Patient Control in Pain Management: Autonomy vs Safety?
Analysis reveals 10 key thematic connections.
Key Findings
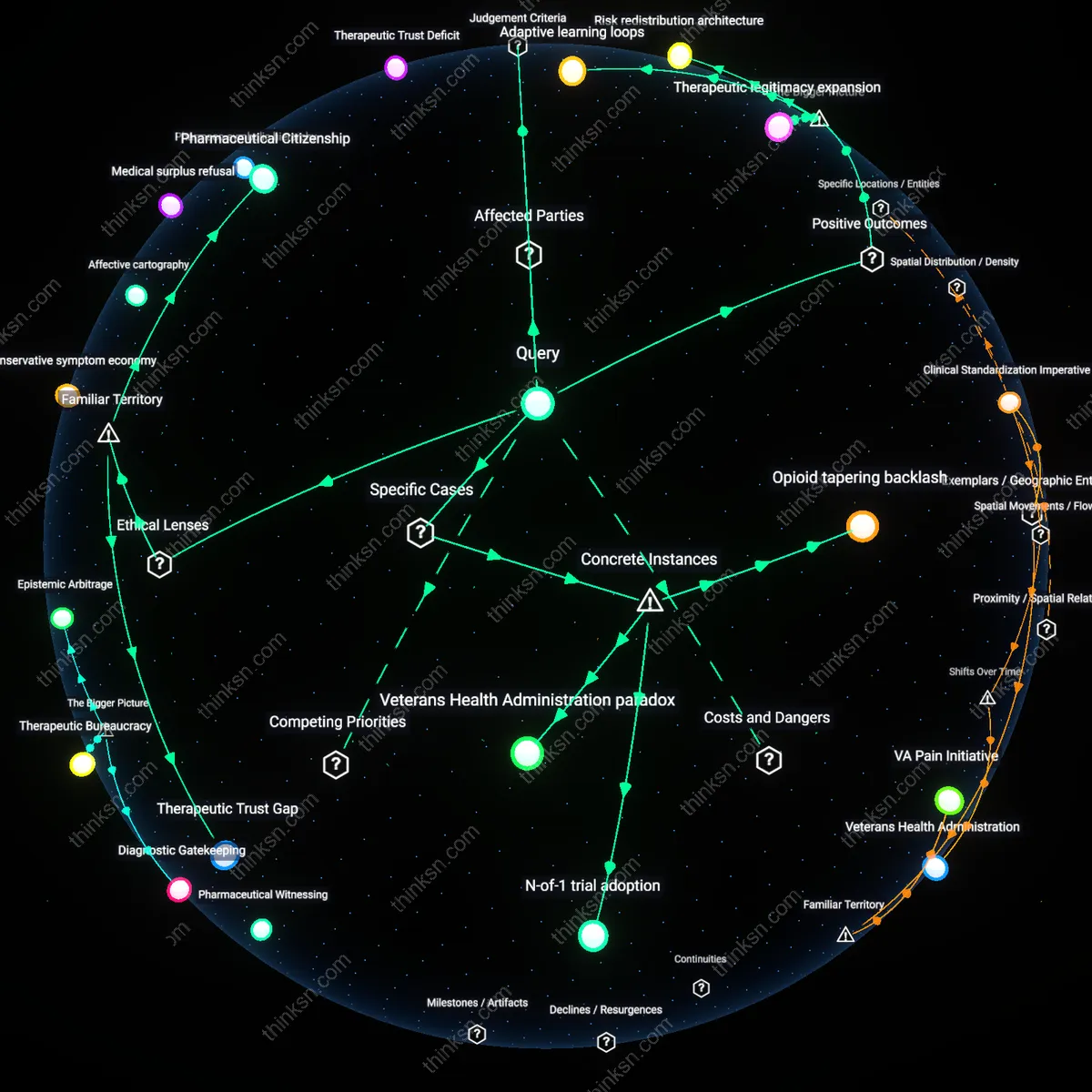
Therapeutic Trust Deficit
Patient-directed dosing reveals that medical safety protocols often function less as neutral safeguards than as institutional expressions of distrust toward patients, particularly those with histories of substance use or mental health conditions. This dynamic plays out in clinical settings where physicians override patient self-reports using opioid risk stratification tools, which embed actuarial assumptions about noncompliance, thereby prioritizing systemic risk-aversion over individual agency. The non-obvious outcome is that autonomy is not simply restricted for safety’s sake but is asymmetrically withdrawn based on prognostic stigma, exposing how clinical judgments codify social biases under the guise of objective medicine.
Pharmaceutical Citizenship
Patient autonomy in dosing is selectively endorsed only when patients perform compliance through precise symptom logging, appointment adherence, and avoidance of ‘red-flag’ behaviors—effectively making responsible self-management a prerequisite for self-direction. This reveals chronic pain management as a conditional social contract where access to autonomy is granted based on the patient’s ability to conform to biomedical norms of legibility and predictability, not clinical need alone. The friction here undermines the assumption that autonomy is a universal right, exposing it instead as a regulated status earned through performative alignment with institutional expectations.
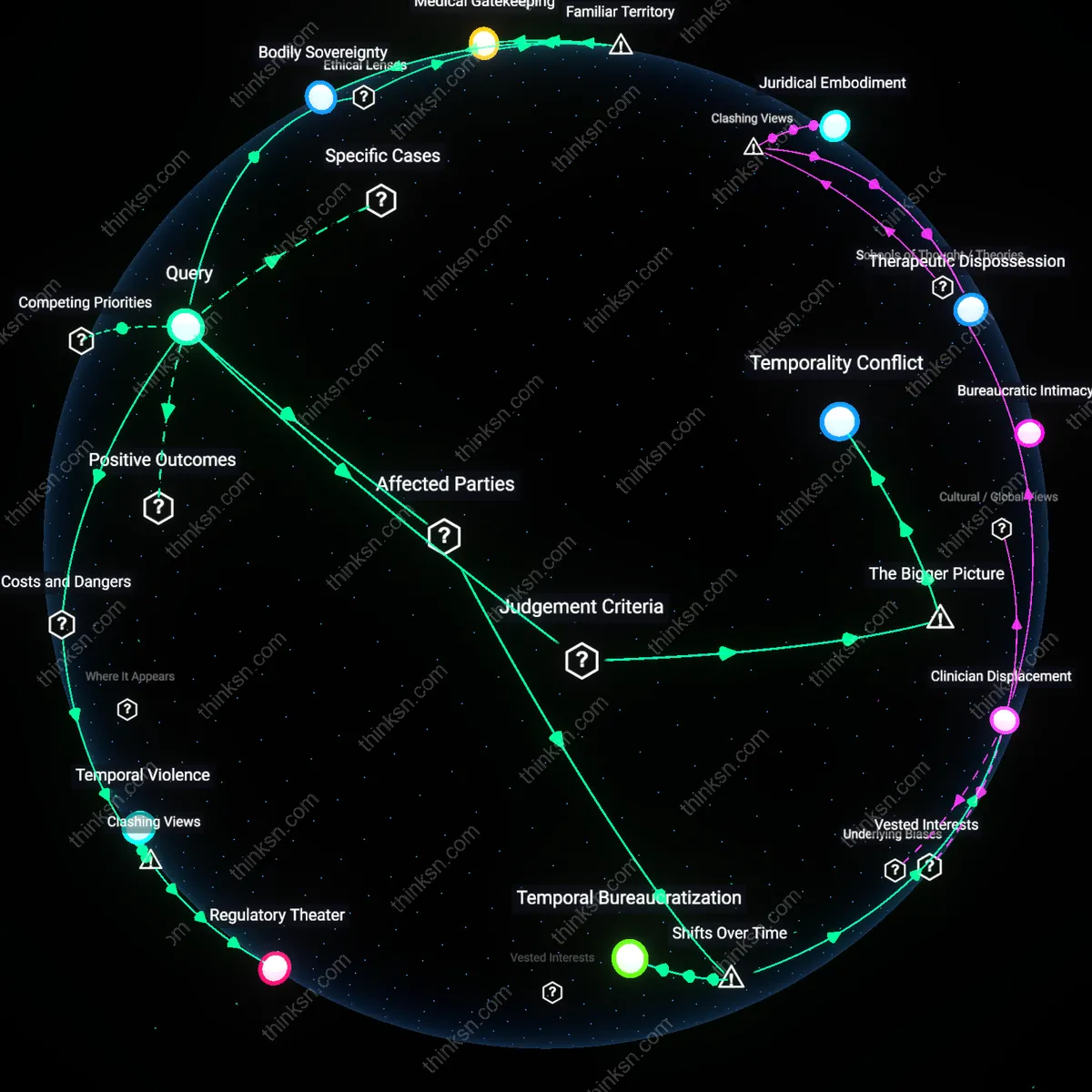
Epistemic Dispossession
When clinicians reject patient-reported pain relief in favor of biomarker thresholds or dosing algorithms, they disqualify experiential knowledge as medically invalid, positioning the body-as-measured over the body-as-lived. This occurs routinely in insurance-mandated pain contracts that cap dosages irrespective of subjective efficacy, privileging third-party data interpretations over first-person narratives. The overlooked consequence is that patient direction is not merely limited by safety concerns but actively unlearned through systems that delegitimize subjective suffering, rendering autonomy not just constrained but epistemologically undermined.
Adaptive learning loops
Patient-directed dosing in chronic pain fosters more rapid individualized treatment adaptation by enabling real-time patient feedback to shape clinical decision-making, which reconfigures the traditional clinician-centered model into a dynamic, bidirectional system of care. This shift is mediated by sustained patient-clinician communication and supported by digital health tracking tools, which allow both parties to observe patterns in symptom response and side effects over time. The mechanism works because patients become active data generators whose experiential input alters prescribing trajectories, creating a feedback-dominant care cycle that improves therapeutic alignment—revealing how decentralized information flows can enhance medical learning without compromising safety when integrated systematically. What’s underappreciated is that safety here is not eroded by autonomy but co-produced through it, as patients’ consistent engagement generates signals that clinicians use to preempt risks, thus embedding safety within adaptive learning rather than top-down control.
Risk redistribution architecture
Allowing patients to adjust their own medication doses redistributes—not eliminates—clinical risk from physicians to a shared responsibility framework, altering liability and accountability dynamics across the care ecosystem. This redistribution is enabled by structured protocols like dose titration guidelines and safety check-ins, which legitimize patient agency while anchoring it in institutional oversight, as seen in models like cancer pain management pathways or methadone maintenance programs. The key systemic mechanism is the formal delegation of bounded autonomy, wherein medical authority is conditionally transferred based on patient reliability and monitoring capacity, transforming the clinic into a hybrid governance space. The non-obvious consequence is that safety is recalibrated through distributed ownership of outcomes, where risk is managed not by centralization but by architectural design that balances trust with structured surveillance.
Therapeutic legitimacy expansion
Patient-directed dosing expands the boundaries of medically legitimate practice by incorporating subjective pain experience as a valid criterion for treatment modification, challenging biomedical norms that prioritize objective biomarkers over patient-reported outcomes. This expansion is made possible by policy shifts such as patient-centered care mandates in the U.S. Affordable Care Act and accreditation standards from organizations like the Joint Commission, which pressure providers to treat patient preference as a clinical variable. The systemic consequence is that medical legitimacy now depends not only on physiological plausibility but also on demonstrated responsiveness to patient autonomy, effectively institutionalizing experiential knowledge within clinical protocols. Underappreciated is how this redefines safety not as adherence to fixed standards, but as alignment with evolving patient-contextual norms—thus making legitimacy itself a dynamic regulatory mechanism.
Therapeutic Trust Gap
Patient-directed dosing exposes a collapse in therapeutic trust, where the clinician’s fiduciary duty under deontological ethics clashes with the patient’s exercise of autonomy grounded in liberal self-ownership. Regulatory frameworks like the Controlled Substances Act impose rigid hierarchies of medical authority, yet chronic pain patients invoking bodily sovereignty often bypass prescribed regimens, revealing an operational schism between ethical obligation and lived agency. This fraying is most acute not in noncompliance itself, but in how routinely it is anticipated and silently accommodated within primary care settings—making the unspoken norm a form of tolerated defiance. The non-obvious reality is that medical safety protocols are often designed less to prevent harm than to preserve institutional legitimacy in the face of distributed, low-visibility patient improvisation.
Opioid tapering backlash
Patient-directed dosing in the aftermath of the 2016 CDC Opioid Prescribing Guidelines reveals a surge in patient-led resistance when clinicians abruptly reduced or discontinued opioids in stable chronic pain patients. In states like Oregon and Colorado, long-term users, some on stable regimens for over a decade, organized advocacy networks such as 'Parents Opposed to Opioid Bans' and documented cases of suicide, hospitalization, and withdrawal following enforced tapering—demonstrating that medical safety protocols, when imposed without patient input, can generate harms that outweigh intended benefits. The non-obvious consequence here is that institutional efforts to enhance safety can destabilize autonomous patient-care equilibria that were clinically effective despite being off-label or guideline-nonconforming.
N-of-1 trial adoption
The NHS Greater Glasgow and Clyde's implementation of patient-directed n-of-1 trials for tramadol in chronic neuropathic pain patients revealed that when individuals control dosing timing and quantity within physician-set boundaries, they consistently self-optimize below standard doses without loss of efficacy. This system used real-time digital logging and monthly clinician review, creating a feedback loop where patient autonomy became a diagnostic input rather than a compliance risk. The underappreciated insight is that patient direction, when structured through iterative experimental frameworks, can transform subjective experience into a safety-enhancing data stream rather than a source of unpredictability.
Veterans Health Administration paradox
Within the Veterans Health Administration's Pain Management Program post-2010, patient-directed dosing for service-related chronic pain frequently conflicted with centralized opioid risk mitigation policies, particularly in rural clinics across Alabama and Nevada where access to pain specialists was limited. Veterans with PTSD-comorbid pain began using VA My HealtheVet portals to adjust medication logs and request dose changes without provider consultation, exploiting system flexibility meant for adherence support. This reveals that when institutional safety mechanisms become geographically and temporally rigid, patient autonomy evolves into a shadow coordination system that maintains function at the cost of regulatory visibility.