Should You Trust Experimental Stem Cells for Parkinsons?
Analysis reveals 8 key thematic connections.
Key Findings
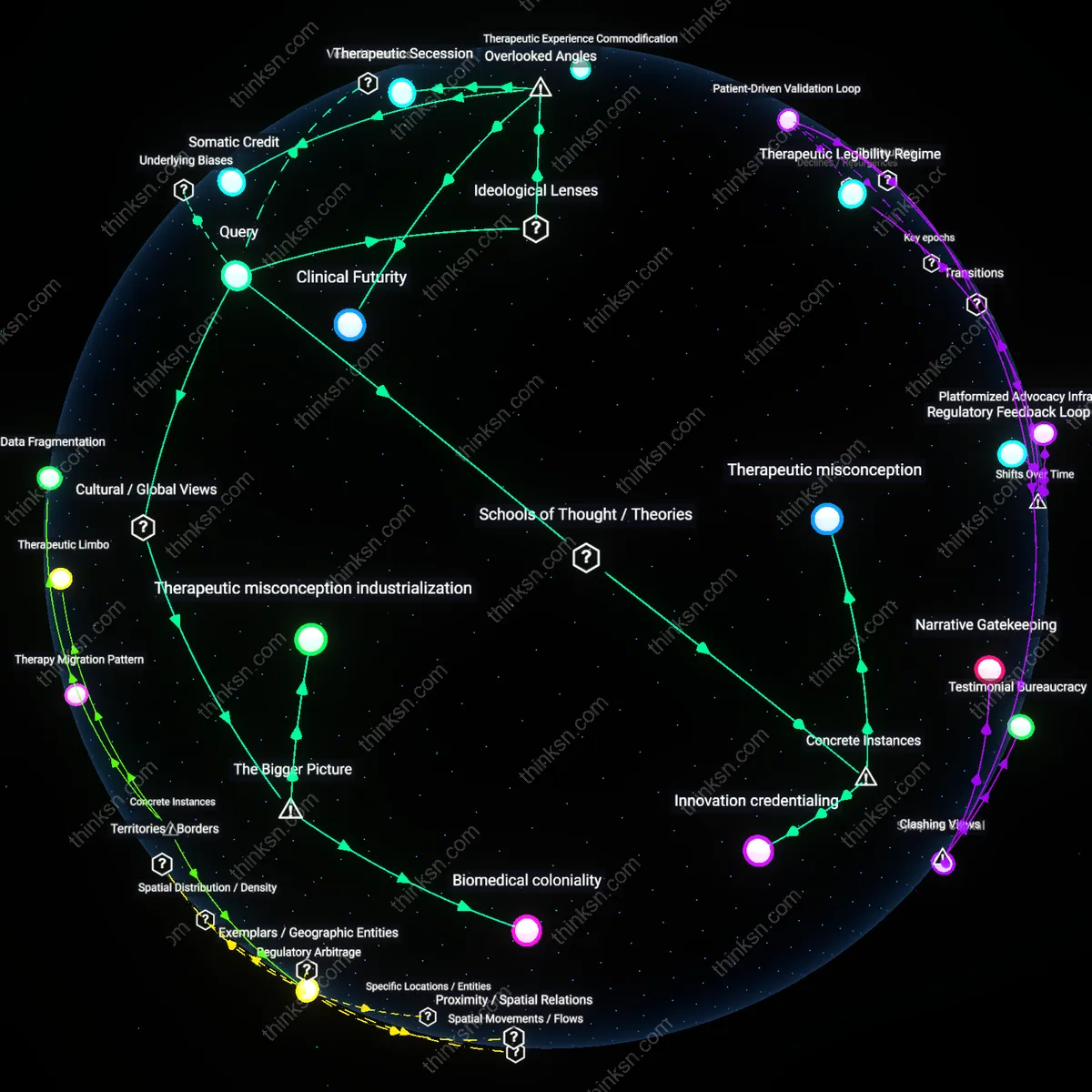
Therapeutic misconception
Patients conflate clinical research with individualized treatment when specialists recommend experimental stem-cell therapies, as occurred in the 2010s clinics offering unproven stem-cell injections in Mexico for Parkinson’s disease, where neurologists repositioned themselves as innovators by bypassing regulatory oversight through cross-border delivery; this shift masked the lack of controlled trial data under the guise of personalized medical breakthroughs, revealing how proximity to experimental authority can dissolve critical distinctions between care and research.
Innovation credentialing
Specialists gain institutional legitimacy by affiliating with high-profile research networks, such as the International Society for Stem Cell Research, which endorsed non-randomized clinical trials for Parkinson’s stem-cell interventions at Kyoto University in the 2018–2022 period; this allowed physicians to present participation in protocol-driven innovation as equivalent to therapeutic efficacy, leveraging prestige asymmetries between academic centers and patient communities to naturalize experimental risks as progressive care.
Evidence arbitrage
Clinics in Panama, such as Cellmedicine, exploited regulatory misalignment by importing U.S.-sourced mesenchymal stem cells under 'minimal manipulation' loopholes to treat Parkinson’s patients from North America, where the FDA prohibits such uses; this transnational therapeutic model profits from differential evidence standards, converting jurisdictional fragmentation into a business strategy that shifts evidentiary burdens onto patients while maintaining a veneer of scientific legitimacy derived from partial trial data.
Clinical Futurity
A patient considering experimental stem-cell therapy for Parkinson’s must confront how the neoliberal restructuring of public research funding shifts risk onto individuals by prioritizing speculative innovation over proven care pathways. In the U.S. and U.K., declining state investment in chronic disease management has inflated the perceived value of unproven interventions, with academic medical centers increasingly dependent on venture-aligned biotech partnerships that frame experimental trials as moral imperatives, thereby pressuring patients to become pioneers in lieu of systemic support. This dynamic is non-obvious because it recasts treatment decisions as outcomes of fiscal policy rather than medical judgment, revealing how deferred public health obligations create demand for experimental solutions.
Somatic Credit
The decision to undergo experimental stem-cell therapy is shaped by an unacknowledged economy in which patients’ biological data and post-procedure monitoring time are extracted as valuable assets under real-world evidence (RWE) collection frameworks tied to regulatory fast-tracking mechanisms like the FDA’s RMAT designation. Biopharmaceutical firms leverage these therapies to accumulate longitudinal patient data under minimal liability, effectively turning individual bodies into subsidized monitoring nodes in a regulated market formation. This reframes consent as a site of silent commodification—rarely acknowledged because it operates through post-trial data rights rather than direct financial transaction.
Therapeutic Secession
Patients from high-income countries who travel to unregulated clinics in Mexico, India, or Ukraine for stem-cell therapies are enacting a form of medical secession that reconfigures sovereign responsibility, where personal autonomy is weaponized to escape domestic regulatory safeguards, effectively privatizing risk in ways that erode collective health governance. This trend is reinforced by transnational networks of concierge medical brokers and digital advocacy platforms that portray regulation as oppression, a narrative that systematically weakens public trust in centralized science institutions. The overlooked dimension is geographic jurisdictional arbitrage—patients don’t just seek treatment, they exit regulatory communities, altering the power of states to enforce medical standards.
Biomedical coloniality
Western medical institutions hold authority over what counts as legitimate evidence for experimental stem-cell therapies, which marginalizes non-Western healing paradigms and reinforces a global hierarchy where clinical trials in high-income countries validate treatments before they are accessible in lower-income regions; this dynamic enables pharmaceutical and research centers in North America and Europe to set epistemic standards that often disregard traditional or community-based knowledge systems in Africa, Asia, and Latin America, where stem-cell interventions may be informally practiced but dismissed as unscientific. The systemic consequence is that patients from Global South contexts seeking treatment for Parkinson’s disease face dual exclusion—both from early access to trials and from having their own cultural frameworks for bodily repair recognized in risk-benefit assessments, revealing how epistemic dominance functions as a form of structural gatekeeping in global health innovation.
Therapeutic misconception industrialization
In regions like Southeast Asia and parts of Eastern Europe, private clinics offer unproven stem-cell therapies for Parkinson’s under the guise of medical tourism, exploiting regulatory gaps and patients’ desperation while Western bioethics frames the issue narrowly as individual informed consent; this commercial ecosystem thrives not because of scientific validity but because global disparities in healthcare access create demand surges that are met by loosely governed for-profit providers who leverage cultural narratives of hope and revival. The systemic trigger is the mismatch between slow-moving, evidence-based regulatory frameworks in Western democracies and the rapid commodification of biomedical hope in jurisdictions where oversight is weak, turning patient vulnerability into a scalable business model and shifting the ethical burden onto individuals ill-equipped to navigate cross-border medical claims.