Do Generic Drugs Save Money or Sacrifice Choice?
Analysis reveals 12 key thematic connections.
Key Findings
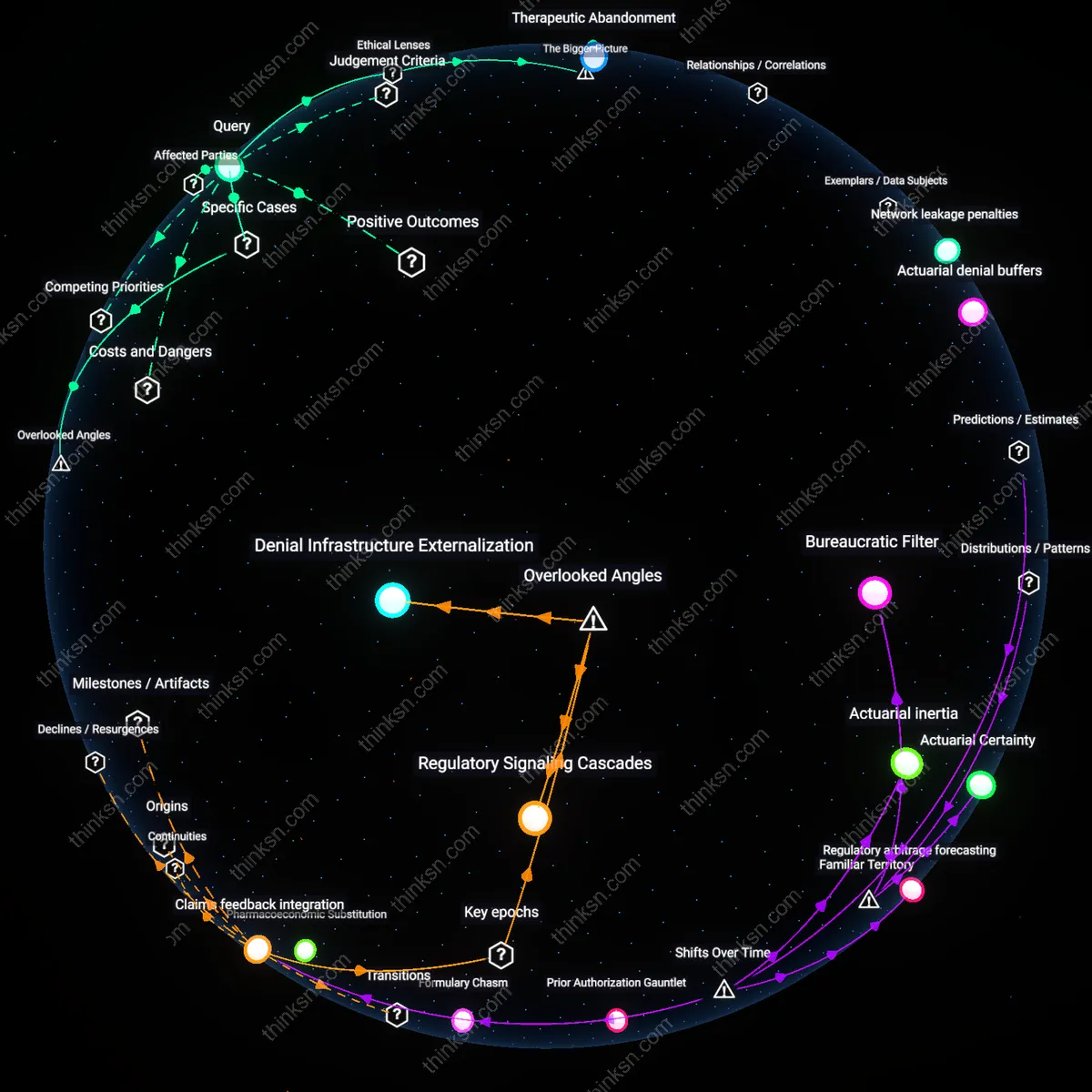
Fiscal Accountability Norms
Mandatory generic substitution enhances public health system sustainability by institutionalizing fiscal accountability norms within state pharmacy benefit frameworks. State Medicaid programs, facing fixed budgets and cost-reimbursement models, leverage mandatory substitution laws to redirect savings into expanded care access, creating a systemic feedback loop where prudent spending enables broader coverage. This mechanism is non-obvious because it reframes cost control not as a constraint on autonomy but as a collective enabler of care scalability, driven by budgetary predictability and administrative standardization across large patient populations.
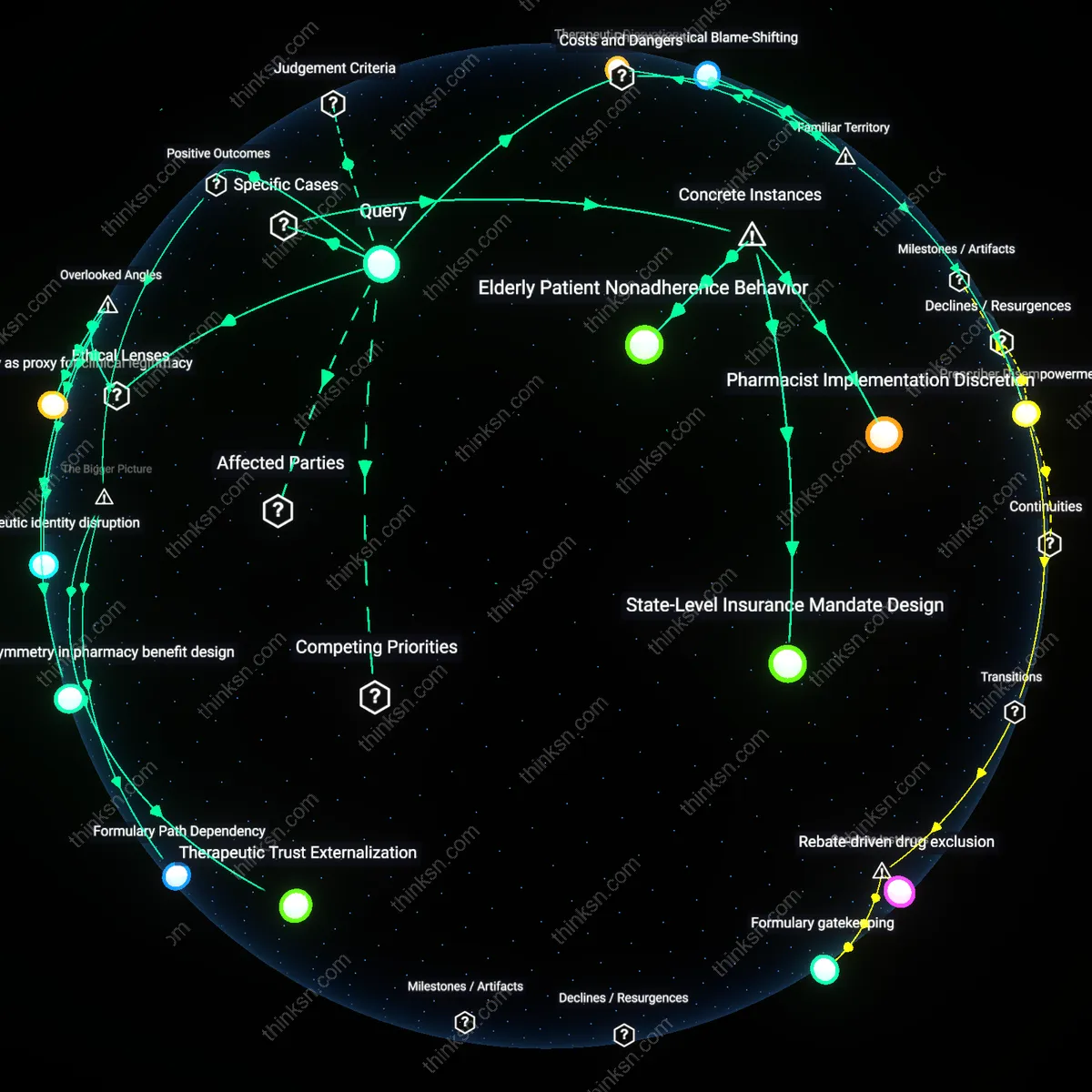
Therapeutic Trust Externalization
Physician and patient acceptance of generic substitution depends on the externalization of therapeutic trust to federal regulatory benchmarks, particularly FDA bioequivalence standards. When prescribers and consumers defer to the FDA's scientific validation process, clinical autonomy becomes decoupled from brand choice, allowing cost containment to proceed without direct conflict. The non-obvious insight is that trust in a centralized regulatory actor—specifically the FDA’s methodological rigor—functions as a social scaffold that aligns economic policy with clinical legitimacy, enabling systemic cost reduction without destabilizing the care relationship.
Formulary Path Dependency
Mandatory generic substitution reinforces formulary path dependency in private and public insurers, where initial cost-based drug selection shapes long-term prescribing trajectories and patient expectations. Insurers, leveraging pharmacy benefit managers (PBMs), create economic incentives that make brand-name prescriptions increasingly exceptional, thereby normalizing generics as the default standard of care. The underappreciated dynamic is that early policy-driven cost containment embeds itself into prescribing infrastructure and insurance design, making reversal politically and economically costly even if individual patient autonomy is notionally compromised.
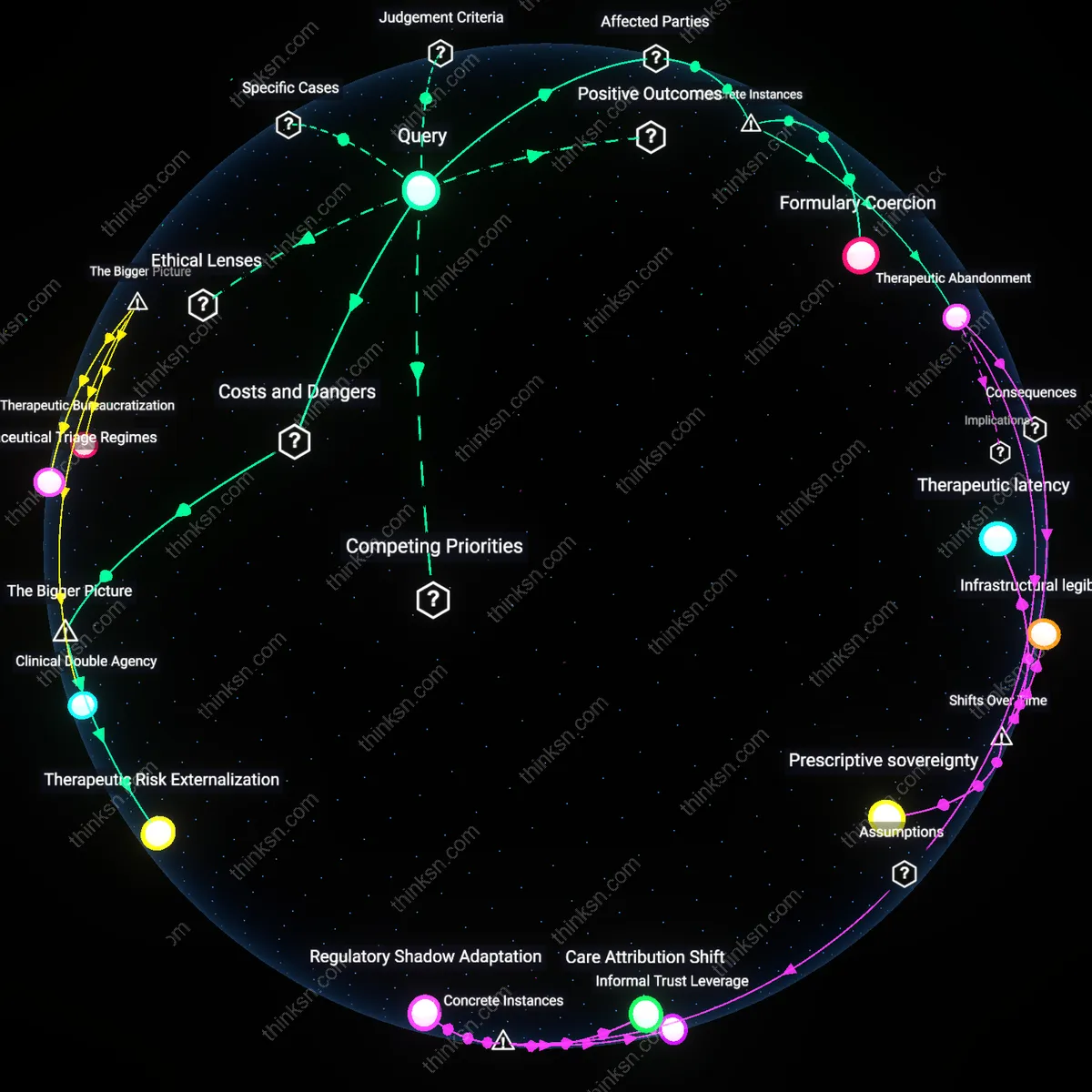
Therapeutic Disruption
Mandatory generic substitution undermines patient trust when visible changes in pill appearance cause confusion and non-adherence. Pharmacists and insurers prioritize bioequivalence standards endorsed by the FDA, but patients associate pill color, shape, and imprint with specific effects, leading some to question whether substitutions are safe or effective—even when chemically equivalent. This mismatch between regulatory metrics and sensory familiarity introduces risk of missed doses or self-discontinued therapy, especially among elderly or mentally ill populations who rely on visual cues, revealing how cost-saving protocols can destabilize the implicit contracts sustaining treatment adherence.
Pharmaceutical Blame-Shifting
When adverse effects occur after a mandatory generic switch, patients and physicians often target the manufacturer of the generic version, not the prescriber or insurer enforcing substitution. Despite identical active ingredients, the branding hierarchy—where innovator drugs are culturally associated with quality and generics with compromise—channels suspicion toward low-cost producers, exposing a liability asymmetry where generic firms absorb reputational harm despite lacking control over the substitution decision. This distorts market accountability and discourages investment in quality manufacturing, as safety perceptions hinge less on performance than on socioeconomic visibility.
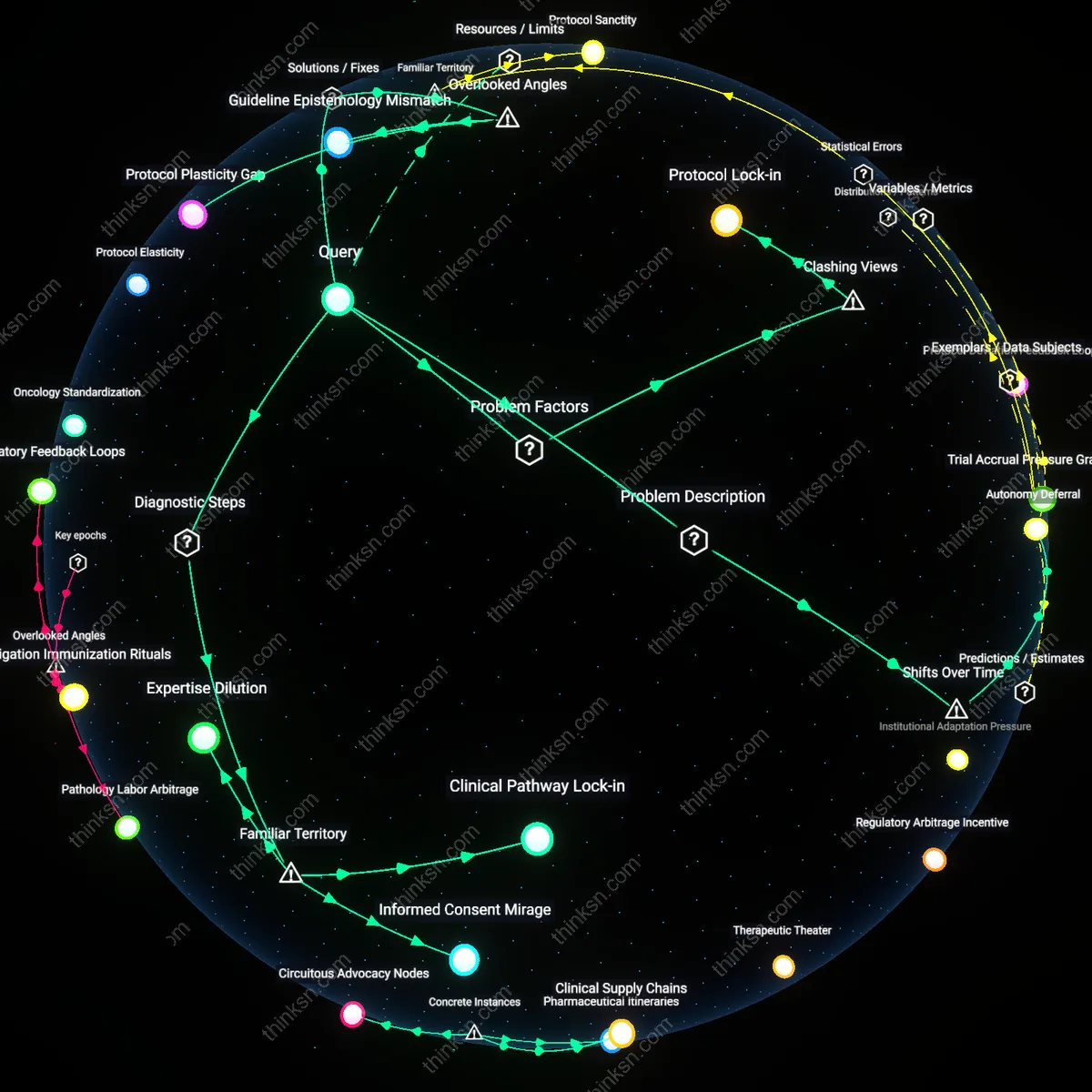
Prescriber Disempowerment
Mandatory substitution laws erode the clinical authority of physicians by removing their final say in medication formulation, transferring decision power to pharmacy benefit managers and state formularies. Even when a doctor specifies 'dispense as written' due to patient sensitivity or prior failure on a generic, pharmacists may override based on payer incentives, creating therapeutic conflicts the provider cannot control. This undermines the perception of medical expertise in treatment individualization, turning the prescription into a negotiable financial document rather than a clinical directive, and weakening the doctor-patient alliance at the moment of care delivery.
Epistemic asymmetry in pharmacy benefit design
Mandatory generic substitution laws undermine patient autonomy not through direct coercion but by entrenching an epistemic asymmetry that favors payer-driven formulary governance over individualized clinical judgment. Pharmacy benefit managers (PBMs), operating under opaque pricing contracts and tiered formularies, leverage cost containment mandates to restrict access to branded versions even when patients and prescribers jointly prefer them for legitimate clinical or psychological reasons, such as perceived efficacy or placebo-level adherence effects. This mechanism is structurally reinforced by Medicare Part D and private insurance protocols that financially penalize deviation from generics, effectively making knowledge about drug equivalence a privileged administrative calculation rather than a shared decision-making domain. The overlooked dynamic is that autonomy is compromised not by the substitution itself, but by the systematic exclusion of patient epistemic claims—like embodied experience or trust in brand—from countering the actuarial epistemology that dominates formulary logic.
Therapeutic identity disruption
Cost containment policies that mandate generic substitution risk destabilizing patients’ therapeutic identity—the internalized sense of self in relation to a specific drug regimen—particularly among chronic disease populations who associate their health stability with a named pharmaceutical entity. For conditions like epilepsy or bipolar disorder, where subjective continuity matters for adherence and perceived control, switching formulations—even bioequivalent ones—can trigger nocebo effects or disengagement, a phenomenon documented in ethnographic studies of patient support groups but ignored in pharmacoeconomic models. The conflict with autonomy arises not from informed refusal but from the silent erosion of self-efficacy when institutional actors (e.g., state pharmacy boards enforcing substitution laws) dismiss patient-reported disruptions as irrational. This angle reveals that autonomy is not just about choice at the point of dispensing, but about the continuity of a person’s medical self-narrative, which generic mandates destabilize in ways invisible to outcomes-based policy metrics.
Brand loyalty as proxy for clinical legitimacy
Patients and physicians sometimes treat brand-name drugs as proxies for clinical legitimacy, not due to misinformation alone, but because the brand serves as a tangible anchor in a healthcare system where trust is diffusely distributed across invisible supply chains and outsourcing networks. Mandatory generic substitution disrupts this symbolic signaling mechanism, particularly in communities with historical medical exploitation (e.g., Black or rural populations), where the brand-name drug may represent a rare visible node of perceived accountability. Cost containment undermines autonomy not merely by limiting options, but by erasing a socially constructed safeguard patients use to navigate systemic opacity—something not captured in standard bioethics frameworks that assume drug equivalence translates directly to experiential equivalence. The residual conflict lies in how generic mandates flatten heterogeneous trust economies into uniform cost metrics, failing to recognize brand loyalty as an adaptive response to institutional illegibility rather than a cognitive bias to be corrected.
Pharmacist Implementation Discretion
In Michigan’s 2008 generic substitution reform, pharmacists gained legal authority to substitute generics unless explicitly prohibited by prescribers, creating a frontline conflict where cost-saving mandates clashed with unspoken patient preferences—pharmacists became de facto arbiters of therapeutic trust, often unaware of patients’ prior negative experiences with generic formulations. This mechanism reveals how cost-containment policy delegates ethical burden to intermediaries who lack tools to assess patient autonomy, making substitution an act of administrative efficiency rather than informed choice.
State-Level Insurance Mandate Design
California’s Medi-Cal program requires mandatory generic substitution unless a prescriber submits a prior authorization for a brand-name drug, directly tying cost containment to bureaucratic friction—patients seeking brand-name drugs for perceived efficacy must navigate delays and documentation, effectively discouraging autonomy unless the physician invests additional labor. This shows how cost-saving structures are operationalized through procedural deterrence rather than clinical dialogue.
Elderly Patient Nonadherence Behavior
In a documented pattern within Medicare Part D populations in Florida, older adults discontinued cardiovascular generics after substitution due to distrust in appearance changes or anecdotal side effects, leading to higher readmission rates—despite cost savings, the autonomy conflict manifests not at the point of substitution but in downstream adherence breakdowns. This reveals that the tension between cost and autonomy is not resolved at dispensing but deferred into clinical outcomes.