function, yet in underserved areas, primary care providers operate under time and training constraints that preclude crafting insurer-optimized medical justification, effectively shifting clinical labor into bureaucratic authorship. The underappreciated insight is that medical necessity is not determined solely by patient condition but by a provider’s ability to linguistically perform necessity within an insurer’s preferred discourse model, turning narrative competence into a structural gatekeeper.
Institutional Veto Power
In 2021, Massachusetts General Hospital’s dermatology department successfully appealed denials for biologic therapies in psoriasis by embedding peer-to-peer review clauses in their narrative templates, whereas safety-net clinics like Boston Medical Center lacked the administrative infrastructure to sustain such advocacy, leading to disparate approval rates despite identical clinical presentations. The differential outcome stems not from medical reasoning but from embedded institutional capacity—elite hospitals codify resistance to payer logic into routine documentation, while resource-constrained sites treat narratives as one-off administrative tasks. This instance reveals the non-obvious mechanism that insurance governance is navigated through organizational memory and standardized pushback protocols, meaning medical necessity is increasingly a product of systemic defiance capability rather than individual patient need.
Gatekeeping Bureaucracy
Insurance companies require a physician’s justification of medical necessity to authorize coverage, creating a procedural barrier that defaults to denial without specialist input. Primary care providers, who often lack subspecialty credibility or detailed knowledge of cutting-edge interventions, are ill-equipped to argue against utilization management algorithms or appeals panels, leaving generalists to navigate systems designed to defer to elite clinical authority. This dynamic reinforces a de facto hierarchy where access hinges not on patient need but on the prestige and persistence of the documenting physician—a structural bias invisible to public conversation focused on insurance red tape alone.
Diagnostic Elitism
Specialists wield outsized influence in constructing what counts as legitimate illness because they define the diagnostic thresholds and treatment algorithms that insurers use to assess medical necessity. When a condition lacks consensus criteria—such as myalgic encephalomyelitis or fibromyalgia—only a specialist’s narrative can confer legitimacy, making the physician’s title more determinative than the patient’s symptoms. This creates a self-reinforcing loop where only diseases recognized by specialist communities gain coverage, a power imbalance rarely discussed in patient autonomy debates that tend to focus on consent rather than epistemic authority.
Information Gatekeeping
The requirement for a physician's 'medical necessity' narrative structurally disadvantages patients without specialist advocacy by instituting specialists as necessary validators of diagnostic legitimacy within insurance and institutional systems. Primary care providers often lack the authority or detailed procedural justification to satisfy payer requirements for advanced imaging or specialty testing, forcing patients to secure referrals from specialists who can produce narratives aligned with reimbursement criteria; this creates a prerequisite of specialist engagement before diagnostic access, even when clinical suspicion exists. The non-obvious consequence is that diagnostic authority shifts from clinical presentation to narrative credibility shaped by specialty status, not medical urgency—enabling institutional gatekeeping where information control, not symptom progression, determines investigation timing.
Narrative Labor Disparity
Patients without specialist advocacy face heavier narrative labor burdens because they must self-generate medically persuasive justifications that insurers require but seldom support structurally. This burden falls most heavily on patients with limited health literacy or cognitive bandwidth due to illness, who lack access to clinical allies capable of translating symptoms into reimbursable diagnostic trajectories. The non-obvious dimension is not just the absence of medical authority but the unacknowledged effort required to perform its function—crafting a legitimate clinical story under conditions of systemic skepticism and temporal urgency. This reframes 'medical necessity' not as an objective threshold but as a narrative competency gap enforced through administrative routines.