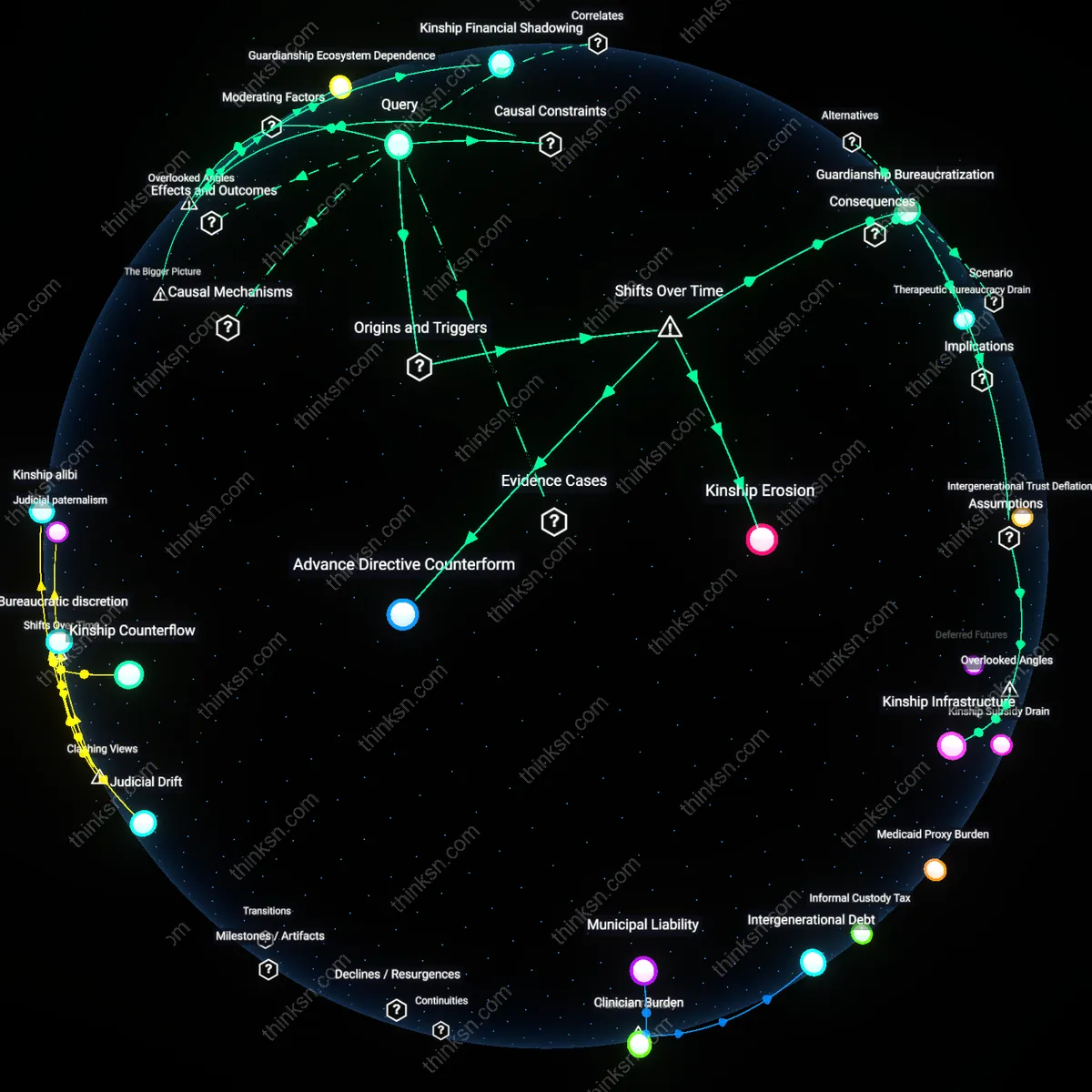
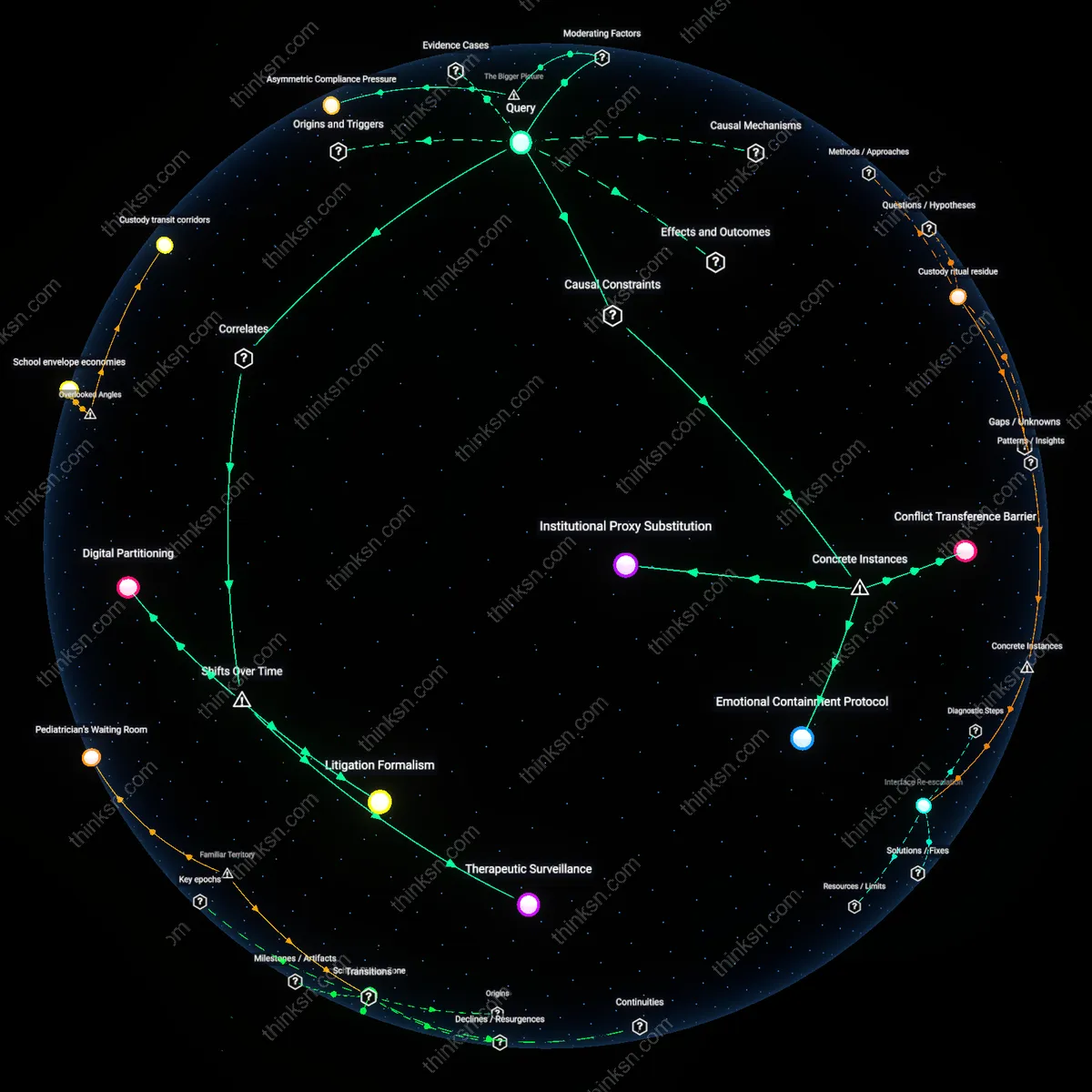
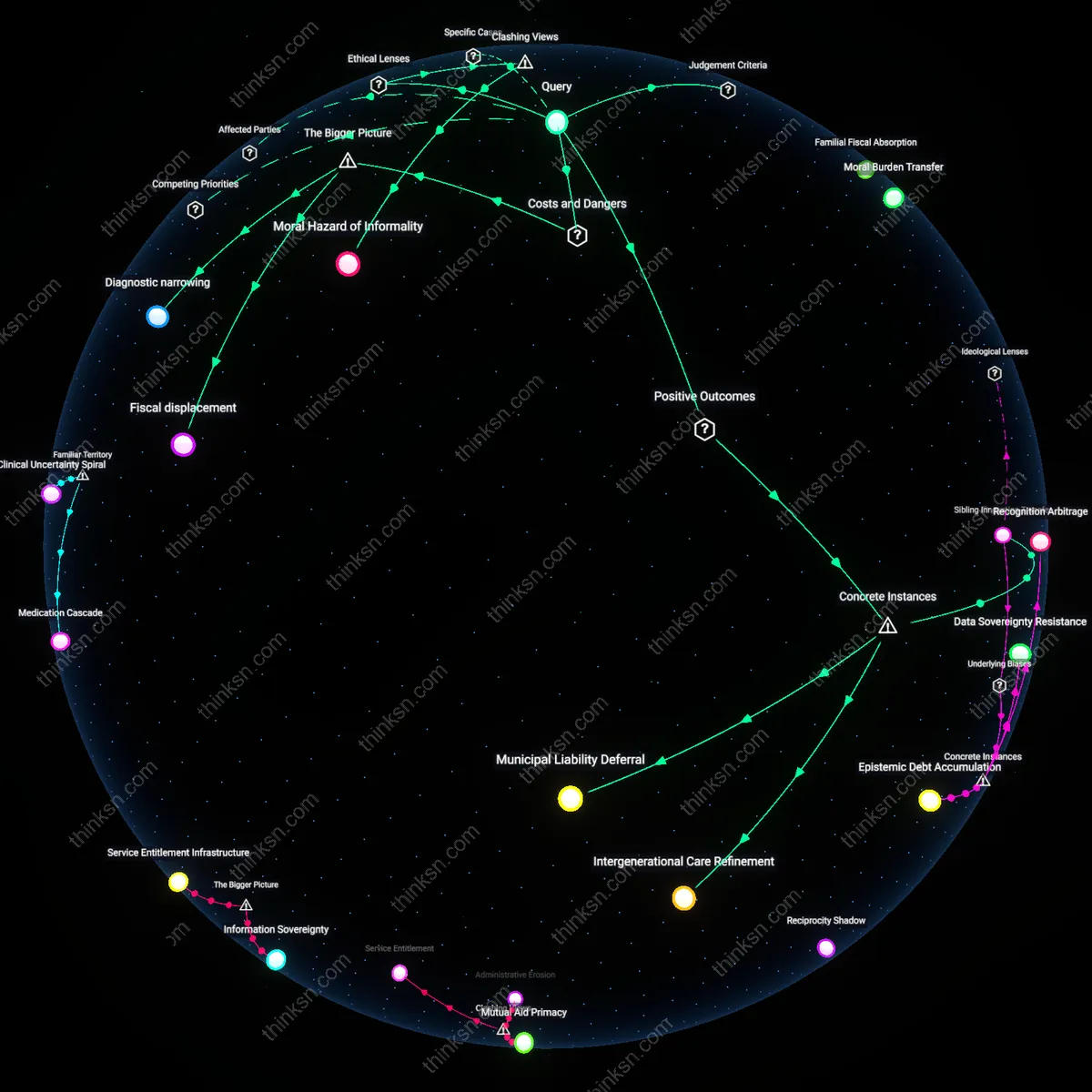
Medicaid Struggles for Mixed-Status Families: Navigating Systemic Barriers?
Analysis reveals 6 key thematic connections.
Key Findings
Administrative Visibility Trap
Mixed-status families avoid Medicaid enrollment because documented family members fear that applying creates a formal record that could be accessed and weaponized by immigration enforcement, even when the applicant child is a citizen; this occurs through the interplay of federal data systems like SAVE and state-level public benefits administration, where participation leaves digital traces that families perceive—correctly or not—as increasing deportation risk; the non-obvious insight is that the barrier is not eligibility or language, but the very act of state documentation, which redefines safety in terms of invisibility rather than rights access.
Kinship Risk Calculus
Undocumented parents decline Medicaid for citizen children not due to lack of need but because acceptance of benefits introduces a moral and logistical dilemma in which parental sacrifice—denying resources to maintain familial cohesion—becomes the safest survival strategy; this operates through daily household negotiations where the parent’s presence is treated as more vital than medical services, a dynamic amplified in communities with high ICE activity such as rural Georgia or Long Island; this undermines the assumption that benefit uptake aligns with legal entitlement, revealing decision-making rooted in relational risk management rather than policy compliance.
Jurisdictional Arbitrage
Some mixed-status families access Medicaid not through direct enrollment but by leveraging regional disparities in implementation, such as applying in urban counties with sanctuary policies like Cook County while residing in restrictive states, exploiting gaps between federal eligibility rules and local bureaucratic discretion; this works through mobile kinship networks that route applications through trusted community health clinics, effectively gaming geographic variation in enforcement culture; the dissonance lies in treating systemic fragmentation not as a flaw but as a tactical opportunity, exposing how noncompliance with intended administrative geography becomes a method of care access.
Chilling Effect
Mixed-status families avoid Medicaid enrollment due to immigration enforcement fears tied to the public charge rule. Families believe any benefit use could endanger a parent’s immigration status, even though citizen children are technically eligible. This fear persists despite legal distinctions because federal immigration policy has historically weaponized benefit participation as a metric for deportation risk. The non-obvious insight is that the barrier is not ineligibility but a state-produced climate of deterrence that overrides accurate knowledge of rights.
Documentation Burden
Families face administrative exclusion through complex verification processes that conflate household applications with individual eligibility. State Medicaid agencies require identification and immigration documents for all household members, creating a de facto barrier when one has none. Caseworkers, lacking training on mixed-status protocols, often misapply rules or refer families to immigration authorities. The underappreciated mechanism is how neutral bureaucratic procedures become discriminatory through differential impact, even without explicit intent.
Kinship Workarounds
Eligibility is accessed when citizen children are enrolled under the care of a relative with legal status, such as a grandparent or aunt. This workaround transfers caregiving responsibility formally or informally to sidestep the undocumented parent’s exclusion from application processes. These arrangements are unstable, relying on extended family capacity often strained by poverty and migration trauma. The insight is that systemic exclusion produces informal care infrastructures that absorb risk but remain invisible to policy design.