How Medicaid Fragmentation Favors Some States Over Others?
Analysis reveals 8 key thematic connections.
Key Findings
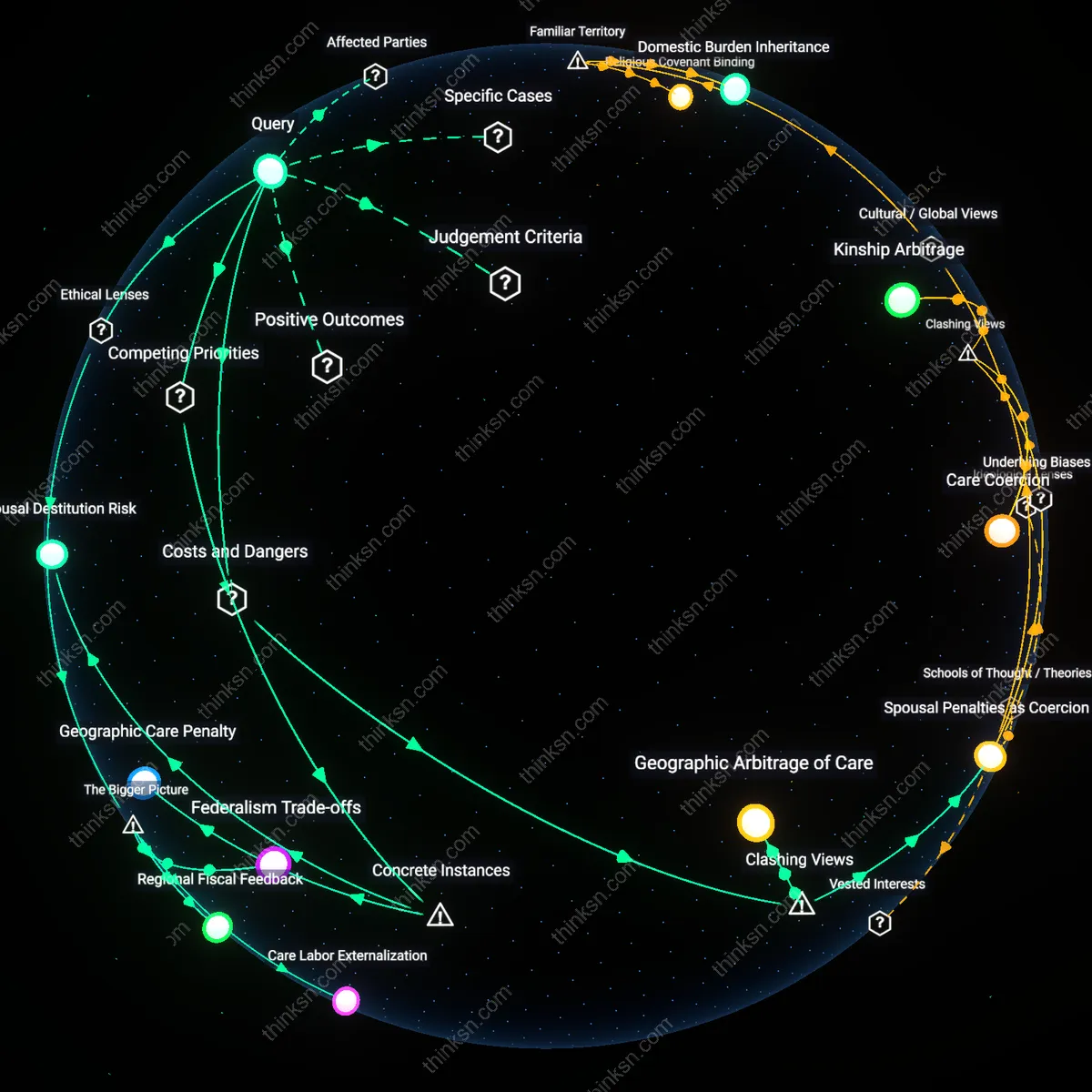
Geographic Arbitrage of Care
States with more expansive Medicaid home and community-based services (HCBS) waivers create de facto migration incentives for families who can physically relocate, turning access to long-term care into a function of mobility rather than medical need. This dynamic favors families with transportation resources, housing flexibility, and private savings—enabling them to 'shop' for eligibility rules across state lines—while trapping lower-income families in states with restrictive asset limits or waiting lists, even when their care needs are identical. The non-obvious consequence is not just inequality but the emergence of an informal market in care access, where geographic placement becomes a strategic decision akin to tax or insurance optimization, undermining Medicaid’s foundational principle of need-based equity.
Spousal Penalties as Coercion
Medicaid’s spousal impoverishment protections vary significantly by state, leading some states to impose aggressive income and asset transfers from community spouses, which in practice pressures healthier spouses to abandon or divorce partners in need of long-term care to avoid financial ruin. In states like Alabama with minimal spousal income allowances, married couples face stark 'divorce to qualify' decisions, while in states like New York, broader protections preserve marital stability at public expense. The clashing view reveals that variation does not merely reflect fiscal discretion but actively reshapes intimate family commitments—transforming Medicaid from a care program into a regulator of marital behavior, where eligibility rules become tools of covert social engineering.
Fiscal Trade-off Trap
Alabama’s strict asset limits for Medicaid long-term care—$2,000 for a single applicant—force middle-class families to fully liquidate homes and savings before qualifying, as seen in the 2022 Montgomery case where a retired couple sold their paid-off home to cover nursing care, sacrificing generational wealth security to access basic health coverage, revealing that state-level austerity in eligibility criteria converts caregiving support into a zero-sum exchange between medical access and family economic resilience.
Geographic Care Penalty
In 2019, a family in Maine accessed home- and community-based services (HCBS) through Medicaid’s waiver program, allowing an elderly parent to age in place, while a nearly identical family in South Dakota was denied such waivers due to capped enrollment and waitlists over 2,000 people long, demonstrating how state-by-state rationing of non-institutional care forces equivalent households into institutionalization or unpaid familial labor, exposing a hidden penalty where residential location dictates whether independence or family time is sacrificed for care access.
Spousal Destitution Risk
When Ohio enforced its ‘spousal impoverishment’ rules in a 2021 Cuyahoga County case, the community spouse was allowed to retain only $134,280 in countable assets—far below the actual cost of independent living—compelling the healthy partner to enter low-wage work while managing full-time caregiving, illustrating how state-specific interpretations of federal safeguards fail to prevent destitution, turning the protection of one spouse’s care into the economic endangerment of the other, an inequity normalized under decentralized Medicaid administration.
Federalism Trade-offs
Variation in Medicaid long-term care eligibility across states produces unequal family burdens because federalism delegates means-tested program design to states, enabling divergent interpretations of need, asset limits, and spousal impoverishment protections under the same federal statute. State administrators, responding to disparate budgetary constraints and political pressures, implement thresholds that systematically advantage families in wealthier or more expansive states—such as New York’s community Medicaid waiver—while disadvantaging those in restrictive states like Alabama, where home equity and income rules disqualify broader populations. This creates ethically significant inequity under utilitarian and Rawlsian frameworks, as similarly situated families experience vastly different access to dignity-preserving care based on geography, not need—a consequence baked into the federalist structure that prioritizes local control over distributive justice. The non-obvious insight is that the enabling condition is not mere policy variation, but the constitutional delegation of welfare design under the Spending Clause, which insulates disparities from judicial or federal correction.
Care Labor Externalization
Differential Medicaid eligibility forces families in restrictive states to absorb uncompensated long-term care labor, whereas families in expansive states can offload such labor to publicly funded home health aides or nursing facilities. In states like Texas, where institutionalization is often the only covered option, adult children—disproportionately women—become de facto providers, constrained by lack of respite, wage loss, and health deterioration; this shift is systemically enabled by the federal waiver system that rewards institutional over home- and community-based services. From a feminist ethics perspective, this spatially uneven burden constitutes structural exploitation of familial care labor, disproportionately impacting lower- and middle-income households that lack private insurance or intergenerational wealth. The overlooked dynamic is that geographic variation functions as a hidden redistribution mechanism—from public systems to private, gendered labor pools—mediated by state-level policy choices that the federal baseline permits but does not correct.
Regional Fiscal Feedback
States with more generous Medicaid long-term care eligibility face higher per capita expenditures, which in turn intensify resistance to tax increases or federal matching reductions, creating a self-reinforcing fiscal-political equilibrium that entrenches geographic disparities. For example, in Minnesota, high public investment in Elderly Waivers has built a constituency of service providers and families reliant on the system, which lobbies to preserve eligibility, whereas in Mississippi, low coverage levels correlate with weaker provider infrastructure and political narratives that frame public support as unsustainable. This feedback loop, driven by path dependency and fiscal federalism, entrenches unequal outcomes not due to differences in need but because early policy choices shape institutional capacity and interest group formation. The underappreciated causality is that Medicaid variation persists not merely from initial design differences, but because regional fiscal dynamics generate political economies that make convergence across states increasingly unlikely—even when ethical imperatives for equity arise.