Prioritizing Cost in Health: Just or Unethical for Rare Diseases?
Analysis reveals 7 key thematic connections.
Key Findings
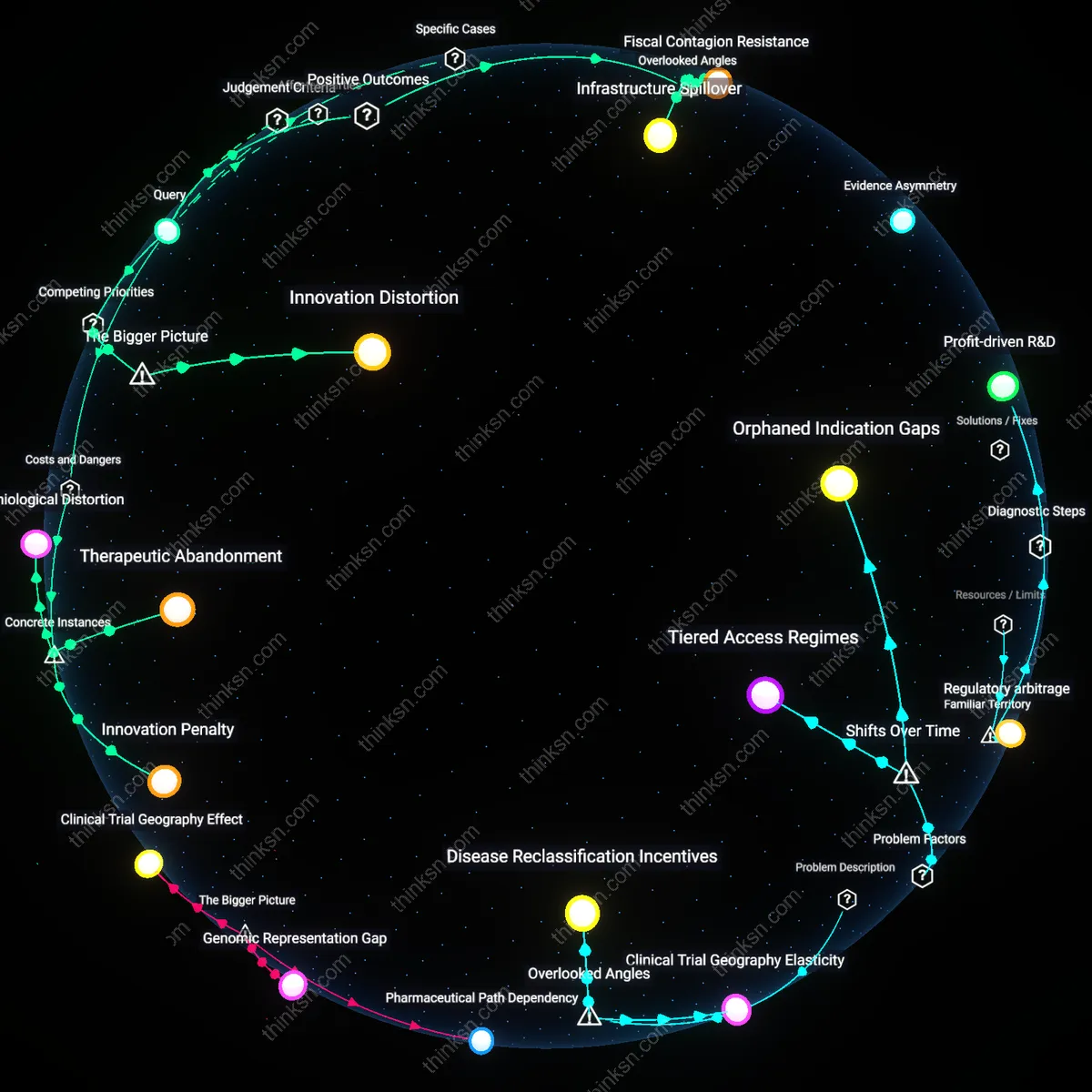
Infrastructure Spillover
Health systems that apply cost-effectiveness thresholds generate underappreciated public health infrastructure improvements by redirecting savings into primary care systems in underserved regions like rural India and sub-Saharan Africa, where integrated diagnostic networks and trained personnel are consolidated under centralized funding decisions; this reinvestment strengthens system-wide surveillance, early detection, and treatment capacity for communicable and chronic diseases alike, a benefit rarely attributed to rationing decisions because the focus remains on excluded therapies rather than distributed gains in care delivery systems.
Innovation Signaling
Cost-effectiveness thresholds create a feedback signal to biopharmaceutical developers in markets like the European Union and Canada, where reimbursement decisions publicly benchmark value, thereby shaping the early-stage R&D pipeline toward molecular targets with broader patient populations and modifiable delivery formats such as oral formulations or durable gene-editing platforms; this steering function is invisible in ethical debates that frame rationing as purely restrictive, yet it systematically alters the risk calculus of venture capital and academic spin-offs seeking predictable market access.
Fiscal Contagion Resistance
By institutionalizing cost-effectiveness thresholds, health systems in countries such as Thailand and South Korea reduce the risk of fiscal contagion from rare disease spending spikes that could destabilize regional budgets and trigger cuts in maternal or infectious disease programs, preserving macro-equity through inter-disease budget insulation—a protective mechanism overlooked because rare disease advocacy rightly emphasizes individual tragedy, but obscures how one category’s funding surge can silently degrade population-level outcomes in high-burden domains.
Therapeutic Abandonment
The UK's National Institute for Health and Care Excellence (NICE) systematically denied funding for treatments like Soliris (eculizumab) for paroxysmal nocturnal hemoglobinuria because its cost per quality-adjusted life year exceeded £300,000—over ten times the standard threshold, effectively withdrawing state-backed therapeutic responsibility from ultra-rare disease patients, a mechanism enabled by rigid cost-effectiveness metrics that delegitimize care based on statistical rarity rather than clinical urgency, revealing how formal cost discipline can become an institutional excuse for medical disengagement.
Innovation Penalty
France’s selective reimbursement of gene therapies like Zolgensma for spinal muscular atrophy only after protracted negotiations and annuity-based payment schemes demonstrates how cost-effectiveness thresholds penalize one-time curative treatments by distorting their value across artificial timeframes, a mechanism in which health technology assessment bodies treat curative innovation as a budgetary threat rather than a systemic benefit, exposing the underappreciated risk that cost controls favor recurring revenue treatments over transformative ones.
Epidemiological Distortion
Australia's Pharmaceutical Benefits Scheme (PBS) delayed listing of Kalydeco (ivacaftor) for cystic fibrosis subtypes for over two years due to cost-effectiveness calculations that treated its narrowly indicated patient pool as a fiscal burden rather than a diagnostic vanguard, a process in which health systems misread precision medicine as inefficient by conflating small population size with low impact, thereby discouraging biomarker-driven development and encouraging a false preference for broad, less effective therapies.
Innovation Distortion
Justifying cost-effectiveness thresholds in health systems is rational from a population efficiency standpoint because pharmaceutical firms adapt drug development and pricing strategies based on the predictable existence of such thresholds, thereby shaping the pipeline of medical innovation toward financially viable niches rather than unmet need. When agencies like Germany’s G-BA or Canada’s CADTH institutionalize thresholds (e.g., €50,000 per QALY), they create a regulatory gravity well that incentivizes biotech firms to engineer high-cost therapies for ultra-rare conditions only when backed by premium pricing and outcome guarantees, often at the expense of broader-spectrum treatments. This reveals a hidden feedback loop where public cost-control mechanisms unintentionally steer private R&D toward ever-narrower indications, making threshold policies not just allocative tools but upstream determinants of innovation direction—what is underappreciated is that cost containment can thus generate its own market failures.