Should You Screen for Melanoma with Ambiguous Evidence and High Costs?
Analysis reveals 8 key thematic connections.
Key Findings
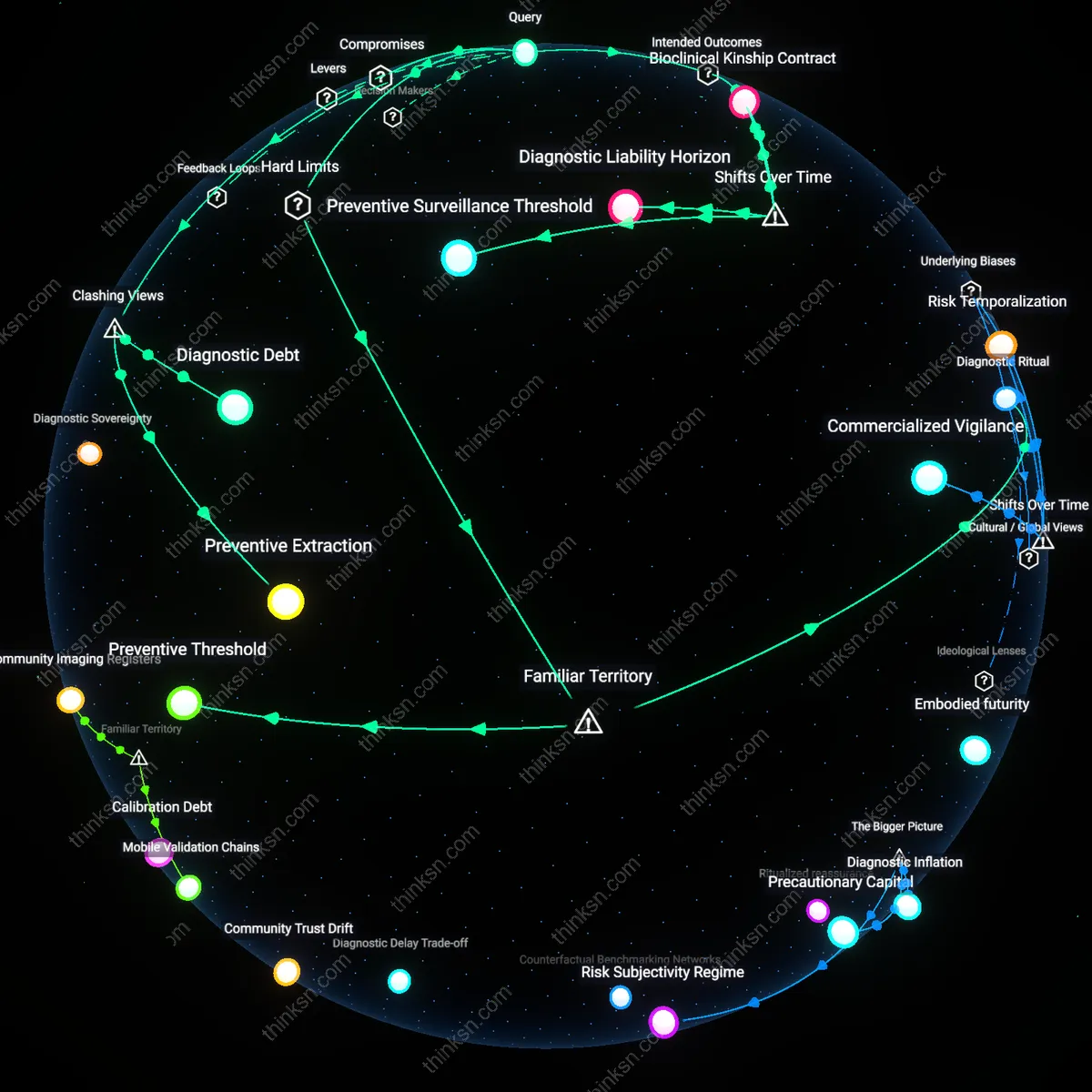
Preventive Threshold
Individuals with a family history of melanoma should undergo full-body skin imaging if they have more than one first-degree relative diagnosed before age 50, as this subgroup shows a demonstrated 10-fold increased risk that offsets cost and uncertainty within clinical guidelines. Dermatologists at major cancer centers apply this threshold because surveillance protocols at institutions like MD Anderson and Memorial Sloan Kettering show improved early detection rates in genetically predisposed cohorts, making cost-benefit calculations secondary to risk stratification. This approach reveals how the public’s fixation on ambiguous evidence often overlooks the existence of clinically defined high-risk brackets where action is no longer debatable but protocol-driven.
Diagnostic Ritual
People should schedule full-body imaging primarily to fulfill a symbolic commitment to vigilance, not because they expect definitive results, since annual skin checks function socially like medical check-ups that affirm personal responsibility for health. In suburban dermatology clinics across states like California and Florida, patients with familial risk describe these visits as 'doing everything I can,' signaling moral adherence to preventive norms even when evidence is uncertain. This exposes how the familiar discourse around cancer prevention masks a deeper cultural ritual—where undergoing imaging becomes less about efficacy and more about enacting the role of the 'responsible patient.'
Diagnostic Debt
Individuals with a family history of melanoma should undergo full-body skin imaging because delaying detection to avoid cost mirrors the long-term consequences of underinvesting in early monitoring infrastructure, where savings today amplify future system burdens. Dermatologists at academic medical centers increasingly observe that genetically high-risk patients who forgo imaging accrue undetected neoplastic changes, converting cost avoidance into later-stage, higher-cost interventions. This dynamic reveals that cost-conscious restraint in imaging reproduces a fiscal logic that prioritizes short-term budgetary control over longitudinal health trajectory management, a trade-off rarely disclosed in patient counseling. The non-obvious insight is that deferring imaging isn’t prudence—it’s deferring liability onto future clinical systems and the patient’s own body.
Risk Theater
Patients should avoid routine full-body imaging because its perceived preventive value often serves a ritualistic function—performing vigilance without proven mortality reduction—particularly in insured populations seeking symbolic reassurance over material outcomes. In private dermatology clinics in high-income regions like Manhattan or La Jolla, full-body imaging has become a normalized rite among affluent families with melanoma histories, even absent evidence of survival benefit, effectively commodifying anxiety into a clinical service. This performance of control through technology displaces investment in more effective but less visible strategies, like behavioral change or household-level sun safety education. The underappreciated reality is that these scans often function not as diagnostics but as medical theater, legitimizing ongoing risk without altering it.
Preventive Extraction
High-risk individuals should selectively engage with full-body imaging only when data access—not personal health outcomes—is the primary goal, such as contributing to research biobanks at institutions like the NIH or Melanoma Institute Australia. In these contexts, undergoing imaging becomes less a personal preventive act and more a form of bodily data donation that advances population-level risk modeling, often with little direct benefit to the individual. This shifts the rationale from clinical care to infrastructural contribution, exposing how preventive medicine increasingly extracts biological information from worried well patients to sustain predictive algorithms they will never see or influence. The overlooked condition is that cost and uncertainty are accepted not for health gains, but because the system profits from their participation as data sources.
Preventive Surveillance Threshold
Individuals with a family history of melanoma should adopt full-body skin imaging when longitudinal dermatological tracking reveals a shift from reactive lesion removal to proactive risk stratification, as occurred in high-risk clinics in Australia after the 2010 implementation of dermoscopic monitoring networks. This transition institutionalized serial imaging as a gatekeeping mechanism for early intervention, embedding cost-benefit calculus into familial risk profiling rather than treating imaging as an isolated diagnostic act, thereby redefining the acceptable threshold for preventive surveillance in the absence of definitive evidence.
Diagnostic Liability Horizon
These individuals should consent to full-body imaging not for immediate clinical benefit but to align with a shifting legal and ethical standard of care that emerged post-2015, when malpractice rulings in the U.S. began recognizing failure to image high-risk patients as a breach of duty, regardless of outcome. This temporal pivot reframed imaging as a risk-mitigation practice for both patients and providers, where the accumulating archive of skin maps functions less as medical data than as a shield against retrospective liability, transforming cost from a barrier into a deferred investment in legal defensibility.
Bioclinical Kinship Contract
Familial melanoma risk carriers ought to undergo imaging as a fulfillment of an evolving expectation of genetic stewardship that crystallized in precision medicine initiatives of the 2020s, where data generation for at-risk relatives became as clinically prioritized as individual diagnosis. In multisite registries like the GenoMEL Consortium, skin imaging shifted from a personal health decision to a kinship obligation, revealing how biospecimen and phenotypic data sharing across generations has reconfigured family responsibility into a structured, medically mediated contract governing surveillance participation.