Why Delay End-of-Life Talks When Planning is Hard Later?
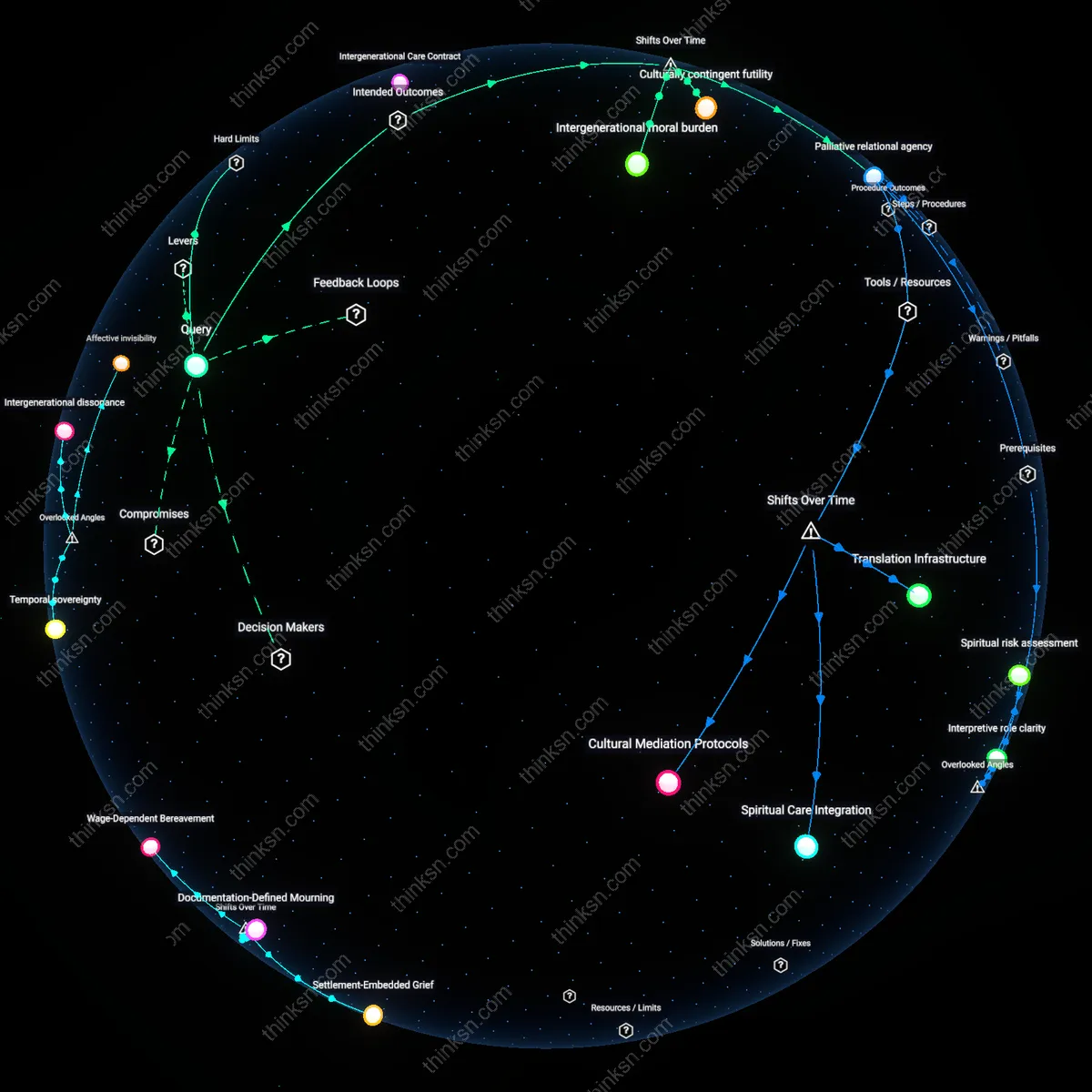
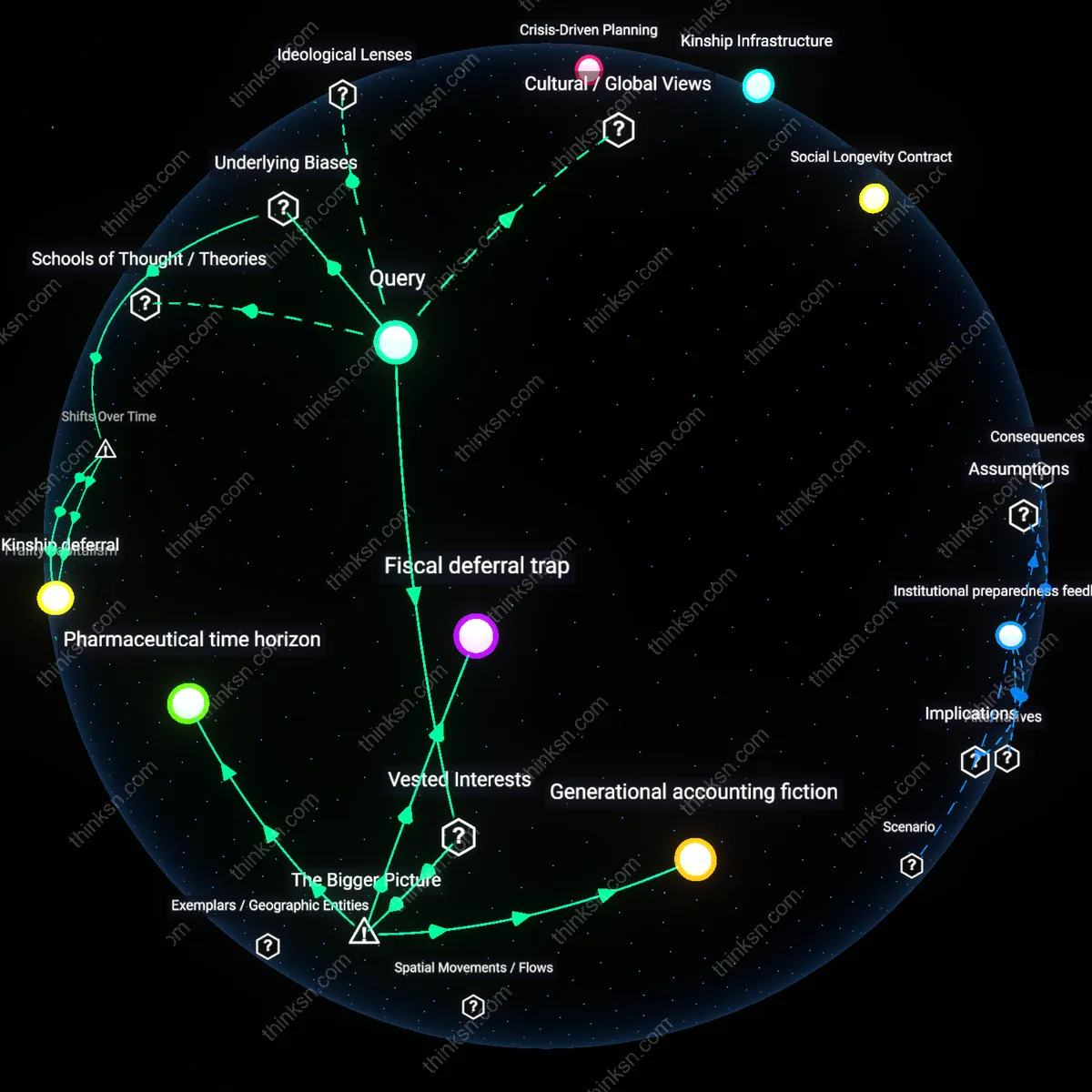
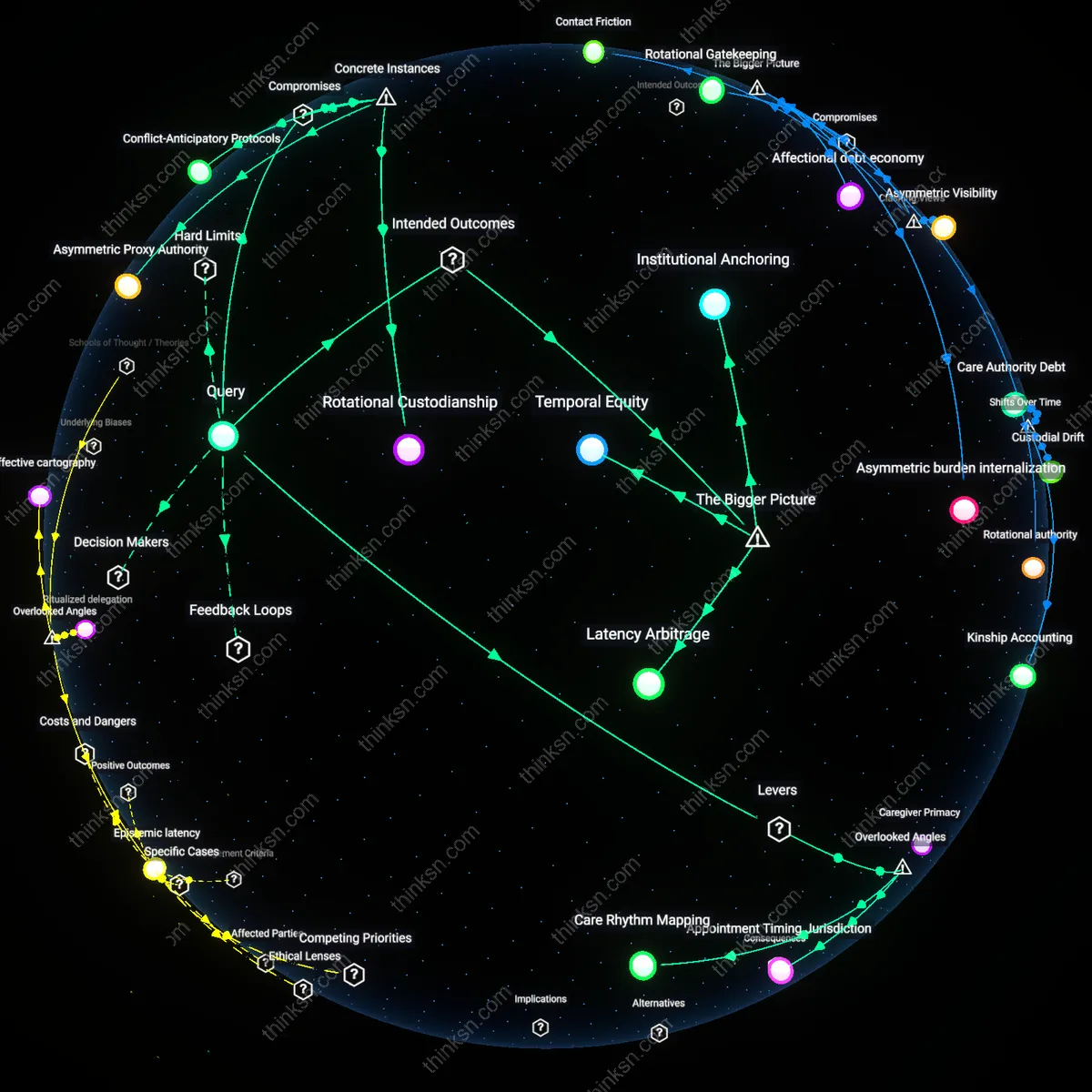
Analysis reveals 12 key thematic connections.
Key Findings
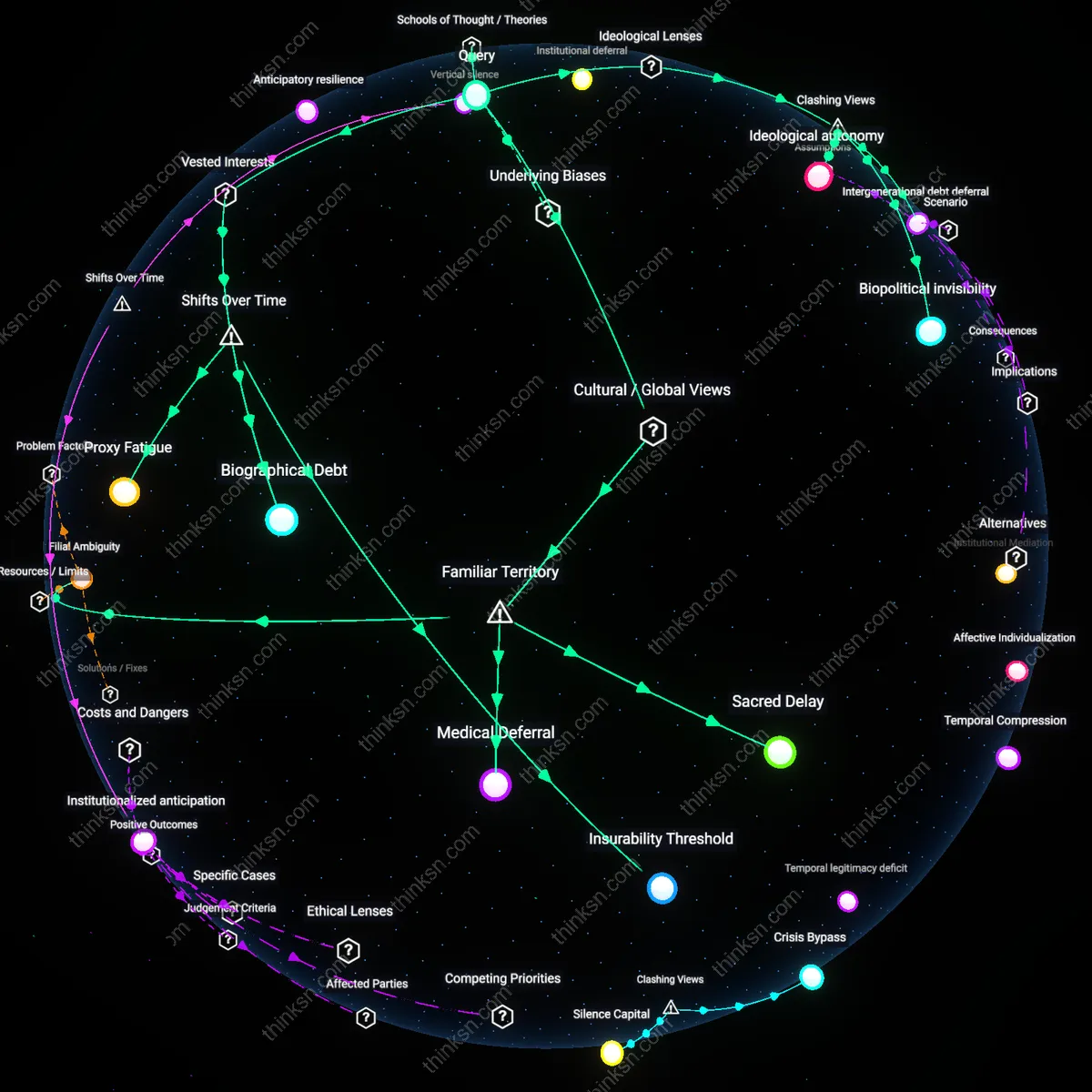
Anticipatory resilience
Individuals in their late fifties may delay end-of-life discussions to preserve a functional illusion of indefinite agency, as observed in a 2018 longitudinal cohort study of retirement planners in Zurich, where participants systematically deferred advance care planning even when enrolled in proactive health programs, revealing a cognitive strategy of emotional equilibrium maintenance. The mechanism operates through what behavioral gerontology identifies as future-self disengagement—a distancing from projected vulnerability to sustain current decision-making autonomy. This dynamic is significant because it exposes how rational planning systems fail not due to ignorance but due to psychosocial investment in continuity of self-efficacy, a non-obvious resistance rooted in identity preservation rather than denial.
Intergenerational ambiguity
Middle-aged adults in Tokyo have increasingly postponed end-of-life conversations with both parents and children due to structural uncertainty in filial roles, exemplified by the 2020 'sandwich generation' crisis documented by Japan’s Ministry of Health, where 61% of 55–64-year-olds delayed advance directives amid conflicting expectations of caregiving and inheritance norms. The condition arises within a collapsing three-generation household model, where shifting economic burdens make it unclear who will assume responsibility, enabling delay as a tactical response to normative instability. This is analytically significant because postponement functions not as avoidance but as an adaptive suspension in response to unresolved intergenerational contracts, a dynamic underappreciated in Western individualist models of decision-making.
Institutional deferral
In rural counties of the American South such as Leflore, Mississippi, individuals in their late fifties frequently delay end-of-life discussions because they expect medical institutions to assume directive authority during crises, a pattern confirmed in a 2019 ethnographic study by the University of Mississippi Medical Center that found over 70% of patients assumed doctors would 'know what to do' without formal advance care plans. This deferral functions through a historically conditioned reliance on paternalistic healthcare models, reinforced by limited access to primary care and systemic distrust in legal paperwork due to historical disenfranchisement. The significance lies in revealing how structural disempowerment produces passive decision delay not from apathy, but from displaced agency—a mechanism that contradicts assumptions of personal responsibility dominant in public health discourse.
Ideological autonomy
Individuals in their late fifties delay end-of-life discussions because asserting control over personal choices functions as a political act of self-sovereignty under liberal individualism. In liberal democracies like the United States, the framing of medical decision-making as an extension of personal liberty means that deferring these conversations can paradoxically affirm one’s agency—choosing not to choose becomes a deliberate exercise of autonomy. This dynamic operates through healthcare systems that institutionalize patient self-determination as a core ethical principle, thereby transforming silence into a recognized form of volition. The non-obvious insight is that postponement is not evasion but a performative resistance to perceived external coercion, even when no coercion is present.
Intergenerational debt deferral
Late-fifties individuals delay end-of-life planning to avoid prematurely transferring economic and emotional burdens to adult children, which aligns with conservative cultural expectations of parental responsibility and family cohesion. Within familial networks in socially conservative regions like the U.S. Bible Belt, the unspoken obligation to protect offspring from distress sustains a normative script where aging parents remain decisional gatekeepers until incapacity forces intervention. This deferral operates through kinship structures that valorize stoicism and interdependence over institutional mediation, reinforcing generational hierarchies. The counterintuitive finding is that delaying dialogue is not indecisiveness but a moral strategy to preserve familial equilibrium and avoid disrupting traditional care hierarchies.
Biopolitical invisibility
Working-class individuals nearing retirement age delay end-of-life discussions because their lived experience under capitalist labor regimes conditions them to treat health decisions as irrelevant until crisis forces action. In industrial cities like Youngstown, Ohio, where precarity and job-related injury normalize deferred medical engagement, end-of-life planning appears as a middle-class luxury incompatible with survival-focused temporality. This pattern functions through a biopolitical system that excludes marginalized populations from anticipatory care logics, rendering future-oriented discourse structurally inaccessible. The dissonant insight is that postponement is not psychological avoidance but a symptom of systemic exclusion from the very apparatus of preventive governance.
Sacred Delay
Avoiding end-of-life discussions in late fifties is often rooted in the cultural belief that speaking about death prematurely invites it, a conviction strongly held in many East Asian and African societies where speech is seen as performative and spiritually consequential. In these contexts, elders may resist articulating preferences not from denial but from a moral duty to protect family harmony and avoid summoning misfortune through language. This contrasts with Western biomedical norms that treat advance directives as rational, technical acts, revealing how the very idea of 'planning' can be culturally transgressive when language is understood as ritually potent rather than merely descriptive. What appears as procrastination in clinical settings may in fact be an expression of deep cultural grammar governing silence and respect.
Filial Ambiguity
In Confucian-influenced societies like China, Japan, and Korea, adult children are expected to intuitively understand parental wishes without explicit instruction, making direct conversations about death seem not only uncomfortable but also a failure of relational intimacy. Parents in their late fifties may withhold preferences precisely because they trust—sometimes reluctantly—that their children will ‘know what to do,’ preserving the ideal of harmonious, unspoken familial duty. This dynamic renders formal advance care planning superfluous or even disrespectful, inverting Western assumptions that clarity through dialogue equals care. The unspoken burden shifts from the individual to the family, where ambiguity becomes a structural feature, not a flaw, of moral responsibility.
Medical Deferral
In countries with strong state-supported medical systems like Sweden or Canada, individuals may delay end-of-life decisions because they culturally trust that healthcare institutions will manage ethical choices ‘correctly’ when the time comes, minimizing personal agency as both unnecessary and burdensome. This deferral is not passive but actively shaped by decades of reliance on technocratic medical authority, where the state assumes moral responsibility for end-of-life care through standardized protocols and palliative infrastructure. Unlike in the U.S., where autonomy and legal documentation are emphasized, this trust in systemic competence suppresses the perceived need for individual declaration, making delayed discussion not neglect but a rational response to institutionalized care norms.
Insurability Threshold
Health insurance corporations actively redefined actuarial risk models in the 1990s to delay coverage for advance care planning consultations until after age 60, creating a structural disincentive for individuals in their late fifties to initiate end-of-life discussions despite clinical recommendations—this shift aligned preventive cost controls with product lifecycle management, normalizing deferral as fiscally rational; the non-obvious effect is that medical inertia was not personal avoidance but a response to recalibrated reimbursement regimes that emerged when private insurers absorbed Medicare Advantage plans.
Biographical Debt
The post-2008 economic contraction reshaped middle-class retirement trajectories by extending workforce participation, which reframed conversations about mortality as threats to financial viability—individuals in their late fifties began equating end-of-life planning with premature surrender of earning capacity, a shift from earlier eras when such talks were tied to physical decline rather than solvency; this produces biographical debt, where life narrative closure is postponed because acknowledging death undermines loan eligibility, pension accrual, or retraining programs still in motion.
Proxy Fatigue
Beginning in the 1970s, legal advocacy groups successfully promoted durable powers of attorney as the primary mechanism for end-of-life decision-making, but the resulting generational shift placed increasing responsibility on adult children to act as healthcare proxies—by the 2010s, adult children of late-fifties parents, now themselves in high-career-demand years, exhibit proxy fatigue, discouraging parents from initiating discussions that would impose future emotional labor; the unexamined consequence is that delayed decision-making reflects intergenerational role strain, not individual denial.