When Cultural Practices Clash with Medical Advice at End of Life
Analysis reveals 5 key thematic connections.
Key Findings
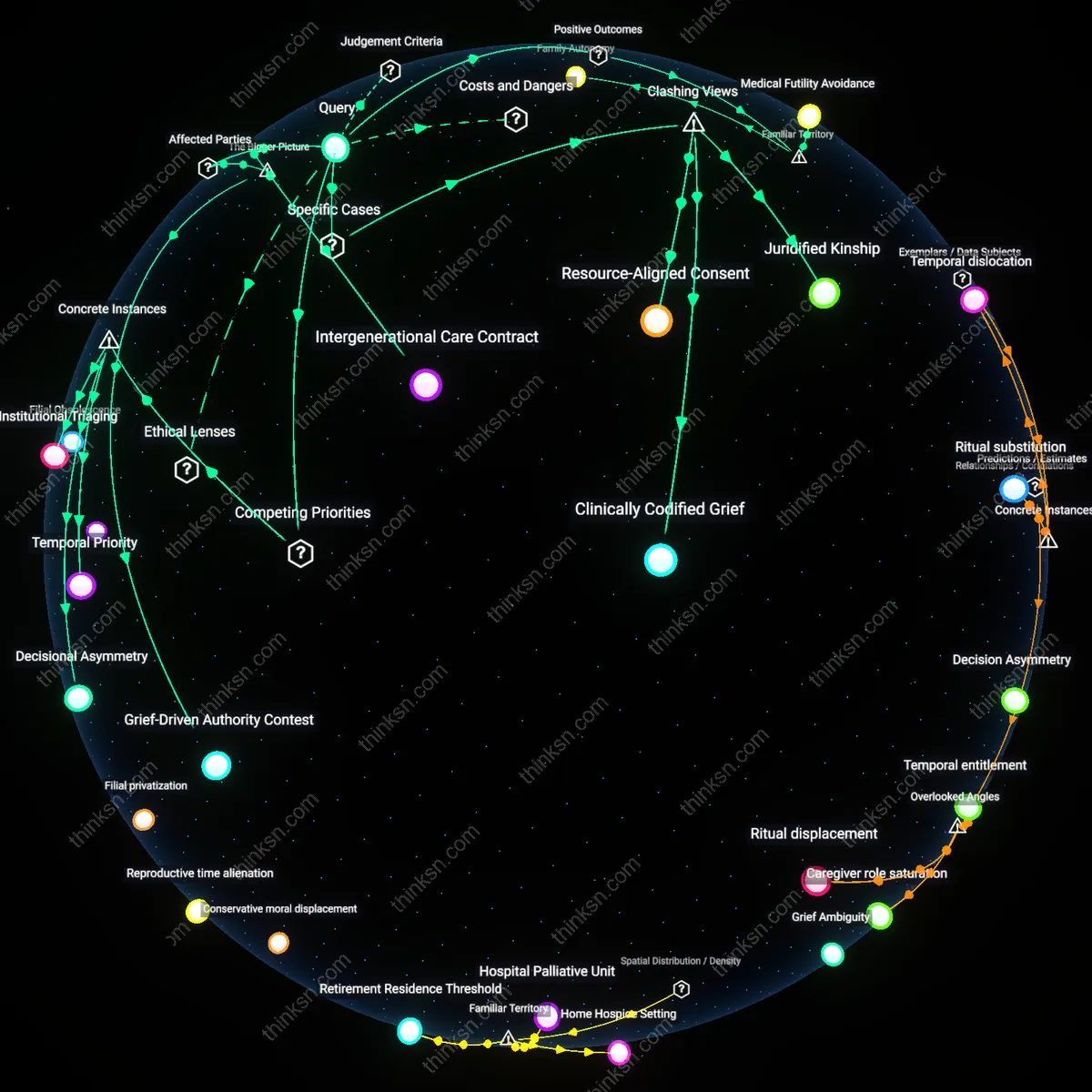
Intergenerational Care Contract
A caregiver should prioritize maintaining relational continuity with the elder by embedding medical recommendations within culturally resonant frameworks, because the success of end-of-life compliance hinges on the pre-existing emotional ledger between caregiver and parent, which functions as a hidden compliance currency in clinical settings. Systems of familial trust—built over decades of reciprocated care, unspoken obligations, and symbolic acts like food sharing or ritual observance—are what ultimately determine whether a parent accepts palliative referrals or resists resuscitation orders, and these are modulated not by medical persuasion alone but by whether clinical advice is framed to honor ancestral obligations. The trigger is not clinical efficacy but perceived respect for filial identity, revealing that medicine becomes actionable only when it is ritually legitimized. The overlooked mechanism is that caregivers operate as cultural translators, not merely medical executors, whose credibility depends on balancing institutional mandates with dynastic duty.
Biopower Allocation Regime
Caregivers navigate end-of-life decisions within an asymmetric biopower structure where institutional actors—hospice administrators, nonprofit insurers, and federally regulated hospitals—pre-select allowable care modalities by controlling reimbursement and drug access, thus shaping what cultural accommodations are logistically feasible. A framework must therefore account for how Medicare’s palliative care codes or Medicaid’s home health stipulations create financial thresholds that de facto exclude certain spiritual practices—such as extended vigils, non-Western herbal adjuncts, or ceremonial gatherings—by refusing to cover staffing or space beyond clinical protocols, making economic eligibility the hidden arbiter of cultural survival. The causal force lies in how third-party payers act as silent veto players, reframing ethical dilemmas as budget compliance exercises. The underappreciated reality is that cultural mediation often fails not from family resistance but from pre-emptive market exclusion enforced through coded billing structures.
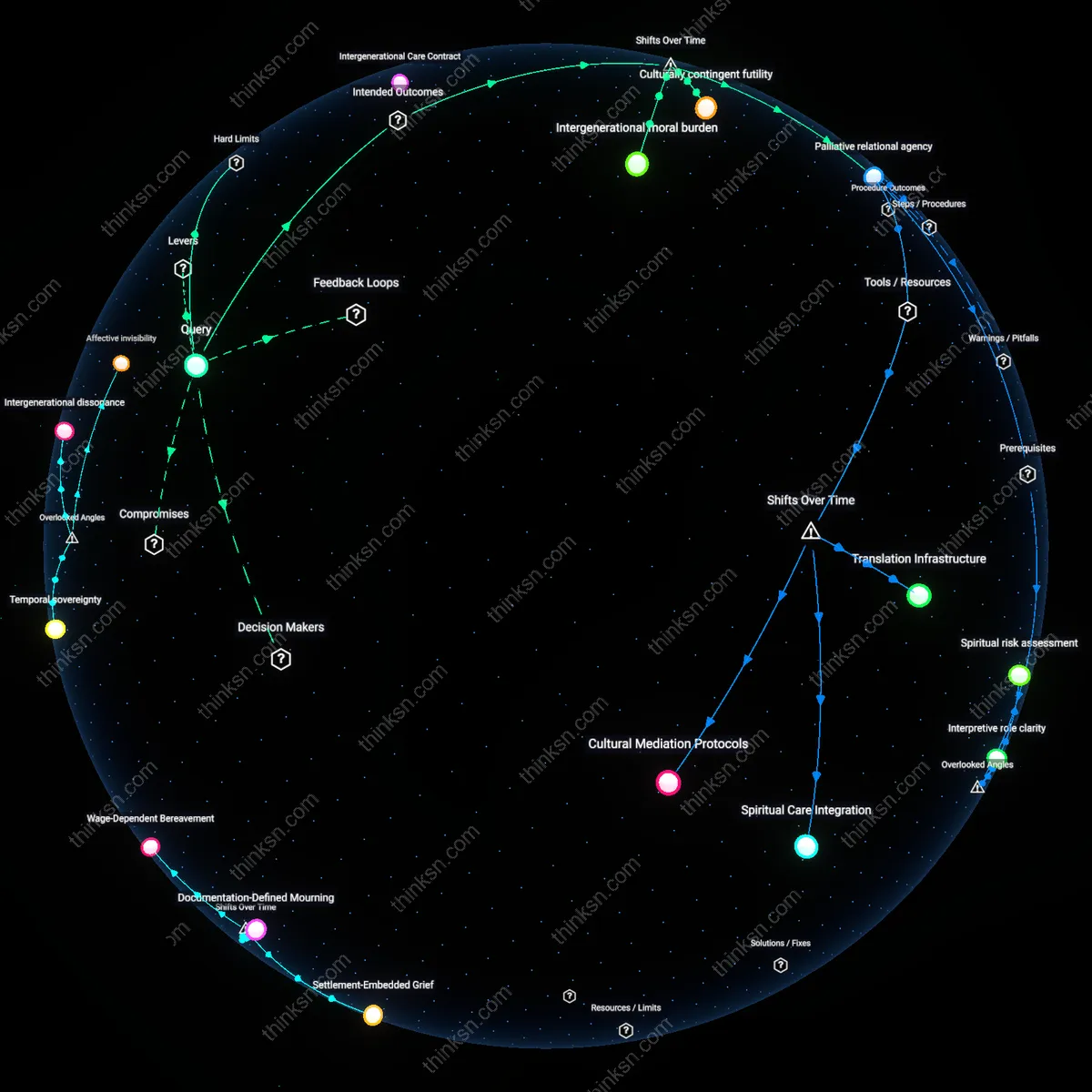
Culturally contingent futility
A caregiver should prioritize a framework that negotiates medical futility through the evolving historical context of multiculturalism in clinical ethics, which shifted decisively in the 1990s with the institutionalization of cultural competence training in U.S. medical education. This mechanism embeds cultural interpretation as part of clinical judgment, transforming previously pathologized practices—like withholding resuscitation due to spiritual beliefs—into legitimate expressions of patient autonomy, thereby redefining 'futility' not as a purely biomedical endpoint but as a culturally negotiated outcome. The significance lies in how this reframing reveals that medical futility is not a fixed threshold but historically contingent on the medical system’s willingness to recognize cultural difference as ethically relevant, a transition marked by accreditation mandates from bodies like the ACGME.
Intergenerational moral burden
A caregiver should use a framework shaped by the shift from communal to individualized end-of-life decision-making that emerged in post-1970s Western societies, particularly after the rise of advance directives and patient autonomy doctrines. This transition displaced elder-centered familial consensus onto younger generations who now bear the responsibility of interpreting both medical advice and inherited cultural norms, creating a new moral burden where the caregiver must reconcile parental expectations with institutional protocols. The underappreciated effect is that this shift has turned the caregiver into a de facto moral translator—not just between languages, but between historical eras of medical authority and kinship obligation—thereby producing the family, rather than the clinic, as the primary site of ethical conflict resolution.
Palliative relational agency
A caregiver should adopt a framework that recognizes palliative care's transformation after the 2000s, when it evolved from symptom management to a relational practice integrated within diverse cultural economies of care, particularly in urban hospitals serving immigrant populations. This shift institutionalized chaplains, interpreters, and cultural navigators as co-agents in care planning, enabling interventions that align hospice protocols with culturally specific rituals around dying, such as post-mortem washing or deathbed blessings. The non-obvious insight is that medical legitimacy is no longer monopolized by clinical guidelines but co-produced through sustained interaction between providers and families, revealing palliative care not as a medical service but as a negotiated field of relational agency that emerged from decades of policy experimentation and community health advocacy.