Navigating Medication Anxiety: Pediatric Conflicts and Insurance Limits?
Analysis reveals 12 key thematic connections.
Key Findings
Prescription Churn
A parent should track and document the frequency and rationale of medication changes over time to identify patterns of iatrogenic escalation driven by fragmented provider incentives. When pediatric psychiatrists, neurologists, and primary care physicians operate in silos with misaligned reimbursement triggers — such as brief follow-up visits favoring dose adjustments over behavioral interventions — the child’s treatment plan becomes subject to prescription churn, a cycle where medications are added or substituted not solely for clinical reasons but due to structural time and billing constraints. This creates an underrecognized form of treatment drift where anxiety symptoms are inadvertently amplified by metabolic load and discontinuation effects, yet remain coded as 'treatment-resistant.' Most analyses overlook how the tempo of prescription decisions — rather than their content — generates cumulative harm, making temporal mapping a critical diagnostic tool.
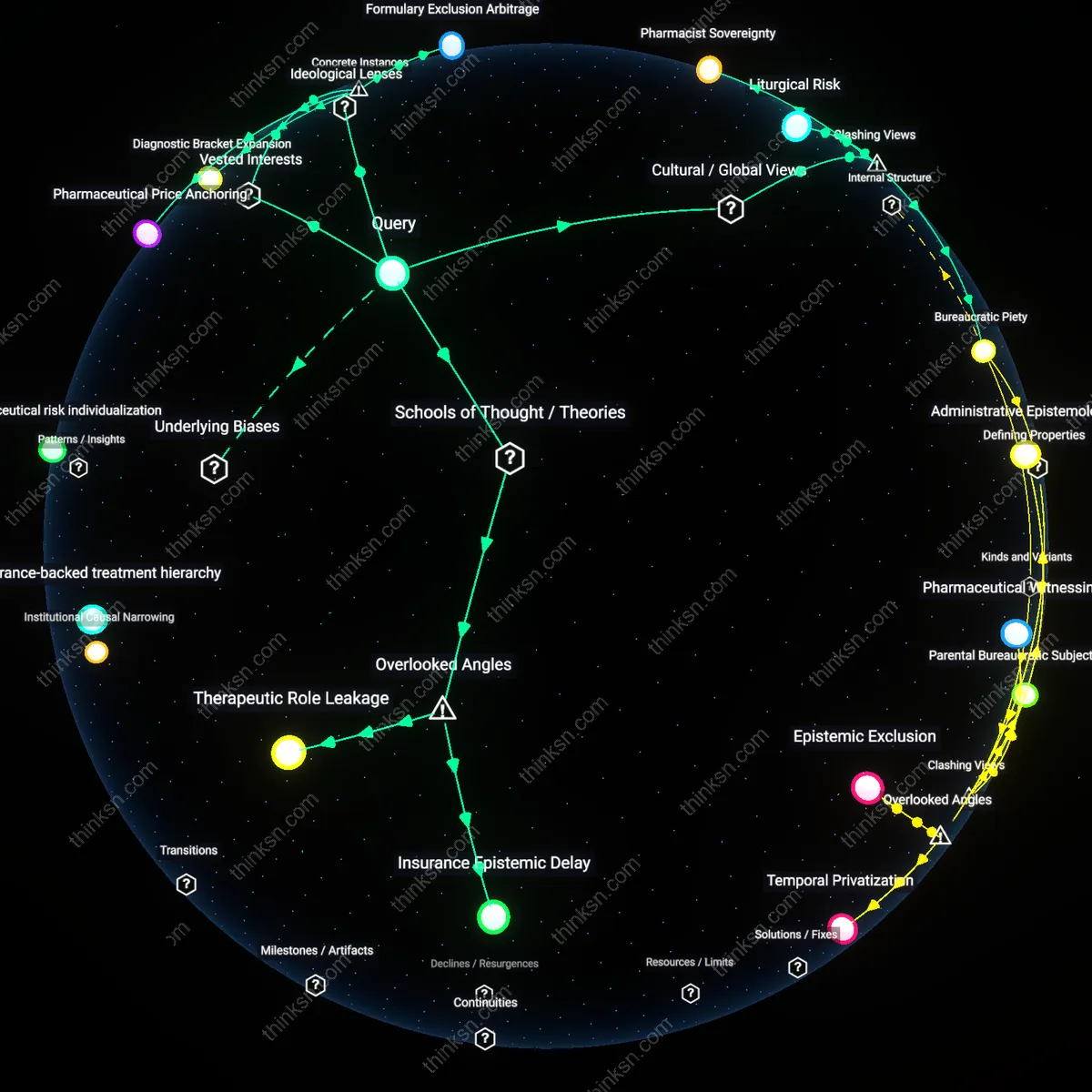
Insurance Epistemic Delay
A parent should treat insurance preauthorization timelines as a clinical variable that actively shapes the trajectory of anxiety expression and medication response. Delays in approving evidence-based medications force reliance on immediately accessible but suboptimal alternatives, which over time condition the child’s neurochemistry to a cascade of partial responses and withdrawal spikes, thereby distorting the clinical picture professionals use to assess medication efficacy. The overlooked dynamic is that insurance administrative rhythm — measured in business days for prior authorization decisions — operates slower than neurodevelopmental response cycles, creating an epistemic delay where the data clinicians interpret are artifacts of access bottlenecks rather than biological patterns. This makes the insurance back-end not just a financial barrier but a constitutive element of the diagnostic process itself.
Therapeutic Role Leakage
A parent should actively redefine their role as a boundary maintainer between professional domains to prevent therapeutic role leakage, where pediatricians assume behavioral monitoring duties beyond their capacity and therapists avoid pharmacological literacy, leaving the parent to synthesize incoherent narratives without institutional support. When insurance restricts access to integrated care models like pediatric psychopharmacology clinics, the responsibility for clinical synthesis defaults to the parent despite no formal training, transforming them into an uncredited cognitive broker. The overlooked mechanism is that fragmented payment structures induce role drift among providers, each narrowing their focus to billable tasks, which in turn increases the child’s exposure to contradictory advice. Recognizing this reframes parental advocacy not as emotional labor but as an essential regulatory function within a broken coordination infrastructure.
Insurance-backed treatment hierarchy
Parents should adhere to the medication protocol approved by their insurer because the alignment of pharmaceutical reimbursement with clinical guidelines creates a de facto standard of care that marginalizes alternative therapies—this occurs through integrated networks of pharmacy benefit managers, formulary design, and provider incentives that prioritize cost-containment over symptom nuance, privileging measurable outcomes like medication adherence over subjective anxiety fluctuations. This structure renders patient-specific contradictions in treatment effects invisible unless they escalate to crisis levels, revealing how financial logistics in managed care systems actively shape diagnostic interpretation and therapeutic escalation.
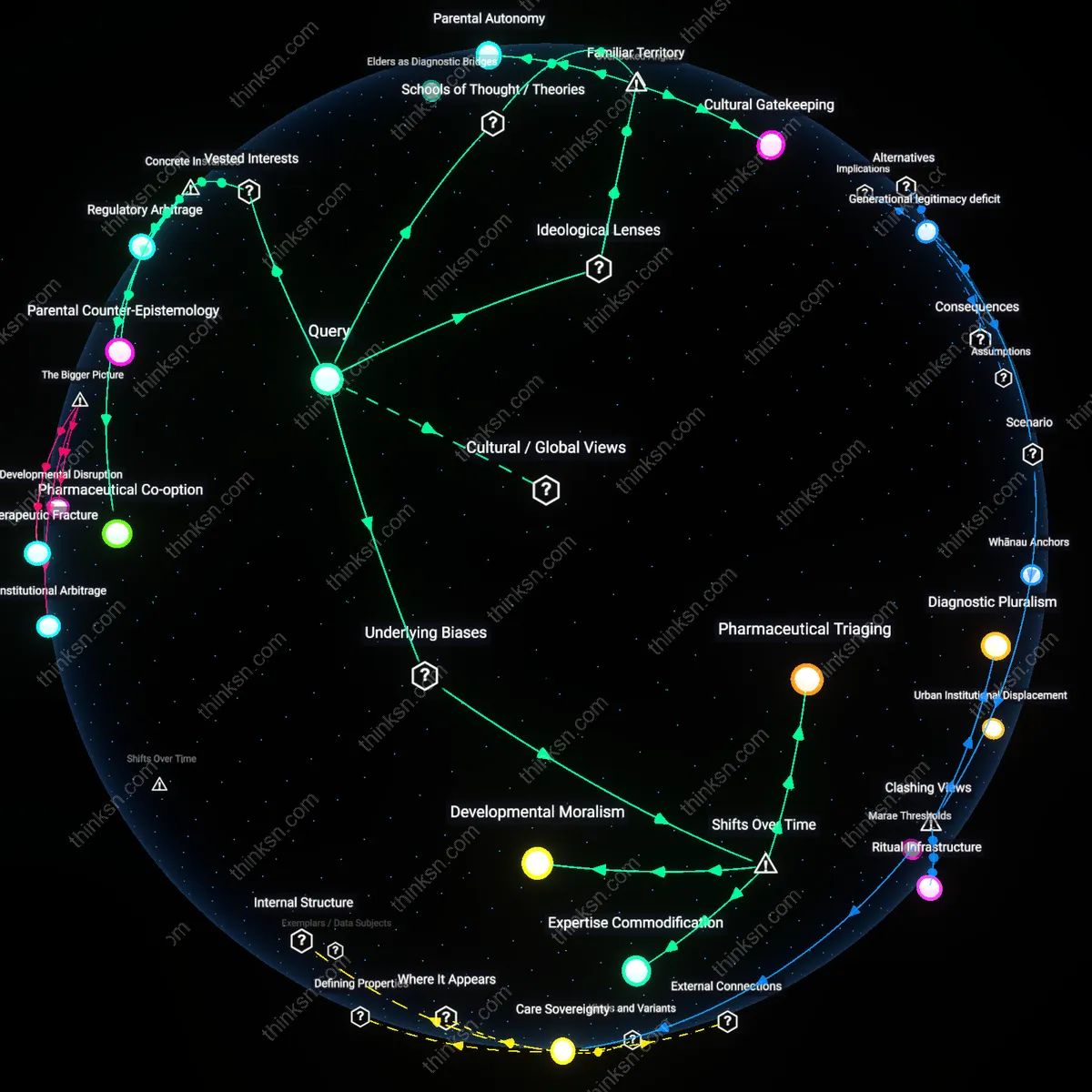
Clinician autonomy under regulatory insulation
Parents should defer to clinicians who practice outside consensus guidelines when such providers leverage professional discretion to prescribe off-formulary medications, as the legal and institutional protection of medical judgment enables a bypass of insurance constraints through mechanisms like prior authorization appeals or compassionate use designations—this occurs most effectively in academic medical centers or federally qualified health clinics where revenue streams are partially decoupled from private payer demands, exposing how fragmented healthcare governance creates uneven pockets of clinical freedom that replicate access along institutional rather than medical need lines.
Pharmaceutical risk individualization
Parents should document and report medication-induced anxiety as a personalized adverse event to shift responsibility from family decision-making to regulatory surveillance systems, because the post-marketing pharmacovigilance model depends on patient-level reporting to recalibrate drug safety profiles over time—this mechanism, operated through the FDA’s MedWatch program and insurer-mandated quality metrics, converts isolated cases into systemic risk data only after threshold accumulation, demonstrating how the deferral of treatment accountability to retrospective, population-level monitoring depoliticizes acute care dilemmas and frames medication harms as emergent rather than structurally foreseeable.
Pharmacist Sovereignty
Parents in rural Punjab resolve conflicting psychiatric advice about medication-induced anxiety by deferring to village pharmacists over clinical specialists, whose recommendations are filtered through kinship networks that prioritize observable behavior over diagnostic categories, thereby making pharmaceutical distribution a localized system of moral authority that contradicts Western medical hierarchy; this mechanism reveals how biomedical individualism fails to account for community-embedded decision-making in South Asian familial structures where treatment adherence depends less on diagnosis accuracy than on social consensus.
Liturgical Risk
In urban Brazil, Pentecostal parents reject insurance-mandated anxiety medication for children not because of cost but because pharmacological intervention is interpreted as surrendering to demonic influence, reframing psychiatric side effects as spiritual warnings; this spiritual risk calculus operates through church-led counseling collectives that displace clinical liability with ritual accountability, challenging the secular assumption that treatment refusal stems from misinformation rather than a competing epistemology of suffering.
Bureaucratic Piety
Japanese middle-class parents comply with contradictory psychiatric recommendations by strictly adhering to insurance protocols not because they trust the state but to perform civic propriety, where submitting forms, attending mandated consultations, and maintaining medication records becomes a ritual of moral motherhood that substitutes therapeutic outcome with procedural virtue; this reveals how bureaucratic compliance functions as a culturally legible form of care, undermining the Western equation of medical advocacy with active treatment resistance.
Pharmaceutical Price Anchoring
A parent should prioritize generic formulations over brand-name medications when managing medication-induced anxiety in children because pharmaceutical companies use formulary placement strategies to steer prescriptions toward higher-cost drugs with greater profitability, as seen when Pfizer leveraged its rebate agreements with UnitedHealthcare in 2018 to keep Vyvanse preferred on the ADHD medication list despite growing clinical reports of anxiety side effects, revealing how list pricing and insurer negotiations silently shape clinical feasibility—this mechanism remains hidden in patient-facing discussions yet directly constrains parental choice, privileging drugs optimized for reimbursement logic rather than symptom compatibility.
Diagnostic Bracket Expansion
A parent should critically assess whether anxiety symptoms are being medically reframed as a separate disorder requiring additional treatment, because advocacy groups such as CHADD (Children and Adults with Attention-Deficit/Hyperactivity Disorder) have historically partnered with pharmaceutical funders to broaden diagnostic criteria for conditions like pediatric anxiety, exemplified in the 2013 DSM-5 revisions where subthreshold anxiety presentations were reclassified as generalized anxiety disorder, thereby justifying adjunctive prescriptions like SSRIs even when initial stimulant-induced anxiety could be managed behaviorally—this shift reflects how definitional authority is mobilized to transform transient side effects into treatable conditions, expanding care pathways that align with therapeutic development pipelines.
Formulary Exclusion Arbitrage
A parent should pursue off-label alternatives when standard treatments provoke anxiety because public insurance programs like Medicaid in Texas apply restrictive prior authorization protocols that selectively exclude costly anxiolytics while fast-tracking stimulants, a policy pattern reinforced during the 2017 Texas Health and Human Services redesign that approved immediate access to amphetamines but required psychiatric review for sertraline in patients under 12, effectively tilting clinical decisions toward initial treatments with known anxiety-inducing effects—this structural preference, justified as cost containment, covertly positions families to accept medication-induced symptoms as unavoidable, normalizing sequential intervention rather than preventive caution.